 |
 |
 |
| |
Rosuvastatin Lowers Cystatin C in HIV-infected Subjects on Antiretroviral Therapy: SATURN-HIV
|
| |
| |
CROI: Rosuvastatin Improves Hip Bone Mineral Density but Worsens Insulin Resistance - (03/07/14)
Reported by Jules Levin CROI 2014
March 3-6 Boston, MA
Chris T. Longenecker1,2, Corrilynn O. Hileman1,3, Norma J. Storer1,2, Danielle E. Labatto1,2, Grace A. McComsey1,2
1 Case Western Reserve University, Cleveland, OH, USA; 2 University Hospitals Case Medical Center, Cleveland, OH, USA;
3 MetroHealth Medical Center, Cleveland, OH, USA

Program Abstract-
Background: In chronic HIV-infection, both creatinine and cystatin C (CysC) based estimates of glomerular filtration rate
(eGFRcr and eGFRcys) are less accurate than combined estimates (eGFRcr-cys) when compared to measured GFR;
however, eGFRcys is a better predictor of mortality. This may be explained by non-GFR determinants of plasma cystatin C levels,
particularly inflammation. Statins may improve CysC by decreasing inflammation.
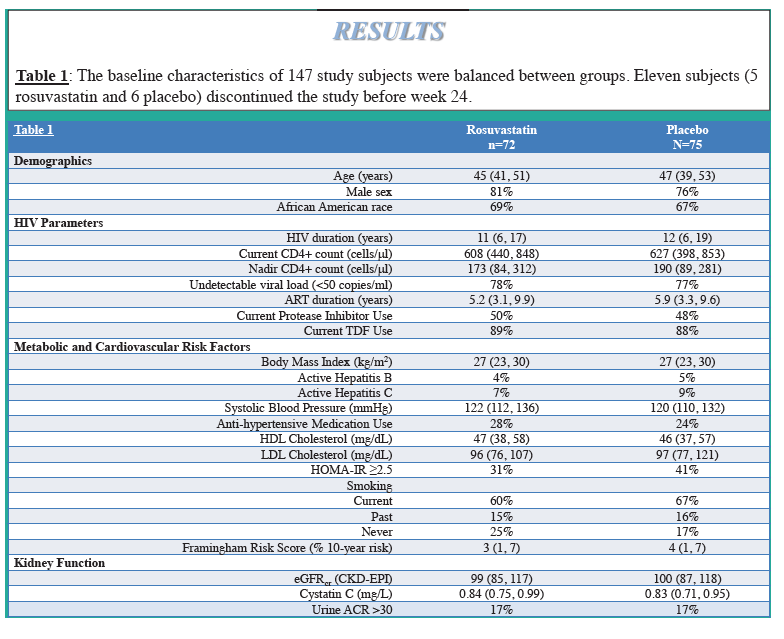
Methodology: The Stopping Atherosclerosis and Treating Unhealthy Bone with Rosuvastatin in HIV (SATURN-HIV) trial randomized
147 patients on stable antiretroviral therapy (ART) with LDL-cholesterol <130mg/dL to 10 mg daily rosuvastatin or placebo.
We analyzed relationships of baseline and 0-24 week changes in plasma CysC concentration with measures of cardiovascular risk
and biomarkers of inflammation and immune activation using Spearman correlation analysis and multiple linear regression.
Results: Median (interquartile range) age was 46 (40-53) years; 78% were male, 68% African American, and 14% had hepatitis C.
Tenofovir and protease inhibitors (PI) were used in 88% and 49% of subjects, respectively. Median eGFRcr was
100 (87-118) mL/min per 1.73 m2 and CysC was 0.83 (0.73-0.95) mg/L, without treatment group differences.
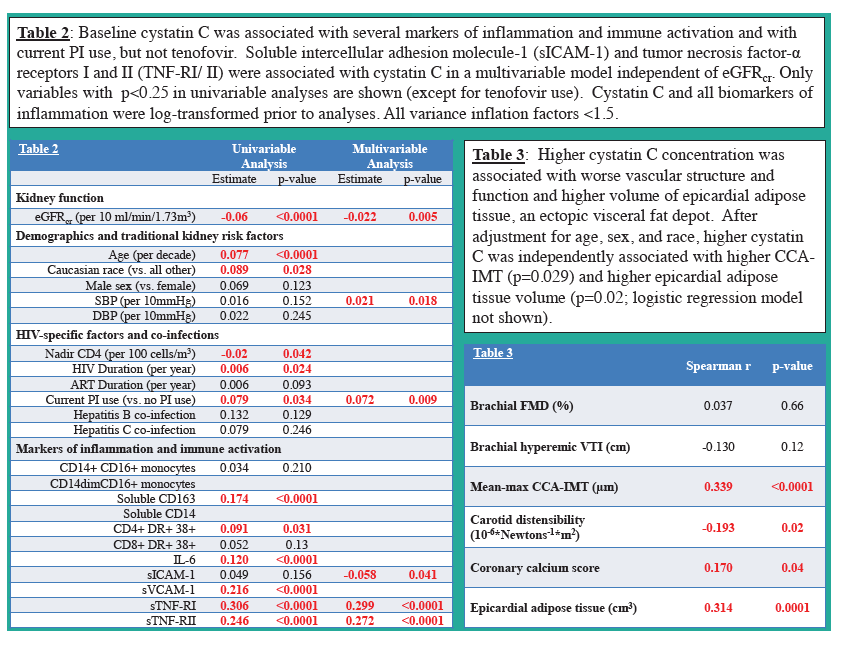
Baseline CysC concentration correlated with carotid intima-media thickness (r 0.324, p<0.001), carotid distensibility (r 0.193, p=0.019),
and coronary calcium score (r 0.170, p=0.040).
