 |
 |
 |
| |
Low Bone Mineral Density among Ugandan HIV infected patients on failing first line Antiretroviral Therapy; a sub-study of the EARNEST trial
|
| |
| |
Reported by Jules Levin
CROI 2014 March 3-6 Boston, MA
Bonnie Wandera1, Agnes Kiragga1 , Fred Semitala1, Jayne Ellis1, Robert Colebunders3, Nicholas Paton4, Andrew Kambugu1, Philippa Easterbrook1
1-Infectious Diseases Institute Makerere University Kampala Uganda , 2- School of Medicine Makerere University ,Kampala Uganda , 3-Institute of Tropical Medicine Antwerp Belgium 4-MRC-Clinical trials unit, London
Uganda , 2- School of Medicine Makerere University ,Kampala Uganda , 3-Institute of Tropical Medicine Antwerp Belgium 4-MRC-Clinical trials unit, London
Program Abstract:
Background: Both HIV infection and use of ART are associated with increased risk of low BMD. There have been few studies of BMD in sub-Saharan Africa.
We examined the prevalence of osteopenia and osteoporosis and factors associated with low BMD among patients failing first-line ART in Kampala, Uganda.
Methodology: Sub-study of the Europe - Africa Research Network for Evaluation of Second-line Therapy, EARNEST trial, a large randomized trial of three
different second-line ART strategies in protease inhibitor - naïve patients with evidence of first-line ART failure in 5 African countries. BMD was measured
using Dual energy x-ray absorptiometry scans (DXA) at lumbar spine (LS) and hip. Data on potential risk factors for low BMD i.e age, CD4 cell count,
plasma viral load, Body mass index (BMI), prior ART regimens, alcohol use, and dietary calcium intake were collected. Low BMD was defined as T-score <
-1, with osteoporosis and osteopenia less than -2.5 and between -2.5 and -1 respectively. Logistic regression was used to identify factors associated with
low BMD (T-score < -1).
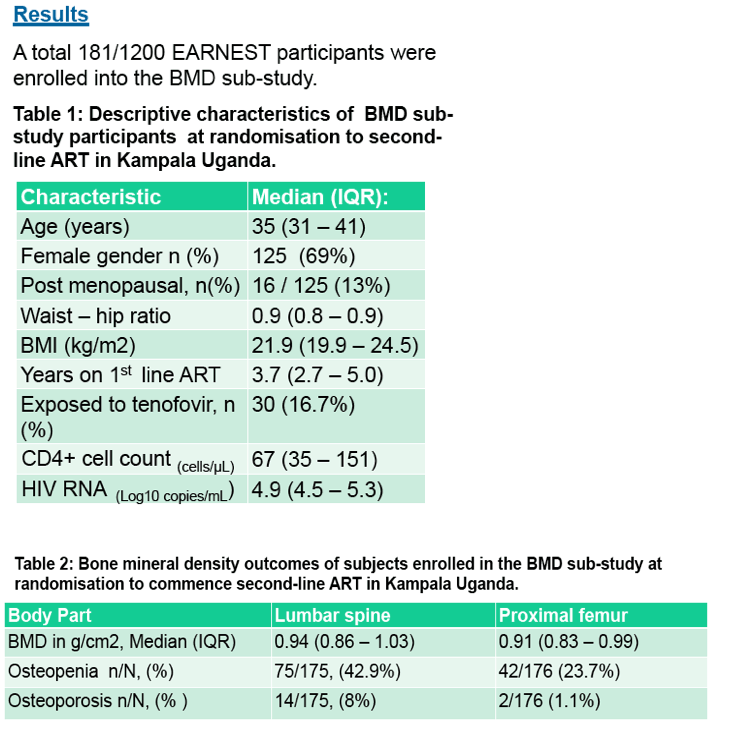
Results: 181/1200 EARNEST participants from 3 sites in Uganda were enrolled into this sub-study. Of these ,125 (69%) were female (16 (12.8%) postmenopausal),
median (interquartile range, IQR) baseline values were: age 35 (31-41) years, duration of 1st line ART 3.7(2.7-5.0) years (30 (16.7%) had used TDF), CD4 67 cells (35-151),
and viral load log 4.9 (4.5-5.3), and a low (<18.5 kg/m2), and high (≥ 25 kg/m2) BMI were present in 19 (10.5%) and 44 (24.3%) of subjects.
Median (IQR) BMD for lumbar spine and left hip were 0.94(0.86-1.03) and 0.91(0.83-0.99) gms/cm2 respectively. A total of 89/175 (50.1%) and 44/176 (25%)
had low BMD at the lumbar-spine and hip respectively. The prevalence of osteoporosis was 8% at the LS and 1.1% at the hip while osteopenia was present in 46.6% and 27.1%
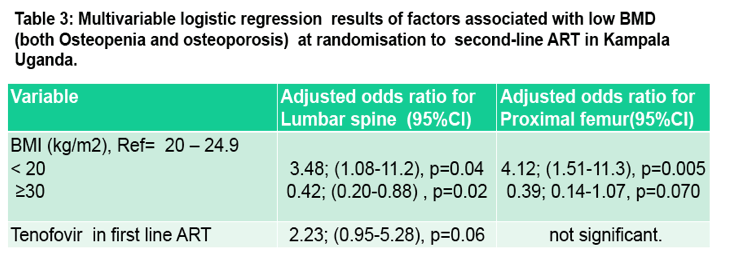
at the LS and hip respectively. Low BMD at lumbar spine was associated with both low BMI (adjusted odds ratio [AOR] 3.48; 95% Confidence interval (CI) 1.08-11.2),
and high BMI (AOR 0.42; 0.20-0.88) as compared to normal BMI, and use of TDF in first-line regimen (AOR 2.23; 95% CI 0.95-5.28, p= 0.06).
At the Hip, a low BMI was predictive of low BMD, (AOR 4.12; 1.51-11.3) while overweight was protective, (AOR 0.39; 0.14-1.07).
Age, gender, and CD4 cell count were not associated with low BMD.
Conclusions: More than half of the Ugandan patients failing first line ART had low BMD but osteoporosis was present in < 10%. The prevalence of low
BMD in general and osteoporosis was comparable with cross-sectional data from Europe and US. However, in the 10% with a low BMI, there was a 3.5 fold
increased risk of low BMD. Subjects with a low BMI and those receiving TDF have an increased risk of low BMD and may need bone health evaluation and
close monitoring of their BMD while on ART.



|
| |
|
 |
 |
|
|