 |
 |
 |
| |
Summary from CROI 2013 for Hepatitis Co-infection
HCV direct acting antivirals (DAAs) in HIV/HCV coinfection:
More drugs on their way. What are the implications?
|
| |
| |
Jurgen K. Rockstroh M.D., Professor of Medicine
University of Bonn, Germany
Introduction
The advent of the so called direct acting antivirals (DAAs) for treatment of hepatitis C infection have significantly changed HCV coinfection treatment guidelines and promise cure of HCV infection in around two thirds of treatment naïve HCV-genotype-1 infected patients with HIV-coinfection undergoing triple therapy with a HCV protease inhibitor together with pegylated interferon (PEG-IFN) and ribavirin (RBV). So far the number of treated patients in published studies however, has been small and limited to early stages of fibrosis. Therefore, this year CROI was eagerly awaited as it promised first data on triple therapy including either boceprevir or telaprevir in more challenging patient populations from real-world patient settings including previous non-responders to dual therapy as well as cirrhotics. Moreover, data on the use of new HCV protease inhibitors in clinical development in HIV/HCV coinfected individuals was presented allowing a first impression on the efficacy and safety of the next-wave HCV protease inhibitor which most likely will become available already in 2014. Finally, more and more data from trials in HCV mono-infected subjects were presented demonstrating that interferon-free regimens will become a very likely option even in more difficult-to-treat populations such as previous null-responders. The current development of HCV compounds occurs at a very fast rate and promises a more than exciting future with potentially very high cure rates in almost all patient populations. One of the big remaining questions though is how will the high costs of these drugs be covered and how will access to these new treatment options roll-out throughout the world
Efficacy and safety of telaprevir or boceprevir in HIV/HCV coinfection
New data on efficacy and safety of telaprevir or boceprevir in HIV/HCV coinfected previous non-responders to HCV therapy
In the oral hepatitis session two ANRS studies were presented which looked at the efficacy and safety of triple HCV therapy (wither with telaprevir or boceprevir) in previous non-responders to dual PEG-IFN/RBV therapy (1,2). Patients with previous null-response and cirrhosis however, were excluded because of the overall low probability of treatment response. Both studies were presented as preplanned interim analyses at week 16 of therapy. In the telaprevir ANRS HC26 study in the interim analyses overall 69 patients who received at least one dosage were included (1). Background HIV therapy contained ATV, ATV/r, EFV, RAL, TDF, FTC, or 3TC. The study design is depicted below (figure 1):
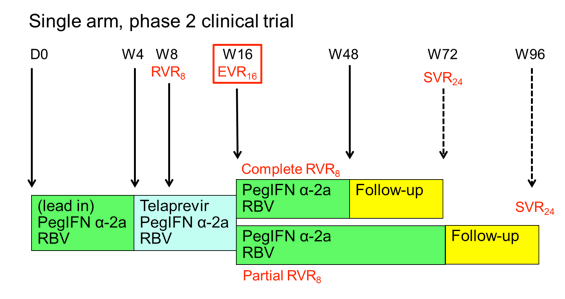
Patients started with a 4 week lead-in of PEG-IFN/RBV. This approach, which is outside the labelling of telaprevir, was chosen to be able to compare the results to the study design wise similar boceprevir study and because data from telaprevir studies in HCV mono-infection in treatment experienced patients had potentially promised some benefit for this approach. After week 4 telaprevir was added for 12 weeks. Patients who achieved a complete rapid virological response at week 8 (RVR8) defined as HCV-RNA <15 IU/mL received 32 weeks of PEG-IFN/RBV after stopping telaprevir at week 16 after 12 weeks of triple therapy (full treatment: 48 weeks). Whereas patients who only obtained a partial RVR8 (15 IU/mL < HCV-RNA < 1000 IU/mL) received an additional 56 weeks of PEG-IFN/RBV (full treatment: 72 weeks). Telaprevir was administered as 750 mg q8h (1125 mg q8h with Efavirenz) and Peg-IFN α-2a as 180 μg sc / week. Ribavirin was dosed as 1000 mg / day (≤75 kg) and 1200 mg /day (>75 kg). EPO, G-CSF, and TPO-R agonists were allowed within the study. Futility rules for telaprevir were HCV-RNA > 1000 IU/mL at week 8 or week 12 or virological breakthrough at any time. For study inclusion patients needed to have CD4 ≥ 200 cells/mm³ and ≥ 15%, as well as plasma HIV-RNA levels < 50 copies/mL At baseline median CD4-count was 630 cells/mm³ (range 459-736) and HIV-RNA was below 50 copies in 99% of patients. Interestingly, 11 (18%) patients had F3 fibrosis and 16 (23%) F4 fibrosis upon inclusion to the study, allowing studying safety and efficacy of telaprevir based triple therapy in this more difficult-to-treat patient population. 39% of patients were previous relapsers to dual therapy, 9% had previous viral breakthrough, 22% were partial responders and 30% null-responders. The week 16 efficacy results in a ITT-analyses are presented below:
Figure 2: Results: Telaprevir + PegIFN + RBV in HIV/HCV co-infected patients with virologic failure on IFN +RBV: virologic response
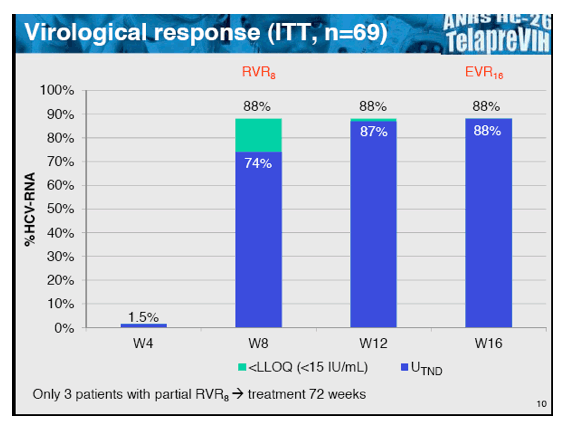
< LLOQ=under the limit of quantification, U= target not detected
With 88% being HCV-RNA negative at week 16 in this patient population with 30% previous null-responders and 40% F3/F4 fibrosis this study showed surprising high early efficacy results. Most interestingly efficacy remained high throughout all sub analyses including sub analyses according to previous dual therapy response (EVR16 was 86% in relapsers versus 86% in previous null-responders) as well as according to baseline fibrosis stage (EVR16 was 92% in F1 and 94% in F4 patients. Concomitant ART also had no impact on early virological response. Adverse events were frequent (99% of patients developed an AE) but were mostly related to IFN side effects. 4% (n=3) of patients discontinued study drugs because of psychiatric adverse events and cutaneous adverse events, respectively. Noteworthy, in contrast to the pilot trial in HCV treatment-naïve patients where no telaprevir discontinuation because of rash was recorded a few discontinuations because of rash did occur in this study. Grade 3-4 anemia, EPO use, transfusion or RBV dose reduction was recorded in 61% of patients. The authors concluded that significant hematological toxicity was observed, despite a proactive management of anemia. This is very well in line with results from the CUPIC trial (a trial in HCV monoinfection in patients with CHILD A cirrhosis which also had reported higher anemia rate in this liver disease wise more advanced patient population).
