 |
 |
 |
| |
FIB-4 Predicts Major Liver Complications
and Death in HCV+ People Starting ART
|
| |
| |
20th International AIDS Conference, July 20-25, 2014, Melbourne
Mark Mascolini
FIB-4 index when people with HCV start antiretroviral therapy (ART) and change in FIB-4 with treatment independently predicted a major liver complication or liver-related death in the Italian Icona cohort [1]. The analysis linked a baseline FIB-4 above 3.25 to almost a 15-fold higher incidence of liver complications or death.
FIB-4 is a much-used noninvasive marker of liver fibrosis validated in people with HCV infection [2]. To improve understanding of FIB-4 prognostic value in people starting ART, Cristina Mussini and Icona colleagues conducted this retrospective analysis. The study included all initially antiretroviral-naive Icona participants with an HCV test, a FIB-4 when starting ART, and a follow-up FIB-4. The investigators excluded people positive for hepatitis B surface antigen. They set the following cutoffs for cirrhosis:
-- FIB-4 below 1.45: absence of cirrhosis
-- FIB-4 1.45 to 3.25: undetermined
-- FIB-4 above 3.25: cirrhosis
The investigators considered the date when ART began as the baseline date. Follow-up continued from when ART began until the first major liver complication or liver-related death. Major liver events were variceal or gastrointestinal bleeding, ascites, hepatic encephalopathy, other signs of liver decompensation including hepatic-renal syndrome, and hepatocellular carcinoma. The Icona team used a multivariable Cox regression model to explore associations between FIB-4 and risk of a major liver event or liver death.
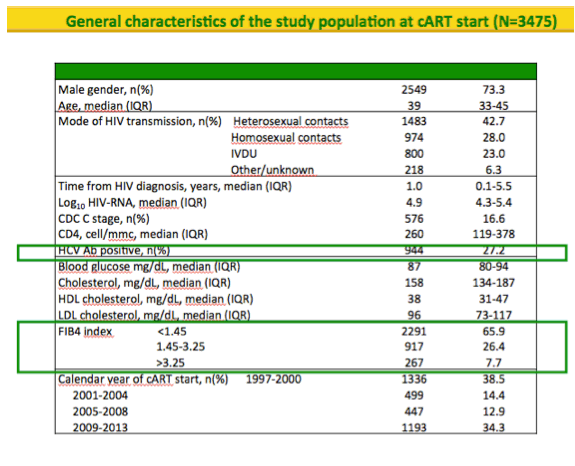
Among 3475 HIV-positive people analyzed, 73% were men and median age stood at 39 years (interquartile range [IQR] 33 to 45). HIV acquisition risks were heterosexual sex in 43%, sex between men in 28%, and injection drug use in 23%. Median time since HIV diagnosis measured only 1 year (IQR 0.1 to 5.5). When ART began, 17% of participants had CDC stage C HIV infection, median CD4 count measured 260 (IQR 119 to 378), and median viral load stood at 4.9 log (about 79,000 copies, IQR 4.3 to 5.4 log).
Of the 3475 cohort members, 944 (27%) were HCV antibody positive. Among 484 people in whom HCV RNA was measured, 446 (92%) were positive, a result indicating active infection.
