 |
 |
 |
| |
Arterial Inflammation Tied to High-Risk Coronary Plaques in HIV Group
|
| |
| |
CROI 2014, March 3-6, 2014, Boston
Mark Mascolini
A study of 41 people on stable antiretroviral therapy (ART) with no history of heart disease linked PET scan-measured arterial inflammation to high-risk coronary artery plaques [1]. The finding extends the understanding of heightened cardiovascular disease risk in people with HIV.
Several studies confirm higher cardiovascular disease rates in men and women with HIV than in the general population. Although reasonable explanations for this association abound, research has not nailed down a physiologic mechanism. To address this question, Markella Zanni and Massachusetts General Hospital (MGH) colleagues explored potential links between arterial inflammation and high-risk coronary artery plaques in HIV-positive people with subclinical coronary atherosclerosis.
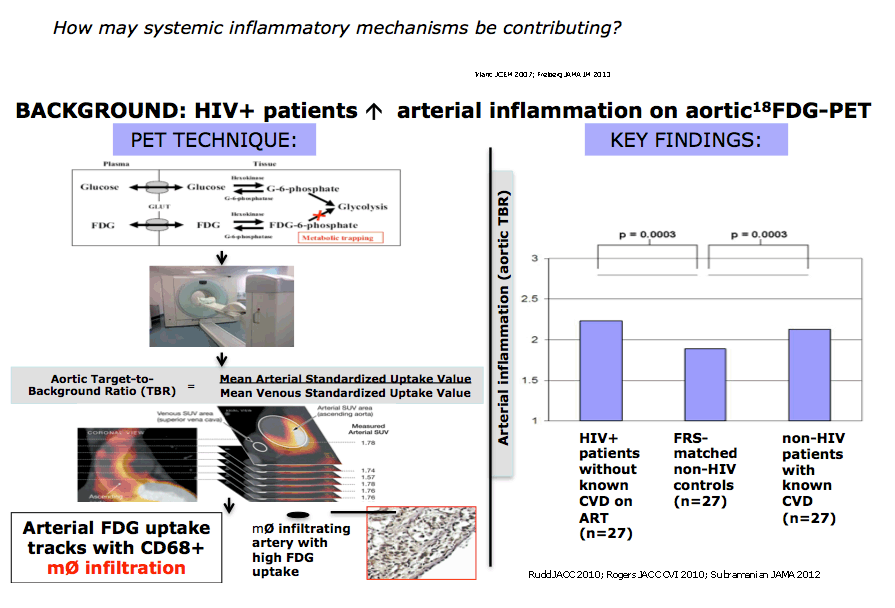
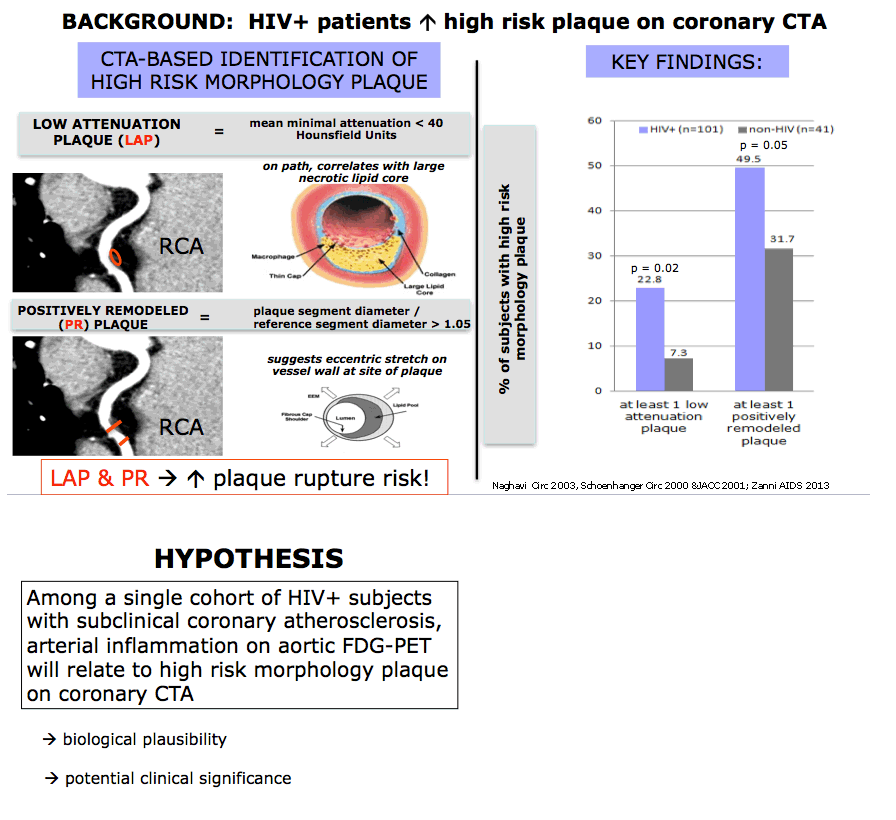
Using coronary computed tomography angiography (CTA), the MGH group previously found a higher prevalence of high-risk coronary plaques (those with a tendency to rupture) in HIV-positive than HIV-negative people [2]. Work by the MGH team [3] and others used PET scans to determine that HIV-positive people have higher rates of arterial inflammation than people without HIV.
