 |
 |
 |
| |
TMC114/r tolerability in treatment-experienced, hepatitis B or C (HBV/HCV)
co-infected patients in POWER 1 and 3
|
| |
| |
Reported by Jules Levin
IDSA, Toronto, Oct 12-15, 2006
Rachlis A,1 Clotet B,2 Baxter J,3 Lefebvre E4
1Sunnybrook Health Sciences Center, Toronto, Ontario, Canada; 2Hospital Universitari Germans Trias i Pujol, Barcelona, Catalonia, Spain; 3Cooper University Hospital/RWJ Medical School, Camden, NJ; 4Tibotec Inc., Yardley,
PA, USA
ABSTRACT
Background: TMC114 with low-dose ritonavir (TMC114/r) had significant antiviral efficacy versus investigator-selected control protease inhibitors (CPIs) in POWER 1 (TMC114-C213) and 2 (TMC114-C202), and was generally well tolerated. Similar results were observed in the open-label POWER 3 (TMC114-C215/208) analysis.
This sub-analysis examines TMC114/r safety in POWER 1 and 3 hepatitis B virus/hepatitis C virus (HBV/HCV) co-infected patients (POWER 2 exclusion).
Methods: POWER 1 and 3 had similar inclusion criteria (NRTI, NNRTI and PI experience, 31 primary PI mutation and HIV-1 RNA >1,000 copies/mL). POWER 1 patients received one of four TMC114/r doses or CPI of choice, plus optimized background regimen (OBR; NRTI ± enfuvirtide [ENF]). POWER 3 patients received TMC114/r 600/100mg bid plus OBR. HBV/HCV co-infected patients with stable condition and not requiring hepatitis treatment were allowed in POWER 1
and 3. Adverse events (AEs) and laboratory abnormalities were evaluated.
Results: Six hundred and thirty-four TMC114/r and 63 CPI patients were assessed;
15% of TMC114/r and 21% of CPI patients had co-infection (active: 12% and 16%, respectively).
Results for patients without co-infection and with active co-infection are reported; those for non-actively co-infected patients are not reported as their number was too small to allow meaningful conclusions.
Patients with active co-infection had a higher incidence of liver-related
AEs than those without co-infection in both treatment groups (TMC114/r: 13% vs 8%; CPI: 20% vs 12%).
These were mainly linked to a higher incidence of aspartate aminotransferase
(AST), alanine aminotransferase (ALT) and gamma glutamyltransferase (GGT) elevations.
Conclusions: TMC114/r was generally well tolerated in treatment-experienced patients, including HBV/HCV co-infected patients. Most liver-related AEs in co-infected patients were due to asymptomatic elevations of liver parameters. No differences in liver-related AEs were observed between treatment groups.
no case of hepatotoxicity was reported.
The three most common treatment-emergent AEs experienced by patients with and without active HBV or HCV co-infection in the TMC114/r treatment groups were diarrhea, headache and nausea.
the majority of ALT or AST laboratory abnormalities were grade 1 or 2.
Standard clinical monitoring of patients with chronic HBV and/or HCV receiving TMC114/r is considered adequate.
The introduction of highly active antiretroviral therapy (HAART), while extending the life of HIV-infected patients, has allowed the less progressive course of HBV and HCV infection to emerge as a leading cause of morbidity and mortality among HIV-infected patients.10,11 The management of HIV-infected patients co-infected with HBV or HCV has now become a major challenge for clinicians around the world.
Patients co-infected with HBV or HCV were allowed to enter the POWER 1 trial or POWER 3 analysis if their condition was clinically stable and they did not require treatment for hepatitis infection during the trial periods. Patients with acute hepatitis A virus (HAV) were not allowed to participate.
Data from 697 patients who received any TMC114/r dose or CPI(s) in the POWER 1 trial and the TMC114 600/100mg bid dose in the POWER 3 analysis were pooled to allow a large enough sample size to draw meaningful conclusions.
Three categories of HBV or HCV co-infection status were defined
- not co-infected: negative on all HBV and HCV tests, and a negative answer on the randomization question: "Is the patient co-infected?"
- active co-infection: positive on hepatitis B surface antigen, or positive on HCV PCR (polymerase chain reaction) test, irrespective of a positive or negative answer to the randomization question:
"Is the patient co-infected?"
- non-active co-infection: applied to all other possible outcomes.
Results for patients without co-infection and with active co-infection are reported; those with nonactive co-infection are not reported due to the small sample size. All available data included in the original NDA submission was included in this analysis. Mean treatment duration (exposure) for TMC114/r patients was 44 weeks and for CPI patients was 36 weeks.
RESULTS
Baseline co-infection status
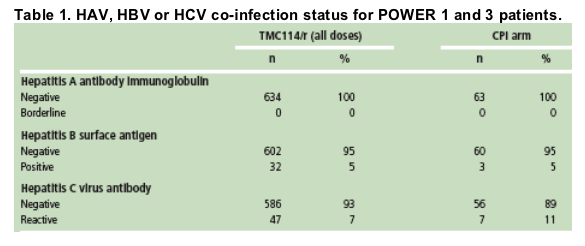
Patients from POWER 1 and 3 were tested at baseline for HAV, HBV or HCV co-infection (Table 1)
- overall, HCV co-infection was more common than HBV co-infection (7-11% vs 5% of patients, respectively).
