 |
 |
 |
| |
HIV, Chronic Inflammation, and CVD: Report back from the 2014 Conference on Retroviruses and Opportunistic Infections
|
| |
| |
Priscilla Hsue, MD Professor of Medicine, UCSF Cardiology Division
Non-AIDS conditions are becoming an increasingly important health issue among HIV-infected individuals. Recent studies have definitely shown that HIV patients have increased risk for MI (Myocardial Infarction), even among well-treated and suppressed individuals, and once developing MI (myocardial infarction), the mortality among individuals with HIV is higher. Ongoing studies are focusing on the challenging task of untangling the complicated mechanisms underlying HIV-associated cardiovascular disease, and addressing ways to target chronic inflammation.
Two studies were focused on using FDG-PET imaging to characterize cardiovascular disease among HIV-infected individuals. 18 fluorodeoxyglucose is a tracer that is taken up preferentially by metabolically active cells such as monocytes and macrophages. Among individuals without HIV infection, FDG-PET/CT imaging is the best modality to detect and monitor arterial inflammation in vivo and has been validated against histologic vascular specimens. Arterial inflammation using FDG-PET predicts CV risk independently of traditional risk factors and is reduced by interventions that reduced CV risk.
There were two oral presentations relating to CV disease (Session 0-10, "CV and Other Complications"), abstracts 130 and 131, and the Themed Discussion.
The first study, entitled "Increased Arterial Inflammation Relates to High-Risk Coronary Plaque Morphology in HIV+ Patients (Abstract 130)." Prior studies by this group have demonstrated increased levels of arterial inflammation using FDG-PET/CT among HIV-infected individuals which correlates with sCD163 (a marker of monocyte activation). In this study, the relationship between HIV-infected individuals with evidence of coronary plaque on CT angiography were studied with FDG-PET/CT. A total of 41 HIV patients on stable ART were studied. Among individuals with higher evidence of vascular inflammation, a higher percentage of individuals had evidence of low attenuation coronary plaque (40% vs. 10%, p=0.02). This finding suggests that arterial inflammation in HIV may be associated with high risk plaque morphology rendering individuals susceptible to plaque rupture and MI. This finding remained significant after adjustment for age, gender, LDL, HIV duration and CD4. [CROI webcast: http://www.croiwebcasts.org/console/player/22264?mediaType=slideVideo&]
Another study was presented entitled "Arterial Inflammation as Measured by FDG-PET/CT is Associated with Splenic Activity (Abstract 131)." The spleen is thought to serve as a reservoir for inflammatory monocytes, and after MI, monocytes exit the spleen, accumulate in injured tissue, and then participate in remodeling and development of subsequent heart failure. Activation of the bone marrow and spleen are increased after recent MI. Among individuals with HIV, the spleen and bone marrow are thought to be HIV reservoirs. This study demonstrated that the metabolic activity of the spleen, bone marrow, and vasculature of HIV infected individuals was higher than that of matched controls. This finding persisted when the analysis was restricted to the treated suppressed. Splenic and bone marrow activation were strongly correlated with vascular inflammation. HIV persistence was associated with splenic activation, suggesting that the spleen may play a role in HIV-associated cardiovascular disease. This study suggests that the spleen and bone marrow may be key HIV reservoirs, and that activation of inflammatory cells in the spleen may play a key role in HIV-associated CVD. [CROI webcast: http://www.croiwebcasts.org/console/player/22265?mediaType=slideVideo&]
These two studies highlight the utility of FDG-PET as a unique modality to characterize the role of HIV infection, inflammation, and CVD. As this technique is new, larger studies will be needed to evaluate the predictive utility of FDG-PET for CV events and mortality.
--------------------------------------
A poster session and moderated poster discussion focused on Heart Failure, Cardiac Steatosis, and HIV. CROI Webcast Discussion leader Wendy Post: http://www.croiwebcasts.org/console/player/22096?mediaType=slideVideo&
Abstract 723 [http://www.croiwebcasts.org/console/player/22098?mediaType=slideVideo&]
was a study of HIV-infected individuals in the WIHS cohort. CVD are common comorbidities in HIV-infected individuals. NT-pro BNP is a marker of cardiac ventricular stress & has been found to be associated with CVD in HIV. They found that NT-pro-BNP levels > 75% percentile, a marker of cardiac strain and systolic dysfunction, were an independent predictor of mortality among women when sampled at both early and late antiretroviral time periods (HR 1.8, 95%CI 1.3-2.4), p<0.001 and HR 2.8, 95%CI 1.4-5.5, p=0.002, respectively), while levels were not associated with mortality in uninfected women in the early period. A total of 387 HIV uninfected, and 936 HIV-infected women were studied. This study suggests that NT-pro-BNP levels, which are markers of ventricular strain are predictive of morality among HIV-infected women and that cardiopulmonary dysunction may be a contributor to mortality.
