 |
 |
 |
| |
Relationship between Current Level of Immunodeficiency and Non-AIDS-defining Malignancies, EuroSida: "Immunosuppression ...current CD4 count....was associated with an excess risk of NADM"
|
| |
| |
Reported by Jules Levin_CROI 2009 Feb 8-12 Montreal__Joanne Reekie*1, A Mocroft1, F Engsig2, A D'Arminio Monforte3, A Wiercinska-Drapalo4, P Domingo5, F Antunes6, N Clumeck7, O Kirk8, J Lundgren8, and EuroSIDA Study Group
1University College London Medical School, London, UK; 2Rigshospitalet, Copenhagen, Denmark; 3Istituto Di Clinica Malattie Infettive e Tropicale, Milan, Italy; 4Medical University, Bialystok, Poland; 5Hospital Sant Pau, Barcelona, Spain; 6Hospital Curry Cabral, Lisbon, Portugal; 7Institue of Tropical Medicine, Antwerp, Belgium; and 8Copenhagen HIV Program, Panum Institute, Copenhagen, Denmark
Background: Incidence of non-AIDS defining malignancies (NADM) may be elevated in patients with HIV. The reasons for this increase remain elusive, but may include immunosuppression and increased prevalence of traditional risk factors such as smoking. The aim of this analysis was to investigate whether current CD4 count was independently associated with the risk of NADM after accounting for traditional and other HIV-associated risk factors.
Methods: We included 12,865 patients with a CD4 count prior to enrollment in EuroSIDA; Poisson regession was used to determine factors related to the development of NADM, classified using the International Classification of Diseases (ICD-10) system. Models were adjusted for year of follow-up, gender, exposure group, race, region of Europe, time on combination ART (cART), age, hepatitis B and C, and smoking status
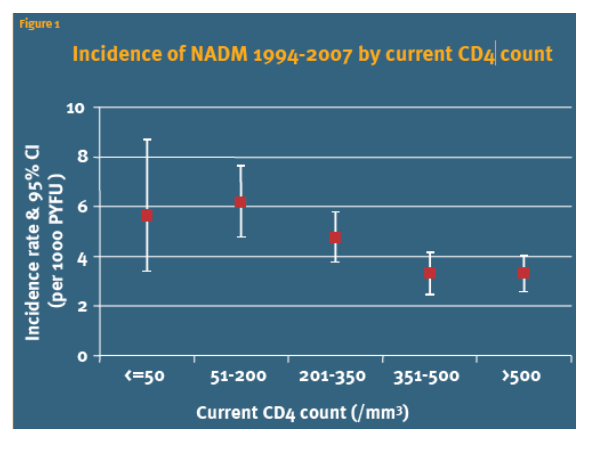
Results: A total of 317 NADM (58 anal, 24 lung, 60 hematological, 48 Hodgkin's lymphoma, 40 genitourinary, 55 digestive, and 80 other) were diagnosed; incidence rate 4.2 per 1000 person-years of follow-up (95%CI 3.7 to 4.7). Within 6 months of NADM diagnosis, 45 patients died. The figure shows the incidence of NADM by current CD4 count. After adjustment, persons with a current CD4 count ≦50/mm3 had a 76% higher rate of developing NADM (IRR 1.76; 95%CI 1.02 to 3.02, p = 0.0408), 51 to 200/mm3 a 82% higher rate (1.82; 1.26 to 2.62, p = 0.0014), 201 to 350/mm3 a 43% higher rate (1.43; 1.03 to 1.97), compared to those with a current CD4 count >500/mm3. There was no significant difference in the adjusted incidence rate between those with current CD4 counts 351 to 500/mm3 and >500/mm3 (p = 0.89). A higher current CD4 count (per doubling) was associated with a decreased incidence of anal cancer (IRR 0.83), heamatological (0.94), gentourinary (0.87), and digestive cancers (0.84), but due to small numbers of events was signifcicant only for anal (p = 0.0038) and digestive cancers (p = 0.0233).
Conclusions: Immunosuppression was associated with an excess risk of NADM. One possible explanation is enhanced oncogenic potential by pro-oncogenic viruses (e.g., human papillomavirus and anal cancer). An infectious oncogenesis has only been established for a few of NADM linked with immunosuppression in this study and other mechanisms may also contribute. As the immunosuppression may be reversed by cART, HIV is a suitable candidate model for improving our understanding of how immunosuppression affects oncogenic transformation.
