 |
 |
 |
| |
A Low CD4/CD8 Ratio During Effective ART Predicts Immunosenescence and Morbidity/Mortality
|
| |
| |
"each 10% decrease in the CD4/CD8 ratio was associated with 48% higher odds of serious non-AIDS events (P=0.045) and 13% higher odds of mortality (P=0.01)......subjects with low CD4/CD8 ratio during effective ART exhibit heightened T cell activation & senescence, while those with normal ratios showed levels closer to normality....."
Reported by Jules Levin
CROI 2014 March 3-6
Boston, MA
Sergio Serrano-Villar1, Talia Sainz2, Sulggi A. Lee3, Peter W. Hunt3, Elizabeth Sinclair3, April L. Ferre4, Vivek Jain3, Frederick M. Hetch3, Santiago Moreno1, Steve G. Deeks3
1Infectious Diseases, University Hospital Ramon y Cajal, Madrid, Spain, 2Infectious Diseases, University Hospital Gregorio Maranon, Madrid, Spain, 3University of California San Francisco, San Francisco, CA, United States, 4University of California Davis, Davis, CA, United States

Program Abstract:
Background: A low CD4/CD8 ratio in elderly HIV-uninfected adults is associated with increased morbidity and mortality. A subset of HIV-infected adults
receiving ART fails to normalize this ratio, even after a normal peripheral CD4 count is obtained. The immunologic and clinical characteristics of this clinical phenotype remain undefined.
Methodology: We evaluated the associations of the CD4/CD8 ratio with 1) maturational subsets and markers of T-cell activation (%HLADR+CD38+)
and senescence (%CD28- and %CD28-CD57+) of CD8+ T-cells in 67 treated HIV+ subjects with CD4≥500 cells/mm3 and VL<50 copies/mL and 15
HIV-CMV+ healthy controls; 2) inflammatory markers in 192 treated HIV+ adults; 3) the CD4/CD8 ratio in gut mucosa and lymph nodes in 32 and 10
treated HIV+ subjects, respectively; 4) early (≤6 months after estimated HIV infection) vs. later (≥2 years) ART initiation in 68 HIV+ adults; 5) the risk of
serious non-AIDS events in two nested case-control studies of in 66 and 192 ART-suppressed HIV+ adults.
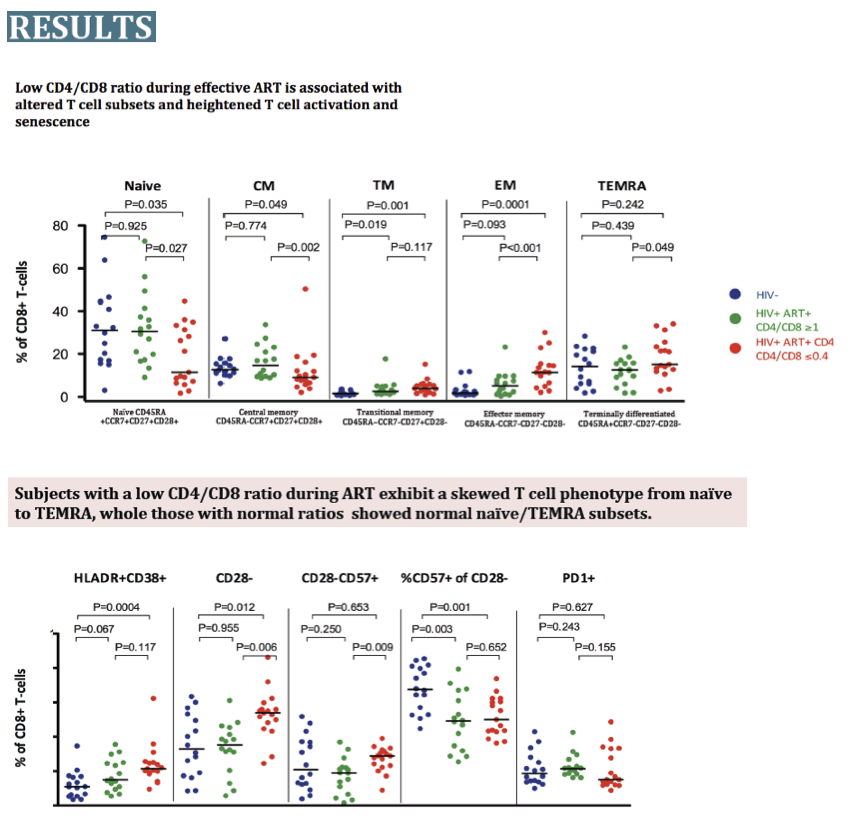
Results: Among individuals with an apparently normal CD4+ T cell count, the CD4/CD8 ratio significantly correlated with the %naïve (rho +0.34,
P=0.005), %TEMRA (rho -0.37, P=0.003), and %CD28- (rho -0.43, P<0.001) CD8+ T-cells. Compared to HIV-CMV+ controls, ART-suppressed
individuals with a low CD4/CD8 ratio (≤1st Qrt, 0.4) showed a markedly skewed CD8+ T-cell phenotype from naïve to TEMRA, and higher %HLADR+CD38, %CD57+CD28- and %CD28- CD8+ T-cells (all P<0.05), while those with a normal CD4/CD8 ratio (≥4th Qrt, 1.0) had normal levels.
