 |
 |
 |
| |
Cancers in HIV+ at CROI
|
| |
| |
CROI: Quadrivalent HPV Vaccine Induces Immune Memory in US Men With HIV - written by Mark Mascolini - (03/06/14)
CROI: Five Cancers Diagnosed at Later Stage in People With vs Without HIV - written by Mark Mascolini - (03/05/14)......NCI team proposed that "the increased stage observed in people with HIV is likely driven by delayed diagnosis due to under-utilization of care, particularly for screen-detectable cancers, and is unlikely to be due to immune suppression increasing cancer progression."
Oral talk at CROI: HIV and Elevated Cancer-Specific Mortality Following Cancer
Diagnosis in the United States, from the NIH NCI
.......Non-AIDS cancers are increasing among HIV+ & nonAIDS cancers which represents most of the types of cancers in the US are experiencing. HIV increases risk of developing cancer. But we don't that much about if an HIV+ cancer patient is different then an HIV-uninfected cancer patient. There isn't that much in the literature on this question. There isn't that much on if the outcome is different based on one's HIV status. Although a published paper last year found HIV+ lung cancer patients were dying more often than the HIV-unifected lung cancer patients. study aim: determine whether HIV-infected cancer patients experience elevated mortality due to cancer compared to HIV-uninfected cancer patients in the US. We identified cancer cases from 5 U.S. cancer registries participating in the HIV/AIDS Cancer Match Study. HIV status of cancer patients was determined through linkage with HIV registries. The HIV+ cancer patients were younger/much younger ages at which cancers were reported, more likely to be African-American, and more likely to have higher stages of cancers, which clearly I think is a problem when trying to treat & arrest a cancer. The risk of dying for an HIV-infected patient was higher than for an HIV-uninfected patient in 8 cancers listed in a table in the slide presentation and includes these cancers melanoma, lung, larynx, liver, colon & rectum, anus and true for 9/14 cancers considered, HIV+ experienced statistically significant elevated cancer mortality compared to HIV-uninfected, and for an additional 3 cancer there were suggested elevations, marginally significant. The authors conclude & summarize: HIV/AIDS patients experience elevated mortality due to cancer compared to HIV-uninfected cancer patients in the US. The relationship was observed after adjustment for cancer stage & was observed or suggested for 12 of 14 cancer diagnoses.Follow-up work is planned.In the Q&A the author said, & I think is this a limitation of the study, that since this is a registry they don't have info on the care of these patients such as are they on HAART, what is their CD4 & viral load. Another Q&A comment said I think your data is correct, in his experience the surgical part of the cancer is not a problem in HIV+ individuals but despite on HAART & good CD4s have less bone marrow reserve & so they end up "less fit" after chemotherapy than someone who is HIV-negative and in response the presenter mentioned a study in which less treatment was administered to lung cancer HIV+ patients and this could be a potential explanation for the survival differences.
CROI webcast:
http://www.croiwebcasts.org/console/player/22230?mediaType=slideVideo&
The presenter refers to this graph & 2011 published study in JNCI [http://www.natap.org/2011/HIV/041311_02.htm]:
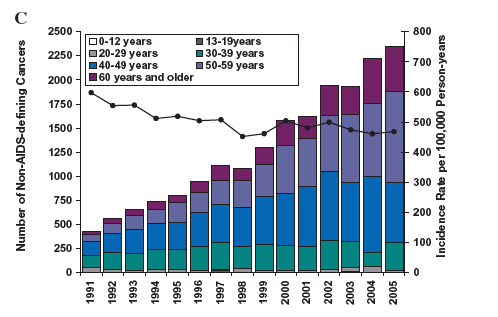
Figure 1 further depicts the trends in cancer burden in the AIDS population. From 1991 to 2005, AIDS-defining cancers declined in most age groups, with the largest declines among 20-39 year olds (Figure 1, B). The decline in cancer burden of AIDS-defining cancers was driven by a steep decline in the standardized incidence rate of these cancers (Ptrend < .001) (Figure 1, B). In contrast, there was an increase in the cancer burden attributable to non-AIDS-defining cancers, which was limited to people aged 40 years or older (Figure 1, C). This rise in cancer burden occurred despite a modest decline in the standardized incidence rate (Ptrend < .001) (Figure 1, C). As a result of these changes, the total cancer burden in the AIDS population decreased during 1991-1998, but increased subsequently, driven by the rise in number of non-AIDS-defining cancers (Figure 1, D).
