 |
 |
 |
| |
Dolutegravir Superior to Darunavir at 48 Weeks in Open-Label ART-Naive Trial (The FLAMINGO Study)
|
| |
| |
53rd ICAAC, September 10-13, 2013, Denver
Mark Mascolini
Dolutegravir, the recently licensed integrase inhibitor, proved superior to darunavir/ritonavir after 48 weeks in previously untreated adults in the FLAMINGO trial [1]. A lower rate of dropouts due to adverse events in the dolutegravir arm and better responses in people with a pretreatment load above 100,000 copies appeared to explain dolutegravir's superiority. Only 2 people in each treatment arm of this 484-person study had confirmed virologic failure.
These FLAMINGO results mark the second time that a randomized trial found dolutegravir superior to another recommended first-line antiretroviral. In the SINGLE trial a dolutegravir regimen was superior to an efavirenz regimen at 48 weeks, and again an adverse-event difference explained the superior outcome with dolutegravir [2]. SINGLE was a double-blind double-dummy trial, while FLAMINGO was open-label. Dolutegravir proved noninferior to raltegravir in the SPRING-2 trial [3].
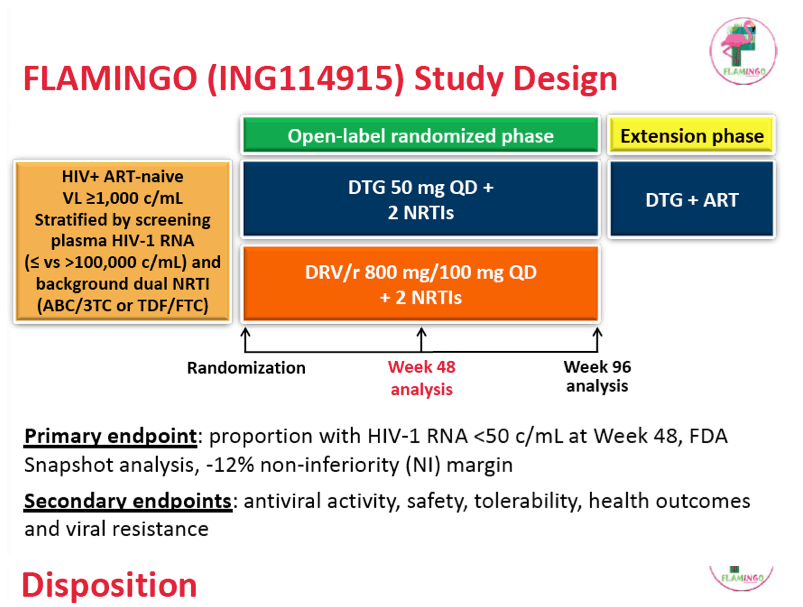
FLAMINGO is a multicenter open-label noninferiority trial that randomized 484 antiretroviral-naive adults to once-daily dolutegravir or darunavir/ritonavir plus investigator-selected tenofovir/emtricitabine or abacavir/lamivudine. No study participants had primary reverse transcriptase or protease mutations upon enrollment, and all had a viral load above 1000 copies. The primary endpoint was the proportion of participants with a 48-week viral load below 50 copies by snapshot analysis.