Abstract 724 [http://www.croiwebcasts.org/console/player/22100?mediaType=slideVideo&] was a cross-sectional study of 95 HIV-infected adults and 30 healthy controls with no known CVD. 84% of HIV-infected had HIV RNA <50 c/ml, undetectable, & an avg CD4 of 615. Magnetic resonance spectroscopy was used to assess intraventricular [cardiac steatosis] and visceral fat. Cardiac steatosis (i.e. lipid deposition in myocardial tissue) has been identified in diabetes and is associated with impaired myocardial function.
The study showed a 38% increase in intraomyocardial lipid (cardiac steatosis) in HIV+ subjects vs. controls, P=0.04). Exposure to ARV was positively correlated with ARV years as was visceral fat volume (r=0.27, p=0007 and r=0.31, p=0.004, respectively). HIV infection was an independent predictor of intramyocardial lipid, along with visceral fat and female sex. The authors concluded that increases in visceral adiposity that occurs with ARV exposure may drive some of the observed increase in cardiac steatosis & convey an increased risk for myocardial steatosis; that their data suggests that women with HIV may be particularly vulnerable to cardiac steatosis, which may be related to BMI & adiposity.
Abstract 725 [http://www.croiwebcasts.org/console/player/22097?mediaType=slideVideo&]
was a study of novel serum biomarkers including ST2, GDF-15, ultrasensitive troponin along with other markers of biomarkers such as IL6, D-dimer and cystatin C and relationship to structural heart disease assessed using echocardiography and mortality via the NDI. Although markers of inflammation (hsCRP, IL6), coagulation (D-dimer), and renal disease (Cystatin-c) are associated with CV events & mortality in HIV they do not reflect cardiac specificity & may not reflect direct pathways, but biomarkers of cardiac stress (ST2, GSF-15, NT-proBNP, high sensitivity Troponin-I) are predictive of CV events and mortality in the uninfected population and thus may improve the risk stratification of HIV-infected patients. HIV patients had higher levels of all biomarkers except IL-6, and 45% had diastolic dysfunction. ST2 was independently associated with diastolic dysfunction in fully adjusted analysis (RR 1.43 per doubling, 95%CI 1.06-1.92, p=0.019). Only ST2 and GDF-15 were individuals associated with mortality in fully-adjusted analysis (HR 1.89, 95%CI 1.04-3.44, p=0.036 and HR 1.35, 95%CI 1.02-1.79, p=0.038). Future studies are needed to elucidate the potential role of ST2 & GDF15 but these data suggest these markers may be more predictive of mortality and cardiovascular disease than other inflammatory markers.
The role of depression and incident heart failure was evaluated in Abstract 726. [http://www.croiwebcasts.org/console/player/22099?mediaType=slideVideo&]
Investigators analyzed data on 81,427 veterans without CVD of whom 33% were HIV infected from the Veterans Aging Cohort Study-Virtual Cohort 9VACS VC). Individuals with both HIV and major depressive disorder were at increased risk for incident heart failure (RR 1.68, 95%CI 1.45-1.95). Depression was associated with increased risk for incident heart failure regardless of HIV status. Both major depressive disorder (MDD) and HIV are associated with heart failure, and individuals with both conditions had the highest risk for HF among both HIV-infected and controls. These results highlight the importance of identifying depression among those with HIV.
Collectively, these studies indicate the role of newer biomarkers and mortality in HIV as well as the possible role of cardiac steatosis and depression in HIV-associated CVD.
---------------------------------------------
A poster session also focused on the role of immune activation, immunodeficiency at CVD.
