 |
 |
 |
| |
Higher Frailty Index Tied to Lower Odds of Successful Cognitive Aging in HIV+ Over 50
|
| |
| |
5th International Workshop on HIV and Aging. October 20-21, 2014. Baltimore
Mark Mascolini
Higher (worse) frailty index scores lowered chances of successful cognitive aging in an Italian cohort of HIV-positive people 50 and older [1]. Only one of eight non-AIDS condition--hypertension--predicted successful cognitive aging, defined as absence of depression, cognitive impairment, or functional disability.
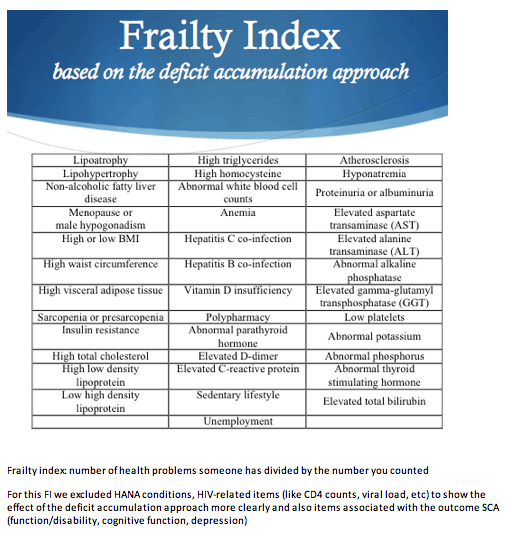
The frailty index used in this study is a score representing the proportion of clinical deficits or lab abnormalities a person has from a list of 30 or more health variables. Possible scores range from 0 (least frail) to 1.0 (most frail). Researchers from Canada and Italy who conducted this study argued that the frailty index permits an overall frailty grading that may be more informative than a one-by-one accounting of individual disorders.
These investigators observed that a higher frailty index score has been linked to neurocognitive impairment in the general population, but the index has not been closely evaluated in people with HIV. This cross-sectional study aimed to assess associations between the frailty index, single or multiple non-AIDS conditions, and successful cognitive aging in a cohort of antiretroviral-treated older adults.
Health workers at the Modena HIV Metabolic Clinic invited consecutive community-dwelling patients 50 or older to enroll in the study. Participants had to be taking antiretroviral therapy for at least 1 year and have an undetectable viral load. No one could have acute psychotic disorders, severe neurologic disease, or end-stage organ failure that could affect neurocognition.
The investigators calculated frailty as the proportion of 37 health variables detected.* Those variables did not include markers of HIV disease severity, immune deficiency, HIV-associated non-AIDS diagnoses, or cognitive impairment. The research team also itemized eight non-AIDS conditions in each person--cardiovascular disease, hypertension, diabetes, chronic kidney disease, liver cirrhosis, chronic obstructive pulmonary disease, osteoporosis, and cancer. They recorded the presence of multimorbidity in each person, defined as diagnosis of 2 or more non-AIDS conditions. Multivariate logistic regression analysis adjusted for age and gender assessed the odds of successful cognitive aging in relation to (1) each of the non-AIDS conditions separately, (2) multimorbidity, and (3) frailty index in increments of 0.1.
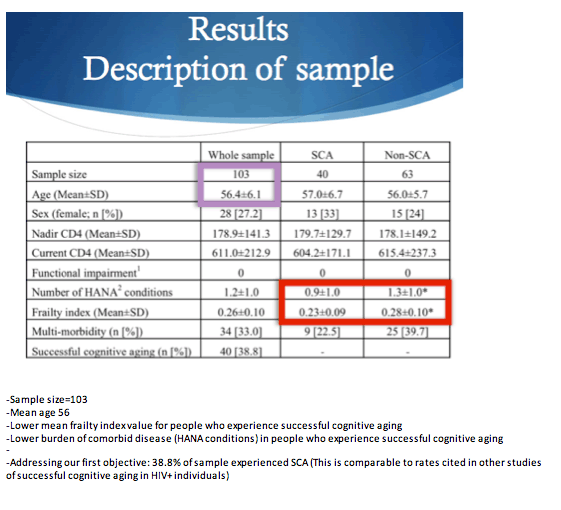
The 103 study participants averaged 56.4 years in age (+/- 6.1) and 28 of them (27%) were women. Forty people (39%) had successful cognitive aging. Chronological age was similar in people with and without successful cognitive aging (average 57.0 and 56.0). Successful agers included a higher proportion of women (33% versus 24%).
