 |
 |
 |
| |
Treatment of Acute HCV in HIV-infected
MSM Incorporating Telaprevir
|
| |
| |
Reported by Jules Levin
CROI 2013
Daniel S. Fierer, M.D.
Division of Infectious Diseases
Mount Sinai School of Medicine
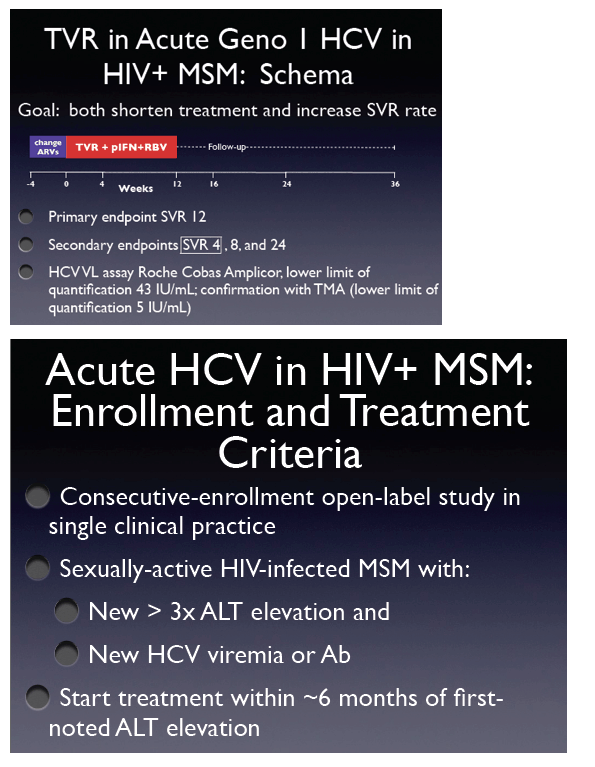
This study is a small study where HIV+ MSM with acute HCV, who were referred from clinicians throughout NYC to Fierer, would receive for 12 weeks telaprevir (750 mg every 8 hrs, but now new data has been released at AASLD in Nov 2012 that twice a day dosing with 1250mg appeared to be as effective) + Peginterferon 2a + weight based RBV, with the standard stopping rule of >1000 IU/mL at week 4. The primary endpoint is week 12 SVR & today he is presenting SVR 4 along with some longer results as well. The assay used: HCV VL Roche Cobas Amplicor, lower limit of detection 43 IU/mL; confirmation with TMA (lower limit of quantification of 5 IU/mL). Patients were enrolled consecutively referred by HIV providers in the community to his single site. The enrollment criteria were sexually active HIV-infected MSM with new 3-fold ALT elevation with new HCV viremia or Ab. He tried to get treatment started within about 6 months of first-noted ALT elevation.
40 patients were enrolled for evaluation between July 2011 to Sept 2012. 13 patients were excluded for having non-1 genotype HCV: n=4 x 2b; 3 x 4). 1 patient was on a salvage regimen where it wasn't safe to change their HAART so PK interactions were a barrier with the HAART the person was on. 5 patients could not get insurance coverage for telaprevir. 5 patients spontaneously cleared. 2 patients refused all treatment.
20 patients were treated, median age 44. 17 white, 2 hispanic, 1 black. 18 genotype 1a, 2 gt 1b. IL28B: 4 CT, 3TT (35%), 13 CC (65%). Several weeks before study treatment if some patients (9/20) had to switch their HAART regimen due to drug interactions with telaprevir that was done.
