 |
 |
 |
| |
Brain Markers of Inflammation Drop to Normal With Early ART
|
| |
| |
CROI 2014, March 3-6, 2014, Boston
Mark Mascolini
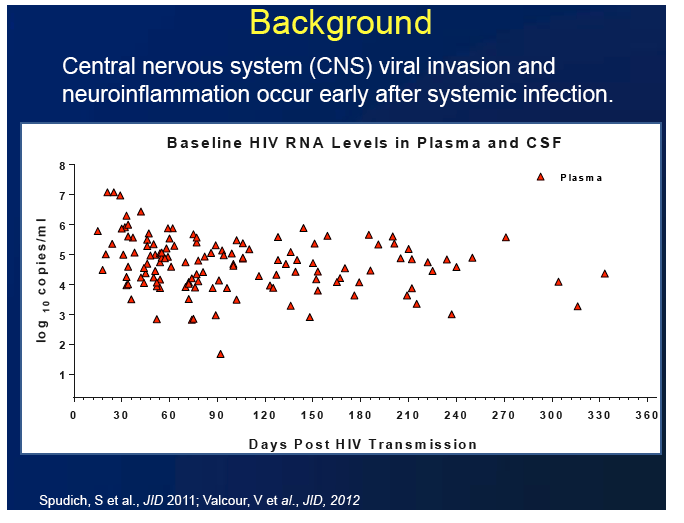
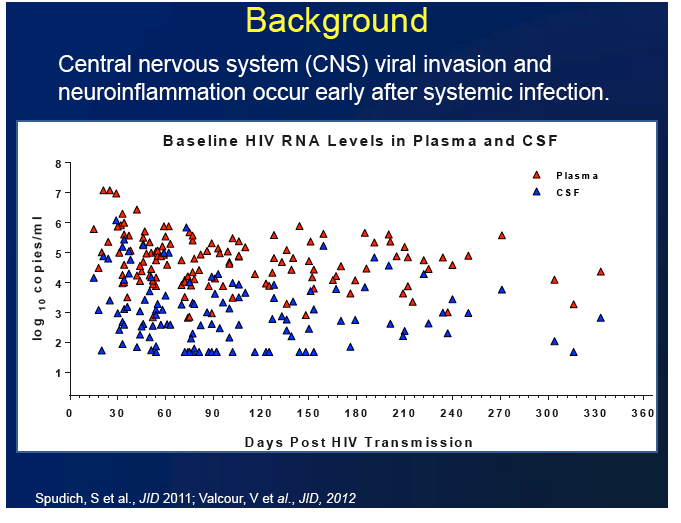
Antiretroviral therapy (ART) begun soon after HIV infection dampened central nervous system (CNS) inflammation in a study of 26 recently infected people in San Francisco [1]. Cerebrospinal fluid (CSF) markers of inflammation returned to normal about 9 months after these people started ART, whereas ART begun during chronic infection has not had this effect.
Markers of CNS inflammation typically remain abnormally high in people responding well to ART begun during chronic HIV infection. Julia Peterson (University of California, San Francisco) and collaborators conducted this study to determine how ART begun soon after HIV infection affects standard markers of inflammation in the CNS.
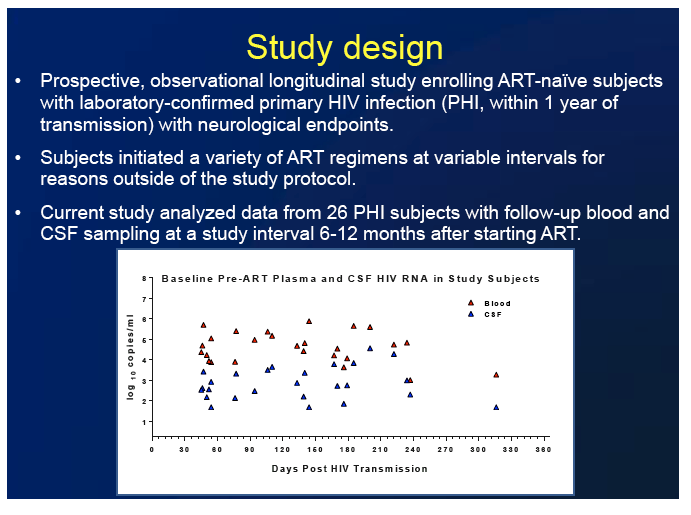
This longitudinal observational study involved antiretroviral-naive people with primary HIV infection, defined as infection within the year after transmission. These people started diverse ART regimens at different intervals after infection for reasons not related to this study. Peterson