 |
 |
 |
| |
National trends in hospitalization and mortality for patients with HIV, HCV, or HIV/HCV co-infection: HCV Hospitalization Rates Increasing
|
| |
| |
Reported by Jules Levin
IDSA
Oct 17-21 2012 San Diego
Oramasionwu C.U., Hunter J.M., Frei C.R.
Assistant Professor
University of North Carolina at Chapel Hill
UNC Eshelman School of Pharmacy
Division of Pharmaceutical Outcomes and Policy
Program Abstract:
Background: There have been many therapeutic advances for Human Immunodeficiency Virus (HIV) and hepatitis C virus (HCV) infections in the past two decades; however, few studies have evaluated trends in health care utilization for these patients over this time period. This study chronicled trends in hospitalization and mortality for HIV, HCV, and HIV/HCV co-infected patients.
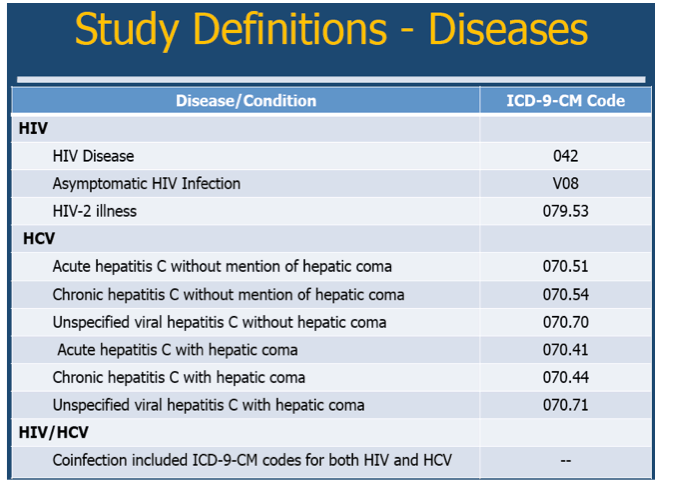
Methods: Data for this study were retrieved from the 1996-2010 National Hospital Discharge Surveys. Hospitalizations with primary or secondary ICD-9-CM codes for HIV or HCV were included. HIV mono-infection hospitalizations excluded HCV codes and HCV mono-infection hospitalizations excluded HIV codes. HIV/HCV co-infection included codes for both HIV and HCV. Patients <15 years of age were excluded. Demographic characteristics and select comorbidities were compared by infection status (HIV, HCV, HIV/HCV). Survey weights and U.S. Census Bureau estimates were incorporated to generate population-level estimates. The U.S. Standard Million Population 2000 age distribution was used to calculate age-adjusted mortality rates.
