 |
 |
 |
| |
Differences in CD4+ T-cell Immune Activation in HIV, Hepatitis C (HCV), and HIV/HCV Coinfection are Influenced by HIV and HCV Infection Status
|
| |
| |
Reported by Jules Levin
Intl AIDS Conf 2012 Wash DC July 22-27
A. Hodowanec1,2, K. E. Brady2, W. Gao3, S. Kincaid1, J. Plants2, M. Bahk1, A. Landay2, G. Huhn1,2
1Ruth M. Rothstein CORE Center, 2Rush University Medical Center, 3University of Illinois at Chicago Chicago, IL, USA
Conclusions
· This well-controlled study highlights patterns of CD4 immune activation in HIV/HCV-coinfection, as manifested by HLADR+ and CD38+ expression:
· HLADR+ expression in HIV/HCV-coinfection with well-controlled HIV appears to arise from chronic HCV viremia
· CD38+ expression is likely driven by underlying HIV infection
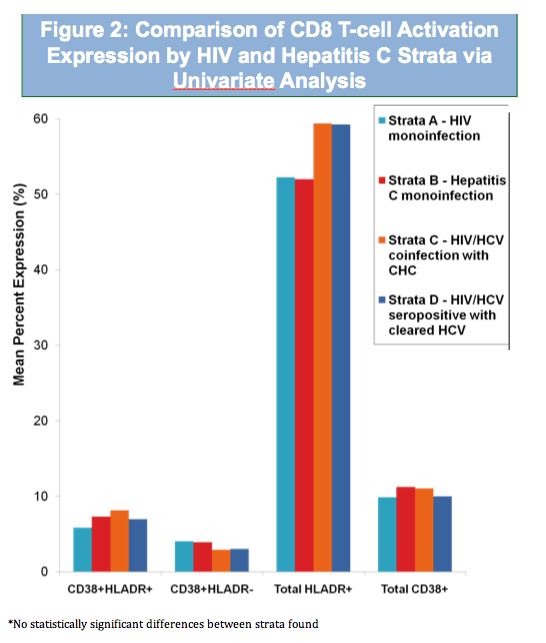
· No differences in CD8 activation were detected between our strata of subjects with well-controlled HIV infection
· Contrasts with findings in earlier studies (Kovacs, et al) with generally poorly-controlled HIV in which there was increased CD8 activation among coinfected patients
· Production of the anti-inflammatory cytokine IL-10 was significantly lower in HIV-monoinfection versus HIV/HCV-coinfection with CHC (p=0.0002)
· There were no consistent correlations between immune activation and TE-determined liver fibrosis stage inferred by HIV and HCV infection status
· Patients with TE-determined mild to moderate liver fibrosis appear to have overall lower levels of CD4 immune activation markers
· Significantly higher TE-determined liver stiffness values were measured in HCV monoinfection and HIV/HCV coinfection with CHC, in which the highest levels of CD4 HLADR+ expression were recorded, though in HCV monoinfection the lowest levels of CD38+ expression were observed
· Increased CD4+ immune activation in patients with longstanding HIV/HCV coinfection with CHC may contribute to amplified inflammatory responses, such as increased IL-10 production, that may lead to deleterious immune exhaustion, having an impact extending beyond known accelerated liver fibrosis
· Successful clearance of HCV may abrogate these immune activation and inflammatory responses
· Additional studies exploring the implications of immune activation in the setting of HCV treatment with newly licensed direct-acting antivirals (DAAs), as well as DAAs and therapeutic HCV vaccines in development, are needed
Revised Abstract
Background: HIV/HCV-coinfected patients have accelerated liver disease compared to HCV-monoinfection. In poorly-controlled HIV with chronic hepatitis C (CHC), immune activation has been primarily attributed to CD8 T-cell subsets. In well-controlled HIV, data comparing inflammatory cytokines and immune activation between HIV/HCV-coinfection with CHC to HIV/HCV-seropositive patients with cleared-HCV are underreported.