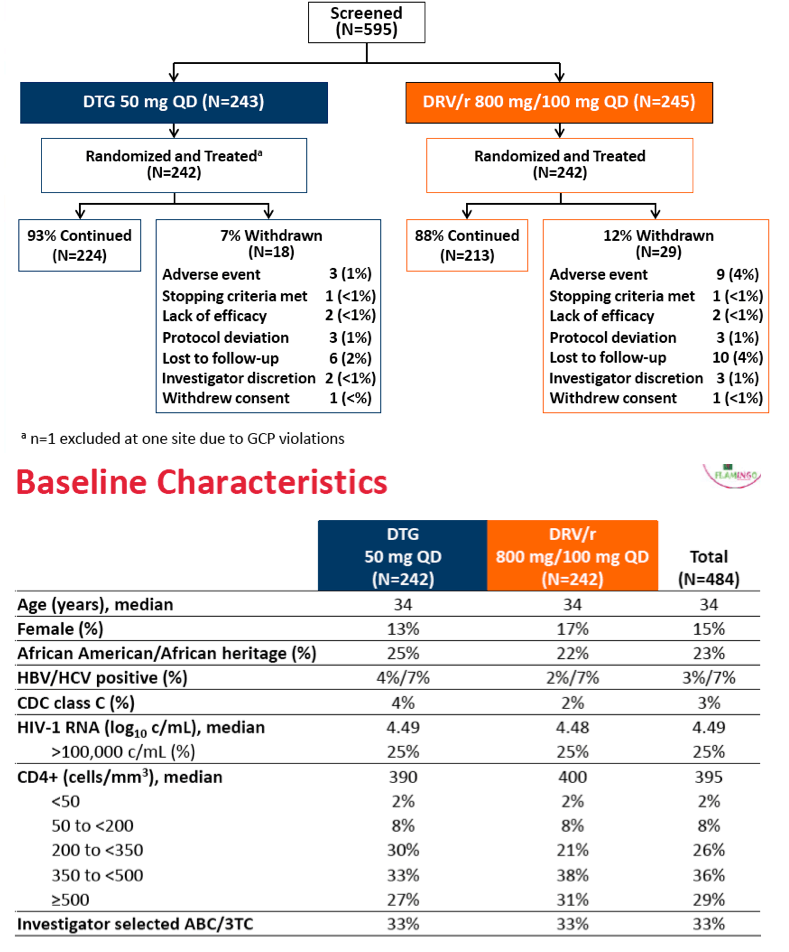
Study participants had a median age of 34, 15% were women, and 28% were nonwhite. One quarter of enrollees had a pretreatment viral load above 100,000 copies, and median pretreatment CD4 count stood at a relatively high 395. One third of participants started abacavir/lamivudine. Baseline characteristics differed hardly at all between treatment arms.
Of the 242 people randomized and treated in the dolutegravir arm, 18 (7%) withdrew, 3 because of an adverse event, 2 because of lack of efficacy, 6 because of loss to follow-up, and 2 because of investigator decision. Of the 242 people randomized and treated in the darunavir arm, 29 (12%) withdrew, 9 because of an adverse event, 2 because of lack of efficacy, 10 because of loss to follow-up, and 3 because of investigator decision.
