 |
 |
 |
| |
Genotype 1b vs 1a and Peg/Rbv Lead-In
|
| |
| |
by Jules Levin, NATAP
The phase 3 presentations at the recent AASLD did not address the genotype 1a vs 1b question, difference in SVR rates but here is data from phase 2. In studies at AASLD and other previous studies examining oral HCV drug regimens that did not contain peg/rbv genotype 1a often is associated with the development of more drug resistance and higher viral failure rates. A more potent regimen and the use of a nucleoside or nucleotide in the regimen would be expected to help, but what's the affect of adding peg/rbv to 1 oral, either boceprevir or telaprevir. Phase 3 presentations of both drugs at AASLD did not address this but here is what I found from phase 2 data.
from Lancet Aug 2010 SPRINT1 publication:
Efficacy of boceprevir, an NS3 protease inhibitor, in combination ...
Aug 9, 2010 ... The aim of the hepatitis C virus SPRINT-1 (Serine Protease Inhibitor Therapy-1) study was to establish the safety and efficacy of boceprevir ...
www.natap.org/2010/HCV/080910_01.htm
In the boceprevir groups, the lead-in groups were associated with a modestly lower rate of breakthrough than were the groups with no lead in. Combining across treatment groups, the rate of breakthrough in the boceprevir lead-in groups was 4% (nine of 206) compared with 9% (19/210) in the boceprevir groups with no lead in (p=0·057).
The lead-in (PR4) allowed us to examine the relation of peginterferon and ribavirin responsiveness at week 4 to SVR with boceprevir-containing regimens. In the PR4 28-week or 48-week groups, SVR was similar in participants with greater than 1·5 log10 reduction in hepatitis C virus RNA from baseline before the addition of boceprevir. Higher SVR was noted in participants who received PRB for 44 weeks with less than 1·5 log10 reduction from baseline at PR4 (figure 5). In patients with less than 1 log10 reduction with PR4, 55% (95% CI 32-76) SVR was noted in the PR4/PRB44 group.
The viral response during the lead-in could help to predict best possible treatment duration. Patients achieving less than 1·5 log10 reduction in viral level after PR4 benefit most from a treatment duration of 48 weeks, whereas those with greater than 1·5 log10 reduction show similar SVR irrespective of treatment duration of 28 weeks or 48 weeks.
The lead-in can identify null responders to peginterferon alfa-2b and ribavirin, who seem to be at greatest risk for treatment failure with specifically targeted therapies and for development of resistance. However, in our cohort, a substantial proportion of null responders during the lead-in period went on to achieve SVR with the addition of boceprevir.16, 27
This study assessed the use of a PR4 lead-in before the addition of boceprevir, as well as the effect of starting all three drugs concomitantly, and compared these groups with PR48 control. In the novel lead-in approach, we recorded increased SVR and a reduction in relapse and breakthrough, and allowed for potential determination of treatment duration on the basis of responsiveness to the PR4 lead-in. However, in the direct comparison between lead-in and non-lead-in groups, relapse reduction did not differ significantly, although the absence of a statistically conclusive result is not surprising since the sample size did not allow detection of modest diff erences between lead-in and non-lead-in groups.
Table 4: Factors aff ecting sustained virological relapse (genotype 1b predicts better respons ethan 1a, but clearly 1a responds.)