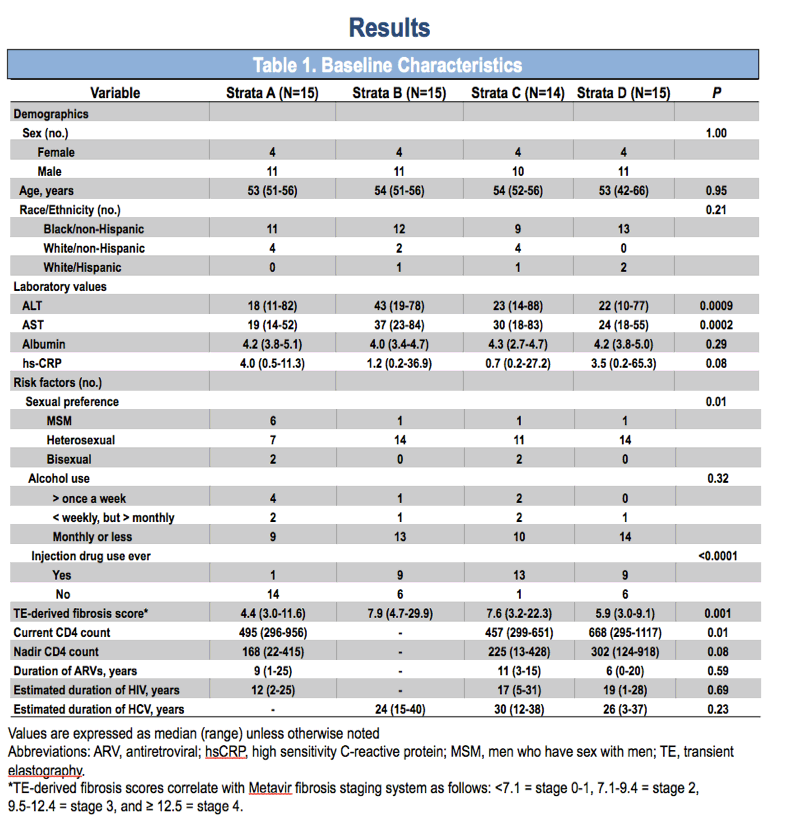
Methods: Fifty-nine age (median, 53 years) and sex (male=43/female=16)-matched patients were stratified: A) HIV-monoinfection (N=15), B) HCV-monoinfection with CHC (N=15), C) HIV/HCV-coinfection with CHC (N=14), and D) HIV/HCV-seropositive with cleared-HCV (N=15). All HIV+ patients had undetectable HIV viremia, and current CD4 counts in strata A and C were matched to CD4 at estimated timepoint of HCV clearance in strata D (median, CD4=420 cells/ml). Risk factors were recorded and serum collected for CD4 and CD8 immune activation (CD38/HLADR) and immune senescence (CD28) markers via flow cytometry, and luminex-multiplex cytokine assay. Immune and inflammatory markers were analyzed across strata using pair-wise t-tests; additional correlations of immune markers and cytokines were examined by multivariate analysis.
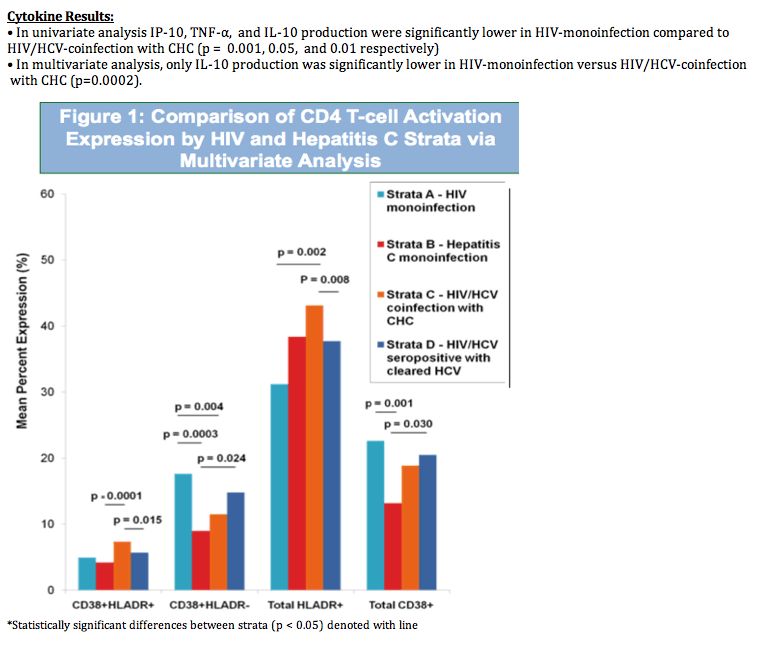
Results: CD38+HLADR+ expression on CD4+ T-cells was significantly increased in HIV/HCV-coinfection with CHC versus HCV-monoinfection and HIV/HCV-seropositive with cleared-HCV. Total CD4+HLADR+ expression was significantly increased in HIV/HCV-coinfection with CHC versus HIV-monoinfection and HIV/HCV-seropositive with cleared-HCV. Total CD4+CD38+ and CD4+CD38+HLADR- expression was significantly higher in HIV/HCV-seropositive with cleared-HCV than HCV-monoinfection and significantly higher in HIV-monoinfection than HCV-moninfection (Figure 1). Other potential predictors of CD4+ activation included elevated transaminases and other habits (Table 2). IL10 production was significantly lower in HIV-monoinfection versus HIV/HCV-coinfection with CHC (p=0.0002). No other differences in CD8+ immune activation markers, CD28, or cytokines across strata were detected.
