 |
 |
 |
| |
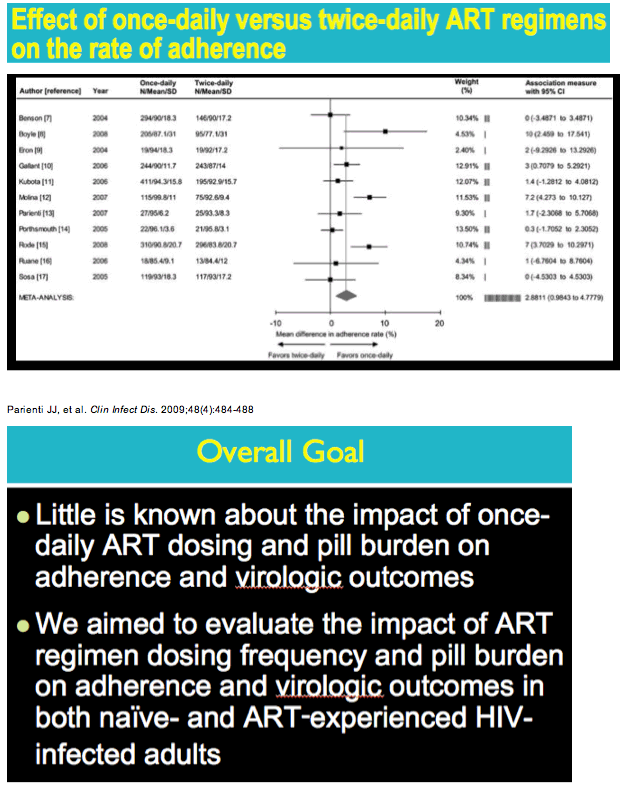
Once-Daily ART v Twice-Daily/Pill Burden Meta-Analysis Evaluates Adherence/Viral Control
|
| |
| |
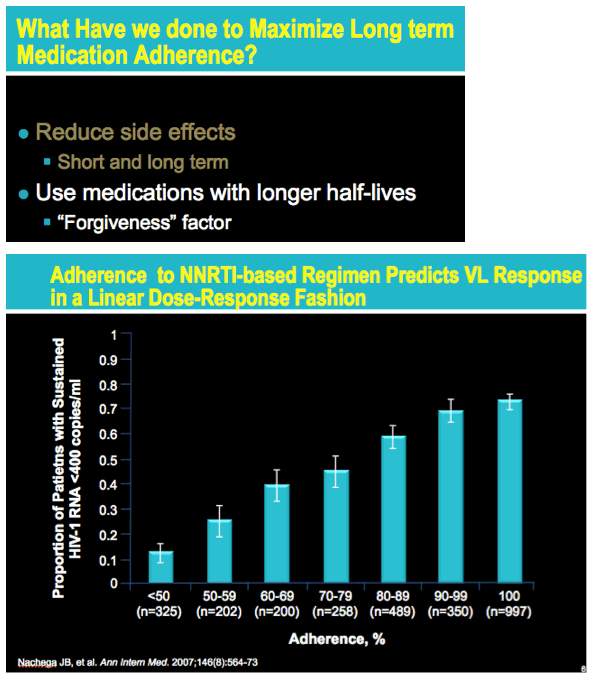
Once-Daily Regimens Modestly Improve Adherence, Not Viral Control, in Meta-Analysis
14th European AIDS Conference. October 16-19, 2013. Brussels
Mark Mascolini
Starting or switching to a once-daily antiretroviral regimen improved adherence compared with twice-daily pill taking, according to results of a 19-trial meta-analysis [1]. But the impact on adherence was modest and did not improve viral suppression.
Fixed-dose combinations and single-tablet regimens have greatly simplified pill taking for people with chronic diseases [2,3]. In people with HIV infection, single-tablet regimens have improved 6-month virologic response rates [4] and cut hospital admission rates [5,6]. But one study found evidence suggesting that one single-tablet combination, Atripla, may not be as durable as a multitablet combination including raltegravir, mostly because of side effects [7].
