 |
 |
 |
| |
Low Risk but Twice Higher Risk of Suicidal Thoughts or Acts on First-Line Efavirenz
|
| |
| |
IDWeek, October 2-6, 2013, San Francisco
AUTHOR SUMMARY: (1) Suicidality was uncommon, but reported in each study and subgroup evaluated; (2) Two-fold increase in risk of suicidality with EFV among patients beginning ART (NNH* ~217 with EFV); (3) ~2.5 fold higher risk of attempted or completed suicide (NNH* ~538 with EFV); (4) EFV treatment, younger age, IDU history, and psychiatric history were associated with a higher risk of suicidality; (5) Death from suicide, injury, or unknown causes paralleled suicidality results, careful attention should be paid to cause of death ascertainment in all clinical trials
Mark Mascolini
People starting antiretroviral therapy with an efavirenz regimen had about a twice higher risk of suicidal thoughts of acts (suicidality) than people taking a nonefavirenz regimen in a 5332-person analysis [1]. The suicidality rate was low even in efavirenz takers at 8 events per 1000 person years.
Efavirenz is well known for its neurologic side effects, including depression. But whether it affects risk of suicidality remains unclear. Prescribing information for efavirenz says postmarketing reports cannot establish a causal relationship between efavirenz and suicide but recommends immediate evaluation of people with serious psychiatric symptoms. A 2011 literature review concluded "there is no clear evidence of a broadly increased risk of suicide or dangerous behavior" in people taking efavirenz [2].
To address this issue, AIDS Clinical Trials Group (ACTG) investigators compared people randomized to efavirenz or nonefavirenz first-line regimens in four ACTG trials during 2001-2007: A5095, A5142, A5175, A5202. Three of these trials were unblinded, three had comparison arms using atazanavir/ritonavir or lopinavir/ritonavir, and one had a triple-nucleoside comparison arm (abacavir, zidovudine, and lamivudine). The investigators used Cox proportional hazards models to determine hazard ratios for suicidality. The primary analysis included follow-up through last study contact or data and safety monitoring board recommendation to stop a nonefavirenz arm because of virologic inferiority, which happened in two trials. The ACTG team defined suicidality as a composite endpoint including suicidal ideation and attempted or completed suicide.
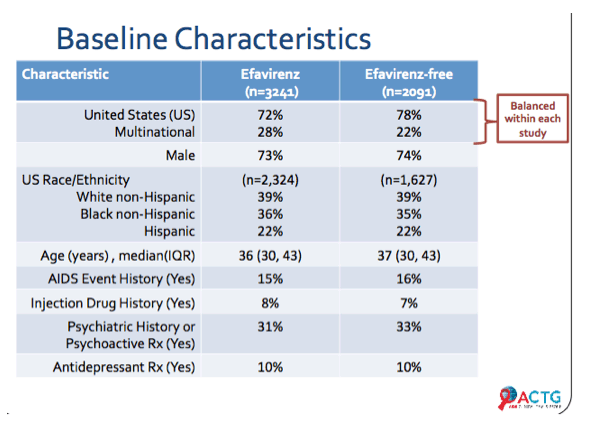
The analysis involved 3241 people randomized to efavirenz and 2091 randomized to comparison regimens. About three quarters of study participants lived in the United States and about three quarters were men. Race/ethnicity distributions were nearly identical in the efavirenz and nonefavirenz arms: 39% and 39% white, 36% and 35% black, and 22% and 22% Hispanic. Median age stood at 36 in the efavirenz group (interquartile range [IQR] 30 to 43) and 37 in the comparison group (IQR 30 to 43). Fewer than 10% in each group had injected drugs, about one third in each group had a prestudy psychiatric event or took psychoactive drugs in the 30 days before study entry, and 10% in each group had taken antidepressants.