Abstract 727 [Impact of Low CD4 Count and HIV Persistence on Endothelial Function in Patients with Low Plasma RNA] looked at the role of HIV persistence in small vessel disease as assessed using hyperemic velocity, which is the stimulus for brachial artery flow-mediated vasodilation (FMD). HIV-positive individuals are at high risk for myocardial infarction and sudden
cardiac death. Chronic inflammation is a contributing factor to increased cardiovascular risk in HIV-infected individuals, even among those with low plasma viral RNA levels. Endothelial impairment is proatherogenic and brachialartery flow-mediated vasodilation (FMD) has been established as a highly sensitive and specific assessment of vascular endothelial function. Hyperemic velocity, a measure of microvascular function, is the stimulus for FMD, a measure of macrovascular function. A total of 71 patients, mostly men, were studied (72% treated suppressed and the remainder were elite controllers). Average age was 53 in the treatment suppressed group and 43 among the elite controllers. Worsened hyperemic velocity was independently associated with lower CD4+ T cell count (RR 1.04 per 100 CD4+ T-cells, p<0.001) while traditional risk factors and higher cell-associated RNA were both associated with worsened FMD. Among HIV-infected individuals with undetectable plasma RNA levels using conventional assays, a lower current CD4+ T-cell count, but not measures of viral persistence, was independently associated with impaired microvascular function, as defined by hyperemic velocity. In contrast, cell-associated HIV RNA was associated with impaired macrovascular function, as measured by FMD, suggesting that HIV may preferentially affect the microvasculature, leading toworsened FMD.
Abstract 728 [Carotid Distensibility and Immune Activation in HIV-Infected Patients Without Coronary Calcium] evaluated the role of carotid artery intima media thickness, distensibility, and CAC, coronary artery calcium. The majority of HIV patients had undetectable CAC, but 29 (31%) of those with zero CAC had carotid atherosclerosis by ultrasound (CCA-IMT>1mm or discreet carotid plaque). Carotid distensibility, a marker of vascular stiffness, correlates with lymphocyte and monocyte activation in HIV infected patients on ART who do not have evidence of coronary calcification on CT. Among subjects with CAC=0, distensibility was significantly or marginally significantly correlated with CCA-IMT (r 0.339, p <0.001) and two measures of endothelial function (r 0.192, p=0.066 for flow-mediated brachial artery dilation; and r 0.374, p<0.001 for hyperemic velocity-time integral). Coronary artery calcium (CAC) scoring significantly improves cardiovascular risk stratification; however, CAC is a late finding of atherosclerotic vascular disease. Increased vascular stiffness (i.e. decreased distensibility) may be an early marker of vascular disease in HIV-infected patients on antiretroviral therapy (ART) prior to the development of vascular calcification. The relationship of chronic systemic immune dysregulation to these early vascular changes in HIV is poorly understood. Among HIV-infected patients on ART who do not have coronary artery calcification, impaired carotid distensibility may be a sign of early vascular disease that is associated with immune activation and inflammation.
Abstract 729 [Microvascular Disease in HIV-Infected Controllers is Mediated by HIV DNA and Immune Dysfunction] was an open label study to evaluate the impact of ART on endothelial function and microvascular function in elite controllers, viremic controllers, and non-controllers.
HIV-infected individuals ("controllers") who are able to maintain low levels of plasma HIV RNA in the absence of ART have stable low-level viremia, elevated T cell activation, and a higher risk of cardiovascular disease (CVD). The mechanisms underlying this increased risk are unknown but may include low-level viral replication leading to chronic inflammation and subsequent endothelial dysfunction.
All individuals were treated with 24-36 weeks of Raltegravir+TDF/FTC and had FMD [endothelial function] and hyperemic velocity [microvascular function] measurements performed at weeks 0, 4, 24, and 36. 24 weeks of ART resulted in significant reductions in ultrasensitive plasma RNA and T cell activation in elite controllers which did not translate into improved FMD. However, controllers had improved small vessel disease (HV), which was mediated by lower markers of both viral persistence and immune dysfunction.
Abstract 730 [Monocyte But Not Cellular Activation Is Associated With Coronary Atherosclerosis in the MACS] was a cross-sectional study of 139 treated and suppressed HIV+ men and 92 uninfected controls in the Multicenter AIDS Cohort Study (MACS). HIV patients had higher levels CD8+ T cell activation and sCD114 and SCD163, that is higher levels of cellular and monocyte activation markers than HIV-uninfected participants, however only monocyte activation markers were associated with coronary calcium and calcified plaque in the controls while sCD163 was associated with calcified, mixed, and total plaque in the HIV-infected group. Although not significant, HIV-infected had increased frequency of non-calcified plaque and coronary stenosis than uninfected participants.
