 |
 |
 |
| |
Early Adopters: Socio-demographic and Behavioral Correlates of Chemoprophylaxis Use in a Recent National Online Sample of Men who have Sex with Men in the U.S.
|
| |
| |
Reported by Jules Levin
CROI 2014 March 3-6 Boston, MA
Kenneth H. Mayer1,2,3, Catherine E. Oldenburg4, David S. Novak5, Steven A. Elsesser1, Douglas S. Krakower2, Matthew J. Mimiaga1,4,6
1 The Fenway Institute, Fenway Community Health, Boston, MA; 2 Department of Medicine, Beth Israel Deaconess Medical Center, Boston, MA;
3 Department of Global Health and Population, Harvard School of Public Health, Boston, MA; 4 Department of Epidemiology, Harvard School of Public Health, Boston, MA; 5 Online Buddies Research Institute, Cambridge, MA; 6 Department of Psychiatry, Massachusetts General Hospital, Boston, MA

Program Abstract-
Background: Although HIV pre-exposure prophylaxis (PrEP) use has been shown to decrease HIV
incidence among men who have sex with men (MSM), uptake has not been widespread, and the
demographics and behaviors of those who initiated PrEP outside of studies is not well known.
Methodology: In August 2013, members of the largest MSM sexual-partner seeking networking
site in the US received an online invitation to complete a survey about their HIV prevention practices.
Responses were analyzed using summary statistics. Multivariable logistic regression analyses were
conducted to determine adjusted odds ratios to assess factors associated with having used PEP or PrEP.
Results: Of 9,179 MSM who responded to the survey, 18% used mobile technology. ParticipantsŐ
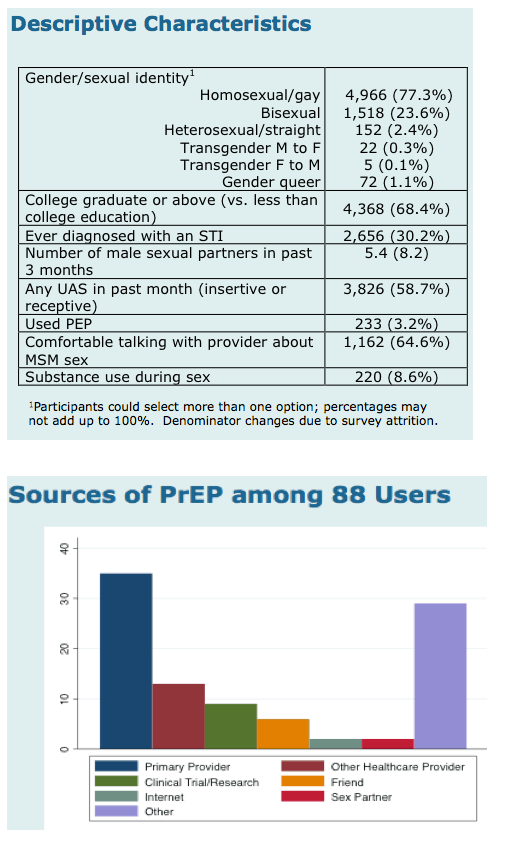
mean age was 26 years; 82% identified as homosexual or gay, 23.6% as bisexual, 2.4% as heterosexual,
0.4% as transgender and 1.1% as gender queer. Most of the respondents were white (85.7%), 3.9% Black,
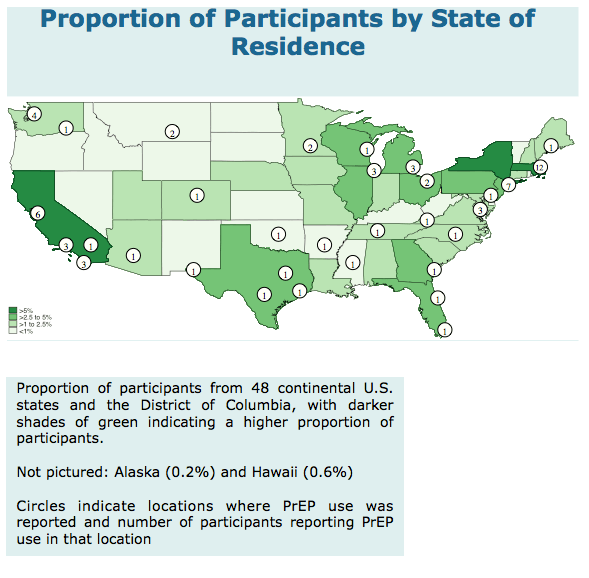
7.5% Latino. Over 2/3 (68.4%) completed college. The sample was geographically diverse.
