 |
 |
 |
| |
Virological evolution in HIV treatment-experienced patients with raltegravir-based salvage regimens
|
| |
| |
Reported by Jules Levin
XVII HIV Drug Resistance Workshop
June 10-14, 2008
Sitges, Spain
Katlama C.1 Caby F.1, Schneider L.1, Andrade R.M.1,Tubiana A.1,Valantin M.A.1, Ktorza N.1, Malet I.2, Peytavin G.3, Canestri A.1V.Calvez
1- Hôpital Pitié-Salpêtrière, UPMC Univ Paris 6, Paris; 2- Service de Virologie, Hôpital Pitié Salpêtrière, Paris; 3- Service de Pharmacologie, Hôpital Bichat, Paris
AUTHOR CONCLUSIONS
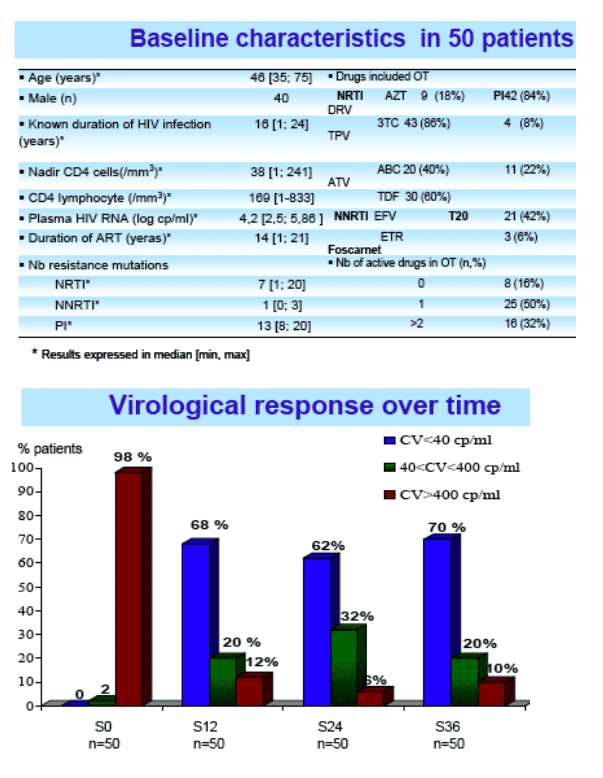
--high success rate in patients with multi-drug resistant virus (68% undetectable)
--in our experience, the majority of patients with virological failure to raltegravir-regimens showed low viremia for a prolonged period of time; low rate of failure with high viremia
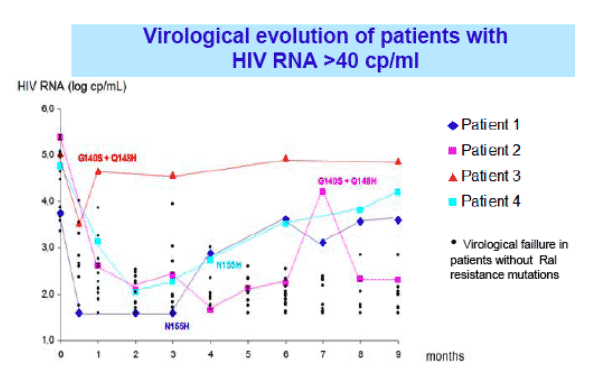
--in patients with low level plasma viremia (HIV RNA <40 copies/ml), there was no rapid onset of rebounds or resistance mutations up to 36 weeks: presence of raltegravir-resistance mutations was associated with the highest viral replication rates.
--a longer follow-up will allow for a better understanding of the evolution of raltegravir resistance profile.
BACKGROUND
Raltegravir (RAL), a novel integrase inhibitor, is indicated in patients in situation of multi-treatment failure in combination with antiretroviral optimized treatment (OT).