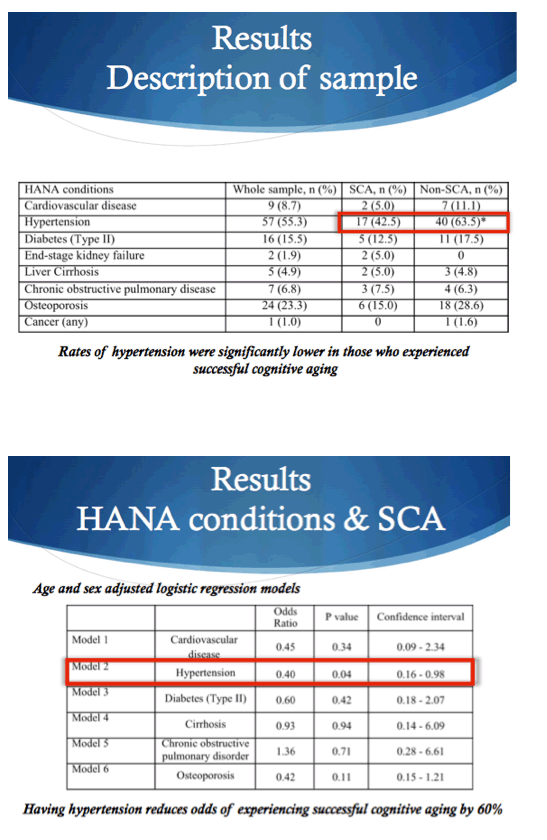
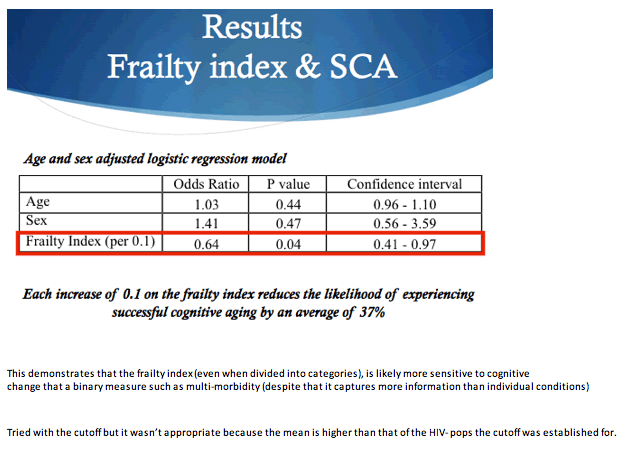
Average frailty index was significantly lower (better) in the 40 people with successful cognitive aging than in the 63 other participants (0.23 +/- 0.09 versus 0.28 +/- 0.10). Successful cognitive agers also had a significantly lower average number of the 8 non-AIDS conditions (0.9 +/- 1.0 versus 1.3 +/- 1.0). A significantly lower proportion of successful agers had hypertension (42.5% versus 63.5%), but successful and unsuccessful agers did not differ significantly in frequency of any other non-AIDS condition.
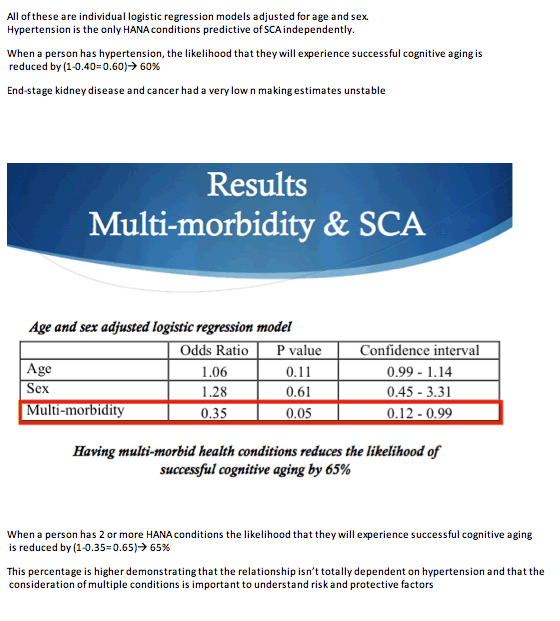
After statistical adjustment for age and gender, having hypertension lowered chances of successful cognitive aging 60% (odds ratio [OR] 0.40, 95% confidence interval [CI] 0.16 to 0.98, P = 0.04). No other non-AIDS condition affected odds of successful cognitive aging. Multimorbidity (2 or more non-AIDS conditions) cut chances of successful cognitive aging 65% (OR 0.35, 95% CI 0.12 to 0.99, P = 0.05).
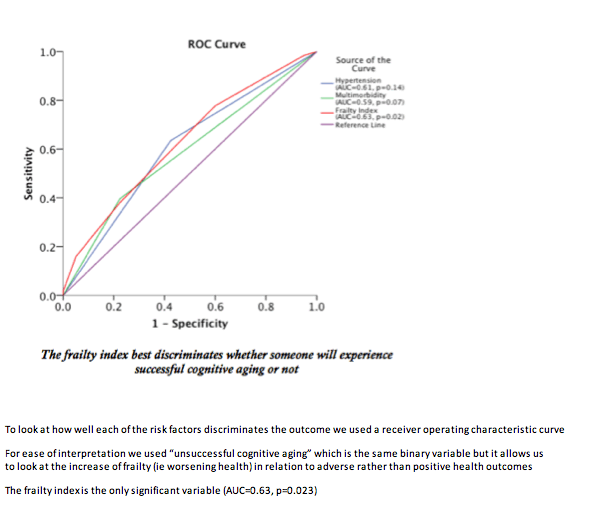
After adjustment for age and gender, every 0.1 higher (worse) frailty index lowered odds of successful cognitive aging 36% (OR 0.64, 95% confidence interval 0.41 to 0.97, P = 0.04). In a receiving operating characteristic (ROC) curve analysis, the frailty index emerged as the only significant variable predicting unsuccessful cognitive aging (area under the curve 0.63, P = 0.023). In the same analysis, hypertension and multimorbidity were not significant predictors of unsuccessful cognitive aging.
The researchers concluded that "the fragility index can be useful in grading levels of frailty and provides more information than . . . individual age-related disease diagnoses or chronological age." They proposed that "considering health status and frailty in a more holistic sense may be useful in the understanding of successful cognitive aging among people living and aging with HIV."
Reference
1. Wallace L, Ferrara M, Brothers T, et al. Lower frailty index is associated with successful cognitive aging among HIV-positive adults age 50 and older. 5th International Workshop on HIV and Aging. October 20-21, 2014. Baltimore. Abstract 9.
*Items in the index included body mass index; variables related to body fat; lipids; numerous common lab values like AST, GGT, bilirubin, and potassium; comorbidities like HBV, HCV, and atherosclerosis; polypharmacy; sedentary lifestyle, and unemployment.



|
| |
|
 |
 |
|
|