More than 1/4 (30.2%) reported a prior sexually transmitted infection (STI); 58.7% reported at least
one episode of unprotected anal sex, and 7.5% reported substance use during sex in the prior 3 months.
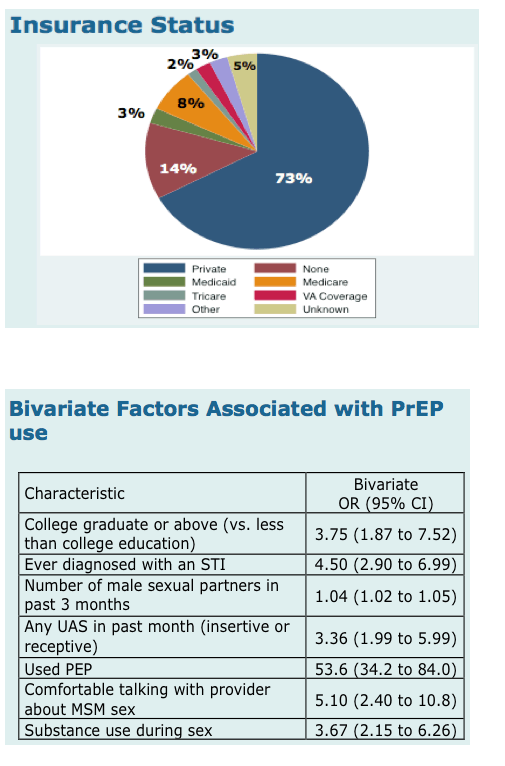
Although 84.0% reported that they had a primary care provider (PCP), only 53.9% reported that they felt
comfortable discussing sex with their PCP.
Only 3.2% of respondents reported prior PEP use, and 1.2% reported PrEP use. PEP users more
often were younger, identified as gender queer (compared to homosexual or gay), had graduated college,
had a prior STI diagnosis, engaged in recent unprotected anal sex, had used substances during sex, and
were more comfortable talking about sex with their PCP compared to MSM who had not used PEP.
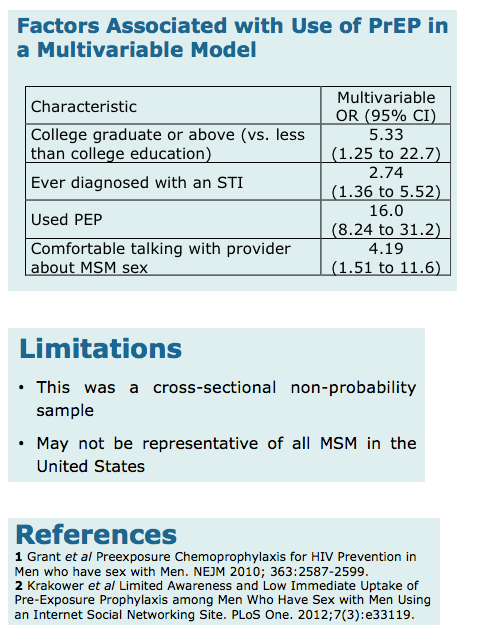
PrEP users more often reported that they had graduated college, had a prior STI, and were more comfortable
talking with their PCP about MSM sex compared to MSM who had not used PrEP. PrEP users had a
16-fold greater odds of having used PEP than PrEP-na•ve MSM.
Conclusions: Although MSM in this online survey reported significant HIV risks, their experience with
PEP and PrEP was limited. In order to increase PrEP uptake among MSM, PCPs need to be educated
to provide culturally competent care, so that patients will be comfortable discussing HIV risks that could
be decreased by PEP or PrEP.

|
| |
|
 |
 |
|
|