HIV Patients at More Risk of Developing 20 Cancers, Study Shows
The Lancet July 7, 2007; 370:59-67
Incidence of cancers in people with HIV/AIDS compared with immunosuppressed transplant recipients: a meta-analysis
http://www.natap.org/2007/HIV/070607_01.htm
"The bulk of the data came from studies that followed people only after the onset of AIDS,4,9,10 and in the era of highly active antiretroviral therapy (HAART), these people comprise an increasing minority of HIV-infected people."
for this program abstract the NCI/authors did not want to share pdf saying they wanted to publish:
Excess Burden of Cancer Among HIV-Infected Persons in the United States
Hilary A. Robbins1, Meredith S. Shiels1, Ruth M. Pfeiffer1, Jianmin Li2, H. Irene Hall2, Eric A. Engels1
1Division of Cancer Epidemiology and Genetics, National Cancer Institute, Bethesda, MD, United States, 2National Center for HIV/AIDS, Viral Hepatitis, STD, and TB Prevention, Centers for Disease Control and Prevention, Atlanta, GA, United States
Background: Nearly 1 million people in the U.S. have diagnosed HIV infection and therefore increased cancer risk, but total cancer burden in the U.S. HIV population has not been quantified. We estimated the total number of incident cancers, and the number in excess of expected, among HIV-infected persons in the U.S. during 2010.
Methodology: To estimate cancer rates among HIV-infected persons, we applied Poisson models to linked HIV and cancer registry data from 6 states in the HIV/AIDS Cancer Match Study. We used data from the Surveillance, Epidemiology, and End Results (SEER) program for general population (expected) cancer rates. We applied these rates to CDC estimates of people living with diagnosed HIV infection, stratified by age, sex, race/ethnicity, HIV risk group, and AIDS-relative time, to calculate total and excess (i.e., total - expected) cancer cases in 2010.
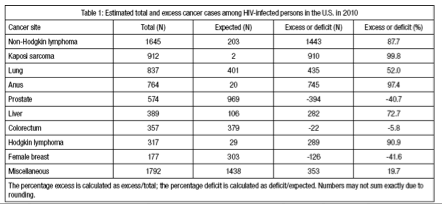
Results: An estimated 7,764 cancers occurred among HIV-infected people, 3,915 (50.4%) in excess of expected. The most common cancer was non-Hodgkin lymphoma (N=1,645, 87.7% excess; Table 1), and nearly all cases were excess for Kaposi sarcoma (N=912, 99.8% excess), anal cancer (N=764, 97.4% excess), and Hodgkin lymphoma (N=317, 90.9% excess). Fewer than expected cases occurred for colorectal cancer (N=357, 5.8% deficit), prostate cancer (N=574, 40.7% deficit), and female breast cancer (N=177, 41.6% deficit). Most cancers occurred among males (N=6,237; 51.5% excess), specifically men who have sex with men (N=4,545; 55.9% excess). By age, the largest excess was among ages 40-49 (N=1,610), though the largest proportional excess was among ages 15-29 (92.7%). There was no excess among the oldest group (age ≥70). While most cancers occurred among non-Hispanic blacks (N=3,293) and whites (N=2,870), a larger proportional excess was among Hispanics (64.4%).
Conclusions: HIV infection in the U.S. is associated with a substantial excess burden of cancer, which largely occurs among men and individuals under 50. Despite major improvements in HIV treatment, approximately half of almost 8,000 cancer cases among HIV-infected persons in 2010 were excess cases.
|
| |
|
 |
 |
|
|