CROI: High Early Virological Response with Telaprevir-PegIFN-RBV in treatment-experienced, HCV genotype 1, HIV coinfected patients: ANRS HC26 TelapreVIH Study - (03/08/13)
The second ANRS study looked at the efficacy and safety of a boceprevir containing triple therapy again in 64 previous IFN/RBV non-responders (2). The study design is depicted below:
Figure 3: Study design: Multi-center single arm open label Phase 2 Trial
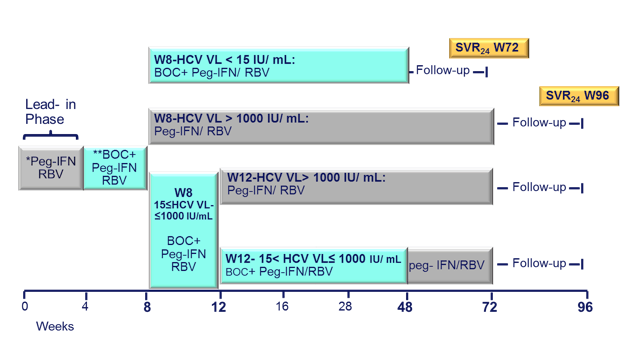
Following a lead-in with dual therapy boceprevir was added at week 4. Complex futility rules were in place during the study warranting discontinuation of boceprevir in all patients with a HCV viral load above 1000 IU/ml at week 8 as well as in week 12. All HCV drugs were discontinued if HCV viral load was >1000 IU/ml at week 16 or still detectable at week 28 and in case of virological breakthrough. Duration of therapy was dependent on initial response as shown above. Patients who achieved a rapid virological response and had an HCV-RNA <15 IU/ml at week 8 were treated for 48 weeks, patients with slower decline in HCV RNA were treated for 72 weeks. Patients recruited for the trial had to be on stable ART for at least 3 months, with at least three molecules among ATV (rtv boosted or not), RAL, TDF, ABC, FTC, or 3TC. Again only previous non-responders to dual therapy with HCV genotype 1 infection were included. Null-responders with cirrhosis were excluded from this trial. Overall, 17% of patients at baseline had F4 fibrosis, 33% were previous null-responders. Only patients who received ≥ 1 dose of treatment Interim week were included into this first interim week 16 efficacy analyses. The corresponding response rate (Patients (%) with HCV-RNA < 15UI/ mLs ) are depicted below:
Figure 4: HCV- Virological response: Patients (%) with HCV-RNA < 15UI/ mL
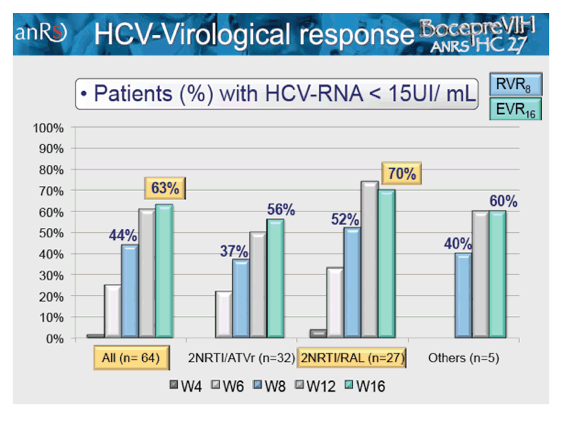
Overall 63% achieved undetectability at week 16, which was slightly higher in the raltegravir treated patients than in patients on other ART regimens. Response rates at week 16 were best for previous relapsers (with 90% < 15 IU/ml) versus patients with previous breakthrough (60% < 15 IU/ml), partial responders (60% < 15 IU/ml) and null-responders (38% < 15 IU/ml), respectively. Response rates according to fibrosis at baseline in contrast were comparable between the different fibrosis stages (62% < 15 IU/ml at week 16 with F1, 67% for F2, 50% for F3 and 73% for F4). Clearly the overall small number of study subjects limits the strength of the comparisons but again the impression is that even patients with more advanced fibrosis seem to respond well to HCV triple therapy containing boceprevir. The safety data again suggests higher haematological adverse events than in the treatment naïve patient population with less fibrosis. Anemia occurred in 42% of patients but only 5% developed grade 3-4 anemia. 42% of patients received concomitant EPO.
CROI: ANRS-HC27 BocepreVIH Interim Analysis: High EVR with Boceprevir+peg-IFN+ RBV in HCV/HIV-co-infected Patients with Previous Failure to peg-IFN+RBV - (03/08/13)
In summary, these first two studies in previous non-responders to dual therapy with PEG-IFN/RBV and a considerable proportion of patients with more advanced fibrosis stages demonstrates very high early response rates in this more challenging to treat patient population. This should remind us not to postpone HCV therapy for all in hope of easier and less toxic HCV treatment regimens in the future but also to at least consider the improved treatment options we already have in our hands which preferably should be used in those patients where risk for development of HCC or progression to cirrhosis and eventually hepatic decompensation is a real threat.
New data on use of telaprevir and boceprevir in the clinics outside of clinical trials
In addition to the ANRS presentations first results from the use of boceprevir and telaprevir from hepatitis clinics in Spain, Italy and the US were presented (3). In this multi-center study all individuals who initiated triple therapy with telaprevir (TLV) or boceprevir (BOC) outside clinical trials were evaluated. The influence of demographics, baseline HCV RNA, HCV-1 subtype, HIV co-infection, liver fibrosis, and IL28B alleles on early viral kinetics was assessed using univariate and multivariate analyses. Rapid virological response (RVR) was defined as undetectable HCV RNA at week 4 for TLV and at week 8 for BOC (4 weeks after lead-in). In the poster presentation, 98 individuals were evaluated, 32 treated with BOC, and 66 with TLV. Mean age, gender, body mass index, baseline HCV RNA, HCV subtype 1b, IL28B-CC alleles, HIV co-infection , and prior pegylated interferon+ribavirin did not differ comparing BOC and TLV groups. RVR was achieved by 88% on TLV vs 59% on BOC (p <0.0001). HCV RNA decay during the first 4 weeks of triple therapy was lower in BOC than TLV groups. A multivariate logistic regression analysis (OR [95% confidence interval (CI)]; p) confirmed that TLV use was the strongest predictor of RVR (4.82 [1.7-13.7]; p<0.003). Another independent predictors of RVR was HCV subtype 1b (2.43 [0.9-6.8]; 0.09). Previous IFN experience versus naive (0.81 [0.2-2.9], p=0.7), did not influence the chances of RVR. The authors conclude that telaprevir may be more efficacious in obtaining RVR. However, as boceprevir is given longer response rates may continue to increase over time in the end potentially resulting in comparable SVR rates despite higher RVR with telaprevir as seen in the naïve boceprevir coinfection pilot trial. Therefore, the only conclusion possible is that telaprevir is associated with a more significant HCV-RNA decline over the first 4 weeks but whether this translates into higher cure rates cannot be concluded from this data.
In a further US study virologic responses to and side effects of telaprevir-based therapy in HIV/HCV co- infected patients vs. HCV mono-infected patients in a real-life setting were compared (4). Overall, 33 HIV/HCV coinfected patients and 117 HCV monoinfected patients were included.
