 |
 |
 |
| |
Burden of Viral Hepatitis C in Japan: A Propensity Analysis of Patient Outcomes
|
| |
| |
Reported by Jues Levin
The 21st Conference of the Asian Pacific Association for the Study of the Liver, APASL 2011, Bangkok, Thailand, February 17-20, 2011
Gordon G. Liu, PhD 1; Marco daCosta DiBonaventura, PhD2; Yong Yuan, PhD 3; Jan-Samuel Wagner2; Gilbert J. L'Italien, PhD 3,4; Paul Langley, PhD5; Isao Kamae, MD, DrPH6
1Peking University Guanghua School of Management, China; 2Health Sciences Practice, Kantar Health, New York, NY; 3Global Health Outcomes, Bristol-Myers Squibb, Princeton, NJ;
4Yale University School of Medicine; 5College of Pharmacy, University of Minnesota, Minneapolis, MN; 6Keio University Graduate School of Health Management, Fujisawa, Japan



RESULTS
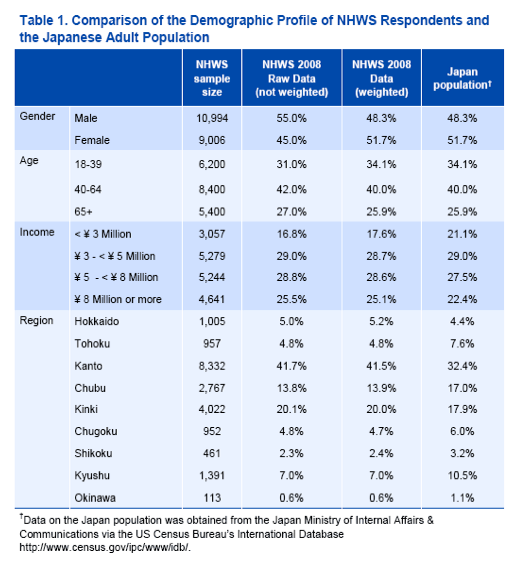
HCV patients were comparable to propensity-score matched controls on all demographic and health history variables except comorbidity burden (Charlson Comorbidity Index), which was marginally greater in the HCV group (see Tables 2 and 3).
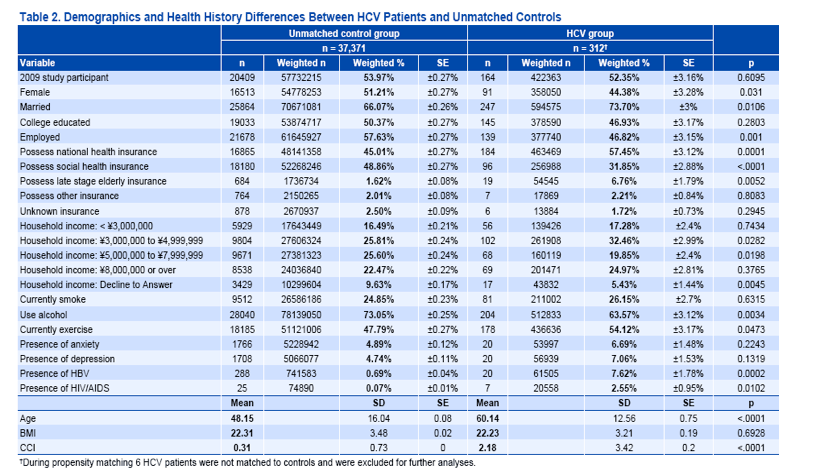
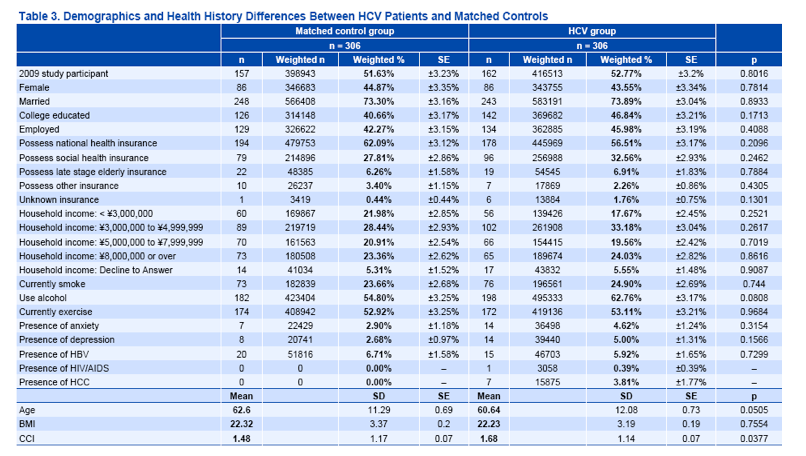
HCV patients also reported significantly more healthcare provider visits in the past six months (14.80 vs. 9.74, p<.05).
Because of the imbalance in comorbidity burden, additional analyses were rerun controlling for CCI. The results remained generally consistent:
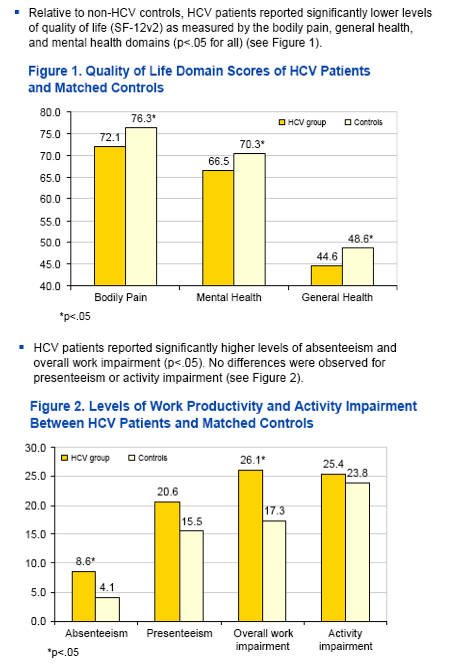
- HCV patients reported significantly lower levels of MCS (Adjusted means = 46.77 vs. 48.63), general health (Adjusted means = 44.35 vs. 48.43), and mental health (Adjusted means = 66.65 vs. 71.26) (all p<.05).
- Bodily pain differences were no longer significant.
- HCV patients reported marginally higher absenteeism (Adjusted means = 8.35% vs. 3.74%, p=.06) and marginally higher presenteeism (Adjusted means = 20.01% vs. 14.96%, p = .09) than matched controls.
-- However, HCV patients did report significantly higher overall work impairment (Adjusted means = 25.43% vs. 16.35%,), emergency room visits (Adjusted means = 0.61 vs. 0.18), and physician visits (Adjusted means = 14.56 vs. 9.87) than matched controls (all p<.05). No differences were observed on activity impairment or hospitalizations.

|
| |
|
 |
 |
|
|