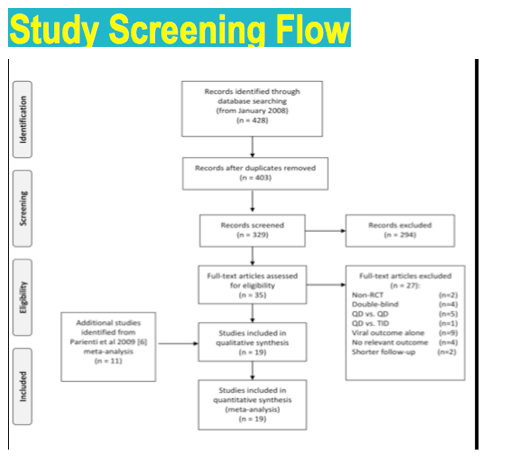
To get a better grasp on how antiretroviral dosing frequency and pill burden may affect adherence and virologic outcome in antiretroviral-naive and experienced adults, an international team conducted a systematic review and meta-analysis of randomized controlled trials of once- versus twice-daily regimens that measured (1) adherence by pill count or electronic monitors or (2) the percentage of participants who reached a viral load below 50 copies in a missing-data-equals-failure analysis.
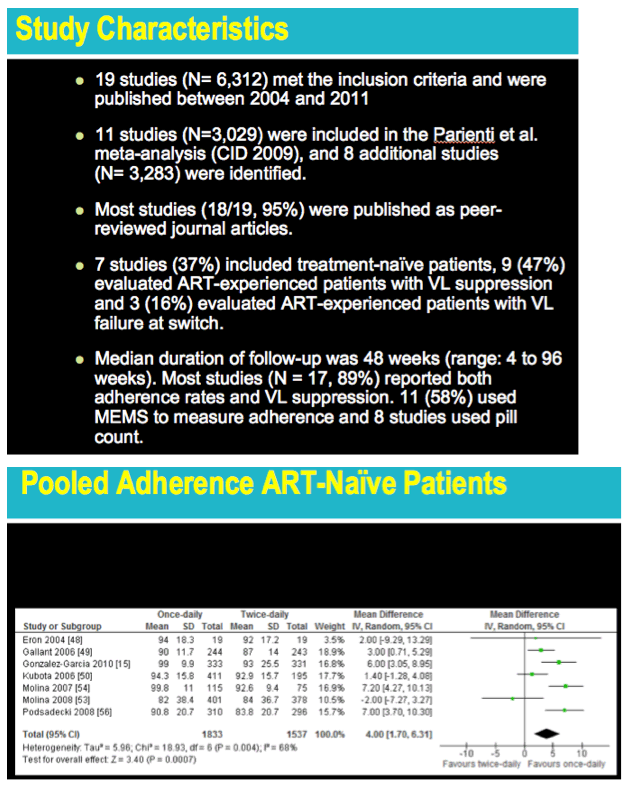
A search of electronic databases and conference abstracts through March 2013 yielded 19 studies involving 6312 people reported from 2004 through 2011. Eighteen studies appeared in peer-reviewed journals. Seven studies (37%) involved antiretroviral-naive people, 9 (47%) involved treatment-experienced people switching to a new regimen with virologic suppression, and 3 (16%) involved experienced people with virologic failure at the switch to a new regimen. Seventeen studies reported both adherence rates and viral suppression, 11 studies used the Medication Event Monitoring System (MEMS) to measure adherence, and 8 studies used pill count. Follow-up ranged from 4 to 96 weeks (median 48 weeks).
Pooled analysis of 7 trials that measured adherence in antiretroviral-naive people starting their first regimen found a small but statistically significant overall adherence advantage of 4% (95% confidence interval 1.70 versus 6.31) for once-daily dosing versus twice-daily dosing (test for overall effect, Z = 3.40, P = 0.0007).