RESULTS
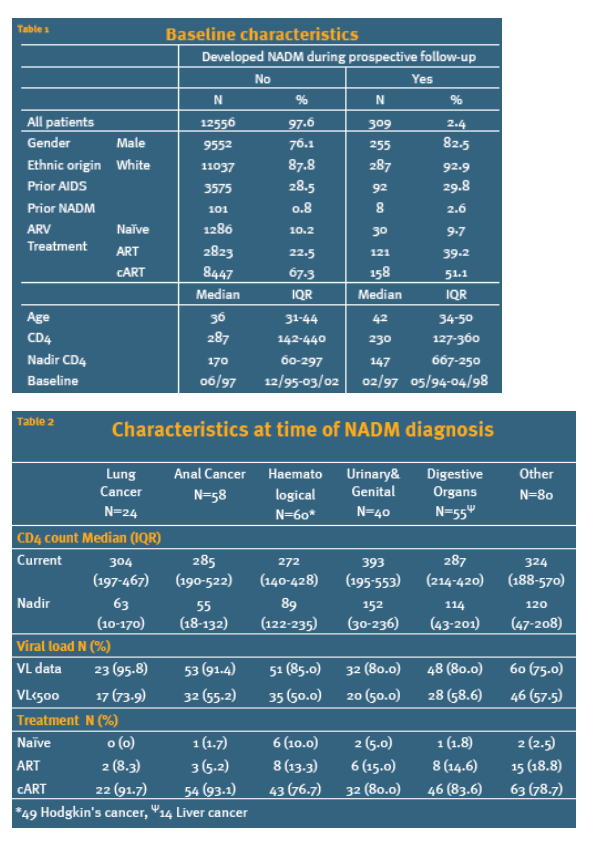
Table 1 shows the baseline characteristics, comparing those who developed a NADM to those who did not. Patients developing NADM were more likely to be male (p=0.01), older (p<0.0001), have a lower CD4 count (p=0.0001), have had a prior NADM (p=0.01) and have been enrolled in EuroSIDA earlier (p<.0001).
317 NADM were recorded over 75,234 person years with an incidence rate of 4.2 per 1000 PYFU 95%CI (3.7-4.7). 301 patients developed one and 8 patients developed two different NADM whilst under follow-up. Table 2 shows the patient characteristics at time of diagnosis for different NADM. Patients with anal or haematological cancer were younger and had lower CD4 counts. 24% (95%CI 18, 30) and 40% (95% CI 33, 47) were estimated to have died at 12 and 24 months after diagnosis of NADM using Kaplan Meier estimation.
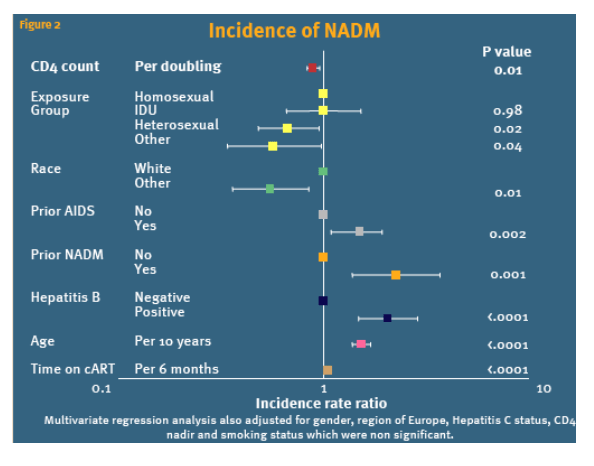
Figure 1 shows the relationship between current CD4 count and incidence of NADM. There was an increasing incidence of NADM as current CD4 count decreases. Figure 2 shows that after adjustment there was a decreasing rate of NADM with increasing CD4 count. For each doubling of the CD4 count there was an 11% decreased incidence of developing a NADM. In addition ethnicity, prior AIDS diagnosis, prior NADM diagnosis, time on cART, hepatitis B status, and age were all significant predictors of developing NADM.
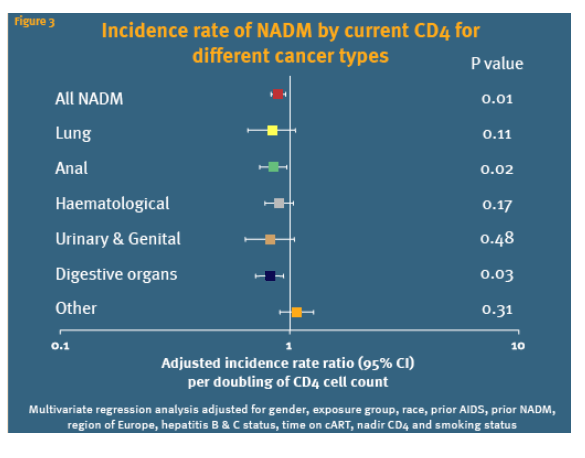
Figure 3 shows the relationship between current CD4 count and the incidence of specific NADM was consistent for the different diagnoses, except the less common, NADM (grouped as other), but due to the small number of events and limited power was only significant for anal (p=0.02) and digestive cancers (p=0.003).
CONCLUSION
Current immunodefiencency was associated with an excess risk of NADM. One possible explanation is enhanced oncogenic potential by pro-oncogenic viruses (e.g. HPV and anal cancer). An infectious oncogenesis has only been established for a few of NADM linked with immunosuppression in this study and other mechanisms may also contribute. As the immunosuppression may be reversed by cART, HIV is a suitable candidate model for improving our understanding of how immunosuppression affects oncogenic transformation.
|
| |
|
 |
 |
|
|