| |
The Burden of Untreated Hepatitis C Virus Infection: A US Patients' Perspective.......
|
| |
| |
Download the PDF here
HCV+ reported greater work impairment (26% vs 16%), more activity impairment (42% vs 23%)....more emergency room visits, hospitalizations & physician visits, greater direct health costs ($22 mill vs $12 mill: ER visits/hospitalization, physician visits) & indirect costs (($10 mill vs $5 mill: work absenteeism/presenteeism), greater productivity losses: $23,000 per patient year, approximately $10,000 more than for average survey respondent & about $7500 more than for matched controls......Average incremental cost for each untreated HCV infected patient was approximately $9,000 compared with matched controls. It is important to remember these costs do not include the cost of HCV treatment, or the adverse events associated with it.
Dig Dis Sci (2012)
Antoine C. El Khoury · Jeffrey Vietri · Girish Prajapati
A. C. El Khoury Merck & Co., Inc., WP 97-A423, 770 Sumneytown Pike, West Point, PA 19486, USA
J. Vietri Kantar Healt
h, One Independence Way, Suite 220, Princeton, NJ 08540, USA
G. Prajapati AllSource PPS, 16371 Beach Blvd, Suite 221, Huntington Beach, CA 92647, USA
Authors Conclusions:
Untreated HCV infection is a costly illness, both economically and in terms of quality of life. The economic cost to society of impaired work productivity and increased use of healthcare resources is substantial, and there is a significant impact on both mental and physical health. The results of this study highlight the economic and humanistic burden that HCV can cause to patients and society if left untreated.
Aims - To estimate the impact of untreated HCV infection on work productivity, daily activity, healthcare use, economic costs, and health-related quality of life (HRQoL).
Methods Respondents to the 2010 US National Health and Wellness Survey (n = 75,000) reporting physician diagnosis of HCV infection but not current or previous treatment (patients) were matched to respondents without HCV infection (controls) by use of propensity scores......Self-reported work impairment, activity impairment, healthcare resource use, and HRQoL were compared between patients and controls. Indirect and direct costs were estimated.
Results: A total of 306 patients met inclusion criteria. Patients were more impaired at work than controls, with overall work impairment of 26 % versus 15 %, respectively (P<0.001), mostly because of presenteeism in both groups. Annual productivity losses were estimated at $10,316 per employed patient compared with $5,469 per control (P<0.001). Patients used more healthcare, with all-cause healthcare costs estimated at $22,818 per patient annually, compared with $15,362 per control (P\0.001). HRQoL and activity impairment were also worse among patients than controls.
---------------------
Treatment-naőve HCV infected patients reported significantly impaired work productivity, greater impairment of non-work activity, more healthcare resource utilization, higher estimated costs, and worse health-related quality of life compared with unmatched and propensity-matched subjects without HCV infection. Overall work impairment averaged more than 25 %, well above the 15 % figure for non-HCV controls. The average employed untreated HCV infected patient loses over $10,000 worth of productivity because of ill health, nearly double that lost by either the average patient in the NHWS without HCV or propensity matched controls. Healthcare resource use was also greater, especially for outpatient physician visits, which were nearly 50 % more frequent than for the matched controls.
Direct costs were even larger than the productivity losses, averaging nearly $23,000 per patient per year, approximately $10,000 more than for the average survey respondent, and approximately $7,500 more than for matched controls. Average incremental cost for each untreated HCV infected patient was approximately $9,000 compared with matched controls. It is important to remember these costs do not include the cost of HCV treatment, or the adverse events associated with it.
HCV patients differed in a variety of ways from unmatched non-HCV controls......
- HCV patients versus non-HCV subjects were older (53 vs. 48 years old, P\0.001),
- more likely to be male (64 vs. 48 %, P\0.001), and
- less likely to be heterosexual (86 vs. 91 %, P\0.01) or to live with a partner (46 vs. 60 %, P<0.001).
