 |
 |
 |
| |
Nearly Nil HIV Transmission Risk Without Condoms and (from Jules: in established couples) With HIV+ Partner on Suppressive ART
|
| |
| |
CROI 2014, March 3-6, 2014, Boston
Mark Mascolini
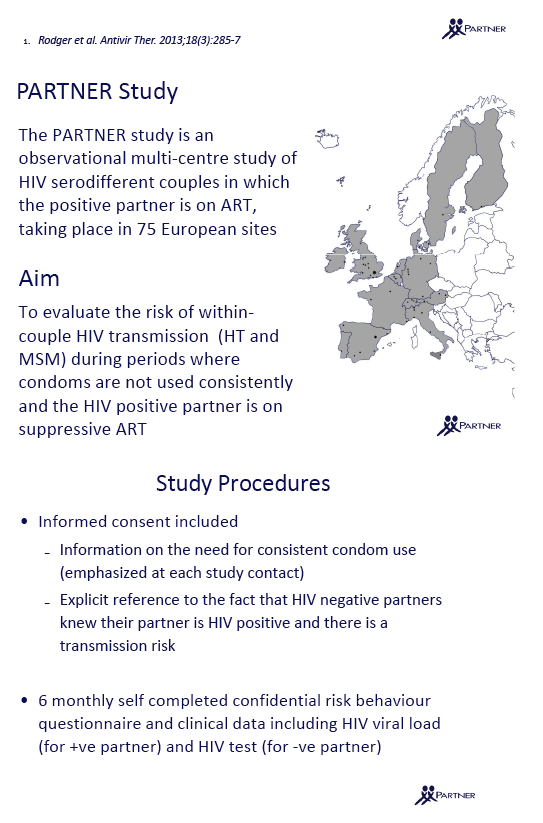
A study of 1110 HIV-discordant European heterosexual and gay couples in which the antiretroviral-treated positive partner had a viral load below 200 found no genetically linked HIV transmissions, even though the partners did not use condoms during the observation time analyzed [1]. Statistical analysis indicated a wider confidence interval for receptive anal intercourse with ejaculation among men who have sex with men (MSM) than for other sex acts.
Although research indicates a low transmission rate within HIV-discordant couples when the positive partner has a low viral load, transmission risk in couples not using condoms has not been rigorously studied. PARTNER study investigators counted only 330 cumulative couple-years of follow-up for condomless sex reported to date [2] and no years of follow-up for condomless anal sex among MSM.
To address these issues, PARTNER investigators recruited HIV-discordant heterosexual and MSM couples at 75 sites across Western Europe, aiming to assess risk of within-couple HIV transmission when the positive partner was taking suppressive antiretroviral therapy (ART) and the couple was not using condoms. Health workers stressed the need for consistent condom use at every study visit, but the analysis considered only periods of condom-free sex during which the positive partner had a sub-200-copy viral load and partners were not using pre- or postexposure prophylaxis. Every 6 months partners completed a risk behavior questionnaire, positive partners had their viral load measured, and negative partners got tested for HIV. When a negative partner became infected with HIV, the researchers phylogenetically compared virus from the partners to see if the transmission occurred within the couple.
