 |
 |
 |
| |
Bone Density Changes after Antiretroviral Initiation with Protease Inhibitors or Raltegravir
|
| |
| |
Reported by Jules Levin
CROI 2014 March 3-6 Boston, MA
Late Breaker
Todd T. Brown1,Carlee Moser2, Judith S. Currier3 Heather Ribaudo2, Jennifer Rothenberg4, Michael P. DubŽ5, Robert Murphy6, James H. Stein7, Grace A. McComsey8, 1Johns Hopkins University, 2Harvard School of Public Health, 3David Geffen School of Medicine at University of California - Los Angeles, 4Social & Scientific Systems, Inc, 5Keck School of Medicine at the University of Southern California, 6Northwestern University, 7University of Wisconsin School of Medicine and Public Health, 8Case School of Medicine
Program Abstract:
Background: The initiation of antiretroviral therapy (ART) leads to a 2-6% loss of bone mineral density (BMD) over 48-96 weeks which depends in part
on the specific medications used. The effect of integrase inhibitors on BMD with ART initiation and how it compares to the changes seen with protease
inhibitors (PIs) have not been clearly established.
Methodology: We compared the percentage change in BMD at the lumbar spine, total hip, and total body over 96 weeks in HIV-infected treatment-naive
participants randomized equally to open labeled Tenofovir Disoproxil Fumarate-Emtricitabine (TDF/FTC) plus Atazanavir-Ritonavir (ATV/r), Darunavir-
Ritonavir (DRV/r), or Raltegravir (RAL) in a substudy of AIDS Clinical Trials Group A5257 (N= 1809) with randomization stratified by substudy participation.
BMD was measured using standardized dual-energy x-ray absorptiometry (DXA) and centrally read. We used linear regression with reverse Helmert
contrasts to compare the 96-week percentage change in BMD in the two PI arms (ATV/r vs DRV/r) and, if no difference was found, the BMD changes in
the combined PI arms were compared to those in the RAL arm. Primary analyses were intent-to-treat, adjusted for the stratification factors of baseline
cardiometabolic risk and HIV-1 RNA.
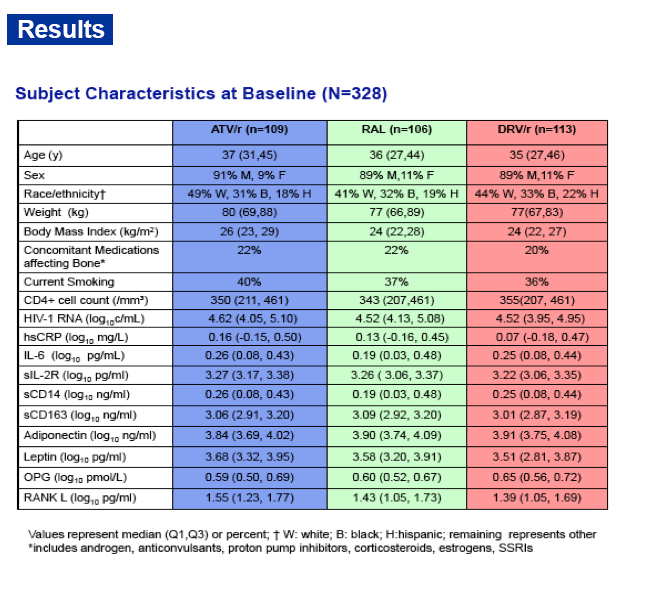
Results: Three hundred and twenty eight participants were randomized and had baseline DXA scans. At baseline, 90% were male and 44% were white,
non-Hispanic; the median HIV-1 RNA load was 4.55 log10 copies/mL; age was 37 years; CD4 count was 349 cells/μL. At week 96, the mean percentage
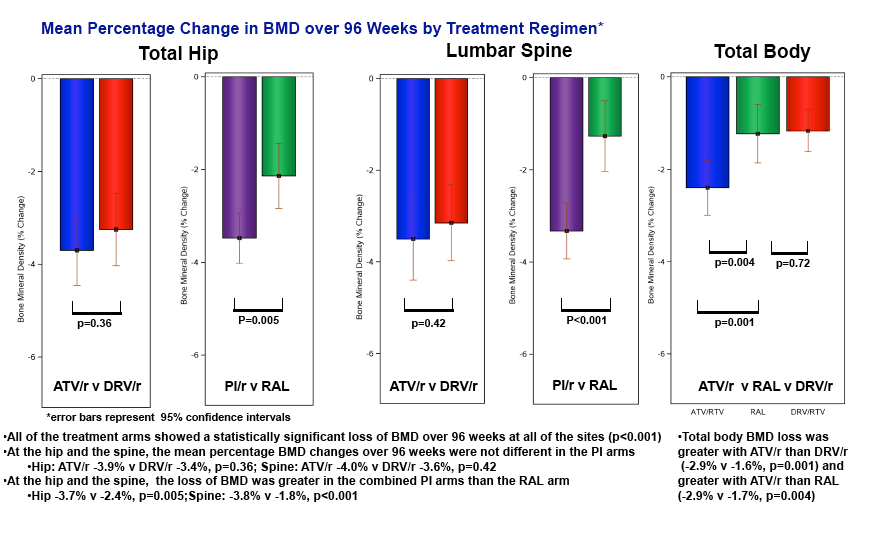
changes from baseline in spine and hip were statistically significant in all arms (p>0.001) and similar in the PI arms (Spine: ATV/r -4.0% v DRV/r -3.6%,
p=0.42; Hip: ATV/r -3.9% v DRV/r -3.4%, p=0.36), but were greater in the combined PI arms than the RAL arm (Spine: -3.8% v -1.8%, p<0.001; Hip
-3.7% v -2.4%, p=0.005). The percentage changes in total body BMD were small, but statistically significant in all of the arms (p<0.001 for all), but the
magnitude of the change was greater with ATV/r than DRV/r (-2.9% v -1.6%, p=0.001) or RAL (v -1.7%, p=0.004), but not different between the DRV/r
and RAL arms (p=0.72). As-treated analyses led to similar results.
Conclusions: In ART-na•ve, HIV-infected individuals initiating ART with TDF/FTC, 96 week BMD losses at the lumbar spine and total hip were similar with
the PIs, ATV/r and DRV/r, whereas the integrase inhibitor, RAL, had significantly less BMD loss at these sites than the combined PIs arms. In contrast, total
body BMD loss was slightly greater with ATV/r than DRV/r.




|
| |
|
 |
 |
|
|