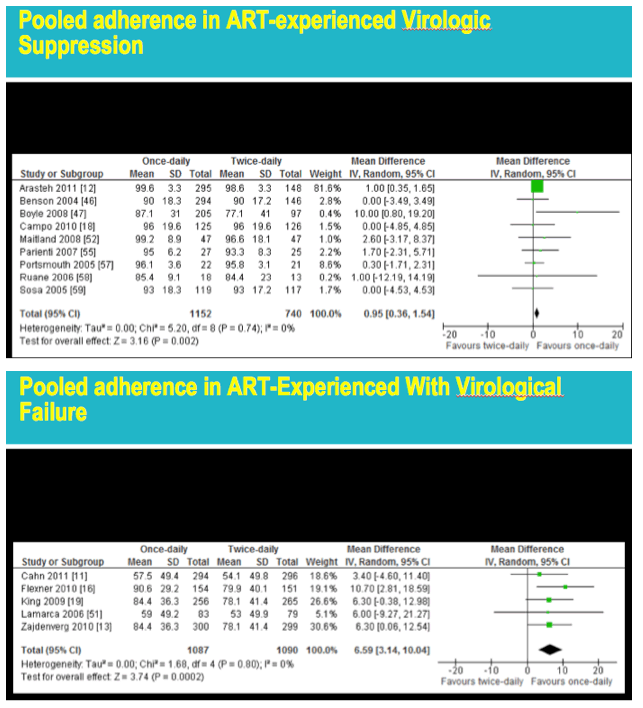
Pooled analysis of 5 trials that measured adherence in antiretroviral-experienced people with virologic failure at the switch to a new regimen also found a significant advantage for once- versus twice-daily dosing (mean difference 6.59%, 95% CI 3.14 to 10.04, test for overall effect, Z = 3.74, P = 0.0002). Pooled analysis of 9 trials that measured adherence in antiretroviral-experienced people with virologic suppression when switching to a new combination found a small but significant advantage for once-daily dosing over twice-daily dosing (mean difference 0.95%, 95% CI 0.36 to 1.54, test for overall effect, Z = 3.16, P = 0.002).
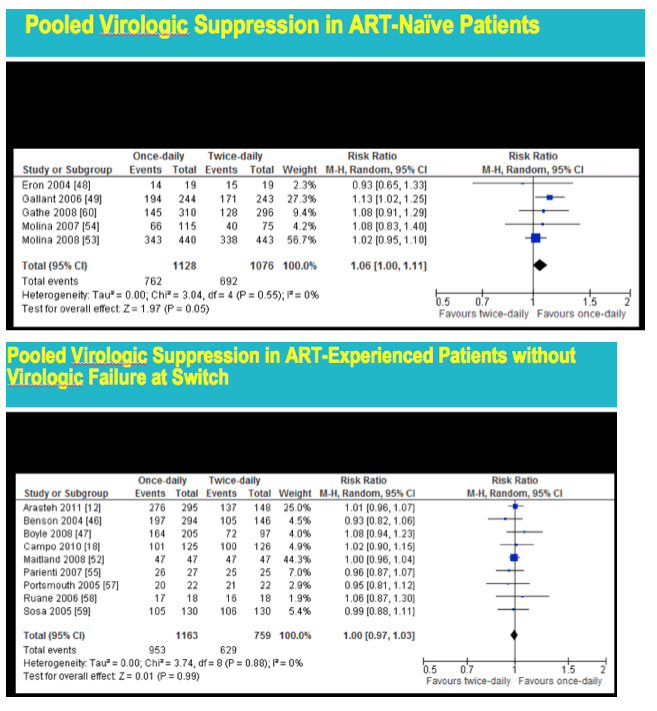
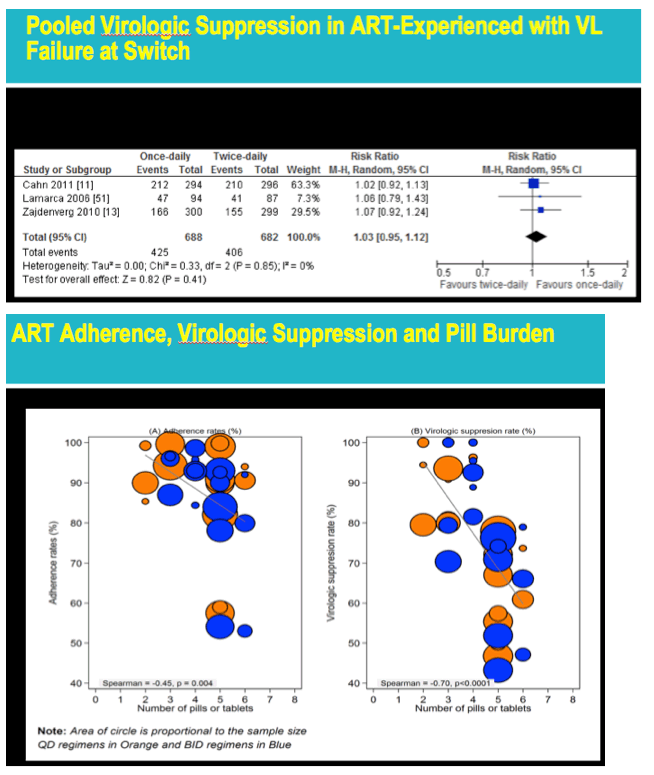
Pooling data from 5 trials of virologic suppression in people starting their first antiretrovirals, the researchers found a marginal advantage for once- versus twice-daily dosing (risk ratio [RR] 1.06, 95% CI 1.00 to 1.11, test for overall effect, Z = 1.97, P = 0.05). Pooled analysis of 9 trials that assessed virologic suppression in antiretroviral-experienced people with virologic suppression at the switch found no advantage for once-daily dosing (RR 1.00, 95% CI 0.97 to 1.03). And once-daily regimens had no advantage in pooled analysis of 3 trials involving antiretroviral-experienced people with virologic failure at the switch (RR 1.03, 95% CI 0.95 to 1.12).