- less likely to have graduated from high school (95 vs. 97 %, P\0.05),
- less likely to be employed (40 vs. 55 %, P\0.001), or
- less likely to have health insurance (73 vs. 83 %, P<0.001) than non-HCV
subjects in the NHWS, and
- tended to have lower household income.
- They also had poorer health habits, being less likely to be normal weight (23 vs. 31 %, P<0.01) and
- more likely to be obese (37 vs. 33 %, P<0.05),
- smoke cigarettes (44 vs. 19 %, P<0.001), and
- less likely to exercise (57 vs. 65 %, P<0.01).
- They were less likely to drink alcohol (56 vs. 65 %, P<0.001), although more than half reported doing so.
- They also suffered from more non-liver co-morbid health conditions (0.78 vs. 0.37, P<0.01). As expected, they were also much more likely to suffer from cirrhosis (3.9 vs. 0.1 %, P<0.001) or liver cancer (0.7 vs. 0.0 %, P<0.001).
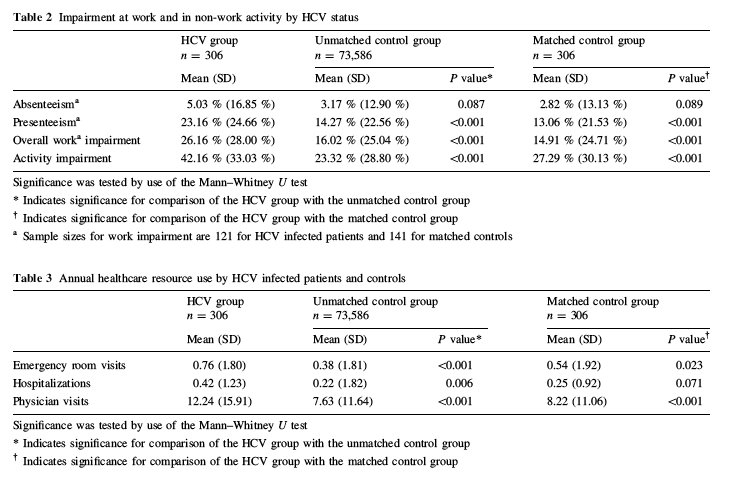
Treatment-naőve HCV infected patients had....
- greater presenteeism,
- overall work impairment, and activity impairment (Table 2), and
- used more healthcare resources (Table 3).
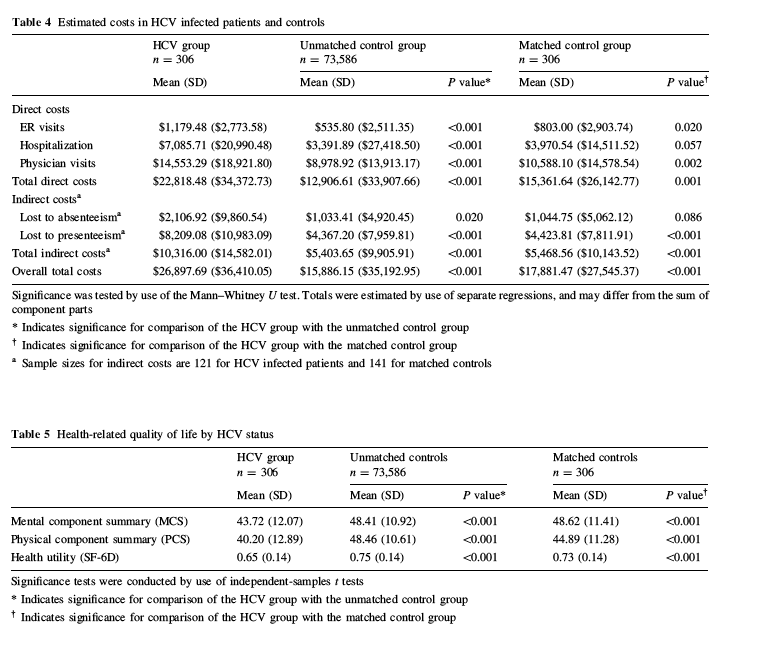
- estimated costs were significantly higher for untreated HCV infected patients than for the unmatched control group.