Interestingly, the SVR12 rate was higher in the co-infected patients. As the number studied is small further studies are needed to rigorously establish the SVR rate of triple therapy for co- infected patients. Nevertheless at least there was no signal of worse response due to HIV infection. With regard to safety telaprevir was associated with numerous adverse events, but there were not significantly more events in the co- than in the mono-infected population.
Important new PK interaction data with telaprevir and boceprevir.
In the oral hepatitis session there was a very interesting presentation on the possible changes in plasma and intracellular ribavirin concentrations under telaprevir therapy (5). RBV pharmacokinetics (PK) were determined in an ongoing study of hepatitis C virus (HCV)-infected, genotype 1, treatment naive subjects receiving TVR+PR or PR alone. RBV dosing was weight based (1 vs 1.2 g once daily [QD]). Subjects underwent 12-hour intensive PK sampling for RBV at SS (weeks 9-14) following observed dosing in the fasted state. RBV in plasma was measured using a validated HPLC-UV assay and RBV mono- (RMP), di (RDP), and triphosphate (RTP) in PBMC and RBC were measured using a validated LC/MS/MS assay. Dose (mg/kg) adjusted RBV plasma area under the concentration time curve (AUC0-12) and RMP, RDP, and RTP in PBMC and RBC were compared (unpaired t-tests) in those receiving TVR+PR vs PR alone. Most surprisingly, RBV plasma AUC 0-12 and RMP, RDP, and RTP in PBMC and RBC were significantly higher in those receiving TVR+PR vs PR alone. This potentially could explain the high anemia rates seen under telaprevir therapy particularly in patients with more advanced fibrosis. The exact underlying mechanism of this observation remains unknown but several explanations were offered in the talk. One hypothesis is that due to the need of taking telaprevir with 20g fat higher levels could derive from the food effect upon ribavirin intake. Obviously a fatty meal can increase ribavirin AUC by 67%. Another theory was pgp interaction. Overall, this means that ribavirin reductions in case of anemia under telaprevir based therapy makes a lot of clinical sense.
Another important pk study looked at possible drug-drug interactions between boceprevir and rilpivirine (6). As efavirenz significantly lowers boceprevir exposure by around 50% the concomitant HIV treatment with NNRTIs and boceprevir has been limited. So far no study has evaluated the possible interactions between rilpivirine and boceprevir. This study was a single-center, fixed-sequence, 3-period, open-label, drug-interaction study in 20 healthy adult subjects. In period 1, subjects received BOC 800 mg three times daily on days 1 to 6 with the last dose administered on the morning of day 6, followed by a 7-day washout. In period 2, subjects received RPV 25 mg once daily on days 1 to 11 followed immediately by period 3, in which subjects received concomitant BOC 800 mg three times daily and RPV 25 mg once daily on days 1 through 11. Blood samples were collected for BOC and RPV pharmacokinetics (PK) in each period. RPV and BOC co-administration increased RPV exposures but not to a clinically significant extent. The GMR (90%CI) for RPV AUC0-24h, Cmax, and C24h were 1.39 (1.27, 1.52), 1.15 (1.04, 1.28), and 1.51 (1.36, 1.68). BOC PK was not affected by co-administration of RPV. Therefore these data suggest that boceprevir and rilpivirine can be coadministered without need for dose adjustments.
Use of telaprevir for treatment of acute hepatitis C in HIV-coinfected individuals.
Currently, according to the consensus guidelines, treatment of acute HCV in HIV is recommended as dual therapy with PEG-IFN/RBV for 24 weeks if early negative HCV-RNA values are obtained after 4 weeks of treatment (RVR) (7). At this year CROI first uncontrolled data was presented for the use of triple therapy in treatment of acute HCV among HIV-coinfected subjects with shortened treatment duration of only 12 weeks (8). This was a small study where HIV-infected MSM with acute HCV, who were referred from clinicians throughout NYC to Dr. Fierer, would receive 12 weeks of telaprevir (750 mg every 8 hrs) in combination with Peginterferon 2a and weight based RBV, with the standard stopping rule of >1000 IU/mL at week 4. Not all referred patients were treated because of cost reimbursement issues or other reasons. There was an unusual high rate of IL2b CC genotype distributiuon (65%) in his cohort which raised the question whether the population was enriched with individuals who per se had a higher likelihood of spontaneous clearance. Nevertheless, overall response was good with 85% of patients (17/20) achieving early treatment response and all of them (17/20) also achieving SVR4. For those patients where longer follow-up was available 11/14 (79%) achieved SVR at 24 weeks. Clearly this data demonstrates that shortened treatment durations of 12 week of telaprevir based triple therapy will work for the majority of patients with acute HCV, however it will not lead to cure in all. Also taken into account increased toxicity risk and cost increase it remains unclear whether this will become a generally recommended strategy. Clearly, prospective and controlled data from a randomized clinical trial are needed to answer this appropriately.
CROI: Treatment of Acute HCV in HIV-infected MSM Incorporating Telaprevir - (03/13/13)
Second-wave HCV protease inhibitors in HIV/HCV coinfection: first efficacy and safety results
The next exciting presentations were around the use of 2nd wave HCV protease inhibitors in combination with PEG-IFN/RBV in HCV coinfected HIV-patients. Obviously the new HCV PIs which can be administered once daily and appear to have a more favorable adverse event profile promise a simplified and potentially better tolerated HCV therapy for coinfected subjects. In addition these new compounds show considerable genotype 4 activity promising also potentially new treatment options for this increasing group of patients.
The first study around the BI HCV protease inhibitor was a pharmacokinetic interaction study of darunavir/ritonavir, efavirenz, and tenofovir with the HCV protease inhibitor faldaprevir (FDV) in healthy volunteers (9).
Co-administration with FDV led to small increases in exposure (AUC) of DRV/r (↑15%) and TFV (↑ 22%) compared with the ARVs given alone. These small increases were not considered to be clinically relevant. Looking the other way around FDV AUC increased by 130% with DRV/r, but decreased by 22% with TFV, and decreased by 35% with EFV. The decrease in FDV exposure with EFV was attributed to a CYP3A4 induction. As a consequence, in the subsequently presented FDV study in HIV/HCV coinfection, patients on efavirenz were allocated to the higher dose of FDV which was being studied (240mg QD) whereas patients on darunavir/r received the lower FDV dose (120mg QD).
The study design of the FDV coinfection study is depicted below (10):
Figure 5: Phase III open-label, sponsor-blinded study in treatment-naïve and relapser patients with chronic HCV GT-1 and HIV infection
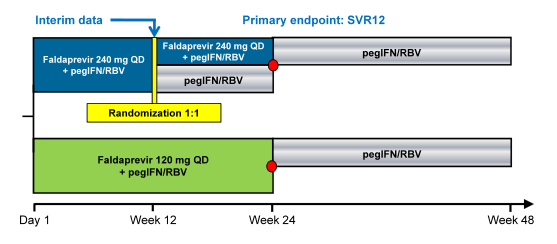
The red dot resembles patients with HCV RNA below LLoQ, at Week 4, and HCV RNA below LLoQ target not detected at Week 8 (=ETS) which were re-randomized 1:1 at week 24 to stop treatment or continue pegIFN/RBV through week 48. Patients who did not achieve ETS had to continue pegIFN/RBV through week 48. Therefore, this is the first coinfection study to address the possibility of RVR guided shorter treatment durations. Patients with no ART or on maraviroc or Raltegravir were randomized to 120 or 240mg FDV QD, respectively. Because of the previously described pk-interactions (see above) patients on efavirenz were allocated to 240mg QD and patients on darunavir/ritonavir or atazanavir/ritonavir based ART to 120mg FDV QD.