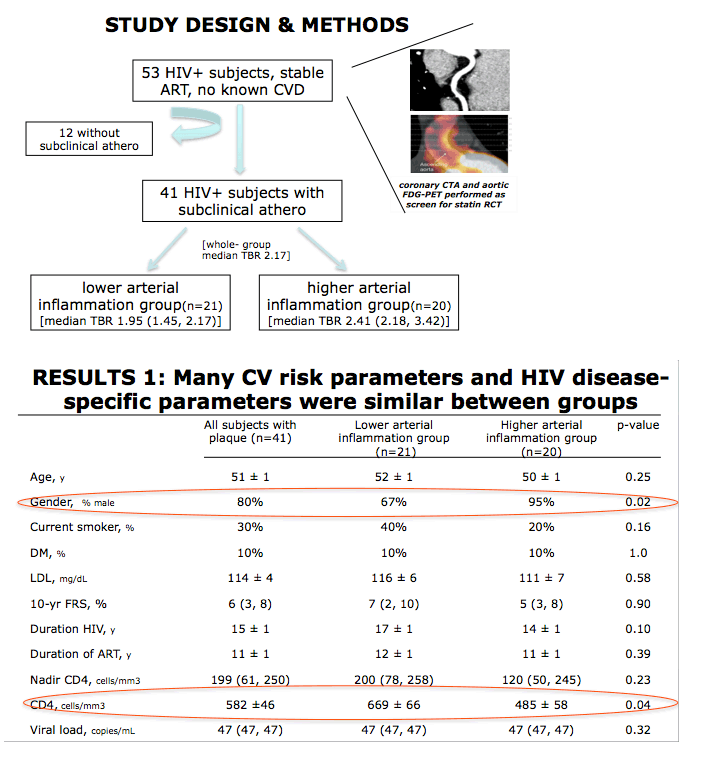
In the new study Zanni and colleagues set out to see whether these two pieces of evidence fit together. They focused on 41 HIV-positive people on stable antiretroviral therapy and without a cardiovascular disease history but with subclinical atherosclerosis indicated by coronary plaque on CTA. The researchers divided this group into 21 people with arterial inflammation below the group median and 20 with inflammation above the group median (PET-determined target-to-background ratio [TBR] of 2.17).
The high-inflammation group had a higher proportion of men than the low-inflammation group (95% versus 67%, P = 0.02) and a lower average CD4 count (485 versus 699, P = 0.04). But the groups did not differ in age (average 51 overall), current smoking (30%), diabetes (10%), 10-year Framingham risk score (6), HIV duration (15 years), antiretroviral duration (11 years), nadir CD4 count (199), or viral load (47 copies/mL).