Conclusions: In contrast to previously reported increased CD8 activation in poorly-controlled HIV, there were no differences in CD8 activation in our populations with undetectable HIV viremia. CD4 immune activation with HLADR+ expression in HIV/HCV-coinfection with well-controlled HIV may arise from chronic HCV viremia. Conversely, CD38+ expression in CD4 cells may be driven by underlying HIV infection in both HIV-monoinfection and HIV/HCV-coinfection.
Introduction
· Given shared modes of transmission, hepatitis C coinfection is common among HIV-positive patients
· Compared to patients with HCV monoinfection, coinfected patients have more rapid progression of liver disease
· Inflammatory cytokine responses and immune activation likely play a pivotal role in the immunopathology of HIV/HCV coinfection and liver fibrosis
· In poorly-controlled HIV with chronic hepatitis C (CHC), immune activation has been primarily attributed to CD8 T-cell subsets (Kovacs, et al)
· Patterns of immune activation in HIV/HCV-coinfected patients with well-controlled HIV have not been fully defined.

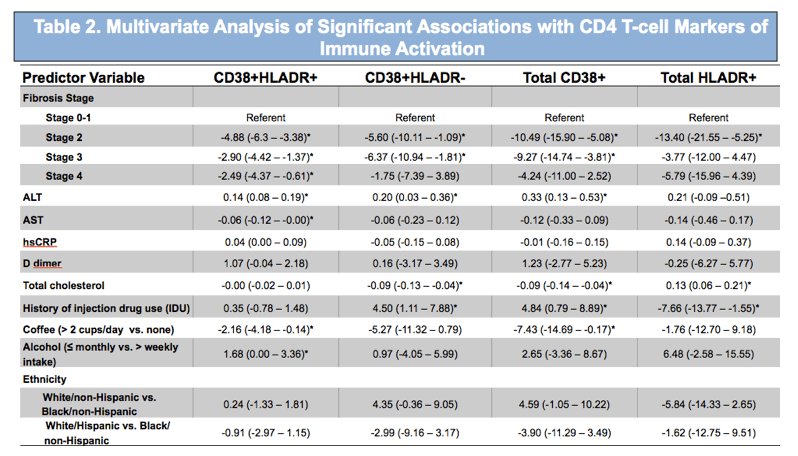
Values determined by Maximum Likelihood Estimates using Generalized Linear Model. Reported as estimates of mean difference (95% CI).
For categorical variables, the estimate is mean difference between two compared groups; for continuous variables, the estimate is mean difference
for one unit increment of independent variable
Abbreviations: hs-CRP, high sensitivity C-reactive protein; TE, transient elastography.
Strata was also included in multivariate model, though not reported here.
*P < 0.05
Study Limiations
· Small sample size as a pilot study
· Subjects with a sustained virologic response (SVR) following HCV treatment and subjects with spontaneously cleared HCV infection were analyzed as a singular strata
|
| |
|
 |
 |
|
|