 |
 |
 |
| |
Post-SVR Liver Decompensation Rate Similar With HCV/HIV and HCV Alone
|
| |
| |
CROI 2014, March 3-6, 2014, Boston
Mark Mascolini
Liver decompensation risk after achieving sustained virologic response (SVR) with interferon-based therapy did not differ substantially between people coinfected with HCV and HIV and those infected with HCV alone, according to results of a 12,000-person Veterans Administration (VA) study [1]. In both coinfected and monoinfected people, decompensation rates were significantly higher in those who did not attain SVR than in those who did.
Research has not rigorously addressed the impact of SVR on subsequent liver complications, especially in people coinfected with HCV and HIV. To assess rates of hepatic decompensation after SVR in HCV/HIV-coinfected people versus monoinfected individuals, researchers from several institutions collaborated on this retrospective analysis of patients treated in the VA system between October 2005 and February 2012.
All cohort members analyzed had received interferon-based therapy, had HCV viremia, and had received VA care for at least 12 months. The researchers excluded people who already had decompensation or HBV infection. Follow-up began the day when HCV therapy started and continued until decompensation, death, or February 28, 2012. The investigators defined decompensation as one hospital diagnosis or at least two outpatient diagnoses of ascites, spontaneous bacterial peritonitis, or esophageal variceal hemorrhage. They defined SVR as undetectable HCV RNA 12 weeks after treatment stopped. Cox regression analysis to determine hazard ratios for decompensation adjusted for age, ethnicity, baseline HCV RNA load, diabetes, and alcohol abuse or dependence.
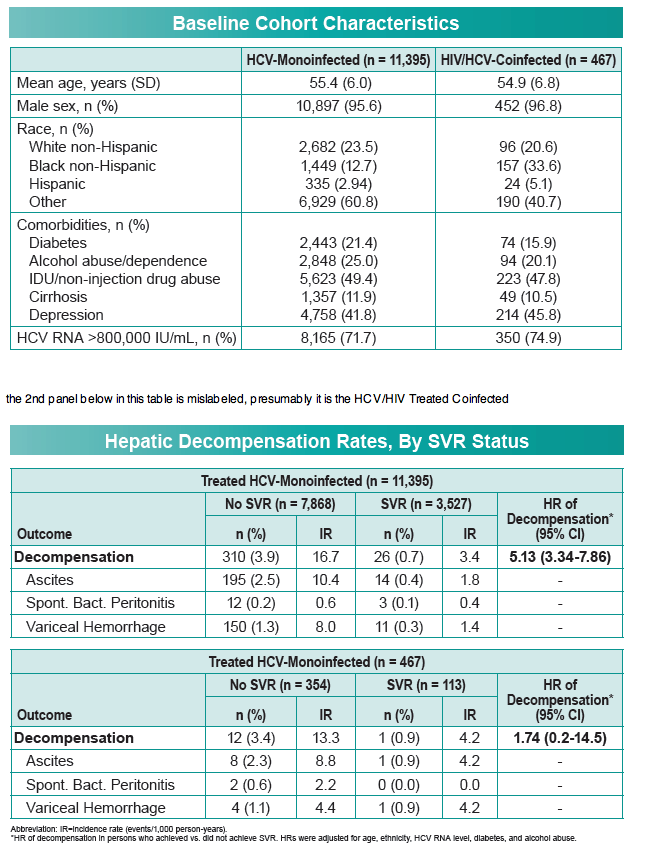
The analysis included 467 HCV/HIV-infected veterans and 11,395 infected only with HCV. More than 95% in each group were men. Proportions of non-Hispanic blacks in the coinfected and monoinfected groups were 33.6% and 12.7%, proportions of non-Hispanic whites 20.6% and 23.5%, and proportions of Hispanics 5.1% and 2.9%. (Large proportions in both groups were racially classified as "other.") Similar proportions in the coinfected and monoinfected groups had diabetes (15.9% and 21.4%), alcohol abuse or dependence (20.1% and 25.0%), injection or noninjection drug abuse (47.8% and 49.4%), cirrhosis (10.5% and 11.9%), and depression (45.8% and 41.8%). About three quarters of the coinfected and monoinfected groups had an HCV load above 800,000 IU/mL (74.9% and 71.7%).