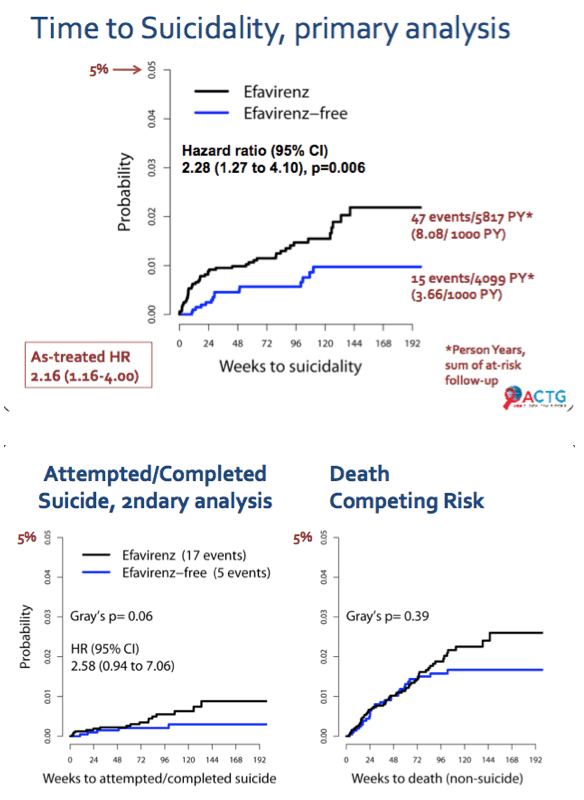
After a median follow-up of 150 weeks, there were 47 cases of suicidality in the efavirenz group and 15 in the comparison group for incidence rates of 8.08 and 3.66 per 1000 person-years. (An incidence of 8.08 per 1000 person-years means 8 of every 1000 people taking efavirenz contemplated or tried suicide every year.) In the primary analysis people randomized to efavirenz had more than a doubled risk of suicidality (hazard ratio [HR] 2.28, 95% confidence interval [CI] 1.27 to 4.10, P = 0.006). In an as-treated analysis follow-up stopped when antiretrovirals stopped or people taking efavirenz switched to another regimen. In this analysis suicidality risk was still more than twice higher in the efavirenz group (HR 2.16, 95% CI 1.16 to 4.00).
Focusing only on attempted and completed suicides, the investigators counted 17 events in the efavirenz group and 5 in the comparison group, which again translated into more than a doubled risk of with efavirenz. But this association stopped short of statistical significance (HR 2.58, 95% CI 0.94 to 7.06, P = 0.06). In an intention-to-treat analysis including all follow-up, the ACTG team counted 27 attempts or suicides in the efavirenz group and 7 in the comparison group, and in this analysis the risk was significantly greater with efavirenz (HR 2.61, 95% CI 1.1 to 5.9, P = 0.03).When the investigators assessed suicidality risk by trial country, the risk was significantly higher with efavirenz in the United States (HR 2.32, 95% CI 1.23 to 4.38) but not in other countries (HR 2.02, 95% CI 0.43 to 9.53).
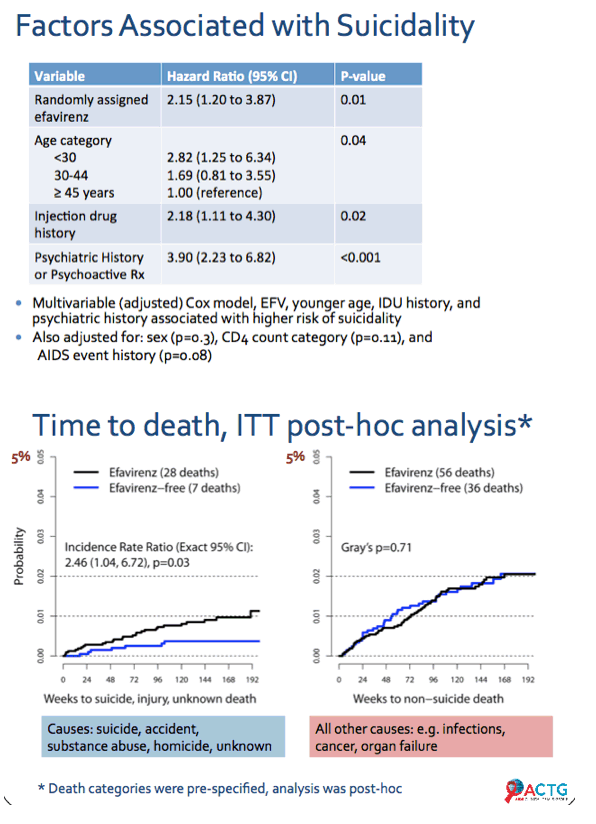
A multivariable Cox model identified four factors independently associated with suicidality:
-- Randomized to efavirenz: HR 2.15, 95% CI 1.20 to 3.87, P = 0.01
-- Age under 30 versus 45 or older: HR 2.82, 95% CI 1.25 to 6.34, P = 0.04
-- Injection drug history: HR 2.18, 95% CI 1.11 to 4.30, P = 0.02
-- Psychiatric history or psychoactive drug use: HR 3.90, 95% CI 2.23 to 6.82, P < 0.001
The researchers also found that death from suicide, injury, or unknown causes paralleled suicidality results. They urged "careful attention" to causes of death in all clinical trials. And they recommended that people treated with efavirenz "should be carefully monitored for suicide risk."
References
1. Mollan K, Smurzynski M, Na L, et al. Hazard of suicidality in patients randomly assigned to efavirenz for initial treatment of HIV-1: a cross-study analysis conducted by the AIDS Clinical Trials Group (ACTG). IDWeek 2013. October 2-6, 2013. San Francisco. Abstract 670.
2. Kenedi CA, Goforth HW. A systematic review of the psychiatric side-effects of efavirenz. AIDS Behav. 2011;15:1803-1818.
----------------------------------------
Reported by Jules Levin







|
| |
|
 |
 |
|
|