 |
 |
 |
| |
Independent Predictors of Carotid Intimal Thickness Differ Between HIV+ and HIV- Patients with Respect to Traditional Cardiac Risk Factors, Risk Calculators, Lipid Subfractions, & Inflammatory Markers (poster)
|
| |
| |
Reported by Jules Levin
IAS 2013 June 30-july 3 Kuala Lumpur
Author(s): R . Hsu1, K. Patton2, J. Liang3, R. Okabe4, J. Aberg5, N. Fineberg2
Institute(s): 1New York University Medical Center, Internal Medicine, New York, USA 2University of Alabama, Biostatistics, Birmingham, USA 3New York University, New York, USA 4New York University, School of Medicine, New York, USA 5New York University Medical Center, Infectious Diseases, New York, USA
BACKGROUND
Carotid Intimal Thickness (CIMT) predicts CAD and helps risk-stratify patients for cardiovascular events. HIV+ patients have greater and more rapid progression of CIMT than HIV- patients. However, testable predictors of CIMT have not been determined and differentiated between HIV+ and HIV- patients. Traditional risk factors, lipids and sub-particles, risk calculators, and inflammatory markers will be correlated with CIMT to determine which markers are most associated
with atherosclerosis in a prospective cohort of HIV+ and HIV- patients.
METHODS
307 patients (179 HIV+,128 HIV-) had their maximal CIMT determined at the CCA and ICA (including bulb). Heart Age, traditional risk factors, Framingham and D:A:D Risk (HIV+), Lipids and sub-particles (Total Cholesterol, LDL, HDL, TG, LDL#, small LDL, Large HDL#, LP(a)-c, ApoB/A1 ratio), and inflammatory indices (d-dimer, IL-6, hsCRP, LPPLA2, homocysteine) were measured in each patient. Differences in demographics, risk factors, and CIMT between HIV+ and
HIV- patients were retrospectively analyzed with Mann Whitney and Chi-square testing. Stepwise multiple regression analysis determined which variables were independently correlated with CIMT.
RESULTS
HIV+ patients (male 97.8%, mean CD4 609, 91% HIV PCR <200) were older by 4 years, had a calculated heart age older by 6.7 years, had overall lower lipid
values, although more likely on lipid lowering and hypertensive medications than their HIV- counterparts (male 89%).
Stepwise multivariate regression of independent variables significantly correlated with CIMT in HIV+ patients included: Heart age, IL-6, Diabetes, Hypertensive Medications, Framingham Risk, and D:A:D.
In HIV- individuals, Heart Age, Hypertension, Hypertensive meds, MI/Stroke history, HDL, Large HDL, Triglycerides, Framingham Risk scores, and hsCRP were all correlated with increased CIMT measurements.
Use of abacavir, lopinavir/ritonavir or indinavir in HIV+ patients was not predictive of CIMT at either the CCA or ICA in HIV+ individuals by either univariate regression or backwards multivariate regression. The duration of HIV infection and T cell nadir were not statistically predictive of CIMT at either CCA or ICA.
CONCLUSION
Today, with HIV suppression, lipid, and hypertension control, HIV+ patients continue to have a disproportionately greater CIMT and calculated heart age than HIV comparators.
Although HIV+ patients generally had lower HDL than their HIV- counterparts, this was not an independent predictor of atherosclerosis in HIV+ patients, in contrast to the HIV- cohort. In the context of LDL control in this HIV+ patient population, LDL size was predictive of ICA CIMT. In the comparator HIV negative population, HDL and Large HDL Particle number was predictive at the CCA CIMT, while LDL number only was predictive at the ICA CIMT. New inflammatory markers like LPLA2 and homocysteine was not predictive of CIMT. Only IL-6 was associated with ICA CIMT in HIV+ patients, whereas hsCRP was associated with ICA in HIV- patients. This contrast in observation from markers associated with cardiovascular mortality in the SMART study (IL-6, d-dimer, hsCRP) may be explained by the reduction of inflammatory markers in the context of HIV suppression in this patient population. Finally, there was no association with atherosclerosis as measured by CIMT with the use of abacavir, or duration of lopinavir or indinavir use, and the D:A:D cardiovascular risk equation was shown to be less predictive than the Framingham risk equation in this HIV+ population.