Despite high potency, raltegravir generates mutations in case of persistent viral replication which appears rapidly in the event of non control of plasma viremia (from Jules: resistance to raltegravir appears to develop not as quickly as NNRTIs and more quickly than proteasr inhibitors).
This study aimed to evaluate in real life conditions the virological response of a raltegravir-containing regimen, in patients with, multidrug resistance and the consequences in terms of resistance in case of persistant viral replication above 40 copies/ml.
METHODS
Prospective cohort study of experienced HIV treated patients with prior exposure to the 3 class drugs, with HIV RNA >1000cp/mL, who have started RALTEGRAVIR between 11/06 et 09/07, and followed for 12 months
Primary end-points : proportion of patients with viral load > 50 cp/ml
Secondary end points:
-% pts with HIV RNA between 40 and 400 cp/ml -Genotypic resistance if HIV RNA > 40 cp/ml
FROM ABSTRACT
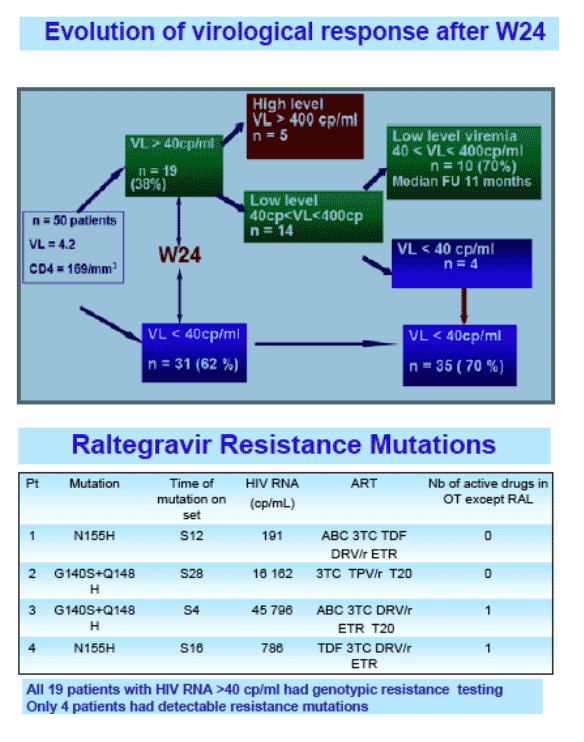
RESULTS: Fifty patients were included. Prior ARV therapy contained enfuvirtide (57%), darunavir(68%), etravirine(37%), foscarnet(12%). Median baseline characteristics were as follows: CD4 T cell count=169/mm3 [1-833]; pHIV-RNA=15136cp/mL [339-724436]. Baseline mutation number was: NRTI=7 [1-10], NNRTI=1[0-4] and PI=13[8-20]. RAL was used in combination with enfuvirtide(35%), darunavir(84%), etravirine(74%), atazanavir(29%), foscarnet(6%). The median follow-up was W36 [6-15]. Thirty-four patients(68%) had virological success with pHIV-RNA<40 at W24. Eleven patients(22%) had low persistent viral load (40< pHIV-RNA<400) and three(6%) had high persistent viremia (pHIV-RNA>400). The viral load of the remaining 2 patients were between 40 and 400cp/mL at W24, but one of them became undetectable at W28, and the other reached levels above 400cp/mL. Among the patients in virological failure, genotype resistance testing was successfully performed in 13 patients and RAL resistance mutations were detected in 4.
G140S+Q148H were detected in 2 patients, N155H in 1 patient and a mutation switch from N155H to G140S+Q148H was observed in the last one. Three of these 4 patients had pHIV-RNA>400.
CONCLUSION: In our experience, the majority of patients in virological failure to RAL-based regimens showed low viremia for a prolonged period without exacerbation. The presence of RAL-resistance mutations was associated to the highest viral replication rates. A longer follow-up of such patients will allow a better understanding of the evolution of RAL resistance profile.
|
| |
|
 |
 |
|
|