Importantly the study also allowed the inclusion of patients with liver cirrhosis allowing to gain some efficacy and safety data in this more difficult to treat patient population. Overall 304 (239 treatment naïve and 69 relapsers) patients were included making this the largest coinfection DAA study so far. Importantly, 17% of patients included had F4 fibrosis, 78% GT1a and baseline HCV RNA was ≥800 000 IU/mL in 80% of patients. Early virologic response in HIV/HCV co-infected patients is shown in figure 6.
Figure 6: Early virologic response in HIV/HCV co-infected patients: HCV treatment-naïve and relapsers
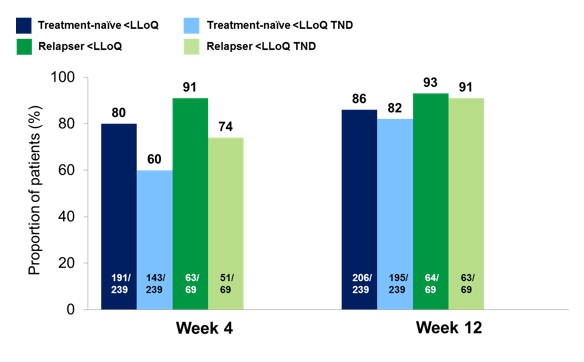
Early virological treatment response was excellent in naïve as well as in previous relapsers. Early ETS was observed in 80% of patients and half of these patients will stop treatment at Week 24 which will provide very interesting data on potentially shorter treatment durations in HIV/HCV coinfecetd subjects for the first time in the near future. AEs were comparable to those with faldaprevir and pegIFN/RBV in HCV mono-infected patients. 18% of patients developed anemia and 18% rash. 2 rashes were documented as SAEs.
In summary, very high early treatment response rates have been observed under triple therapy with feldaprevir. Indeed 80% of patients achieved HCV RNA below the level of quantification at week 4 and complete undetectability at week 8 allowing for entering the randomized second part of the study looking at 24 vs 48 weeks of treatment.
CROI: STARTVerso 4: High rates of early virologic response in HCV genotype 1/HIV-co-infected patients treated with faldaprevir plus pegIFN and RBV - (03/04/13)
CROI: Pharmacokinetic interactions of darunavir/ritonavir, efavirenz, and tenofovir with the HCV protease inhibitor faldaprevir in healthy volunteers - (03/04/13)
The other second wave HCV protease inhibitor study evaluated efficacy and safety of simeprevir based triple therapy in HIV/HCV coinfection in study C212. C212 is a phase III, open-label, single-arm, international trial assessing simeprevir (150 mg QD) plus pegIFN/RBV in treatment-naive and -experienced patients (N=106) co-infected with genotype-1 HCV and HIV-1 (11). Patients who were treatment-naïve and non-cirrhotic (n = 50) or prior relapsers (n = 14) received a response-guided treatment (RGT) regimen of simeprevir (150 mg once daily) for 12 weeks plus PR for 24 or 48 weeks. Prior partial (n = 10) or null (n = 28) responders and patients with cirrhosis (3 treatment-naïve patients and 1 relapser) received treatment for 48 weeks. The study design of the study is shown in figure 7.
Figure 7: C212 Study design
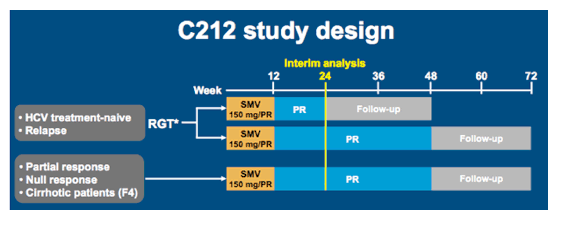
Primary endpoint of the study was SVR12, safety, and tolerability. Secondary endpoints: virologic response at other time points, on-treatment failure, and relapse rates. For the interim analysis all patients were included which had completed 24 weeks of treatment or had discontinued prior to that point. No. of patients: Week 24: N=100, Week 28: N=71 and Week 36: N=27.
Patients were either receiving HAART (abacavir [ABC], tenofovir [TDF], stavudine [3TC], emtricitabine [FTC], rilpivirine (RPV), raltegravir [RAL], maraviroc [MVC], or enfuvirtide [ENF]) or not receiving HAART. 12% of patients at baseline had F3 fibrosis and 9% F4. The efficacy results are shown in figure 8.
Figure 8: Virologic response of patients treated with SMV/PR at Week 4 (RVR)
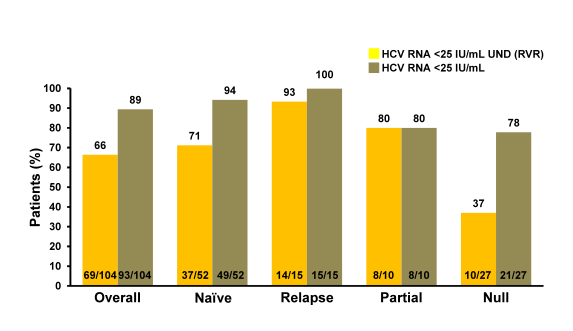
Simeprevir 150 mg QD + pegIFN/RBV led to high virologic response rates in co-infected patients, regardless of prior response (SVR12 77% in treatment-naïve and prior relapsers). Relapse occurred only in patients infected with HCV genotype-1a: 5/31 overall population; 3/22 treatment-naive; 2/9 prior relapsers. 64% of all prior null responders had not experienced failure at the time of the interim analysis. Of 88% of patients who met RVR 75% achieved SVR 12.
30% of patients developed grade 3 or 4 events. A rash was reported for 17% of patients. Hyperbilirubinemia (a known side effect of simeprevir was noted in 5% of study subjects. Only 4% of patients discontinued simeprevir because of adverse events. Overall, Simeprevir was well tolerated, with a safety profile similar to HCV mono-infected patients.
In conclusion the two second wave HCV protease inhibitor studies with simeprevir and feldaprevir respectively, demonstrate that in the very near future (2014) new HCV protease inhibitors will become available which will offer once daily dosing, improved tolerability profile and most importantly shortened treatment duration at least for those patients who achieve RVR. Also the drug interaction profile is different and at least with feldaprevir the combination with boosted darunavir is possible.