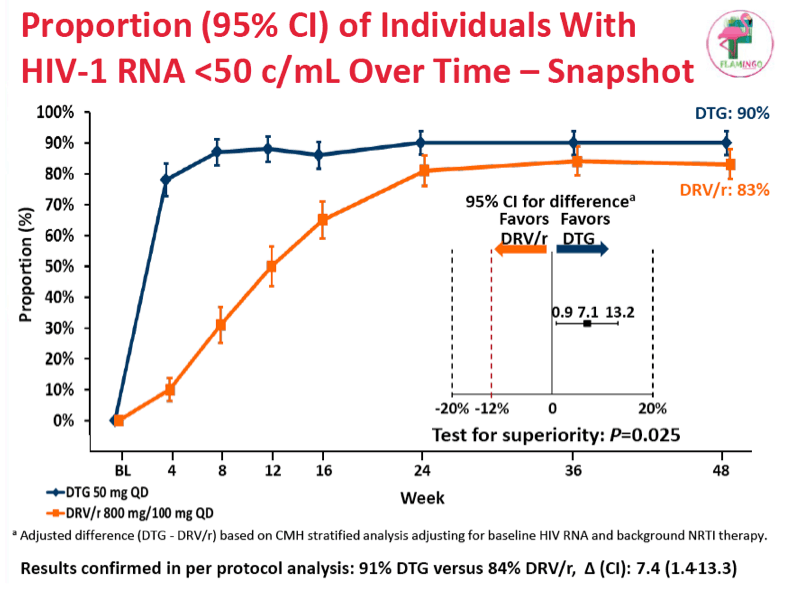
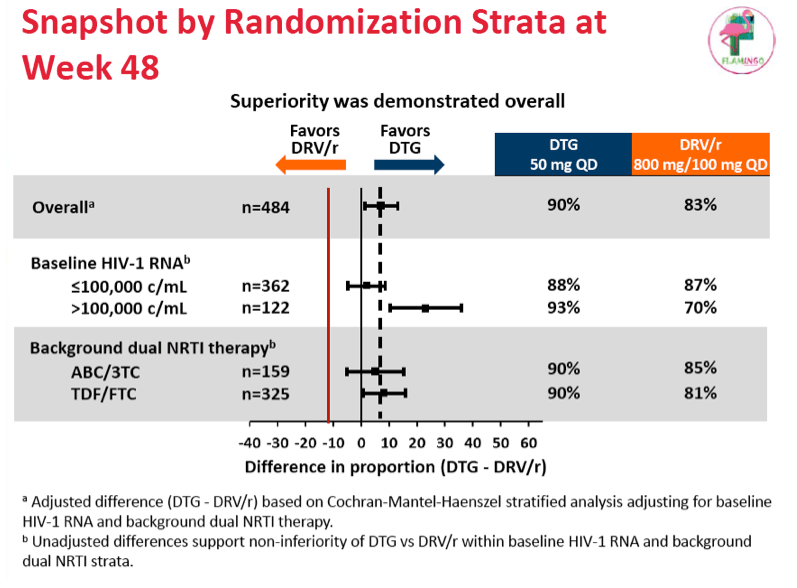
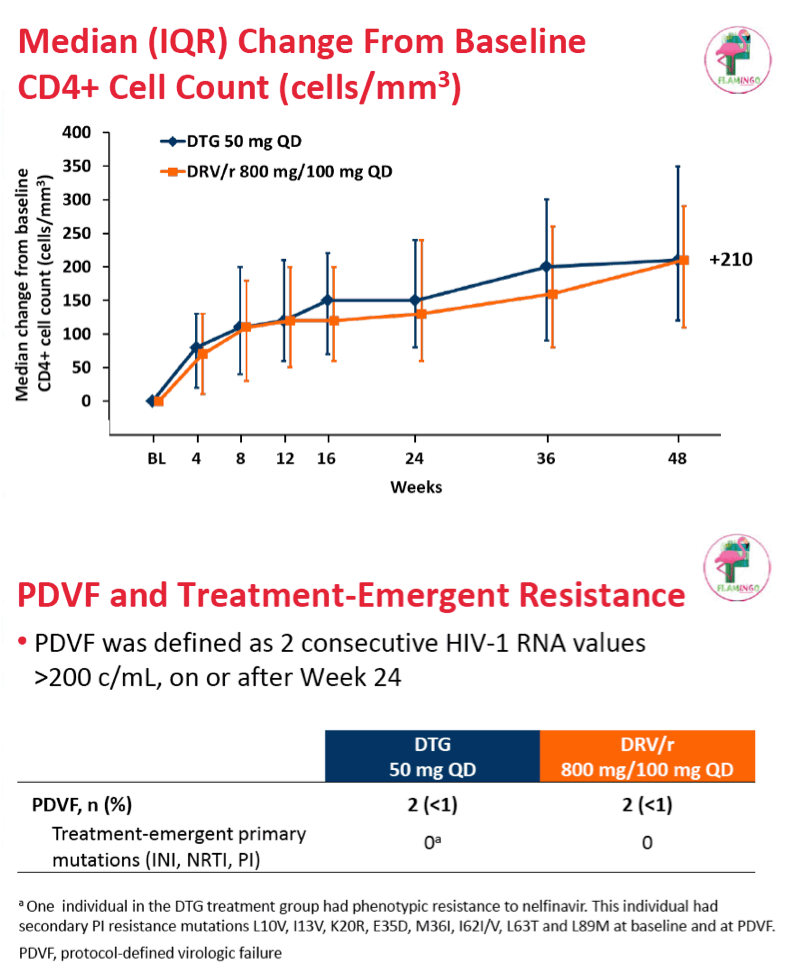
At study week 48 the snapshot analysis determined that 90% randomized to dolutegravir and 83% randomized to darunavir/ritonavir had a viral load below 50 copies. The adjusted difference of 7.1% (95% confidence interval 0.9% to 13.2%) established the superiority of dolutegravir to darunavir/ritonavir in previously untreated adults (P = 0.025). In a per protocol analysis, 91% randomized to dolutegravir and 84% randomized to darunavir had a viral load below 50 copies at week 48 (difference 7.4%, 95% confidence interval 1.4% to 13.3%). Confirmed virologic failure (a viral load above 200 copies) occurred in 2 people in each study arm, and no primary integrase, reverse transcriptase, or protease mutations arose in either arm.