and colleagues analyzed data from 26 people with pretreatment blood and CSF samples as well as follow-up samples collected at intervals 6 to 12 months after they started ART. The investigators measured the following indicators:
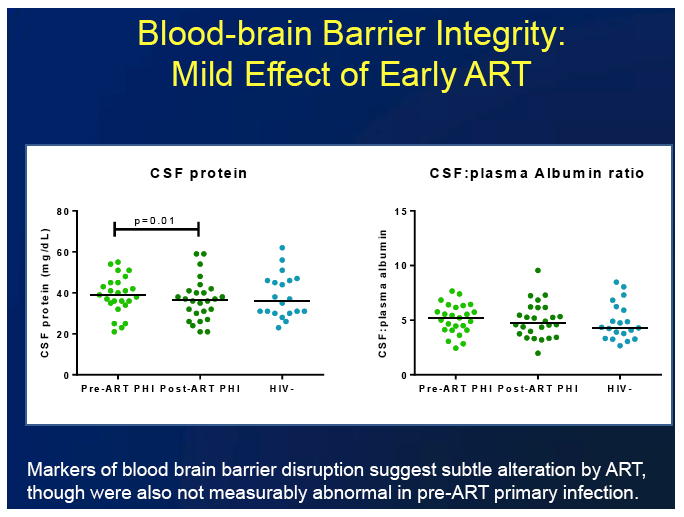
-- CSF/plasma albumin ratio and CSF protein, markers of blood-brain barrier disruption
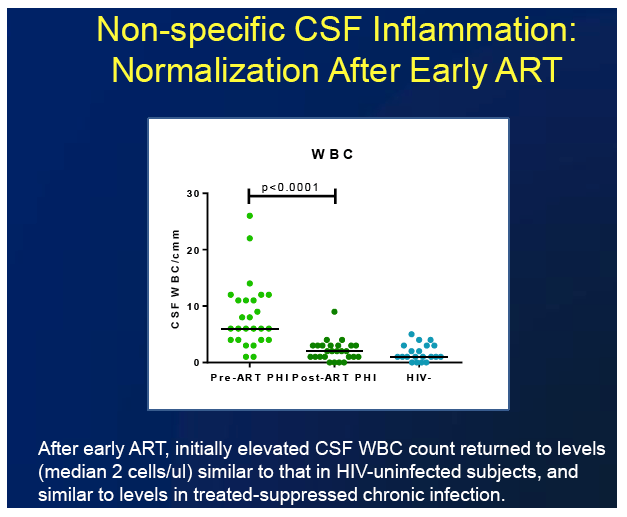
-- CSF white blood cells (WBC), a marker of CNS inflammation
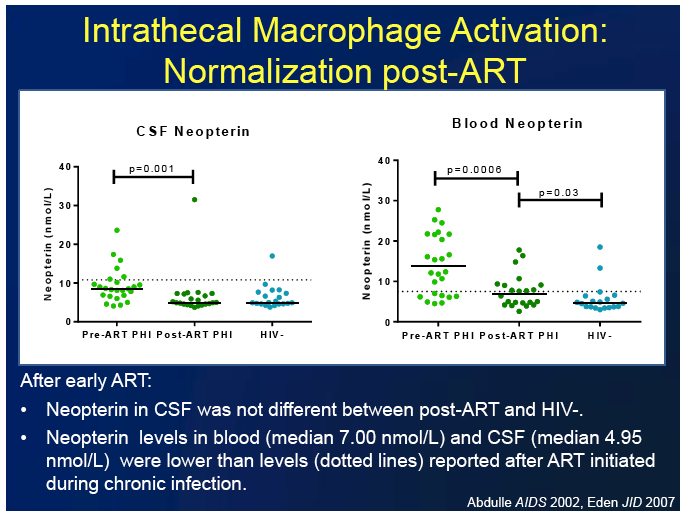
-- CSF and plasma neopterin, markers of immune activation, particularly macrophage activation
The researchers compared these values with those in 20 age-matched HIV-negative controls.
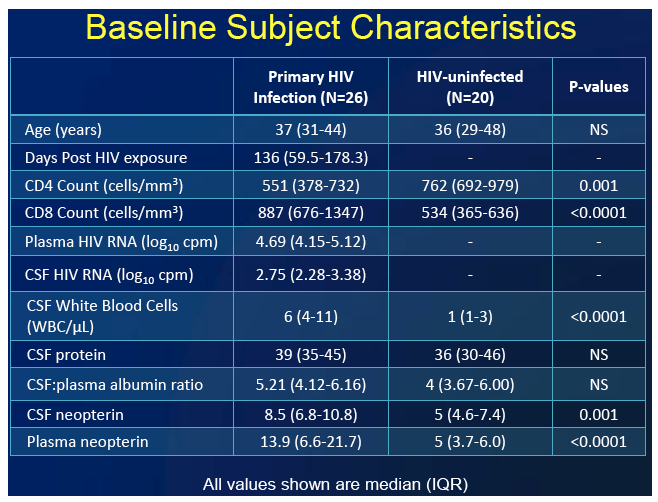
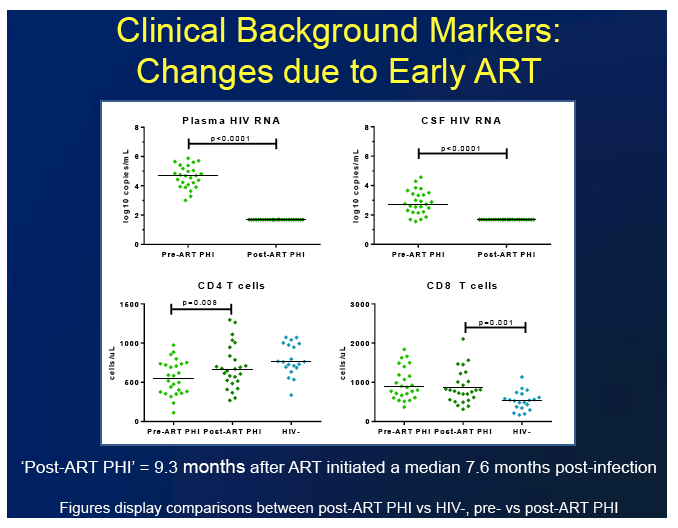
The 26 people with HIV had a median age of 37 (interquartile range [IQR] 31 to 44) and had HIV infection for a median of 136 days (IQR 59.5 to 178.3). The HIV group's median CD4 count was significantly lower than that of the 20 HIV-negative controls, but four values were significantly higher in the HIV group: CD8 count, CSF WBC, CSF neopterin, and plasma neopterin. CSF protein and CSF/plasma albumin ratio were nonsignificantly higher in the HIV group.