CROI: Simeprevir (TMC435) with peginterferon/ribavirin in patients co-infected with chronic genotype-1 HCV and HIV-1: Week-24 interim analysis of the TMC435-C212 study - (03/07/13)
New data on interferon-free HCV treatment approaches in HCV monoinfection
Clearly, the ultimate goal in treatment of hepatitis C in HCV monoinfected just as well as in HIV coinfected subjects is to develop interferon-free DAA regimens which allow cure in the majority of patients and because of less toxicity and shorter treatment durations will revolutionize HCV management within the next years. Nevertheless, despite numerous studies demonstrating good efficacy for the first interferon-free studies which were performed it also became clear that success rates may be more difficult to achieve in former non-responders to dual therapy and patients with advanced liver fibrosis. At last year CROI excellent response rates had been reported for the treatment of HCV monoinfected, treatment-naïve GT1 patients under the all oral combination of sofosbuvir and ribavirin for 12 weeks (12). In contrast SVR12 in HCV patients with previous non-response was only 10% in patients receiving the same combination of sofosbuvir and ribavirin. Obviously, there are at least two straight forward ways of potentially improving response rates. One could be to prolong treatment duration and the other to increase potency of the regimen by adding a further DAA to the therapy. Indeed at this year CROI a study looking at the efficacy of the newly developed fix-dose combination tablet sofosbuvir and ledipasvir (a NS5a-inhibitor) in combination with ribavirin for 12 weeks was studied again in HCV treatment naïve GT1 patients (n= 25) as well as in previous null-responder (n= 9) also with HCV GT1 infection (13). The corresponding results from last years and this year's study are summarized in Table 1:
Table 1: ELECTRON study results: Patients with HCV RNA < LOD* Over Time, n/N (%)
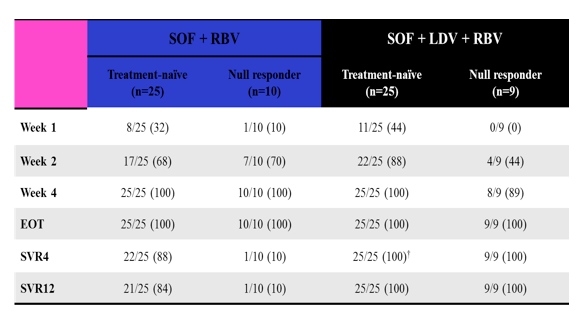
Although the number of studied subjects is small it does clearly show that the addition of a second DAA in previous null-responders dramatically improves HCV cure rates. Since cirrhotics were not included into this study it remains unclear whether cirrhotic null responders would also respond to this combination therapy as the most difficult group of patients to treat overall. The overall safety data once again was very impressive with far less hematological adverse events as well as no treatment limiting CNS toxicity in this interferon free approach. Indeed there was no grade 4 lab abnormalities recorded during the study and only one patient stopped all treatment because of an adverse event at week 8 at time of partial colectomy for diverticular perforation. Clearly this will be the major advantage of IFN-sparing regimens which will not cause treatment-related depression and have no major impact on platelets or white blood cell count. As long as ribavirin remains in the equation, risk for anemia persists however, but with much lower severity than observed in the first HCV protease inhibitor based triple therapies.
CROI: ELECTRON: 100% SVR Rate for Once-Daily Sofosbuvir Plus Ledipasvir Plus Ribavirin Given for 12 Weeks in Treatment-Naïve and Previously Treated Patients With HCV GT 1 - (03/04/13)
Obviously if combinations of DAAs become potent enough there may even be a chance to obtain high cure rates in the absence of additional ribavirin therapy. Indeed at this year CROI results from the COSMOS trial were presented which evaluated an once-daily regimen of simeprevir (TMC435) plus sofosbuvir (GS-7977) with or without ribavirin in HCV monoinfected genotype 1 null-responders (14). An interim analysis of Cohort 1(Cohort 1: n=80 patients randomized 2:1:2:1) was conducted when all patients in 12-week treatment arms (arms 3 and 4) reached SVR4 time point or discontinued early. The study design is depicted below in figure 9.
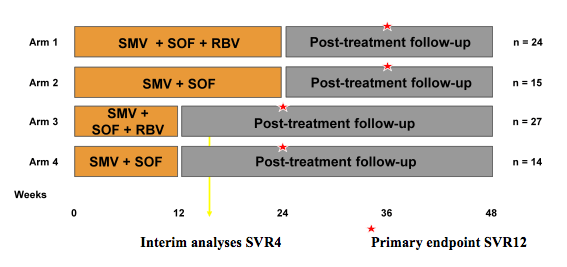
Within the study only prior null-responders were included. Prior null response to PegIFN/RBV was defined as a failure to achieve >2 log10 decline in HCV RNA by Week 12. Liver biopsy had to be performed or available from the last 3 years consistent with HCV and demonstrating METAVIR F0-F2 fibrosis in order to be enrolled into the study. Indeed at baseline 59% were classified as F2, and 41% as F0-1. IL28b genotype was unfavorable in most patients with IL28CT in 70% of patients and IL28bTT in 24%.
The main result of the study was that 12 weeks of SMV + SOF led to an SVR8 rate of 96% with RBV and 93% without RBV. RVR rates were however, higher in presence of ribavirin. No viral breakthrough was observed and similar SVR rates were obtained in GT 1a and 1b patients. More detailed results are summarized in table 2.
Table 2: Efficacy results from the COSMOS trial
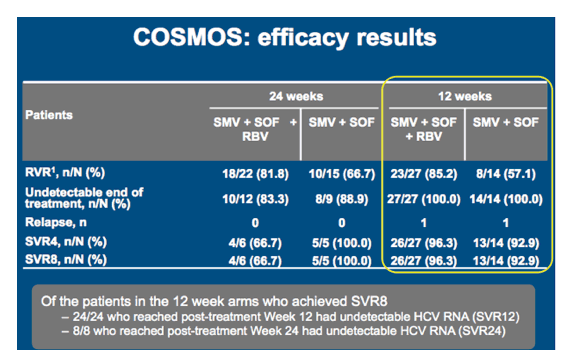
From a safety perspective SMV + SOF with/without RBV was generally well tolerated. Anemia was seen only in RBV arms. Infrequent (5%) grade 3/4 bilirubin increases, which are consistent with the known inhibitory effects of SMV on OATP1B1/MRP2 were observed within the trial. Interestingly, bilirubin increases only occurred in RBV containing arms.
The findings of the trial are important as obviously there are patient groups such as dialyses patients where ribavirin therapy has been extremely difficult if not impossible and so developing ribavirin free IFN-sparing approaches for renally impaired patients as well as anemic patients would be of great clinical importance.
CROI: SVR4 results of a once daily regimen of simeprevir (TMC435) plus sofosbuvir (GS-7977) with or without ribavirin in HCV genotype 1 null responders - (03/06/13)
A further study on sofosbuvir was presented at the oral coinfection session which investigated the efficacy of sofosbuvir with weight-based ribavirin for 24 Weeks in difficult-to-treat Patients (15). In this study 60 HCV monoinfected GT-1, treatment naïve subjects were enrolled in 2 parts. In part 1 of this study, 10 subjects with stage 0-2 liver fibrosis were treated with SOF 400 mg once daily and weight based RBV (1000 mg if <75 kg or 1200 mg if >75kg). Part 2 randomized 50 subjects with stage 0-4 fibrosis to receive SOF 400 mg once daily with either low (600 mg once daily) or weight based RBV. Treatment duration was 24 weeks. Subjects were predominantly black (83%), male (62%), IL28 CT/TT genotype (80%) with GT-1A infection (70%). 48% had a BMI >30, 23% had advanced liver disease, and 62% had HCV VL >800,000 IU/mL. So clearly, the study population was characterized by many independently demonstrated negative prediction factors to HCV therapy. Virologic decline however, was rapid with a median decline of 4.14 log10 IU/mL by day 7. Treatment response in the first 10 patients from part 1 was very favorable with all patients achieving cure of HCV (100% SVR24). In part 2 while ETR was 100% among subjects that completed treatment, 10 (45%) and 7 (29%) subjects on low and weight based RBV respectively relapsed by 12 weeks post-treatment completion. Relapse was associated with low ribavirin dose, male gender and high HCV-RNA levels. In conclusion in an inner-city population of HCV monoinfected GT1 patients with negative treatment predictive factors an IFN-sparing regimen with sofosbuvir and weight adapted ribavirin was effective in achieving high SVR rates. Lowering the ribavirin doses may lead to increased risk for relapse. (from Jules: harder-to-treat patients, cirrhotic null-responders will need the most potent therapy and this will be available, may need 3 or perhaps 4 potent oral HCV drugs or orals + Peginterferon [PegLambda], Rbv).
