 |
 |
 |
| |
In chronically HIV-1-infected patients long-term antiretroviral therapy initiated above 500 CD4/mm3 achieves better HIV-1 reservoirs' depletion (HIV-DNA) and T cell count restoration
|
| |
| |
Slides below
......'from Jules: early HAART with CD>500 & ongoing full viral suppression <50 c/ml maximized in this study HIV-DNA reduction compared to starting HAART at lower CD4/delayed ART'
Presented by Laurent Hocqueloux (France).
L. Hocqueloux1, V. Avettand-Fenoel2,3, T. Prazuck1, A. Melard2, E. Legac4, M. Niang1, C. Mille1, J. Buret1, C. Rouzioux2,3, "Coordinated Action on HIV Reservoirs" (AC32) of the ANRS (Agence Nationale de Recherches sur le Sida et les hepatites virales)
1CHR d'Orleans - La Source, Infectious and Tropical Diseases, Orleans, France, 2APHP, Hopital Necker-Enfants Malades, Laboratory of Virology, Paris, France, 3Universite Paris Descartes Sorbonne Paris Cite, Paris, France, 4CHR d'Orleans - La Source, Laboratory of Immunology, Orleans, France
DISCUSSION & Conclusions
· Our results support early treatment, even in patients with high CD4 count
· One third of CHI>500 achieved a 'normal' T cell count (CD4 ≥900/mm3 and CD4/CD8 >1) together with a low viral reservoir
· no less than those treated at PHI (unpublished personal data)
· as seen in most of PTC
· whereas CHI-infected pts treated <500 CD4 are unlikely to achieve it
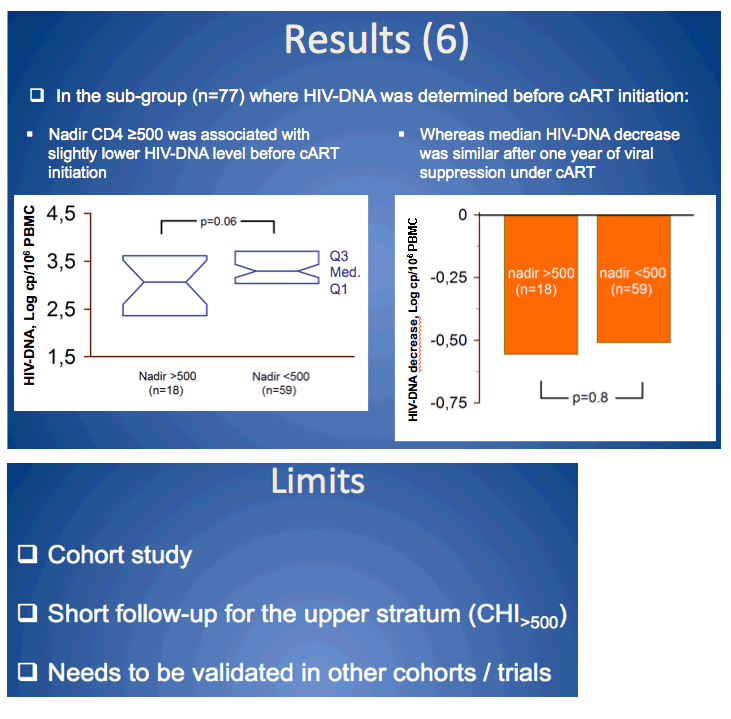
· In CHI>500, a lower pre-therapeutic HIV-DNA level is likely to explain part of this good viro-immunologic outcome
· CHI>500 may be better candidates to benefit from a therapeutic vaccine and / or drugs emptying viral reservoirs
(and thus to achieve a functional cure?)