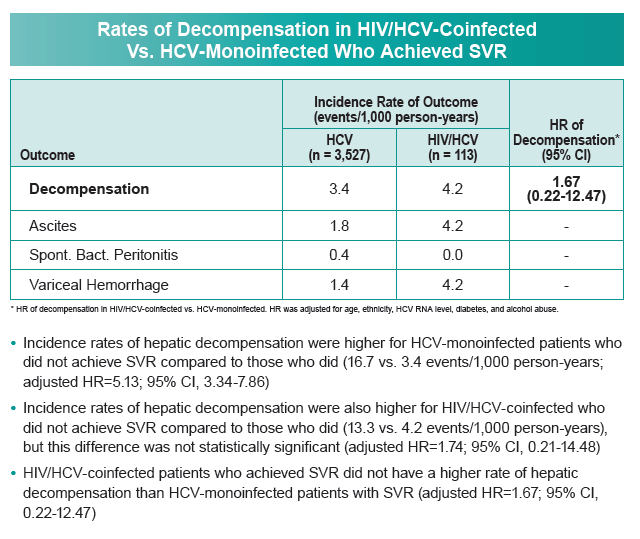
Among HCV/HIV-coinfected people, decompensation incidence was 4.2 per 1000 person-years in people who achieved SVR versus 13.3 per 1000 in people without SVR. Those rates translated into a 74% higher adjusted decompensation risk in people without SVR (hazard ratio [HR] 1.74, 95% confidence interval [CI] 0.2 to 14.5). Among HCV-monoinfected people, decompensation incidence with and without SVR was 3.4 and 16.7 per 1000 person-years, which meant monoinfected people without SVR had more than a 5 times higher risk of decompensation (HR 5.13, 95% CI 3.34 to 7.86).
Comparing decompensation incidence in coinfected and monoinfected people who achieved SVR (4.2 versus 3.4 per 1000 person-years), the investigators determined that incidence was not significantly higher in the coinfected group because the confidence interval for the adjusted hazard ratio crossed 1.0 (HR 1.67, 95% CI 0.22 to 12.47).
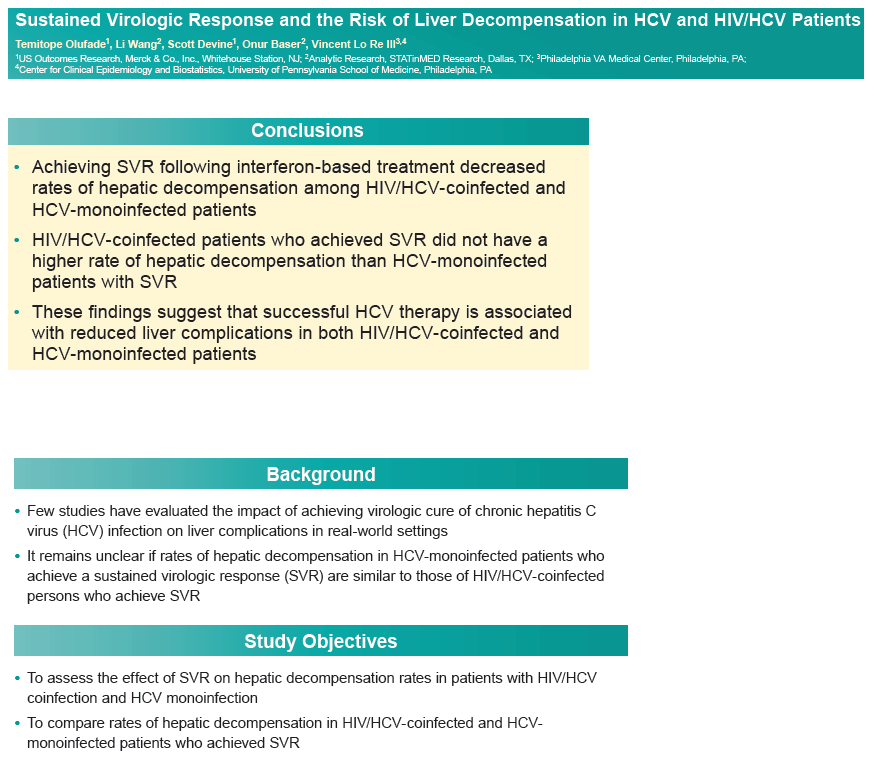
The researchers believe their findings "suggest that successful HCV therapy is associated with reduced liver complications in both HIV/HCV-coinfected and HCV-monoinfected patients."
Reference
1. Olufade TO, Wang L, Devine S, Baser O, Lo Re V. Sustained virologic response and the risk of liver decompensation in HCV and HIV/HCV patients. CROI 2014. Conference on Retroviruses and Opportunistic Infections. March 3-6, 2014. Boston. Abstract 641.
--------------------------------------------
Reported by Jules Levin
Hepatic Decompensation Rates, By SVR Status

|
| |
|
 |
 |
|
|