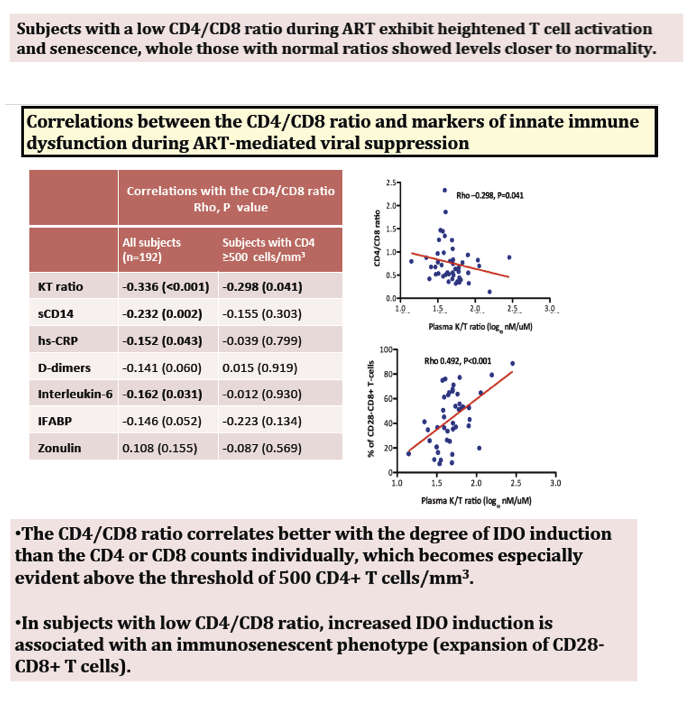
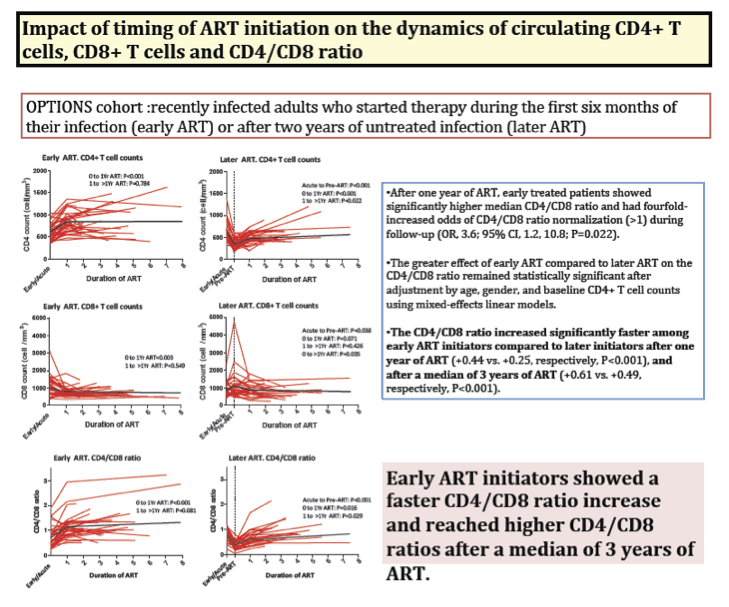
The CD4/CD8 ratio correlated substantially with sCD14, hs-CRP, IL-6 and the KT ratio-a marker of indoleamine-dioxygenase-1 induction-with only the KT ratio significantly correlated in the subgroup with CD4≥500 cells/mm3 (Rho -0.29, P=0.041). The peripheral CD4/CD8 ratio was similar to the ratio in gut mucosa (Rho=0.68, P<0.001) but not in lymph nodes. In a longitudinal study, early ART initiators had a faster CD4/CD8 ratio increase than later ART initiators (+0.44 vs. +0.25, respectively, P<0.001). After a median of 3 years of ART, early ART initiators had more CD4/CD8 ratio normalization (OR, 3.6; 95% CI, 1.2, 10.8).
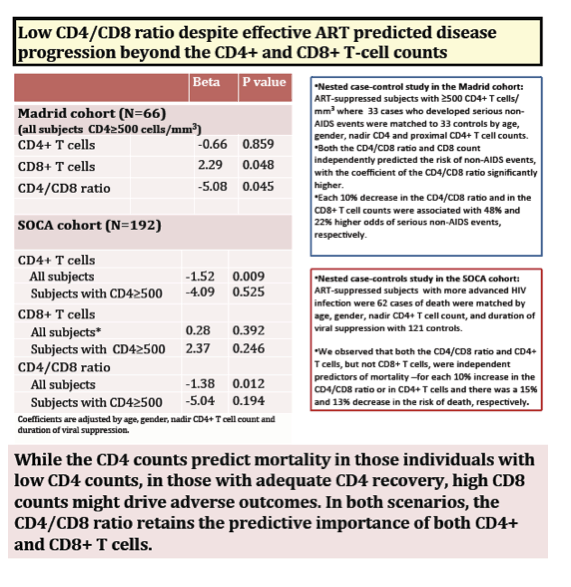
After controlling for age, gender, ART duration, nadir and CD4 count, each 10% decrease in the CD4/CD8 ratio was associated with 48% higher odds of serious non-AIDS events (P=0.045) and 13% higher odds of mortality (P=0.01).
Conclusions: A persistently low CD4/CD8 ratio during otherwise effective ART is associated with increased innate and adaptive immune activation, an
immunosenescent phenotype, and higher risk of morbidity/mortality. This ratio may prove useful in monitoring response to ART and could identify a unique subset of individuals needed of novel therapeutic interventions.

|
| |
|
 |
 |
|
|