RESULTS
Success Rates
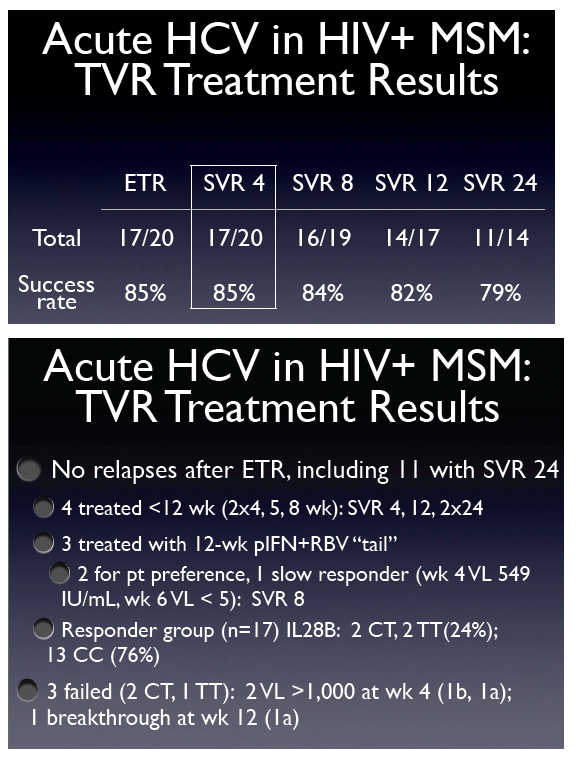
ETR: 17/20 85%
SVR 4: 17/20 85%
SVR 8: 16/19 84%
SVR 12: 14/17 82%
SVR 24: 11/14 79%
- No relapses after ETR, including 11 with SVR24.
- 4 treated for <12 weeks (2 for 4 weeks, 1 for 5 wks, 1 for 8 wks), 2 stopped for adverse events, 2 negotiated a shorter treatment: SVR 4, 12 2 x 24. "all of them had a pretty good response".
- 3 were treated for a total of 24 weeks, treated with a 12-wk tail of P/R, 2 because they requested it, one because they were a slow responder, did not meet stopping rule, wk 4 VL 549, but wk 6 VL <5: SVR8.
- all the CCs responded, the 3 failures were non-CC: 2 VL >1000 at wk 4 (1b, 1a), 1 breakthrough at wk 12 (1a) (from jules: so of the 7 non-CCs 3 failed and all CCs were successful).
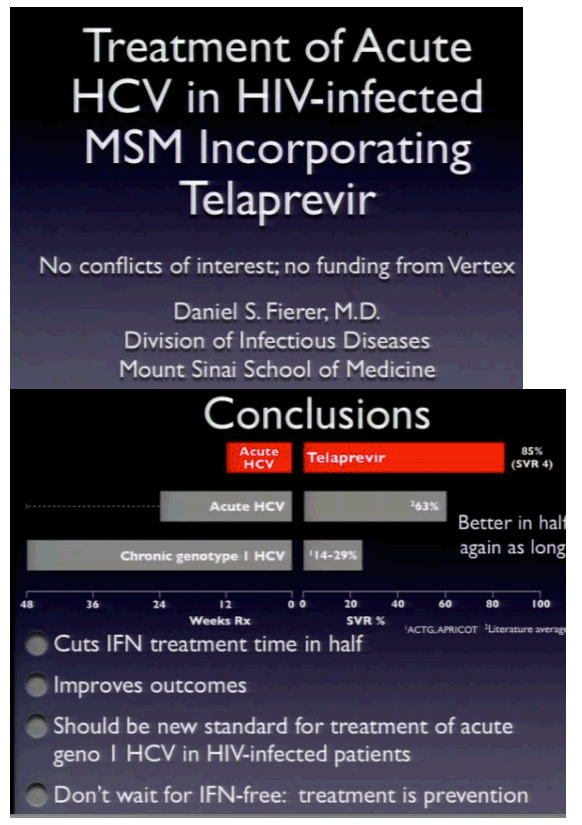
Dr Fierer started his talk by noting the seminal study from German researchers finding a 98% SVR rate with interferon alone without RBV for 24 weeks in acute HCV, not HIV-infected. Then he noted the global epidemic of acute HCV among HIV+ MSM in 4 continents, 2 hemispheres. Then he noted the studies conducted in HIV+ MSM with acute HCV for 24 to 48 weeks with SVR rates ranging from 53% to 82% with on average as he said about a 63% SVR. He hypothesized that treating acute infection with telaprevir+P/R would be better & half as long so with the goal to both shorten treatment & improve the SVR rate. During the 4 weeks prior to starting treatment in this study some patients had to have their HIV treatments switched due to drug-drug interactions between some HIV protease inhibitors & NNRTIs, but as noted by Fierer raltegravir, Reyataz/r, RPV, TDF/FTC (from Jules: and I think abacavir as well) and EFV can be used, with EFV there is a 50% TLV dose increase.