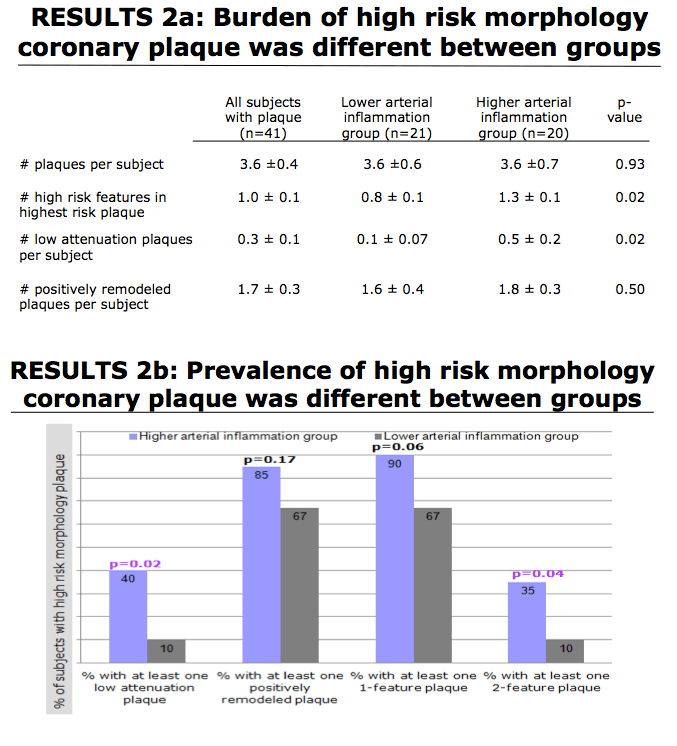
People in the high-inflammation group did not differ from those in the low-inflammation group in average number of plaques per person (3.6 in both groups). But the high-inflammation group had a higher average number of high-risk plaque features in the highest-risk plaques (1.3 versus 0.8, P = 0.02) and a higher number of low-attenuation plaques (average 0.5 versus 0.1 per person, P = 0.02). Among people in the high-inflammation group, 40% had at least one low-attention plaque, compared with 10% of the low-inflammation group (P = 0.02). The high- and low-inflammation groups also differed in the proportion with at least one plaque that had two high-risk features (35% versus 10%, P = 0.04).
Multivariate modeling determined that both median TBR in the high-inflammation group (beta estimate 0.35, P = 0.004) and HIV duration (beta estimate 0.04, P = 0.05) were associated with number of low-attenuation plaques per person. Gender, CD4 count, and LDL cholesterol were not associated with number of low-attenuation plaques in this analysis.
The MGH team concluded that their findings "are the first to demonstrate a relationship between arterial inflammation and high-risk morphology coronary plaque in HIV-positive patients." They cautioned that their analysis is limited by measurement of arterial inflammation in the aorta rather than coronary arteries, the small sample size, and the cross-sectional design. The researchers called for further study to determine whether arterial inflammation measured over time predisposes HIV-positive people to high-risk plaques and to test inflammation-quelling strategies to see if they prevent plaque rupture and myocardial infarction.
Link to CROI webcast:
http://www.croiwebcasts.org/console/player/22264?mediaType=slideVideo&
References
1. Tawakol A, Zanni MV, Lo J, et al. Increased arterial inflammation relates to high-risk coronary plaque morphology in HIV+ patients. CROI 2014. Conference on Retroviruses and Opportunistic Infections. March 3-6, 2014. Boston. Abstract 130.
2. Zanni MV, Abbara S, Lo J, Wai B, Hark D, Marmarelis E, Grinspoon SK. Increased coronary atherosclerotic plaque vulnerability by coronary computed tomography angiography in HIV-infected men. AIDS. 2013;27:1263-1272.
3. Subramanian S1, Tawakol A, Burdo TH, et al. Arterial inflammation in patients with HIV. JAMA. 2012;308:379-386.
http://jama.jamanetwork.com/article.aspx?articleid=1221700.
http://www.natap.org/2012/HIV/072512_01.htm
Arterial Inflammation in Patients With HIV.......from Jules: patients with low-risk on Framingham score, subclinical heart disease, can have arterial inflammation placing them at increased risk at heart disease events and traditional tools to assess risk may be inadequate
JAMA. July 25 2012
Sharath Subramanian, MD; Ahmed Tawakol, MD; Tricia H. Burdo, PhD; Suhny Abbara, MD; Jeffrey Wei, BA; Jayanthi Vijayakumar, MD; Erin Corsini, BS; Amr Abdelbaky, MD; Markella V. Zanni, MD; Udo Hoffmann, MD, MPH; Kenneth C. Williams, PhD; Janet Lo, MD, MMSc; Steven K. Grinspoon, MD
http://www.natap.org/2012/HIV/072512_01.htm
"Participants infected with HIV vs noninfected control participants with similar cardiac risk factors had signs of increased arterial inflammation, which was associated with a circulating marker of monocyte and macrophage activation.......monocyte and macrophage activation could play a critical role in the early expression of subclinical atherosclerosis in patients with HIV."
"Our observation that HIV infection is associated with increased arterial inflammation, even among relatively young patients with HIV with low FRS [Framingham risk score] and undetectable viremia, is concordant with the epidemiological observations that patients with HIV have a higher risk of stroke and myocardial infarction than patients without HIV1 ,20 and demonstrates that this risk may not be measured adequately by traditional risk assessment tools, such as the FRS."
------------------------------


|
| |
|
 |
 |
|
|