CROI: High Efficacy of Sofosbuvir in Combination with Weight Based Ribavirin for 24 weeks in Difficult to Treat HCV Infected Genotype-1 Patients - (03/06/13)
The AVIATOR Study and more
The next set of exciting interferon-sparing regimens was presented from AbbVie which aimed at identifying the optimal treatment duration for minimizing risk of virological relapse (16). The study population included treatment-naïve patients and prior pegIFN/RBV null responders which had been randomized within the AVIATOR study to ABT-450/r (HCV NS3/4A protease inhibitor co-administered with ritonavir once daily) + ABT-267 (NS5A inhibitor dosed once daily) + ABT-333 (non-nucleoside polymerase inhibitor dosed twice daily) + RBV for 8, 12, or 24 weeks, with final on-treatment HCV RNA value < LLOQ and at least one post-treatment HCV RNA value available. The study design of the treatment arms included into the study are depicted below in figure 10 (overall study population n=321).
Figure 10: Treatment arms included into the analyses

Treatment duration was highly significantly associated with relapse (p = 0.001, lower relapse with longer duration). Baseline HCV RNA and HCV sub-genotype were also marginally associated with relapse: Higher relapse rates with higher baseline HCV RNA (p = 0.1) and higher relapse rates with genotype 1a (p = 0.1). In contrast no association was found between
IL28B genotype (CC vs. non-CC) and relapse (p = 0.5). A further analyses looks at time of relapse (see Table 3).
Table 3: Time of relapse in the study
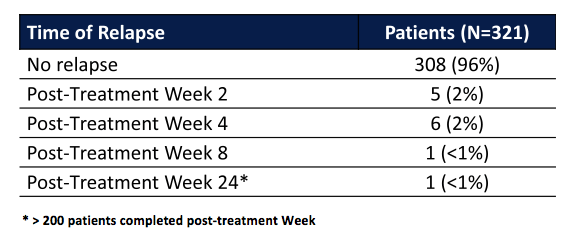
Interestingly, there were some rather unusual late relapses suggesting that in interferon-free regimens we may see different relapse time points than under interferon containing regimens. Clearly close monitoring and follow-up will be needed with expanded use of new DAAs to better understand risks around possible late relapse in a given HCV patient undergoing HCV therapy. In conclusion, for the drug regimen studied, 12-week treatment duration appeared to be optimal across treatment-naïve patients and prior null responders. Durations < 12 weeks were associated with an increasing risk of relapse whereas durations > 12 weeks did not further reduce risk of relapse. This enhances that in the future on average HCV therapy will most likely be in the range of 12 weeks which obviously will also help to improve uptake of HCV therapy as many patients are scared about the length of current HCV treatment strategies.
In a further study the 48 week follow-up data from the first studies of
ABT-450/r + a non-nucleoside polymerase inhibitor without interferon in HCV monoinfected GT1-infected patients were presented (17). Clearly response rates of the previous study with 3 DAAs (one boosted with ritonavir) in combination with ribavirin was very high. The question though is whether a reduced number of DAAs would work just as well in distinct HCV patient populations allowing potentially cost and pill burden reduction as well as a reduction in therapy associated adverse events. The corresponding study design is depicted below in figure 11.
Figure 11: Study design
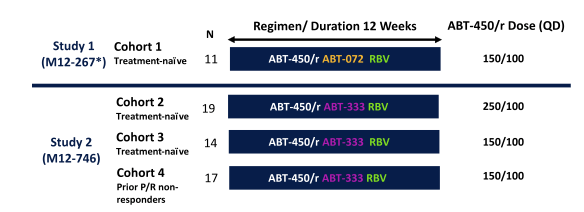
*Enrollment was limited to patients with the IL28B SNP rs12979860 CC genotype
The study included treatment-naïve (never received previous HCV treatment (Cohorts 1, 2, 3), previous non-responders to pegIFN/RBV per protocol (Cohort 4; defined as: failure to achieve 2 log10 HCV RNA decrease by week 12 (null responder), or failure to achieve HCV RNA below the limit of detection at the end of treatment (partial responder). Figure 12 summarizes the efficacy results. Patients received ABT-450/r and either ABT-072 400mg QD or ABT-333 400mg BID as well as RBV weight-based 1000-1200 mg daily dose divided BID. All Patients were followed through 48 weeks post-treatment. The efficacy results for the various study arms is shown below in figure 12.
Figure 12: Virologic Efficacy Rates by Arm
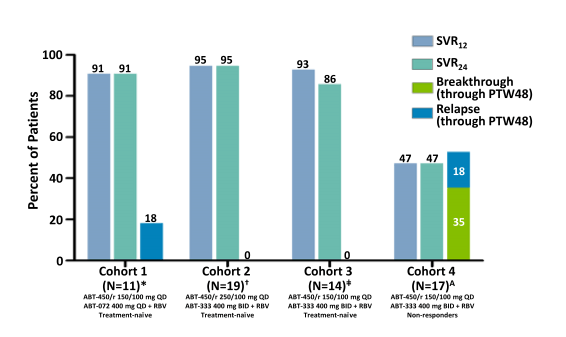
*10 patients with data through PTW48, 18 patients with data through PTW48, ≠11 patients with data through PTW48, 17 patients with data through PTW48
Among treatment-naïve HCV genotype 1 patients no virologic breakthroughs on treatment were seen. One patient relapsed at PTW8 and a second relapsed at PTW36. Overall, SVR24 rates were 86-95%, including 100% (18 of 18) of IL28B T allele patients. ABT-450/r 250/100 mg and 150/100 mg doses showed comparable response rates. Among previous P/R non-responders only 47% achieved SVR24. All patients who relapsed did so by their first post-treatment visit. In these studies relapse after PTW12 was very uncommon.
With regard to the safety data, no deaths or serious adverse events were documented in the trial. Only one adverse event led to premature discontinuation in Cohort 2. This event was an isolated ALT and AST elevation at week 2 (maximum ALT = 308 U/L, Grade 3). The patient was asymptomatic and no associated bilirubin increase was observed. ALT and AST improved promptly after study drug discontinuation. Four patients with adverse events were assessed as severe, none however, requiring study drug interruption or discontinuation. In one case hyperbilirubinemia maximum 6.2 mg/dL [106 mmol/L]), predominantly indirect bilirubin, was documented and which eventually led to RBV dose reduction. Transient asymptomatic elevation of indirect bilirubin was seen throughout the trial and is considered to be consistent with the known effect of ABT-450 on the bilirubin transporter OATP1B1.The other adverse events were fatigue, pain and vomiting, respectively.