Participants began ART a median of 229 days (IQR 119.5 to 741.8) after HIV infection. The first on-treatment visit came a median of 278.5 days (IQR 199.5 to 369.3) after people started ART. Median antiretroviral CNS penetration effectiveness score of regimens was high at 7 (IQR 7 to 7).
Viral load in plasma and CSF both dropped significantly a median of 9.3 months after ART began (P < 0.0001). CSF protein also fell significantly after ART began (P = 0.01), while the CSF/plasma albumin ratio fell nonsignificantly. CSF WBC declined significantly after ART started (P < 0.0001), returning to levels recorded in HIV-negative people (median 2 cells/uL).
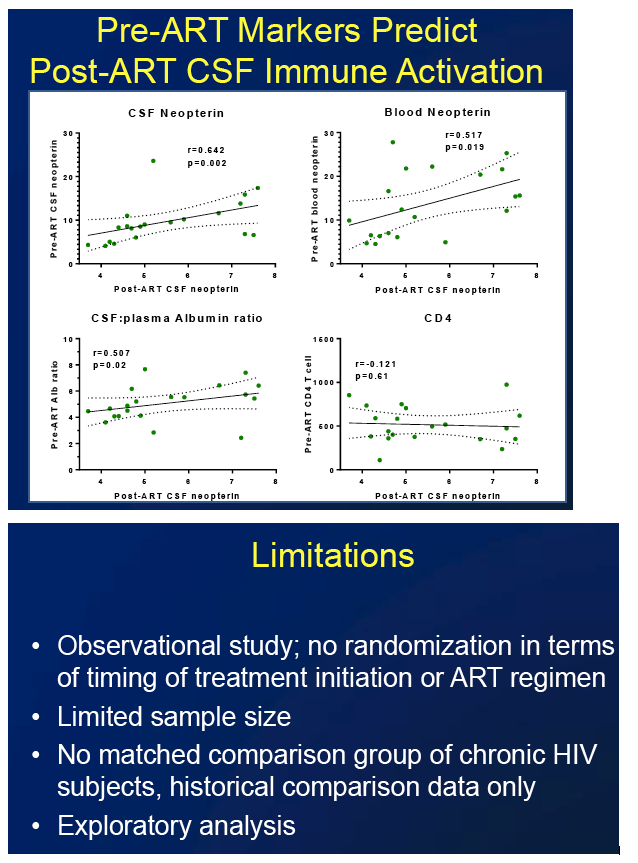
CSF neopterin fell significantly with ART (P = 0.001) to levels equivalent to those in HIV-negative controls. After treatment began, neopterin levels in blood and CSF were lower than those recorded in a historical comparison group of people who began ART during chronic infection. Pre-ART levels of CSF neopterin, plasma neopterin, and CSF/plasma albumin ratio correlated with on-ART CSF neopterin.
Peterson and colleague concluded that CNS inflammation markers abnormally high during primary infection returned to normal within 1 year of starting ART. Specifically, they observed that "CNS immune activation markers measured 9 months after early ART were similar to those in HIV-negative controls" and that "CSF neopterin after early ART was lower than that reported after treatment initiated during chronic HIV infection."
Noting that these findings contrast with earlier reports of persistent CNS immune activation when treatment begins during chronic infection, the researchers suggested their results may indicate another benefit of starting ART early in the course of infection.
Reference
1. Peterson J, Lee E, Fuchs D, Price RW, Spudich S. Early antiretroviral therapy appears to normalize intrathecal markers of immune activation. CROI 2014. Conference on Retroviruses and Opportunistic Infections. March 3-6, 2014. Boston. Abstract 35.
-----------------------
CROI Webcast Link:
http://www.croiwebcasts.org/console/player/22054?mediaType=slideVideo&





|
| |
|
 |
 |
|
|