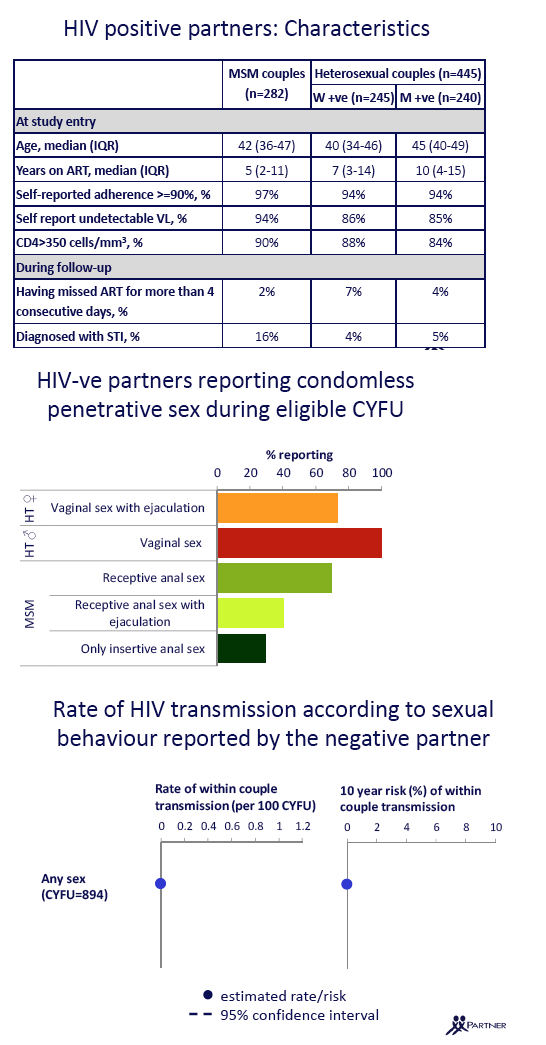
The investigators recruited 1110 couples by November 1, 2013, and 767 couples contributed 894 couple-years of follow-up to this analysis. There were 282 MSM couples, 245 heterosexual couples with a negative male partner, and 240 heterosexual couples with a negative female partner. Median ages at study entry for those three groups were 40, 45, and 40 and median years of condom-free sex at entry 1.5, 2.7, and 3.5. While one third of MSM (34%) had condomless sex with a person outside the couple during follow-up, only 3% of heterosexual men and 4% of heterosexual women did. During a median follow-up of 1.1 years in MSM, 1.5 years in heterosexual men, and 1.5 years in heterosexual women, estimated total numbers of condom-free sex acts were 16,400, 14,000, and 14,000. MSM, HIV-negative heterosexual men, and HIV-negative women had a median of 43, 37, and 37 condomless sex acts per year.
Among HIV-positive MSM partners, positive male heterosexual partners, and positive female heterosexual partners, median ages at study entry were 42, 40, and 45. Respective median years of ART were 5, 7, and 10, and rates of self-reported adherence at or above 90% were 97%, 94%, and 94%. Proportions who missed ART for more than 4 consecutive days during follow-up were 2%, 7%, and 4%. Proportions diagnosed with a sexually transmitted infection were 16%, 4%, and 5%.
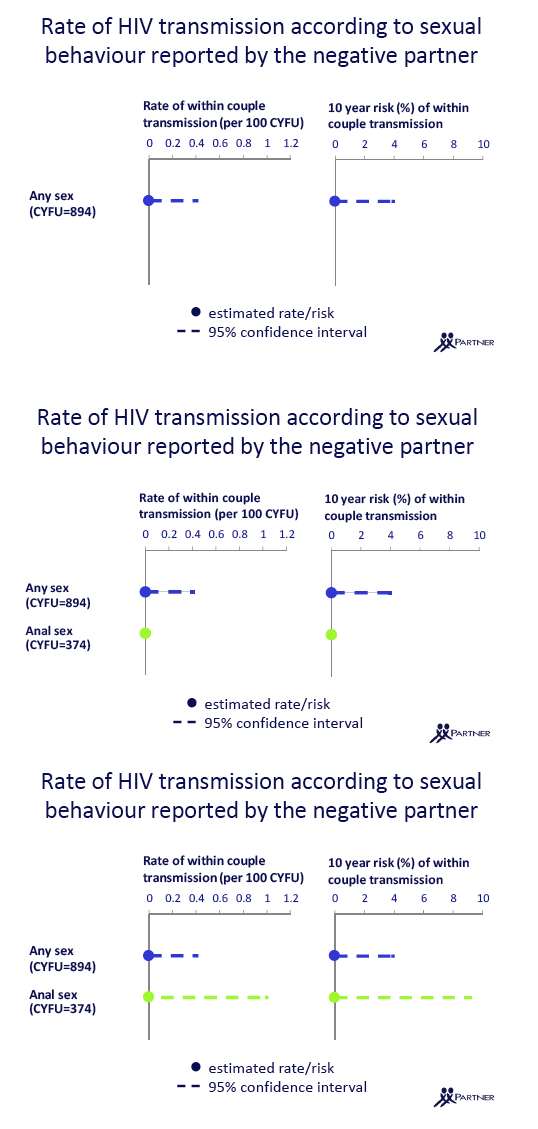
During follow-up the researchers detected no phylogenetically linked HIV transmissions within these couples. Within-couple HIV transmission risk during periods of condom-free sex was 0 for any sex act. Transmission risk was also 0 for anal sex, vaginal sex by men, receptive vaginal sex with ejaculation, insertive anal intercourse by MSM, receptive anal intercourse without ejaculation by MSM, and receptive anal sex with ejaculation by MSM.