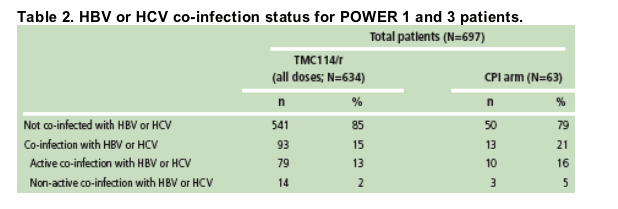
A total of 697 POWER 1 and 3 patients who were receiving TMC114/r treatment for HIV-1 infection were assessed in this analysis; these patients consisted of 634 TMC114/r patients and 63 CPI patients. The co-infection status of HBV and HCV is shown in Table 2.
Safety
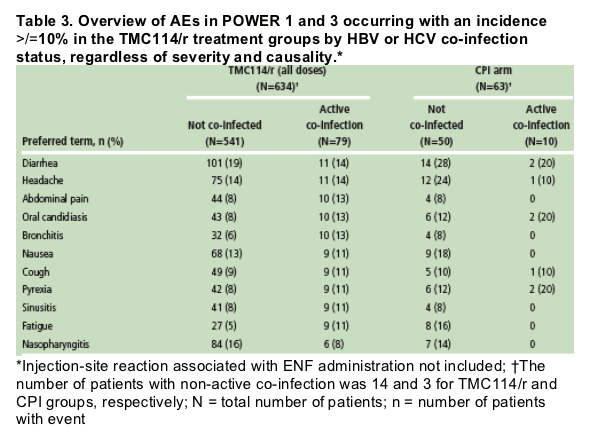
Overall, there were no specific safety concerns following treatment with TMC114/r in patients co-infected with HBV or HCV. Table 3 presents an overview of the most common AEs reported during treatment with TMC114/r or CPI(s) by HBV or HCV co-infection status
- apart from injection-site reactions associated with enfuvirtide administration, the three most common treatment-emergent AEs experienced in at least 10% of patients in both TMC114/r treatment subgroups (not co-infected versus active co-infection) were diarrhea, headache and nausea.
No meaningful difference between the incidences of liver-related AEs was observed between the TMC114/r and the CPI(s) groups.
There were no deaths due to liver-related disorders in this population.
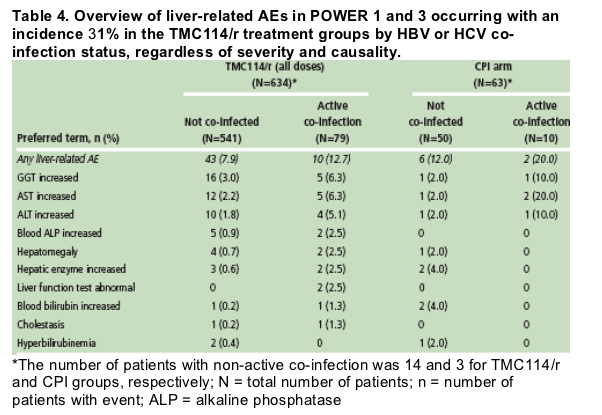
There was a higher incidence of liver-related AEs in patients with active HBV or HCV co-infection than in those without co-infection in both the TMC114/r and CPI groups (Table 4)
- these AEs were mainly related to the higher incidence of increased AST, ALT and GGT, which occurred in 5-6% of TMC114/r-treated patients with active HBV and HCV and 2-3% of patients without HBV and HCV co-infection
- no case of hepatotoxicity was reported.
Out of those patients with active co-infection, one patient receiving TMC114/r in POWER 3 and one from the CPI arm of POWER 1 discontinued treatment due to liver-related AEs resulting from grade 3 or 4 increases in ALT and AST; none was related to treatment.
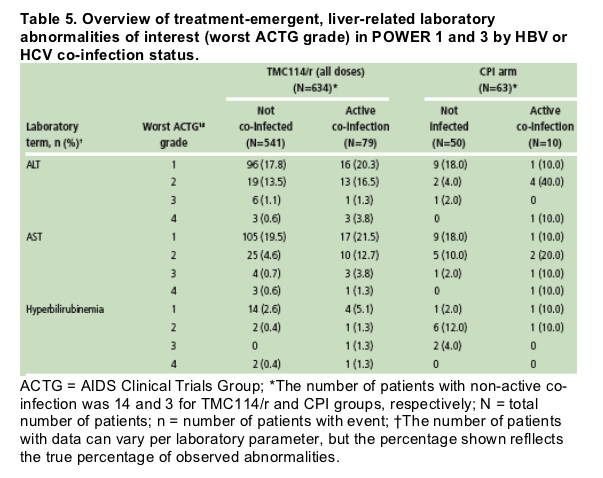
In this analysis, baseline and treatment-emergent increases in ALT or AST were observed more frequently in patients with active hepatitis B or C co-infection versus those without (treatmentemergent shown in Table 5)
- no meaningful difference was observed between the TMC114/r and the CPI(s) groups
- most laboratory abnormalities were grade 1 and 2, and there was a 5% incidence of grade 3 and 4 ALT or AST in patients treated with TMC114/r with active co-infection.
Efficacy
TMC114/r efficacy was similar in co-infected and non-co-infected HBV or HCV patients. The proportion of patients with active co-infection and without co-infection initiating treatment at the approved dose of TMC114/r 600/100mg bid in POWER 1 and 3 and reaching <50 copies/mL of plasma HIV-1 RNA at 24 weeks (time to loss of virologic response algorithm) was 46% (n=46) and 42% (n=261), respectively.
|
| |
|
 |
 |
|
|