This series of studies underlies the growing recognition of viral persistence and CVD among individuals with treated and suppressed HIV disease, and the differential ability of imaging techniques and biomarkers to identify HIV individuals at risk for CVD.
-----------------------------------
The next series of studies evaluated the role of smoking and alcohol in atherosclerosis in HIV.
Abstract 731 [The J-Curve in HIV: Better Cardiovascular-Disease-Free Survival With Moderate Alcohol Intake] from the Swiss Cohort Study identified 464 CV disease events among 10,547 individuals studied. The study objectives were to study the association between the level of alcohol consumption and cardiovascular disease events (CADE) free survival in a large, nationwide HIV cohort, and to evaluate the association between the level of alcohol consumption and secondary endpoints including CADE, heart CADE and overall survival, [major cardiovascular disease events, CADE; CADE included myocardial infarction, coronary angioplasty, coronary artery bypass grafting, carotid endarterectomy, procedures on other arteries, cerebral infarction and cerebral haemorrhage. Compared to abstention, low and moderate alcohol were associated with a lower incidence of the combined endpoint (HR 0.73, 95%CI 0.6-0.88, p-0.001, and HR 0.67, 95%CI 0.56-0.80, p<0.001), with a better CADE free survival and overall survival in participants of the Swiss HIV Cohort Study on antiretroviral therapy. No association was seen for severe intake, high alcohol consumption. Traditional risk factors and low CD4 counts were associated with higher HR for CV events or death. All classical cardiovascular risk factors, including family history, diabetes, smoking, obesity and arterial hypertension, as well as low CD4 cell count were significantly associated with a higher hazard of CADE or death.
In Abstract 732 [Soluble CD14 and D-Dimer Are Associated With Smoking and Heavy Alcohol Use in HIV-Infected Adults], the SUN study evaluated the role of markers of monocyte activation and D-dimer to evaluate the role between cigarette smoking and heavy alcohol use. In the general population and among HIV-infected adults, biomarkers of monocyte activation (soluble CD14 [sCD14]) and altered coagulation (D-dimer) have been independently associated with increased risk for myocardial infarction, coronary heart disease, and all-cause mortality. The objective was to examine whether cigarette smoking and heavy alcohol use were associated with higher levels of sCD14 and D-dimer in PLWH to inform CVD prevention efforts. We hypothesized that cigarette smoking and heavy alcohol use would be associated with higher sCD14 and D-dimer levels. Current cigarette smoking was associated with elevated sCD 14 (ß=135.57, 95%CI 85-186, p=.000 while heavy alcohol was associated with significantly lower D-dimer levels (ß=-0.059, 95%CI -.102, -0.16, p=0.007).
Finally, Abstract 733 [Antiviral Therapy and Smoking Associated With Coronary Vessel Thickening in HIV-Infected Youth] was a prospective study 35 young HIV patients and 11 controls using MR imaging of the RCA and CT angiography. Increased CVD risk was associated with HIV infection in young adults with perinatal infection. Vessel wall thickness and quantification of plaque in coronary vessels may be more predictive of cardiovascular events than other indicators of CVD. HIV patients with a mean age of 22 had significantly increased thickness of the proximal RCA (1.32mm vs. 1.09mm, p=0.002). Both HIV and smoking were predictors of RCA thickness. There was no significant difference in plaque in HIV patients vs. controls. Among HIV patients only, duration of ART and stavudine were most closely correlated with RCA thickness.
Individuals infected with HIV early in life have premature vascular injury compared to healthy volunteers, as shown by coronary vessel wall thickness. Coronary vessel wall thickening was independent of atherosclerotic plaque, indicating that vessel wall thickening related to ART exposure occurs through a mechanism distinctive from traditional atherogenesis.
These abstracts demonstrate a potential protective effect of low to moderate alcohol use and CVD and differential impact of smoking and alcohol on monocyte activation and D-dimer. Finally, young HIV patients were found to have thicker proximal RCA which was associated with smoking.
----------------------------
A large group of studies focused on risk factors and the incidence of MI and Stroke.