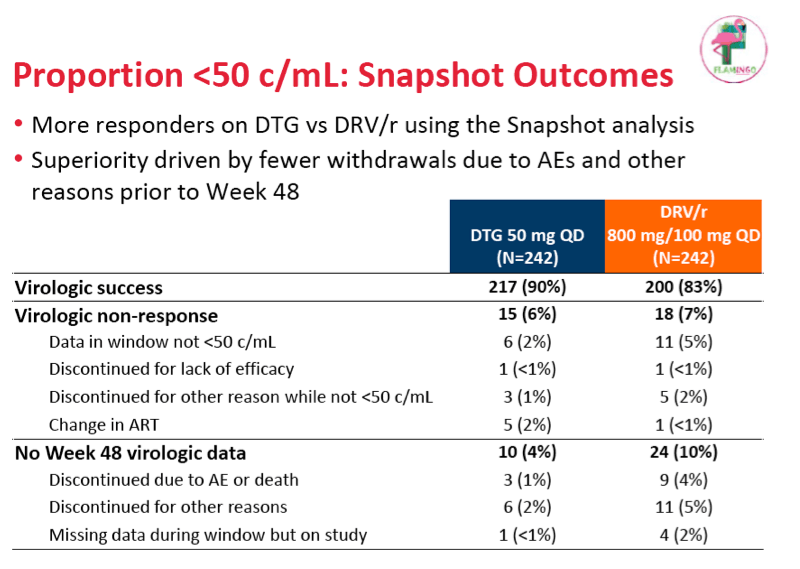
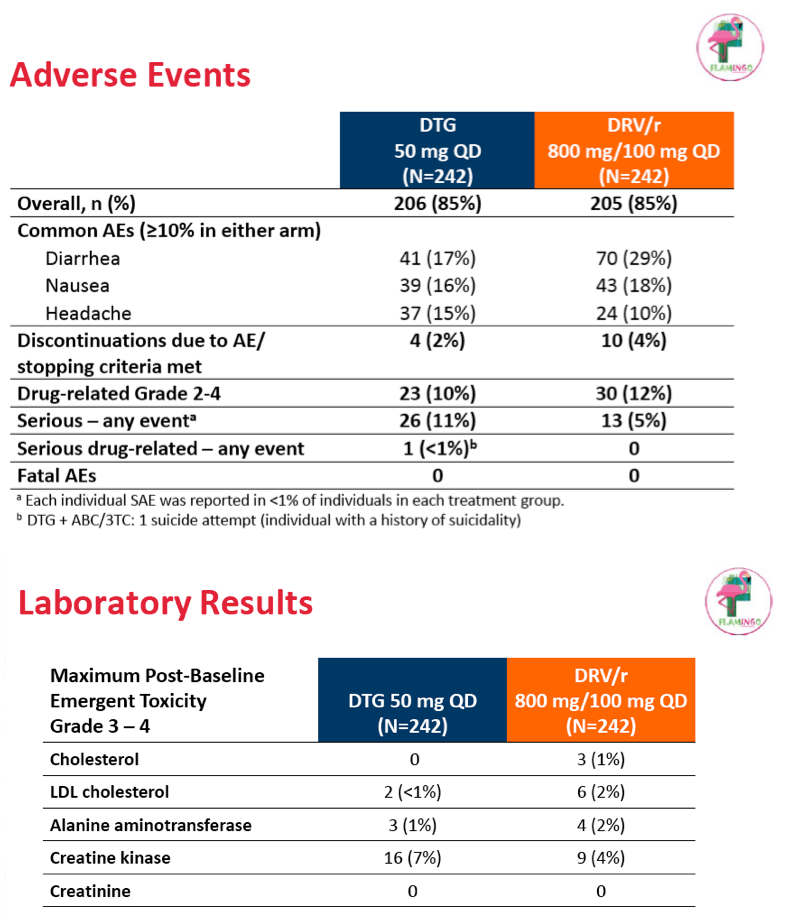
The investigators proposed that the superiority of dolutegravir to darunavir reflected fewer withdrawals due to adverse events and other reasons before week 48 in the dolutegravir arm and a better dolutegravir response rate among people starting treatment with a viral load above 100,000 copies. Nine people (4%) withdrew from the darunavir group because of an adverse event or death, compared with 3 (1%) from the dolutegravir arm. Drug-related grade 2 to 4 adverse events affected 30 people in the darunavir arm (12%) and 23 in the dolutegravir arm (10%).
Among people with a pretreatment load below 100,000 copies, snapshot analysis determined a 48-week sub-50-copy response rate of 88% in the dolutegravir group and 87% in the raltegravir group. Among people with a pretreatment load above 100,000 copies, 48-week sub-50 response rates were 93% with dolutegravir and 70% with darunavir/ritonavir. Whether a person took abacavir/lamivudine or tenofovir/emtricitabine did not affect virologic results.
Participants randomized to dolutegravir had significantly fewer grade 2 or worse low-density lipoprotein cholesterol values (2% versus 7%, P < 0.001). Among other adverse events affecting 10% or more study participants, diarrhea proved less frequent with dolutegravir than with darunavir/ritonavir (17% versus 29%), headache was somewhat more frequent with dolutegravir (15% versus 10%), and nausea affected similar proportion in each treatment arm (16% versus 18%).