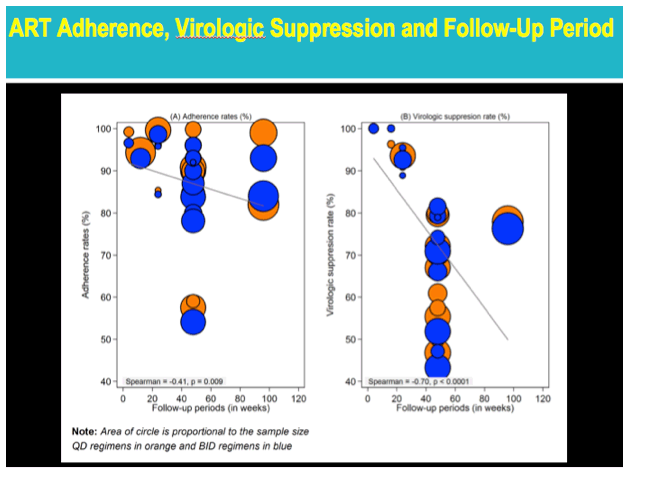
These analyses also showed that both adherence and virologic suppression waned as follow-up continued, but adherence declined less with once-daily dosing than with twice-daily regimens.
Overall absolute increase in antiretroviral adherence with once-daily regimens was 2.5%. That meager gain, the researchers suggested, may partly explain why once-daily dosing did little or nothing to bolster virologic suppression in these trials. Other factors that may have contributed to the apparent lack of virologic impact with once-daily pill taking include (1) relatively short duration of several trials, (2) recruitment of antiretroviral-experienced people who were already highly adherent and virologically suppressed, and (3) lower drug exposure at the end of dosing intervals with once-daily regimens that may make those regimens less forgiving of suboptimal adherence. For all these reasons, the researchers proposed, their analysis may underestimate the difference in virologic suppression between once- and twice-daily regimens.
Taken together, the data may mean that switching people from once- to twice-daily regimens--if necessary--"may be a reasonable option," the investigators suggest. But that hypothesis could crumble if the twice-daily regimen requires more pills, because this study also disclosed a significant negative correlation between virologic suppression rate and pill burden regardless of dosing frequency. The investigators called for research on switching from once-daily single-tablet regimens to once-daily multitablet regimens.
References
1. Nachega JB, Parienti JJ, Uthman OA, et al. Effect of once-daily dosing and lower pill burden antiretroviral regimens for HIV infection: a meta-analysis of randomised controlled trials. 14th European AIDS Conference. October 16-19, 2013. Brussels. Abstract PS4/5.
2. Bangalore S, Kamalakkannan G, Parkar S, Messerli FH. Fixed-dose combinations improve medication compliance: a meta-analysis. Am J Med. 2007;120:713-719.
3. Parienti JJ, Bangsberg DR, Verdon R, Gardner EM. Better adherence with once-daily antiretroviral regimens: a meta-analysis. Clin Infect Dis.
2009;48:484-488. http://cid.oxfordjournals.org/content/48/4/484.long
4. Kapadia S, Grant R, Hodder S. Virologic response better with single tablet fixed dose antiretroviral regimens compared with multiple tablet regimens in an urban population of HIV-infected persons. IDWeek 2013. October 2-6, 2013. San Francisco. Abstract 168.