- lower HRQoL than matched controls on all three SF-12 metrics (Table 5). Differences on MCS (43.72 vs. 48.62, P<0.01) and PCS (40.20 vs. 44.89, P\0.01) were more than four points lower than for those without HCV, suggesting a clinically important difference
- Health utilities were 0.08 point lower (0.65 vs. 0.73, P\0.001), which would also be considered clinically meaningful
"Consistent with previous studies of chronic HCV infection, we found HCV diagnosis had a significant impact on a range of outcomes. The magnitude of these effects was comparable with those in other studies which relied on different data sources or inclusion criteria. Our analysis of self-reported work productivity found that absenteeism was approximately 80 % higher for untreated HCV infected patients, similar to a recent analysis of the Human Capital Management Services Research Reference Database, although the values for the patients and controls were half of those reported in that study [19]. Absenteeism figures reported here are also similar to those in an analysis of the 2009 NHWS data that did not exclude HCV patients on the basis of treatment status [18]. Our results for presenteeism and overall work impairment show a greater [20] decrement in the HCV group than the 2009 data, however, perhaps because of the inclusion of successfully treated patients in that analysis. We are not aware of another study estimating the indirect costs of work productivity loss, which were substantial among the employed patients. The impact of HCV on direct costs reported here is consistent with a recent analysis of untreated HCV infected patients in the Ingenix database, which found all-cause medical expenditure to be approximately $19,000 per year in 2007 dollars, not including pharmacy costs [9]. It is, however, higher than another recent analysis, which is, in part, likely to be because of the inclusion of patients achieving SVR in that sample [12]. The HRQoL burden is slightly larger than that reported in previous studies of HCV infected patients which did not exclude currently or previously treated patients [24], suggesting that studies which include treated patients may underestimate the impact of HCV infection.
Although these analyses revealed an impact of HCV on a broad range of health outcomes, not every metric was significantly affected. Treatment-naőve HCV infected patients were much more impaired while at work, but did not miss significantly more work than controls. Part of this could be lack of sensitivity of the WPAI, because the recall period is only seven days, and even those who miss a substantial amount of work per year are relatively unlikely to miss work in a given week. A previous study using an employer database revealed a significant, but relatively subtle, impact of HCV on work attendance, and a larger impact on productivity [19]. Likewise, untreated HCV infected patients had more physician visits and use of the ER. The difference in hospitalizations was not statistically significant, although the magnitude of the difference-68 % higher among patients than controls-suggests this null result may be because of small sample size and the resulting lack of statistical power rather than comparable rates of hospital admission."
"The advent of new direct-acting antiviral agents will shorten treatment duration, likely increase the number of people offered treatment, and improve HCV cure rates (final two steps of the HCV treatment cascade) [15], [35]. However, educating providers and the general public about HCV prevention, care, and treatment; ensuring access to providers skilled in the treatment of HCV infection; and addressing the high cost of these agents will be critical to maximizing the benefits of these new therapies [14], [39]. In a recent cost-effectiveness simulation evaluating birth-cohort HCV screening and subsequent treatment of HCV-infected adults, Rein and colleagues [http://www.natap.org/2012/HCV/022212_04.htm] note that birth-cohort screening followed by HCV treatment including direct-acting antiviral agents will increase quality-adjusted life-years (QALYs) by $532,200 and medical costs by $19.0 billion, for an incremental cost-effectiveness ratio of $35,700 per QALY saved (95% credible interval, $28,200 to $47,200) [40]. While these simulations accounted for common HCV-associated complications, funders, public health administrators, and providers should be aware of the financial burden of untreated HCV infection. Using data from the 2010 U.S. National Health and Wellness Survey, El Khoury et al. note that persons with untreated HCV infection had significantly (p<0.001) higher annual productivity losses ($10,316 vs. $5,459 per employed person) and annual all-cause healthcare costs ($22,818 vs. $15,362 per person) compared to HCV-uninfected individuals. [41] Evaluating the trade-off between the benefits and costs of these new agents will be critical to scaling up HCV treatment [35].......