Median CD4 gain measured 210 in both treatment groups.
Session attendees wondered whether the open-label trial design favored dolutegravir. Perhaps people enrolled in the trial hoping to get randomized to the then-investigational integrase inhibitor. Some randomized to the already licensed darunavir may have dropped out in disappointment. But Judith Feinberg, who presented the data, said withdrawals did not occur predominantly in the early weeks of the trial, as one would expect with a disappointed-patient scenario.
References
1. Feinberg J, Clotet B, Khuong MA, et al. Once-daily dolutegravir is superior to darunavir/ritonavir in antiretroviral naive adults: 48 week results from FLAMINGO (ING114915). 53rd ICAAC. September 10-13, 2013. Denver. Abstract H-1464a.
2. Walmsley S, Antela A, Clumeck N, et al. Dolutegravir (DTG; S/GSK1349572) + abacavir/lamivudine once daily statistically superior to tenofovir/emtricitabine/efavirenz: 48-week results--SINGLE (ING114467). 52nd Interscience Conference on Antimicrobials and Chemotherapy (ICAAC). September 9-12, 2012. San Francisco. Abstract H-556b. http://www.natap.org/2012/ICAAC/ICAAC_29.htm
3. Raffi F, Rachlis A, Stellbrink HJ, et al. Once-daily dolutegravir versus raltegravir in antiretroviral-naive adults with HIV-1 infection: 48 week results from the randomised, double-blind, non-inferiority SPRING-2 study. Lancet. 2013;381:735-743. www.natap.org/2013/HIV/PIIS0140673612618534-2.pdf
--------------------------------------


|
| |
|
 |
 |
|
|