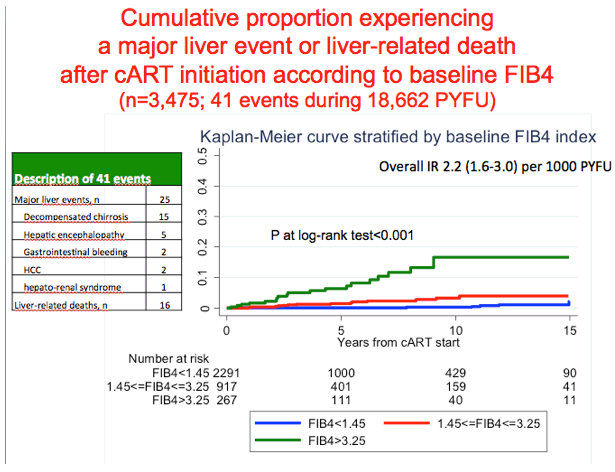
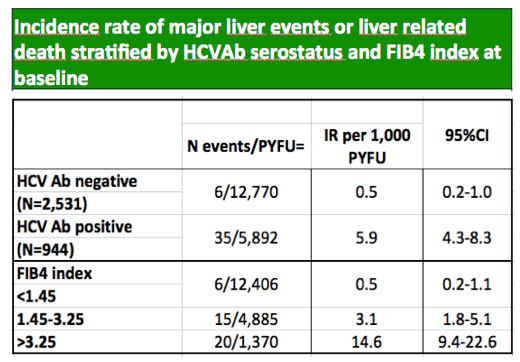
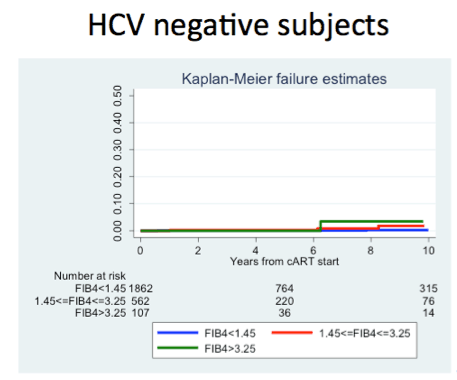
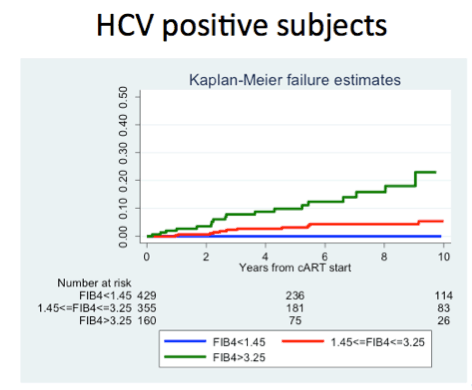
Through 18,662 person-years of follow-up, the investigators counted 41 liver events, including 25 major liver complications and 16 liver-related deaths. Overall liver event incidence measured 2.2 per 1000 person-years, meaning about 2 of every 1000 people had a serious liver problem or liver death every year. Incidence was significantly higher in HCV antibody-positive people (5.9 per 1000, 95% confidence interval [CI] 4.3 to 8.3) than in HCV antibody-negative people (0.5 per 1000, 95% CI 0.2 to 1.0).
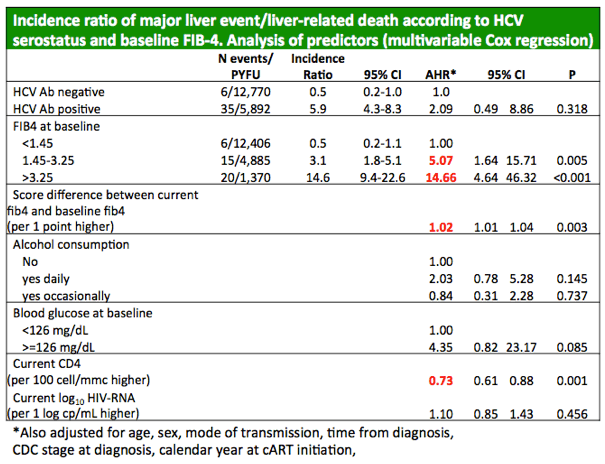
Two thirds of cohort members (65.9%) had a FIB-4 below 1.45, and in them incidence of major liver events was 0.5 per 1000 person-years (95% CI 0.2 to 1.1). One quarter of cohort members (26.4%) had a FIB-4 between 1.45 and 3.25, and in them liver event incidence was 3.1 per 1000 (95% CI 1.8 to 5.1). The remaining cohort members (7.7%) had cirrhosis defined as a FIB-4 above 3.25, and in them liver event incidence measured 14.6 per 1000 (95% CI 9.4 to 22.6).