In a study from the Veteran Aging Cohort Study (Abstract 734; HIV Infection and the Risk of Cardiovascular Disease in Women), incident CV events were significantly higher among HIV+ vs. HIV- women (13.5, 95% CI 10.1, 18.1 and 5.3, 95%CI 3.9, 7.2, p<0.001). After adjustment, HIV women had a higher risk of CVD compared to HIV-. The elevated CV risk remained among individuals with RNA levels ≥ 500 and those < 500, being on ART reduced risk but still had increased risk compared to HIV-neg. The risk of CVD was greater among those with CD4 cell counts ≥ 200 cells/mm3 vs. those < 200 cells/mm3, p=0.047), but there was increased risk at all the studied CD4 categories: >500, 200-499, and <200.
HIV infection has been associated with an increased risk of cardiovascular disease (CVD) in women. Whether this association is driven by HIV specific or traditional risk factors remains unclear.
Sample size: 2190 women (32% HIV+), Median follow-up: 6.0 years; CVD events : Total: 86 (53% HIV+): AMI: 24%; ischemic stroke: 20%; heart failure: 56%
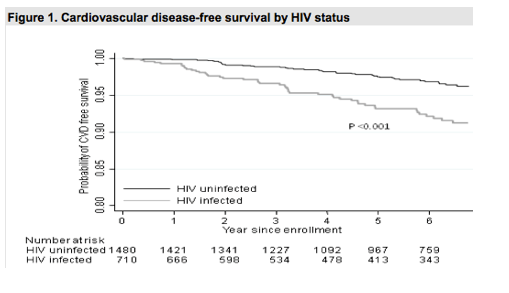
Abstract 735 [Depression Predicts Incident Myocardial Infarction in HIV+ Veterans: Veterans Aging Cohort Study] studied 27,362 HIV infected men from the Veterans Aging Cohort Study Virtual cohort. Any type of depressive disorder (major depressive disorder or dysthymic disorder) was a predictor of incident acute myocardial infarction (HR 1.35, 95%CI 1.07-1.70, p=0.01 as was each diagnosis individually. Using this same cohort, in abstract 736, the CV risk factor profiles including cholesterol, blood pressure, smoking and diabetes were evaluated with respect to incident MI in HIV patients. They demonstrated that an optimal risk factor profile was associated with lower MI rates, and compared to HIV- veterans with similar profiles, HIV+ veterans had higher adjusted AMI (acute myocardial infarction) rates, especially among those with at least 1 major risk factor present. 858 AMIs (acute myocardial infarction)(42% HIV+) occurred over 5.9 years (median). Prevalence of optimal cardiac health was <2%. Optimal CVDRF profile was associated with the lowest adjusted AMI rates.
Compared to HIV-Veterans, AMI rates among HIV+ Veterans with the same CVDRF profile were higher with each additional major CVDRF. Compared to HIV-Veterans without major CVDRFs, HIV+ Veterans without major CVDRFs had a 2-fold increased adjusted risk of AMI (HR: 2.0 95%CI: 1.0-3.9, p=0.044). The prevalence of optimal cardiac health is low in this cohort. Among those without major CVDRFs, HIV+ Veterans have twice the risk of AMI. Compared to HIV-Veterans AMI rates in HIV+ Veterans were higher with each additional major CVDRFs. Preventing/reducing CVDRF burden may reduce excess AMI risk among HIV+ people.
Depressive disorders are associated with a 31% increased risk of AMI beyond that explained by known risk factors.
Incident AMI rates per 1000 person-years were higher among those with versus without any depressive disorder (rate ratio 1.28, 95% CI: 1.01-1.62), MDD (rate ratio 1.24, 95% CI: 0.96-1.59), and dysthymic disorder (rate ratio 1.46, 95% CI: 1.06-1.98), although the HRfor MDD fell slightly below significance (Figure 1).
Cox proportional hazards models (adjusted for demographics, CVD risk factors, other important covariates, and HIV-specific factors) revealed that any depressive disorder (p=.03; Figure 2) and dysthymic disorder (p=.01)predicted incident AMI, while the HR for MDD (p=.06) fell just short of significance (Table 2).
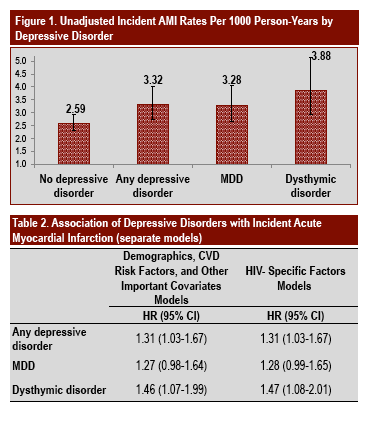
These findings provide preliminary support for future clinical trials to evaluate whether delivering evidence-based depression treatment may be a novel approach to managing the excess cardiovascular risk of HIV-infected patients with depression.