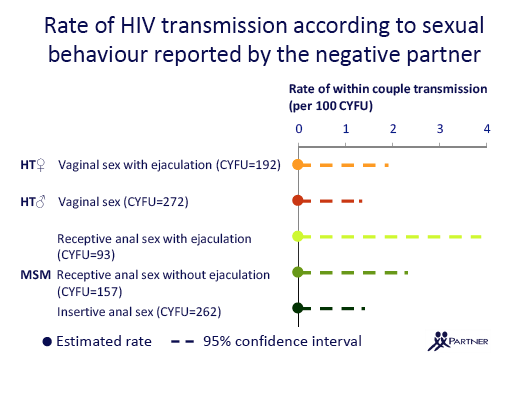
Because couple-years of follow-up differed for each of these sex acts, 95% confidence intervals (CIs) around the 0 for each estimated risk differed substantially (see slides at link following reference 1). For example, the any-sex analysis considered 894 couple-years of follow-up and the 95% CI was 0 to 0.4 per 100 couple-years (from Jules: estimated 10-year risk of 4%). The anal sex analysis had 374 person-years of follow-up and the 95% CI stretched 0 to 0.96 per 100 couple-years (from Jules: 10-year risk approaching 10%). Women having vaginal sex with ejaculation had 192 couple-years of follow-up and the 95% CI reached from 0 to about 2 per 100 couple-years. For receptive anal intercourse with ejaculation among MSM there were only 93 couple-years of follow-up, and the 95% CI extended from 0 to about 4 (from Jules: "the most risky type of sex for the transmission of HIV which is still a significant risk of transmission & that translates into 32% risk at 10 years, but looking at slide you will see this group had the smallest N, number of participants").
Link to CROI webcast:
http://www.croiwebcasts.org/console/player/22072?mediaType=slideVideo&
"The overall risk of HIV transmission (in the context of previous sex without transmission) through condomless anal or vaginal sex from HIV-positive people on ART with plasma viral load below 200 copies/mL is extremely low," the researchers conclude. But "uncertainty over the upper limit of risk remains, particularly over receptive anal sex with ejaculation." They noted that additional follow-up of MSM through the 2014-2017 PARTNER 2 study should provide more precise estimates of transmission risk in this group.
from Jules: during the Q&A a question was raised about that this study was conducted among couples who had sex with out transmission, established couples with a history of condomless sex without transmission, so the question raised the issue ("the healthy survivor effect") what about for new couples without a history of sex, would this finding hold true, would you in this study miss transmissions that might occur in other new couples, in other words in this study you captured only couples who had condomless sex without transmission, maybe there are couples for whom this might not happen, maybe transmission would occur, and the presenter Alison Rodger said I completely agree with you, that is the trouble with all transmission studies, that is why I said this is in the context of condomless sex without transmission.
References
1. Rodger A, Bruun T, Cambiano V, et al. HIV transmission risk through condomless sex if HIV+ partner on suppressive ART: PARTNER Study. CROI 2014. Conference on Retroviruses and Opportunistic Infections. March 3-6, 2014.
Boston. Abstract 153LB. www.chip.dk/portals/0/files/CROI_2014_PARTNER_slides.pdf
2. Rodger AJ, Bruun T, Vernazza P, et al. Further research needed to support a policy of antiretroviral therapy as an HIV prevention initiative. Antivir Ther. 2013;18:285-287.


|
| |
|
 |
 |
|
|