ABSTRACT
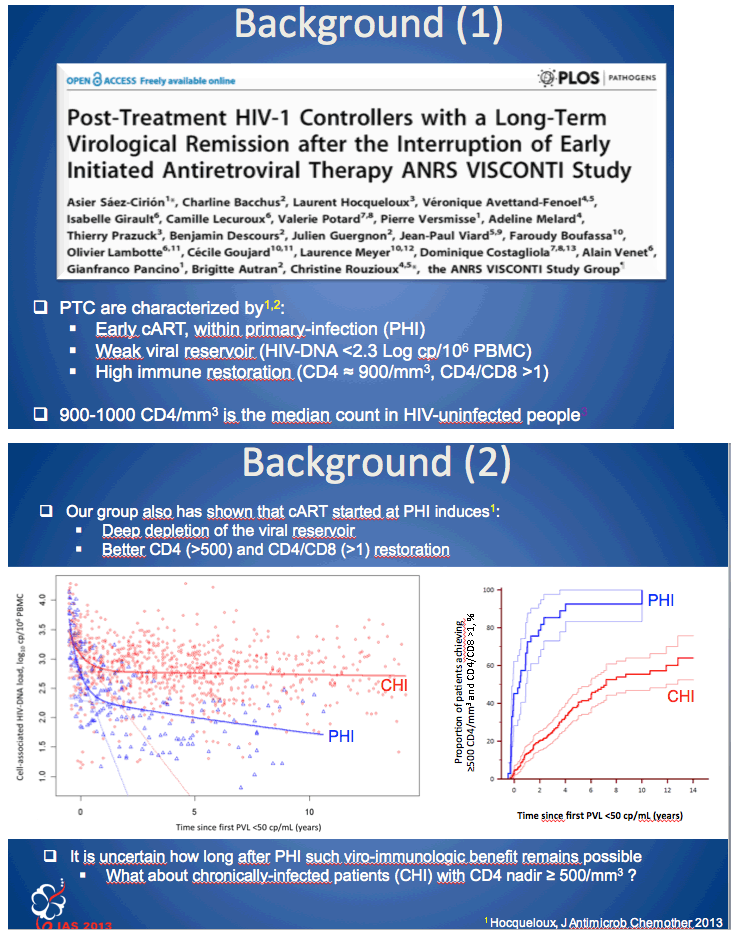
Background: Our group has already shown that antiretroviral therapy (ART) initiated during primary HIV-infection is associated with a profound reduction of viral reservoirs and restores optimal immunity. Present study aimed whether such benefit could be also observed in chronically infected patients (Fiebig VI) treated before the CD4+ count falls below 500/mm3 (CHI>500).
Methods: Prospective cohort-study of HIV-1-infected patients enrolled from 2005 to 2012 in Orleans' Hospital. Patients on ART achieving plasma viral load (PVL) < 50 copies/ml were included and followed as long as PVL remained controlled. Patients were stratified according to CD4+ nadir: >500, 350-500, 200-350 and < 200 cells/mm3. Total HIV-DNA in PBMC was measured at least once a year (Biocentric, Bandol, France), before (when possible) and during treatment; T-cell count (CD4+, CD8+) and PVL were measured every 3-4 months. Factors leading to a low reservoir in blood (HIV-DNA < 2.3 log/M PBMC) and a normal T-cell count (CD4+ >500/mm3, CD4/CD8 >1) were determined using Cox proportional-hazards regression.