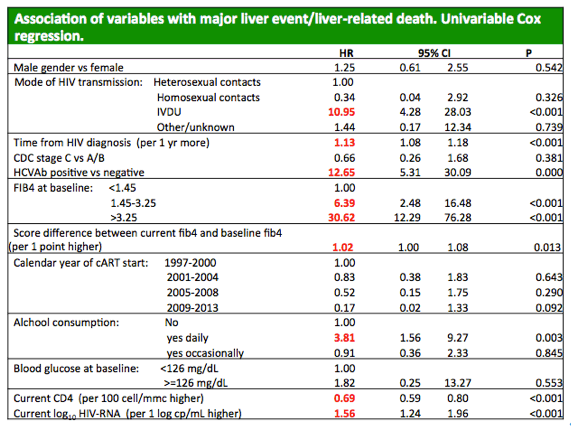
Multivariable analysis adjusted for age, sex, alcohol consumption, and numerous HIV variables identified four independent predictors of a major liver event or liver-related death at the following adjusted hazard ratios (aHR) (and 95% CIs):
-- Baseline FIB-4 1.45 to 3.25 vs below 1.45: aHR 5.07 (1.64 to 15.71, P = 0.005)
-- Baseline FIB-4 above 3.25 vs below 1.45: aHR 14.66 (4.64 to 46.32, P < 0.001)
-- Every point higher current FIB-4 vs baseline: aHR 1.02 (1.01 to 1.04, P = 0.003)
-- Every 100-cell higher current CD4 count: aHR 0.73 (0.61 to 0.88, P = 0.001)
These factors predicted a major liver event independently of HCV infection.
The Icona team concluded that baseline FIB-4 and change in FIB-4 "could be used as surrogate markers of severe clinical events" and as "a simpler marker to prioritize HCV treatments in the HIV-positive population."
References
1. Mussini C, Lorenzini P, De Luca A, et al. Prognostic value of FIB-4 in HIV positive patients of the Icona cohort co-infected or not with HCV. AIDS 2014. 20th International AIDS Conference. July 20-25, 2014. Melbourne. Abstract MOAB0101.
2. Vallet-Pichard A1, Mallet V, Nalpas B, et al. FIB-4: an inexpensive and accurate marker of fibrosis in HCV infection. comparison with liver biopsy and fibrotest. Hepatology. 2007;46:32-36. http://onlinelibrary.wiley.com/doi/10.1002/hep.21669/full
-----------------------------

Program abstract
Background: Liver-related death due to HCV, HBV or metabolic complications remains a main cause of death among patients (pts) with HIV infection. FIB4 is a non-invasive serum fibrosis marker validated in HCV positive pts. Aim of the present study is to evaluate the role of FIB4 at starting cART to predict major liver events or liver-related death.
Methods: Retrospective cohort study including all pts naive for ART with an HCV serology in the Icona Foundation Study. HBsAg positive pts were excluded. We used a FIB4 cut off of 3.25 for cirrhosis, a cut off < 1.5 for the absence of cirrhosis and for a value between 1.5 and 3.25 cirrhosis status was considered as undetermined. cART starting was considered as baseline and patients were follow-up to the date of the first major liver event or liver-related death. Multivariable Cox regression model was used to determine the association of FIB4 with the risk of major liver events or liver-related death.
Results: 3,475 patients were analysed, 73.3% males, median age 39 years (IQR 33-45), heterosexuals 42.7%, MSM 28%, intravenous-drug users 23%. At baseline, 16.6% were in CDC stage C, median CD4 were 260 cells/ul (IQR 119-378), median HIV RNA 4.9 log10/mL (IQR 4.3-5.4). 944 (27.2%) pts were HCVAb+: 446 had HCVRNA+ among 484 pts with available test. Over a follow-up of 18,662 person years there were 41 events (25 major liver events and 16 liver-related deaths), IR=2.2 per 1,000 PYFU (95%CI 1.6-3.0). Incidence rate of major events or liver related death was 0.5
(95%CI 0.2-1.0) in HCV Ab- subjects and 5.9 (95%CI 4.3-8.3) in HCV Ab+. IR for subjects with baseline
FIB4< 1.45 (65.9%) was 0.5 (95%CI 0.2-1.1), FIB4=1.45-3.25 (26.4%) IR=3.1 (95%CI 1.8-5.1), FIB4>3.25 (7.7%) IR=14.6 (95%CI 9.4-22.6). At multivariable analysis only FIB4 at baseline, current progression of fibrosis expressed as difference between current and baseline FIB4 and current CD4 were independently associated with the risk of developing a major liver event or liver-related death.
Conclusions: Our study shows that FIB4 at baseline and its modification detected after cART initiation are risk factors for major liver events or liver-associated death independently of infection with HCV.


|
| |
|
 |
 |
|
|