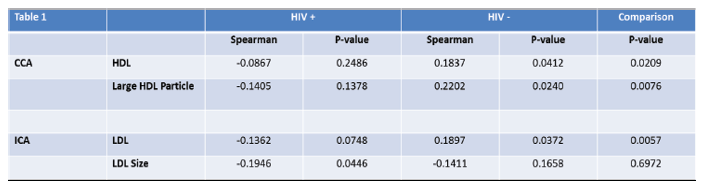
We used Spearman correlations for the analysis of the relationships between CIMT and lipid sub particles. In HIV+ patients, the only statistically significant correlation occurred with ICA measurements and LDL particle size (p=0.04). In HIV- individuals, both HDL (p=0.04) and large HDL particle number (p=0.02) were significantly correlated with CIMT values at the CCA, and LDL (p=0.03) was significantly correlated at the ICA. The only statistically significant differences between HIV+ and HIV- individuals in terms of correlations with CIMT was at HDL (p=0.02) and large HDL particle number (p=0.008) at CCA CIMT, and LDL (p=0.006) with ICA CIMT. (Table 1)
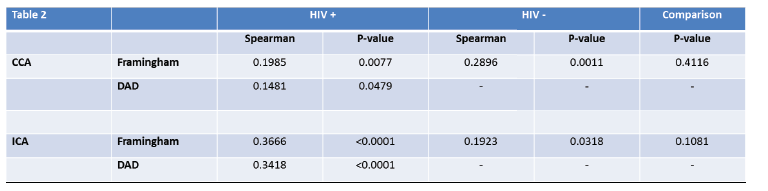
Framingham risk factors were strongly correlated with CIMT at both the CCA (p=0.008) and ICA (p=<0.0001) in both HIV+ and HIV- individuals (CCA p=0.001) and (ICA p=0.03). Interestingly, although the D:A:D risk calculator was just as strongly correlated with ICA CIMT(p<0.0001) as the Framingham risk calculator, it was less correlated with CCA CIMT (p=0.05) than the Framingham risk calculator (p=0.008). The correlations in Framingham risk equations and CIMT were not statistically different between the HIV+ and HIV- groups at both the CCA and ICA. (Table 2)
Use of abacavir, lopinavir/ritonavir, or indinavir in HIV+ patients was not predictive of CIMT at either the CCA or ICA in HIV+ individuals by either univariate regression or backwards multivariate regression. The duration of HIV infection and T cell nadir were not statistically predictive of CIMT at either CCA or ICA.
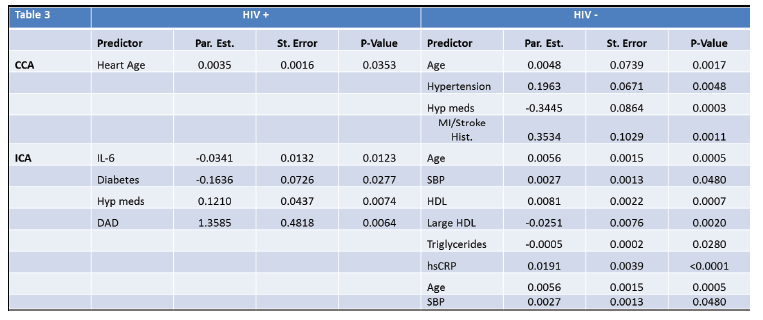
At the CCA, heart age was the only significant predictor for HIV+ patients; however for HIV- patients, age, hypertension, hypertension medications, and history of MI/stroke were all significant predictors of CCA CIMT. At the ICA, IL-6, diabetes, hypertension medications, and D:A:D risk calculator all were significant for HIV+ patients. In contrast, for HIV- patients, age, SBP, HDL, large HDL, triglycerides, and hsCRP were each significant predictors of ICA. (Table 3)
|
| |
|
 |
 |
|
|