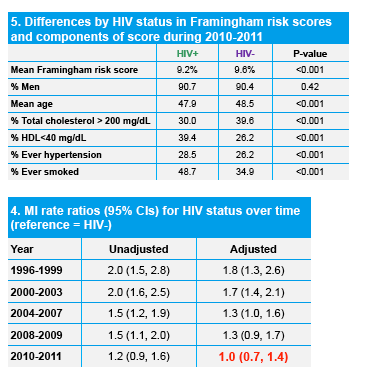
In contrast, Abstract 737 [No Difference in Incidence of Myocardial Infarction for HIV+ and HIV- Individuals in Recent Years] evaluated HIV+ individuals and controls in the Kaiser Permanente California health plan. In earlier years, both adjusted and crude rates of MI were higher among HIV infected individuals compared to controls including 1996-99, 2000-2003, 2004-07, and 2008-2009. However in 2010-2011, adjusted rates were similar among the two groups. During this time, the calculated Framingham risk scores were lower among HIV+ patients, which were 9.2% vs. 9.6% respectively, p<0.001). HIV+ adults have a 40% increased risk of MIs overall compared with HIV- adults from the same health system, independent of risk factors. The higher risk for HIV+ adults no longer observed in more recent years. HIV+ adults have similar or slightly improved Framingham scores in recent years. The reduced MI incidence rates for HIV+ adults in recent years is likely a result of a combination of factors such as cardiovascular risk factor reduction, use of more lipid-friendly antiretroviral therapy, and reduced immunodeficiency.
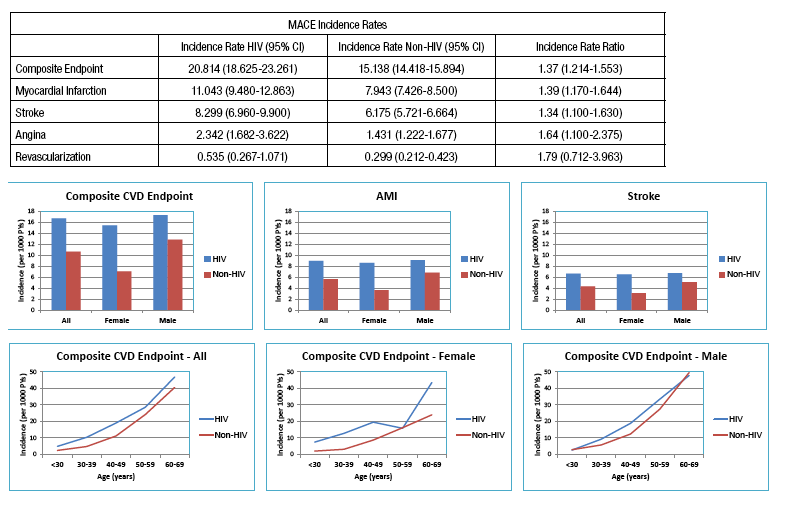
The incidence of major adverse CV events were studied in the Partner's HealthCare System in Abstract 738 [MACE Incidence Among HIV- and Non-HIV-Infected Patients in a Clinical Care Cohort]:
Partners HealthCare System HIV longitudinal cohort, comprised of Brigham & Women's Hospital and Massachusetts General Hospital; 3,109 HIV-infected and 23,237 non-HIV-infected control patients matched on age, gender, and race; Followed 4.8 years (14,942 person-years [PYs]) for HIV 4.6 years (106,885PYs) for control patients. Rates were higher among HIV+ patients vs. non-HIV (20.8, 95%CI 18.6-23.3 per 1000PY vs. 15.1, 95%CI 14.4-15.9 per 1000 PY) in patients ≥40 years.
Rates of composite CVD endpoint were 16.7 events per 1000 PYs (95% confidence interval [CI] 15.1-18.5) for HIV versus 10.7 (95% CI 10.2-11.2) for control group. The Incidence rate ratios for HIV vs. non HIV were 1.4 for a composite endpoint, 1.4 for MI, 1.3 for stroke, 1.6 for angina, and 1.8 for revascularization.