Baseline CysC was associated with several markers of inflammation and immune activation and with use of PI, but not tenofovir
(see Table). Soluble intercellular adhesion molecule-1 (sICAM-1) and tumor necrosis factor-α receptors I and II (TNF-RI/ II)
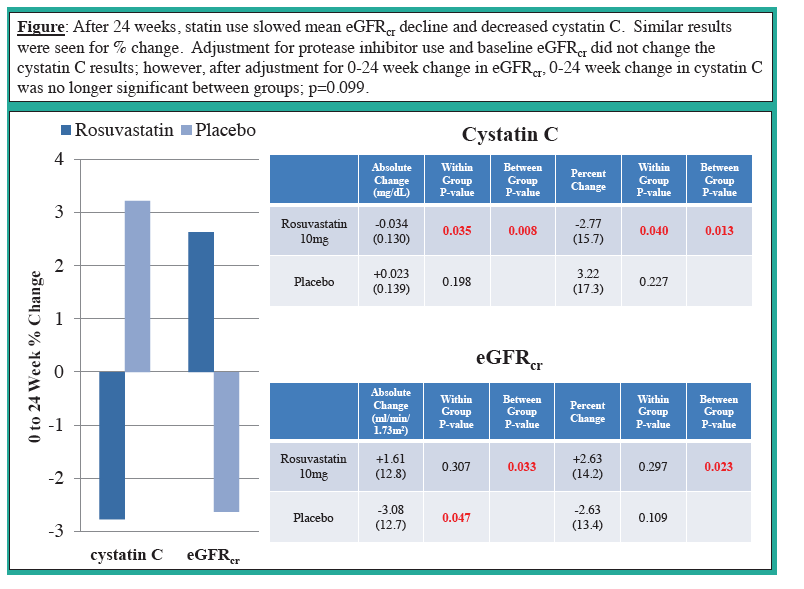
were associated with CysC in a multivariable model independent of eGFRcr. After 24 weeks, mean CysC decreased significantly
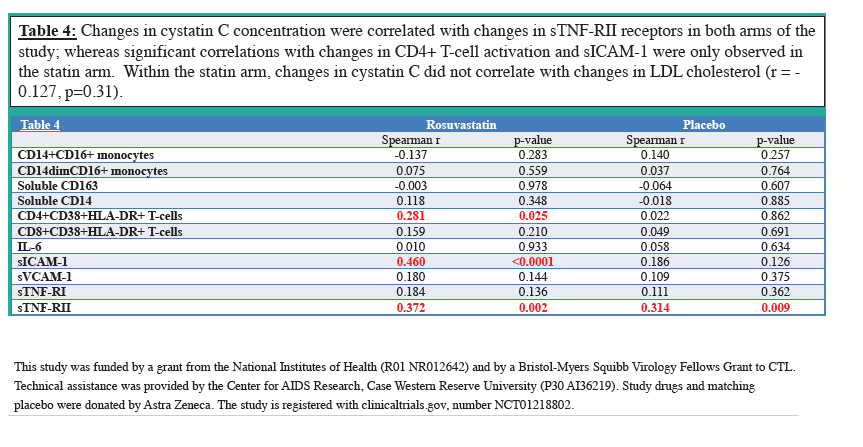
with statin therapy compared to placebo (-0.034mg/L vs. +0.010mg/L, p=0.008). Within the statin group,
changes in CysC correlated with changes in sICAM-1 and TNF-RI (r 0.460, p<0.001 and r 0.372, p=0.002, respectively).
Conclusions: Rosuvastatin 10mg daily reduces plasma CysC in HIV-infected patients on ART. Baseline CysC
concentrations are associated with cardiovascular risk, inflammation and immune activation.
Reductions in CysC with statin therapy correlate with reductions in inflammatory biomarkers.
The relationship between Cystatin C, cardiovascular disease, and mortality in HIV may partly be related to non-GFR
factors such as inflammation.


|
| |
|
 |
 |
|
|