5. Sax PE, Meyers JL, Mugavero M, Davis KL. Adherence to antiretroviral treatment and correlation with risk of hospitalization among commercially insured HIV patients in the United States. PLoS One. 2012;7:e31591. http://www.plosone.org/article/info%3Adoi%2F10.1371%2Fjournal.pone.0031591
6. Cohen CJ, Meyers JL, Davis KL. Association between daily antiretroviral pill burden and treatment adherence, hospitalisation risk, and other healthcare utilisation and costs in a US Medicaid population with HIV. BMJ Open. 2013;3:e003028. http://bmjopen.bmj.com/content/3/8/e003028.long
7. Trottier B, Machouf N, Thomas R, et al. Single tablet regimens do not necessarily translate into more durable HIV treatments. 7th IAS Conference on HIV Pathogenesis, Treatment and Prevention. June 30-July 3, 2013. Kuala Lumpur. http://pag.ias2013.org/EPosterHandler.axd?aid=2764
----------------------------------
Reported by Jules Levin
from Jules: this is a very interesting & well done meta-analysis. The convenience factor however I believe matters quite a lot to at least a large proportion of patients, particularly ART-naive patients or patients who have never virologically failed regimen, and what about patients who have switched from a suppressive regimen for simplification purposes or because the once daily or FDC or STR they switched to may also have more friendly toxicity or tolerability profile. In looking at the table below of "Pooled Adherence ART-Naive Patients", there are 7 studies with 3 of these studies shower a larger difference in adherence, 6-7.2% with the other studies less of a difference so when you average them all out there is a 4% adherence difference. When looking at the table "Pooled Adherence in ART-Experienced With Virological Failure" the average/pooled adherence difference is 6.59% where there is 1 study with a 3.40% adherence benefit but the others find benefits as much as 10.70% in one study and 6.30%, 6.30% & 6.00% in the other 4. Regarding virology suppression, in the table "Pooled Virologic Suppression in ART-Naive Patients" there are 5 studies each showing respectively 13% benefit, 8% benefit, 8% benefit and then 1 study showing 2% benefit & another a negative 7%, so the pooled affect is a 6% benefit, there is a divergence in outcomes between the studies with several showing much more benefit in my view and a few much less difference in suppression ending up with a pooled suppression showing a Risk ratio of 1.06 (6%). Then there are these other groups of analysis that showed little benefit: Pooled Virologic Suppression in ART-Experienced with VL Failure at Switch, Pooled Virologic Suppression in ART-Experienced Patients without Virologic Failure at Switch, Pooled adherence in ART-experienced Virologic Suppression.





TRANSITION
How do we improved adherence?
MAIN MESSAGES
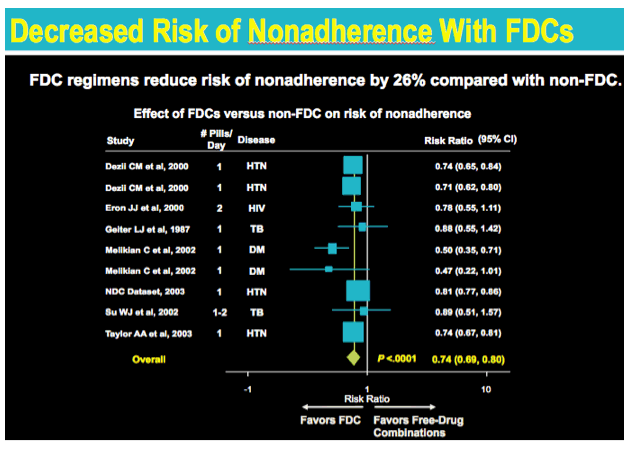
This large meta-analyses revealed an adherence benefit of FDC over non-FDC regimens in decreasing non-adherence in multiple therapeutic areas. The RR was 0.74 or a 26% reduction. Note that all 9 studies came to the same conclusion favoring FDC as beneficial in decreasing the risk of non-adherence. However due to sample size some results were not statistically significant.
BACKGROUND
Meta-analysis of 9 clinical trials in 4 therapeutic areas (TB, HTN, HIV, DM) 11,925 FDC patients and 8317 non-FDC patients. Only studies reporting FDC vs "free-drug combos" were selected.
For simplicity, compliance in this MA was considered as either adherence or persistence to regimen. Investigators extracted mean age of population, length of f/u, and efficacy differences between 2 treatment modalities, if available.
Disease state for each author/article
Geiter TB
Su TB
Eron HIV
Taylor HTN
Dezii HTN
NDC HTN
Melikian DM




|
| |
|
 |
 |
|
|