In conclusion these data demonstrate that there may be a potential for different HCV treatment strategies in more or less challenging to treat patient populations. So whereas HCV treatment naïve patients with GT 1 do very well with the combination of ABT-450/r + non-nucleoside polymerase inhibitor, further combination partners may be needed for obtaining equally high success rates in previous PEG-IFN/RBV non-responders.
CROI: RISK OF VIROLOGIC RELAPSE IN HEPATITIS C, GENOTYPE 1-INFECTED SUBJECTS AFTER 8, 12, OR 24 WEEKS OF TREATMENT WITH ABT-450/r + ABT-267 + ABT-333 + RBV: IDENTIFYING OPTIMAL TREATMENT DURATION - (03/04/13)
CROI: 12 WEEKS OF ABT-450/r, NON-NUCLEOSIDE INHIBITOR AND RBV ACHIEVED SVR24 IN >90% OF TREATMENT-NAïVE HCV GT1 PATIENTS AND 47% OF PRIOR NONRESPONDERS - (03/04/13)
Any news on hepatitis B ?
A very interesting cohort study from Amsterdam addressed the question in how far HBV active combination antiretroviral therapy can protect against new HBV infections in those HIV-patients which show no signs of past HBV infection and who have not been HBV vaccinated (HBV-PrEP) (18). All HBV susceptible patients at entry with an anti-HBc & anti-HBs negative (<10 IU/L) and a second sample available in time for follow-up HBV serology (if possible: before start or switch of treatment) were included into this analyses. Overall, 349 msm were available for analyses, of whom 33 developed an incident HBV infection during follow-up. In the Kaplan-Meier analyses HBV free survival was significantly higher in patients on a tenofovir containing antiretroviral treatment regimen versus a 3TC containing regimen (p<0.004). Both HBV active antiretroviral therapies had a better HBV free survival than patients who received no treatment (p<0.001).
These findings imply that potentially in patients not responding to HBV vaccination or not being vaccinated for HBV at all may benefit from an HBV active antiretroviral (preferentially tenofovir) in their antiretroviral combination therapy.
Further interesting studies were around the potential benefit of adding interferon to a tenofovir containing ART in order to improve HBV treatment outcome. Although HBV therapy with tenofovir allows for durable HBV suppression in most patients loss of HBe-Ag or even HBs-Ag and seroconversion with anti-HBs-Ab production remains a rare event. In this French pilot study (19) the effect on HBV-DNA, HBeAg, and HBsAg after adding PEG-IFN to HIV/HBV co infected patients undergoing TDF-containing antiretroviral therapy was evaluated in 10 patients. Patients with PEG-IFN intensification were matched 1:3 to controls (from the cohort of TDF treated patients without PEG-IFN) on total length of follow-up and HBeAg status at intensification. PEG-IFN intensification during TDF treatment was associated with accelerated HBeAg loss, yet without any effect on qHBeAg/qHBsAg decline or long-term serological outcomes. The authors concluded that adding PEG-IFN to a TDF-containing regimen may not be a beneficial option in patients with HIV coinfection.
CROI: Protective Effect of HBV-active c-ART against primary HBV-Infection - (03/05/13)
Summary
· Studies on the efficacy and safety of the HCV protease inhibitors boceprevir or telaprevir in HCV genotype 1 HIV co-infected individuals who have previously shown a non-response under dual HCV therapy with PEG-IFN/RBV have clearly demonstrated high early virological response rates at week 16. Response rate in the telaprevir treated patients was also independent from baseline fibrosis stage. These data underline that even in more difficult to treat patients with previous non-response to dual therapy and more advanced fibrosis stages HCV cure is achievable in the majority of patients and therefore needs to be considered in more advanced patients who may develop HCC or decompensate prior to the availability of interferon-free HCV therapies.
· HCV treatment including telaprevir or boceprevir in more advanced patient populations (higher fibrosis stages) may be associated with a higher rate of haematological toxicities and warrants careful monitoring and aggressive anemia management (ribavirin dose reduction or EPO use)
· Telaprevir administration can increase ribavirin levels. The pathomechanism remains unclear but could derive from higher ribavirin levels through intake with high fat meals or pgp interactions.
· New PK data suggest that boceprevir and rilpivirine can be coadministered without need for dose adjustment.
· 12 week of telaprevir based triple therapy in HIV patients with acute HCV will work for the majority of patients (around 80%) with acute GT1 infection; however, it will not lead to cure in all. Data from a randomized clinical trial are needed to investigate safety and cost-effectiveness of triple therapy versus the current gold standard of PEG-IFN/RBV which also has obtained high treatment success rates of about 70-80%.
· The two second wave HCV protease inhibitor studies in HIV/HCV coinfected individuals with simeprevir and feldaprevir, respectively have demonstrated excellent early virological response rates. The majority of patients achieved RVR and were able to be randomized to shorter treatment durations of 24 weeks. Therefore, it appears very likely that in the very near future (2014) new HCV protease inhibitors will become available which will offer once daily dosing, improved tolerability profiles and most importantly shortened treatment duration at least for those patients who achieve RVR. Also the drug interaction profile is different and at least with feldaprevir the combination with boosted darunavir is possible.
· Interferon-free treatment of hepatitis C with sofosbuvir and ledipasvir fix dose combination and ribavirin for 12 weeks in previous GT1 null-responders leads to 100% SVR12 response rates, suggesting that more potent oral combination therapies can overcome some of the treatment challenges in the non-responder population. Nevertheless these data also need to be obtained in cirrhotics as the most difficult to treat patient group.
· 12 weeks of simeprevir + sofosbuvir led to an SVR8 rate of 96% with RBV and 93% without RBV (in prior null-responders), indicating that in very potent DAA combinations there may be a room for IFN and ribavirin free strategies.
· The AbbVie studies demonstrate that there may be a potential for different HCV treatment strategies in more or less challenging to treat patient populations. So whereas HCV treatment naïve patients with GT 1 do very well with the combination of ABT-450/r + non-nucleoside polymerase inhibitor, further combination partners may be needed for obtaining equally high success rates in previous PEG-IFN/RBV non-responders.
· HBV-active combination antiretroviral therapy (cART) protects against primary HBV infection (≈ HBV PrEP); TDF-cART in this cohort was significantly more protective than 3TC-only-cART.
· Adding interferon to HBV nucleos(t)ide therapy does not improve outcome of HBV therapy.