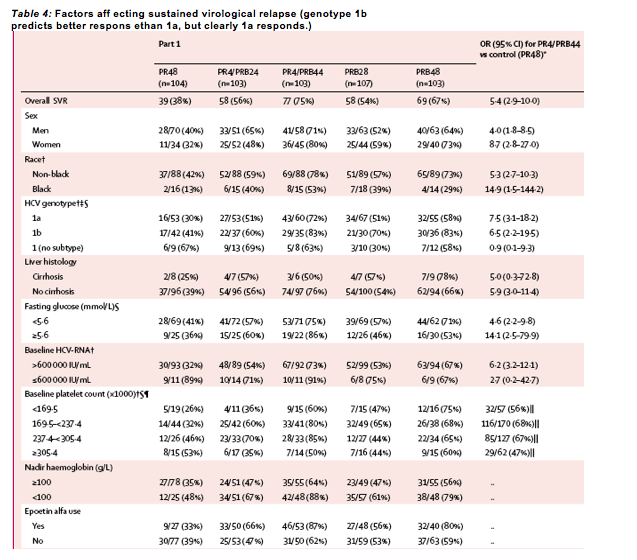
PR4 (lead-in)=peginterferon alfa-2b 1·5 µg/kg plus ribavirin 800-1400 mg per day for 4 weeks. PR48 (control)=peginterferon alfa-2b 1·5 µg/kg plus ribavirin 800-1400 mg per day for 48 weeks. PRB24/28/44/48=peginterferon alfa-2b, ribavirin, and boceprevir 800 mg three times a day for 24, 28, 44, or 48 weeks. OR=odds ratio. SVR=sustained virological response. HCV=hepatitis C virus. *For each baseline subgroup, the odds ratio and 95% CI for treatment eff ect (PR4/PRB44 vs PR48) are based on logistic regression model with adjustment for stratification factors (race and cirrhosis status). Significant predictor of SVR based on multivariable logistic regression analysis (all boceprevir-containing groups combined): race (non-black vs black; OR 2·7, 95% CI 1·49-5·04); genotype (1b vs 1a/other; 2·0, 1·22-3·32); baseline viral load (low vs high; 2·3, 1·04-5·12); and standardised baseline platelet count (continuous; 0·8, 0·61-0·94). Viral genotype was measured with the TruGene assay (Bayer HealthCare, Berkeley, CA, USA). §Analyses of the relations between SVR and hepatitis C virus genotype, fasting glucose, and baseline platelet count were not preplanned. Baseline platelet count included in multivariable logistic regression analysis as a continuous variable, standardised by transforming each patient's count as: (count-overall mean)/(overall SD). SVR rates are provided as descriptive statistics for platelet count intervals based on mean and SD: 169·5=1 SD below mean; 237·4=mean; 305·4=1 SD above mean. ||Data are number (%) for pooled boceprevir groups.
Telaprevir PROVE 2 publication NEJM April 30 2009:
Independent Predictors of Sustained Virologic Response
The association between a sustained virologic re- sponse and independent variables was explored with the use of a logistic-regression model. Treat- ment group and baseline HCV RNA level were the only two variables significantly associated with a sustained virologic response (P<0.001) (Table 1 in the Supplementary Appendix, available with the full text of this article at NEJM.org).
PROVE1
The viral population at the time of breakthrough consisted predominantly of variants containing mutations V36M and R155K (in 10 patients infected with HCV genotype 1a) or A156T (in 1 patient with HCV genotype 1b). The remaining patient had missed several days of dosing and had a breakthrough at day 8; this patient was infected with predominantly wild-type virus.
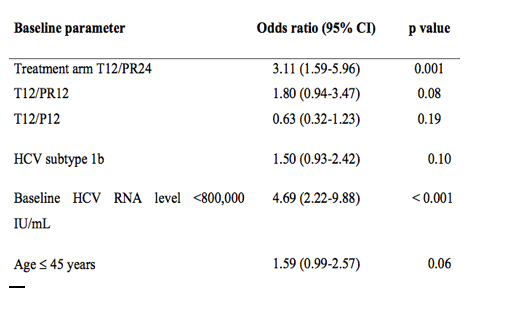
In PROVE2 (genotype 1b was not a significant predictor but a nonsignificant predictor):
Supplementary Table 1. Independent predictors of an SVR in multivariate analysis of baseline parameters. The following baseline variables were included in the analysis: gender, age (less or more than 45 years), BMI, baseline HCV RNA level (less or more than 800,000 IU/mL), genotype 1 subtype (1a vs 1b), ALT level, glucose level and treatment arm. Variables with a weak association (P>0.20) with the SVR in the initial logistic regression model were excluded from the final model. 95% CI: 95% confidence interval.
|
| |
|
 |
 |
|
|