Khoury et al.- Table 1 shows that the demographic characteristics of treatment-naőve HCV patients differed in a variety of ways from unmatched non-
HCV controls. HCV patients versus non-HCV subjects were older (53 vs. 48 years old, P\0.001), more likely to be male (64 vs. 48 %, P\0.001), and less likely to be heterosexual (86 vs. 91 %, P\0.01) or to live with a partner (46 vs. 60 %, P<0.001). HCV infected patients were also less likely to have graduated from high school (95 vs. 97 %, P\0.05), to be employed (40 vs. 55 %, P\0.001), or to have health insurance (73 vs. 83 %, P<0.001) than non-HCV subjects in the NHWS, and tended to have lower household income. They also had poorer health habits, being less likely to be normal weight (23 vs. 31 %, P\0.01) and more likely to be obese (37 vs. 33 %, P<0.05), smoke cigarettes (44 vs. 19 %, P<0.001), and less likely to exercise (57 vs. 65 %, P<0.01). They were less likely to drink alcohol (56 vs. 65 %, P<0.001), although more than half reported doing so. They also suffered from more non-liver co-morbid health conditions (0.78 vs. 0.37, P<0.01). As expected, they were also much more likely to suffer from cirrhosis (3.9 vs. 0.1 %, P<0.001) or liver cancer (0.7 vs. 0.0 %, P<0.001).
"The employed HCV group (n = 121) reported an average of 23 % impairment while at work, approximately 10 percentage points greater than employed controls (n = 141; 13 %, P\0.001). Overall work impairment was also greater than that reported by those without HCV infection (26 vs. 15 %, P\0.001), although untreated HCV infected patients did not report missing more hours of work than matched controls (5.0 vs. 2.8 %, P = 0.09). Activity impairment also was higher among untreated HCV infected patients, with 42 % impairment in non-work activity on average, compared with 27 % among matched controls (P\0.001).....
....Greater use of healthcare resources was also reported among treatment-naive HCVinfected patients compared with matched non-HCV subjects (Table 3). Untreated HCV infected patients went to the ER more often (0.76 vs. 0.54 times per year, P\0.05) and made more annual visits to traditional healthcare providers (12.24 vs. 8.22, P\0.001). There was also a trend for untreated HCV infected patients to have more hospitalizations on average (0.42 vs. 0.25), although this did not reach statistical significance (P = 0.07).
.....Estimated costs are presented in Table 4. These were also significantly higher among the untreated HCV infection group than matched controls. For employed treatment-naőve HCV infected patients, productivity impairments were worth $10,316 per patient per year, compared with $5,469 for matched controls (P\0.001). Indirect costs were primarily because of productivity lost to presenteeism in both groups, which was significantly higher among untreated HCV infected patients ($8,209 vs. $4,424, P\0.001). Annual incremental costs were approximately $400, $3,100, and $3,950 dollars more for ER visits, hospitalizations, and physician visits, respectively, for untreated HCV infected patients than for matched controls. Total direct costs were $22,818 for untreated HCV infected patients and $15,362 for matched controls (P\0.001). The direct costs estimated here do not include outpatient pharmacy costs, which can be substantial for HCV infected patients undergoing treatment. The average total costs were nearly $27,000 per untreated HCV infected patient per year, approximately 150 % of the total costs of the matched controls. This is an incremental cost of $9,017 per patient per year.....
|
|
| |
| |
|
|
|