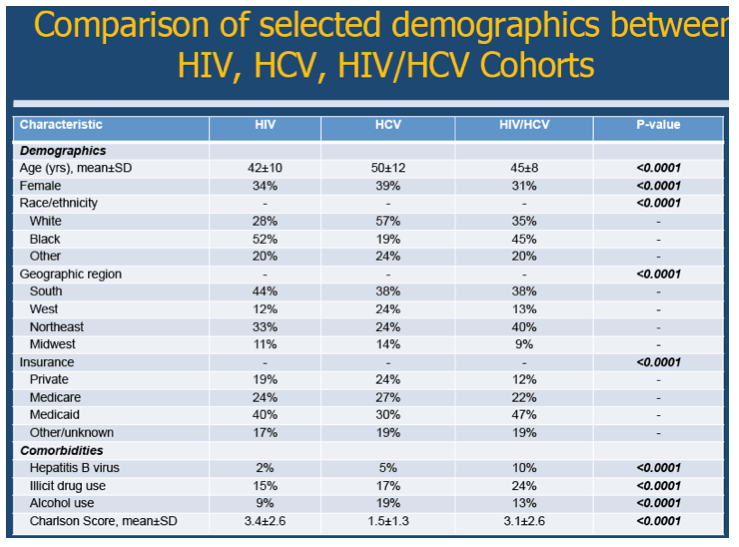
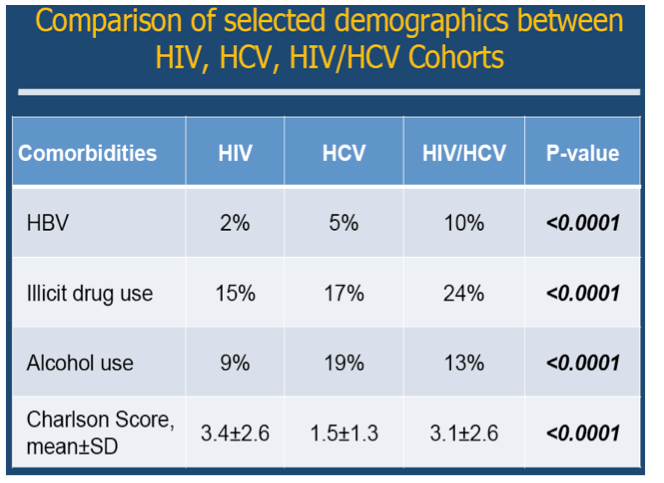
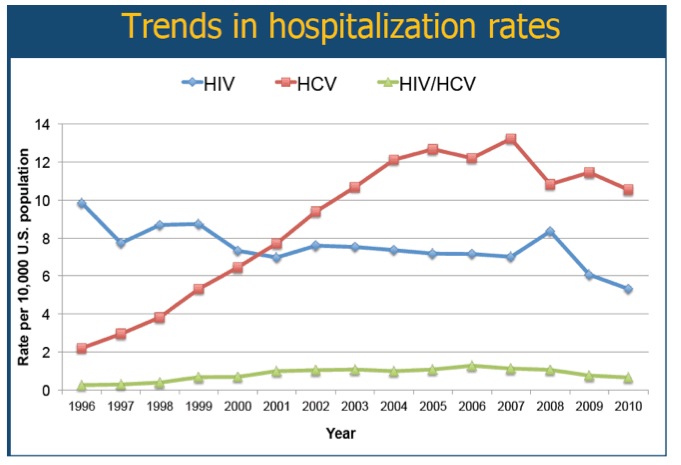
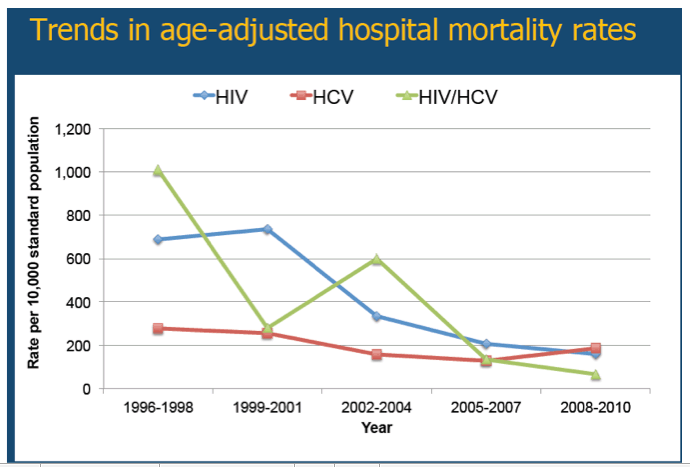
Results: Approximately 6.6 million hospitalizations occurred in patients with HIV (39%), HCV (56%), or HIV/HCV (5%). The HCV cohort, as compared to the HIV and HIV/HCV cohorts, was older in age and had a higher proportion of females. The following comorbidities varied significantly across the three cohorts (HIV, HCV, HIV/HCV): hepatitis B (2%, 5%, 10%), illicit drug use (15%, 17%, 24%), and alcohol use (9%, 19%, 13%) (p<0.001 for all variables). The hospitalization rate (per 100,000 population) decreased for the HIV cohort (9.9 in 1996; 5.3 in 2010). Conversely, the hospitalization rate increased greatly for the HCV cohort (2.2 in 1996; 10.5 in 2010) and increased slightly for the HIV/HCV cohort (0.3 in 1996; 0.7 in 2010). The age-adjusted mortality rates decreased for all three cohorts; however, the rate of decline was least pronounced in the HCV cohort.
Conclusion: The burden of inpatient health care utilization is increasing for patients with HCV, underscoring the need for further investigation and intervention in this patient population.





|
| |
|
 |
 |
|
|