In abstract 739 [Lower CD4 Count and Higher Viral Load Are Associated With Increased Risk of Myocardial Infarction], the CNICS cohort was used to study the role of traditional and HIV-specific factors and MI. Among 18,115 participants, there were 314 confirmed incident MIs. Smoking, age, total and HDL-C, and systolic BP were significant predictors of MI. Interestingly, higher CD4 count was associated with decreased risk of MI (per 300cell/ml OR 0.75, 95%CI 0.64, 0.88) while HIV viral load was associated with increased MI risk (log copies OR 1.10, 95%CI 1.05, 1.16).

Using data from the MACS study, the role of substance abuse and CV, renal and malignancies in HIV were characterized in Abstract 740 [Long-Term Effects of Nitrite Inhalants On Cardiovascular and Renal Outcomes in the MACS Cohort]. The heavy use of nitrite inhalants was associated with increased frequency of cardiovascular, renal, and malignancy comorbidities in both HIV negative and positive patients. Poppers were one of the most common and heavily used drugs in the MACS cohort. In HIV-negative and HIV-positive subjects (n=1670 and 1589, respectively, 107 seroconverters; >30,000 person-visits), nitrite inhalants (53%), marijuana (44%), cocaine/crack (20%), uppers (10%), and MDMA/MDA (7%) were drugs used most commonly within the prior 6 months. The incidence rate of cardiovascular outcomes was increased more than two-fold in Caucasian HIV-negative non-smokers with heavy popper use relative to HIV negative subjects classified as episodic popper users or non-users. These outcomes included ischemic heart disease, angina pectoris, myocardial infarction, and cardiac dysrhythmias. We also found weaker associations in Caucasian HIV-negative smokers and in HIV-positive non-smokers and smokers.
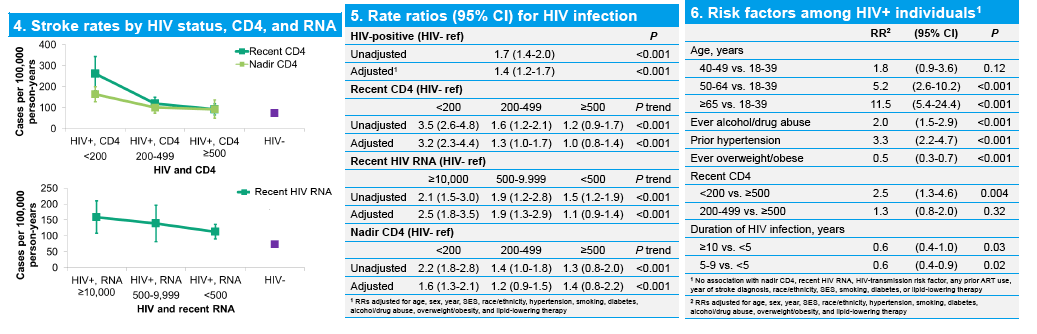
In abstract 741 [HIV Infection and Immunodeficiency as Risk Factors for Ischemic Stroke], risk factors for ischemic stroke among HIV+ and HIV- individuals receiving care in the KP California system. The adjusted RR for HIV patients was 1.4, 95%CI 1.2-1.7) and compared to controls, HIV + subjects with a recent CD4 < 500 ml (RR 1.3, 95%CI 1.0-1.7, P<0.001) and a recent HIV RNA ≥500/ml were at higher risk (RR 1.9, 95% CI 1.3-2.9, P<0.001) with a weaker association with nadir CD4< 200 (RR 1.6, 95%C I 1.3-2.1,P=0.16).
Recent CD4 and recent HIV RNA are stronger risk factors than nadir CD4. HIV+ individuals have a 40% higher risk of ischemic stroke compared with HIV- individuals after adjustment for risk factors. HIV+ individuals with recent CD4 ≥500 or recent HIV RNA <500 are not at significantly greater risk compared with HIV- individuals after adjustment for stroke risk factors, but lower recent CD4 and higher recent HIV RNA are associated with increased risk.
Overall, these studies show that in most but not all cohorts, the increased rate of CVD among HIV-infected individuals remains. Traditional risk factors and careful control of traditional risk factors are key in targeting CV risk in HIV patients. However, HIV-specific features including poorly controlled HIV and immunodeficiency are independently associated with both risk of MI and stroke. Future studies aimed at identifying optimal methods to identify at risk individuals as well as the optimal methods to treat at risk patients are needed.
|
| |
|
 |
 |
|
|