References
1. Cotte L, Braun J, Lascoux-Combe C, Vincent C, Pol S, Valentin M-A, Lacombe K, Nau D, Aboulker JP, Molina J-M, and ANRS HC26 Study Group. High Early Virological Response with Telaprevir-Pegylated-Interferon-Ribavirin in Treatment-experienced Hepatitis C Virus Genotype 1/HIV Co-infected Patients: ANRS HC26 TelapreVIH Study. 20th Conference on Retroviruses and Opportunistic Infections, March 3-6, 2013; abstract 36
2. Poizot-Martin I, Bellissant E, Piroth L, Renault A, Quertainmont Y, Rosenthal E, Alric L, Guyader D, Bourliere M, Molina J-M, and ANRS-HC27 BOCEPREVIH Study Group. ANRS-HC27 BocepreVIH Interim Analysis: High Early Virologic Response with Boceprevir + Pegylated Interferon + Ribivirin in Hepatitis C Virus/HIV Co-infected Patients with Previous Failure to Pegylated Interferon + Ribivirin. 20th Conference on Retroviruses and Opportunistic Infections, March 3-6, 2013; abstract 37
3. Benito JM, Bichoupan K, Soriano V, Maida I, Branch A, Sanchez C, Rallon N, Aguilera A, Barreiro P, Dieterich D. Triple Combination Therapy for Hepatitis C with Telaprevir Exhibits Higher Early Antiviral Potency than with Boceprevir Regardless HIV Status. 20th Conference on Retroviruses and Opportunistic Infections, March 3-6, 2013; abstract 676
4. Martel-Laferriere V, Brinkley S, Bichoupan K, Posner S, Stivala A , Perumalswami P, Schiano T, Sulkowski M, Dieterich D, Branch A. On-treatment Responses to Telaprevir-based Hepatitis C Treatment Are Similar in HIV/Hepatitis C Virus Co-infected and Hepatitis C Virus Mono-infected Patients. 20th Conference on Retroviruses and Opportunistic Infections, March 3-6, 2013; abstract 679
5. Hammond K, Jimmerson L, MacBrayne C, Ray M, Bushman L, Burton J, Baouchi-Mokrane F, Everson G, Anderson P, Kiser J. Increased Plasma and Intracellular Ribavirin Concentrations Associated with Telaprevir Use. 20th Conference on Retroviruses and Opportunistic Infections, March 3-6, 2013; abstract 34
6. Rhee E, Feng H-P, Xuan F, Lin W, Smith C, Zhu Y, Butterton J. Absence of a Significant Pharmacokinetic Interaction between the Hepatitis C Virus Protease Inhibitor Boceprevir and HIV-1 NNRTI Rilpivirine. 20th Conference on Retroviruses and Opportunistic Infections, March 3-6, 2013; abstract 537
7. European AIDS Treatment Network (NEAT) Acute Hepatitis C Infection Consensus Panel. Acute hepatitis C in HIV-infected individuals: recommendations from the European AIDS Treatment Network (NEAT) consensus conference. AIDS. 2011 Feb 20;25(4):399-409.
8. Fierer D. Telaprevir for Acute Hepatitis C Virus in HIV+ Men both Shortens Treatment and Improves Outcome. 20th Conference on Retroviruses and Opportunistic Infections, March 3-6, 2013; abstract 156LB
9. Sabo J, Kort J, Haschke M, Ballow C, Girlich B, Feifel U, Lang B, Schobelock M, Elgadi M. Pharmacokinetic Interactions of Darunavir/ritonavir, Efavirenz, and Tenofovir with the Hepatitis C Virus Protease Inhibitor Faldaprevir in Healthy Volunteers. 20th Conference on Retroviruses and Opportunistic Infections, March 3-6, 2013; abstract 35
10. Dieterich D, Soriano V, Nelson M, Rockstroh J, Arasteh K, Bhagani S, Talal A, Tural C, Vinisko R, Kort J. STARTVerso 4: High Rates of Early Virologic Response in Hepatitis C Virus Genotype 1/HIV Co-infected Patients Treated with Faldaprevir + Pegylated Interferon and Ribavirin. 20th Conference on Retroviruses and Opportunistic Infections, March 3-6, 2013; abstract 40LB
11. Dieterich D, Rockstroh J, Orkin C, Gutierrez F, Klein M, Reynes J, Jessner W, Lenz O, Peeters M, Beumont-Mauviel M. Simeprevir with Pegylated Interferon/Ribavirin in Patients Co-infected with Chronic Hepatitis C Virus and HIV-1: Week-24 Interim Analysis of the TMC435-C212 Study. . 20th Conference on Retroviruses and Opportunistic Infections, March 3-6, 2013; abstract 154LB
12. Gane G, Stedman C, Anderson J, Hyland R, Hindes R, Symonds W, Berrey. 100% Rapid Virologic Response for PSI-7977 + Ribavirin in Genotype 1 Null Responders (ELECTRON): Early Viral Decline Similar to that Observed in Genotype 1 and Genotype 2/3 Treatment-naïve Patients. 19th Conference on Retroviruses and Opportunistic Infections, March 5-8, 2012; abstract 54LB
13. Gane E, Hyland R, Ding X, Pang P, McHutchison J, Symonds W, Stedman C. ELECTRON: 100% Suppression of Viral Load through 4 Weeks' Post-treatment for Sofosbuvir + Ledipasvir (GS-5885) + Ribavirin for 12 Weeks in Treatment-naïve and -experienced Hepatitis C Virus GT 1 Patients. 20th Conference on Retroviruses and Opportunistic Infections, March 3-6, 2013; abstract 41LB
14. Lawitz E, Ghalib R, Rodriguez-Torres M, Younossi Z, Corregidor A, Jacobson I, Callewaert K, Symonds W, Picchio G, Lindsay K. Suppression of Viral Load through 4 Weeks Post-Treatment Results of a Once-daily Regimen of Simeprevir + Sofosbuvir with or without Ribavirin in Hepatitis C Virus GT 1 Null Responders. 20th Conference on Retroviruses and Opportunistic Infections, March 3-6, 2013; abstract 155LB
15. Osinusi A, Bon D, Herrmann E, Teferi G, Talwani R, Masur H, Symonds W, McHutchison J, Fauci A, Kottilil S, and NIAID SPARE Study Team. High Efficacy of Sofosbuvir with Weight-based Ribavirin for 24 Weeks in Difficult-to-Treat Patients. 20th Conference on Retroviruses and Opportunistic Infections, March 3-6, 2013; abstract 157
16. King M, Xie W, Larsen L, Cohen D, Podsadecki T, Bernstein B. Risk of Virologic Relapse in Hepatitis C Virus GT1-infected Subjects after 8, 12, and 24 Weeks of ABT-450/r+ABT-267+ABT-33+Ribavirin: Identifying Optimal Treatment Duration. 20th Conference on Retroviruses and Opportunistic Infections, March 3-6, 2013; abstract 39
17. Lawitz E, Cohen D, Poordad F, Kowdley K, Everson G, Freilich B, Jensen D, Heckaman M, Pilot-Matias T, Bernstein B. 12 Weeks of ABT-450/Ritonavir, Non-nucleoside Inhibitor and Ribavirin Achieved SVR24 in >90% of Treatment-naïve Hepatitis C Virus GT1 Patients and 47% of Prior Non-responders. 20th Conference on Retroviruses and Opportunistic Infections, March 3-6, 2013; abstract 38
18. Heuft M, van den Berk G, Houba S, Smissaert T, Blok W, Regez R, Dijksman L, Brinkman K. Protective Effect of HBV-active c-ART against primary HBV-Infection. 20th Conference on Retroviruses and Opportunistic Infections, March 3-6, 2013; abstract 33
19. Boyd A, Miailhes P, Maylin S, Gozlan J, Lascoux-Combe C, Delaugerre C, Girard P-M, Lacombe K. Intensification with Pegylated Interferon during Treatment with Tenofovir in HIV/Hepatitis B Virus Co-infected Patients. 20th Conference on Retroviruses and Opportunistic Infections, March 3-6, 2013; abstract 668
|
| |
|
 |
 |
|
|