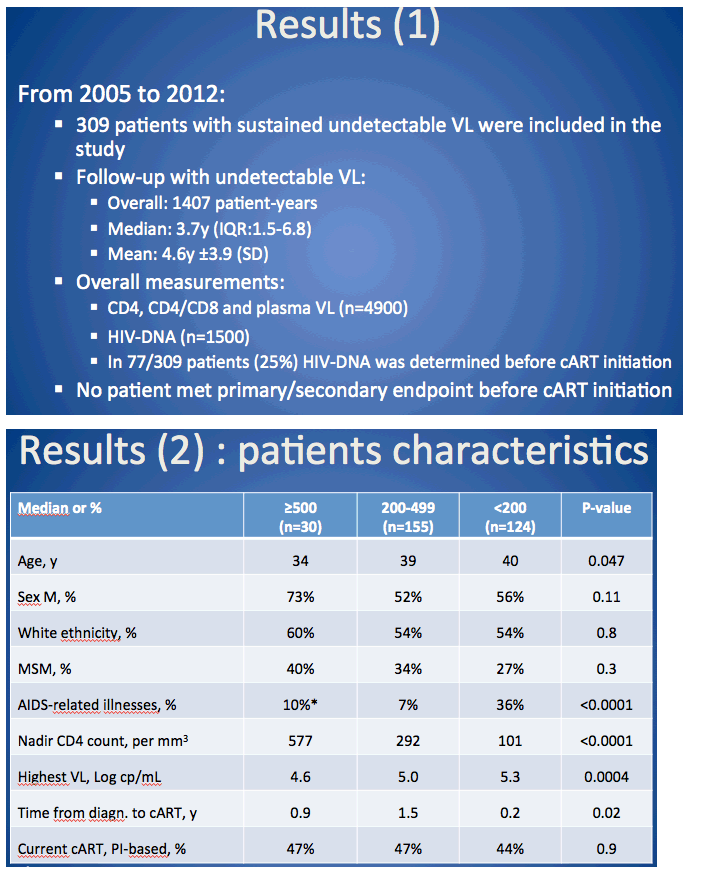
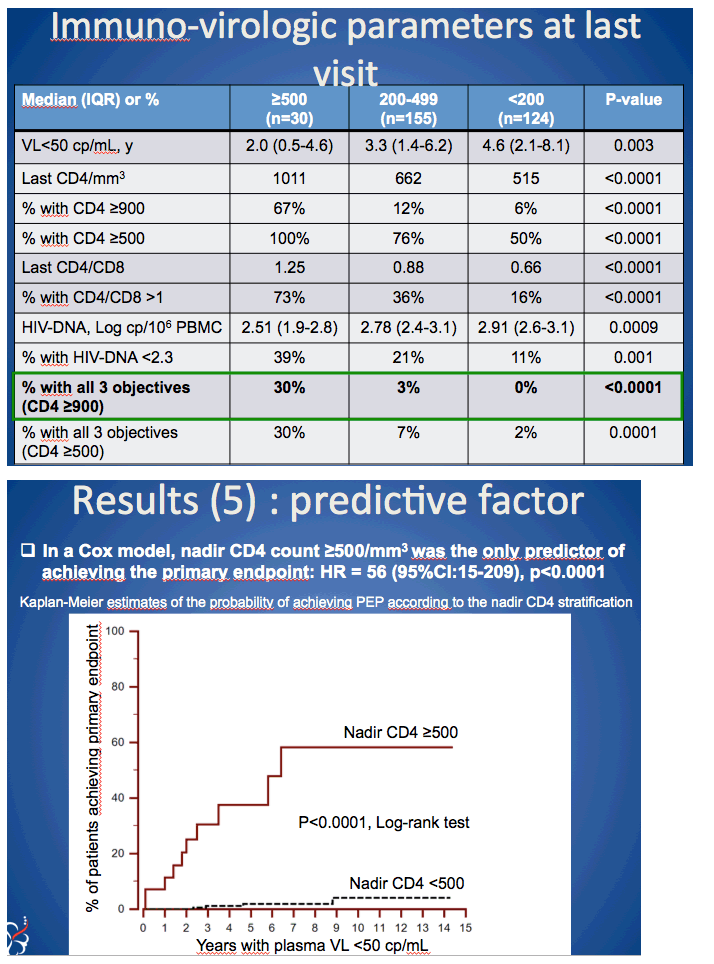
Results: 283 patients were included (n=28, 26, 113 and 116 for >500, 350-500, 200-350 and < 200 strata, respectively) and followed during a median 4 years. At last visit, CHI>500 patients had significantly lower HIV-DNA level (median=2.50 log) as compared with other strata (2.88, 2.78 and 2.91, respectively; p=0.003). Immune reconstitution was faster and better
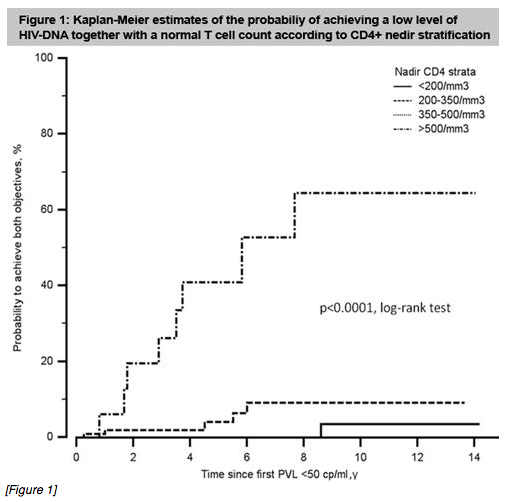
[Figure 1]
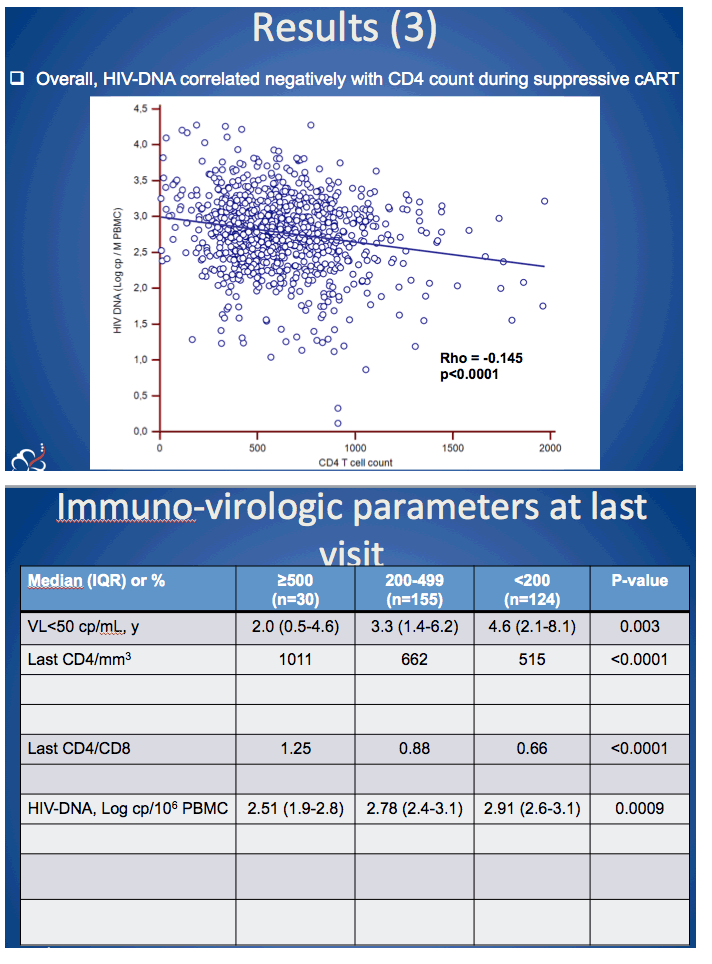
in CHI>500 than in other strata (median CD4+=883/mm3 vs. 722, 645 and 520, respectively; p< 0.0001; median CD4/CD8=1.22 vs. 0.96, 0.85 and 0.68, respectively; p< 0.0001). In multivariate analysis, ART started above 500/mm3 was highly predictive to achieving low HIV-DNA (< 2.3 log) and normal T-cell count (HR=32.4, 95%CI:10.5-99.5, p< 0.0001) (Fig.1).
Conclusion: Even patients treated at the chronic phase could benefit from early treatment. This reinforces the value of public health programs to promote early HIV testing and treatment, especially among highly-exposed risk groups.
---------------------------------------


|
| |
|
 |
 |
|
|