All the 13/13 CCs responded and of the 7 non-CCs (CT, TT) only 4 responded and 3 were failures. 2 of the failures were "dramatic", rebounded >1000 by week 4 and 1 was a gt1b (1 1a, 1 1b), and there was 1 breakthrough at week 12 (1a). 9 of the 20 patients treated in the study had to change their HIV HAART regimen within the first few weeks of the study and all patients in the study maintained their undetectable viral load through the end of followup. 2 patients discontinued: 1 for anemia that required a transfusion (Hg 6.6), he developed zoster & a skin abscess, and 1 person stopped at week 5 for general interferon intolerance, and Fierer said both of these patients had a response through 24 weeks. 3 patients had to reduce RBV dose, 1 with a Hg <10 and the other 2 close to 10. 19 patients developed pruritus, anal pruritus was common although it was "very mild" and all they needed was topical hydrocortisone, and only 2 had a rash and it was barely detectable, Fierer said so was "well tolerated".
Fierer summed up his talk, see the data in the Conclusion slide: [this] "should be the standard of care for treatment of acute geno 1 HCV in HIV-infected patients; don't wait for IFN-free - treatment is prevention."
"I think this is a great result, cuts IFN time down in half, this study treatment was 12 weeks compared to previous studies with P/R in acute infection in HIV+ MSM (see slide with data from studies below) for as little as 24 weeks but as much as 48 weeks achieving on average 63% SVR in gt1, improved outcome ie 85% SVR, I've been controversial in this field, I really think although its a small study, for treaters, experienced treaters of acute HCV & good at recognizing it, experienced using TLV this is the way to go for acute infection, there is a large study ongoing now in Europe doing a direct comparison, with the release of all the new drugs coming the results of that study may not be as relevant, it needs to be done quickly, its tantalizing to say there are so many new good drugs coming out so why not wait for IFN-free regimens to treat these men but I would strongly discourage not thinking that way, there is decent evidence not just from me now but from others that there is significant disease in these men, these are a group of men that are transmitting HCV to others at a high rate, treating these men early is important to prevent further infections as well. During the Q&A one person raised this point, 5 of the original 40 patients, 20 who were not treated, 5 of them cleared spontaneously. Vincent Soriano said it was a small study, mostly CCs, and raised a concern they might have spontaneously cleared without treatment if you treat before waiting 6 months. In response Feirer said he waits quite a while, most patients seem to clear early regardless of the IL28, and he alluded to something he heard at this conference that IL28 was not significant in clearance. Marion Peters asked about the 15 patients who didn't get TLV, Fierer said 5 couldn't get insurance coverage & 7 were non-gt1. Some apparently were treated with P/R and Peters asked what was their SVR, Fierer couldn't recall exactly but estimated it was about 63-67%. Doug Dieterich said "this is a very effective demonstration of a high SVR rate in CC patients and I agree with Dr Soriano's data, how do you account for all the CCs in this study? I think like Vincent you have to be careful generalizing CC data to all patients with acute hepatitis C", in response Fierer said its probably just chance that he got so many CCs and he said there is data that there hasn't been a treatment affect noticed (CC vs non CC) with P/R. [from jules: is it possible that CC is more prevalent when HCV is transmitted sexually among MSM, is there any data on this?] Lynn Taylor said thanks for a provactive presentation and asked if the rebounder at week 12 was a reinfection, Feirer said a lot of his patients are very sexually active during treatment, he is waiting on sequencing to try to answer that question, he said I could have been a reinfection.
link to webcast of entire oral HCV session on wednesday:
http://webcasts.retroconference.org/console/player/19444?mediaType=podiumVideo






|
| |
|
 |
 |
|
|