 |
 |
 |
| |
Effect of viral suppression below 20 copies of HIV-RNA /mL of
plasma on virological outcome of treated HIV- infected patients
|
| |
| |
Reported by Jules Levin
20th International AIDS Conference, July 20-25, 2014, Melbourne
Ramon Teira and the VACH Study Group
From the authors slides follow below:
BACKGROUND
Beyond the unquestionable causality of HIV in HIV disease and AIDS, in the late nineties the strong association between plasma concentrations of HIV-RNA (commonly referred to as VL) and the prognosis of untreated HIV infection was demonstrated. Furthermore, the validity of the inability to detect HIV-RNA in plasma , as a surrogate marker of the beneficial effects of ART was also shown.
There is little need to remind here the validity of measuring plasma concentration of HIV-RNA (commonly referred to as VL) as a surrogate marker for both estimating the prognosis of untreated HIV infection and the beneficial effects of antiretroviral treatment
But for the purpose of this presentation, it can be reminded that the landmark validation studies were performed with earlier generation assays with a lower limit of detection of 200 to 400 hundred copies per mL; while a majority of clinical trials and cohort studies that generated the prevailing body of evidence in this subject were performed in the first decade of this century using assays with a lower limit of detection of 50 copies per mL.
In early two thousand and nine, the leading manufacturers of HIV VL assays released their new tests with a dynamic range expanding down to detect as low as 20 copies per mL. Necessarily and immediately after this happened, we started to see in clinical practice patients with VL in the range between 20 and 50, to whom an informed judgement on prognosis and treatment recommendation could not be guaranteed. We decided to investigated the prognostic implications of the detection of VLoLV in treated HIV infected patients in the Spanish VACH Cohort
METHODS
The VACH Cohort is an open cohort of HIV-infected adults that was constituted in Spain in 1997, by the association of 16 (currently, 26) hospital-based HIV clinics. Patients are included in the cohort provided they are older than 18 and that they give their informed consent. The Cohort and our studies abide by the Spanish laws and regulations regarding confidentiality, patient autonomy, data protection and medical investigation.
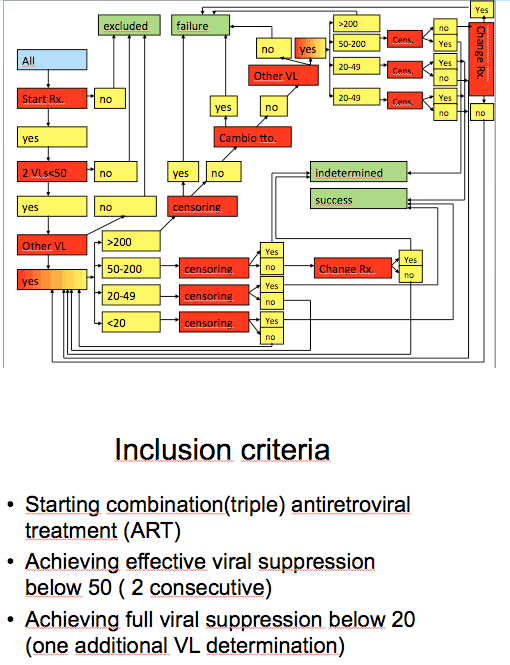
This graph displays the main selection and outcome criteria used for this study. In brief: of all patients who started ART, we selected those who ever achieved confirmed viral suppression below 50, and who had an additional VL determination below 20. Henceforward patients would be classified as treatment success if no failure occurred and VL at administrative censoring remained below 50; treatment failure if an episode of viremia over 200 was followed by a second one, a treatment change or administrative censoring or loss to follow-up; or indeterminate result if no failure or success was applicable.
Patients were further classified in one of four exclusive groups: 1) persistently suppressed below 20 if all VL determinations remained so; 2) experiencing
VLoLV, if any posterior VL determination was between 20 and 50, but never above this value; 3) experiencing LoLV if any posterior VL determination was between 50 and 200, but never above this value; and 4) experiencing HL blip if any posterior VL determination was higher that 200, but did not define VF.
We constructed Kaplan-Meier curves of time until VF according to the groups defined above, with a main objective of the study focused in the comparison between patients remaining fully suppressed and those experiencing VLoLV twenty-to-fifty. We investigated the possible association between VF and other variables commonly studied in this setting (age, sex, risk group for the transmission of HIV, race or ethnicity, baseline VL, representative CD4 cell count, calendar period and time of effective viral suppersion). We included those which appeared associated with VF in the bivariate analyses in Cox regression models to estimate their independent effect with a particular interest in any controlled association between VLoLV and VF.
RESULTS
Out of a total of twenty one thousands four hundreds and eighty (21480) patients who started cART after January 1st 1997, thirteen thousands six hundreds and seventy one (13671) (63.7%) ever achieved effective suppression below 50. Six thousand eight hundreds and thirty four (6834)(50%) progressed to full suppression (below 20) at any time point, but only four thousands two hundreds and eighty nine (4289) did so after June 2009 when the Roche Taqman Cobas test became commercially available, and these constitute the population of our study.
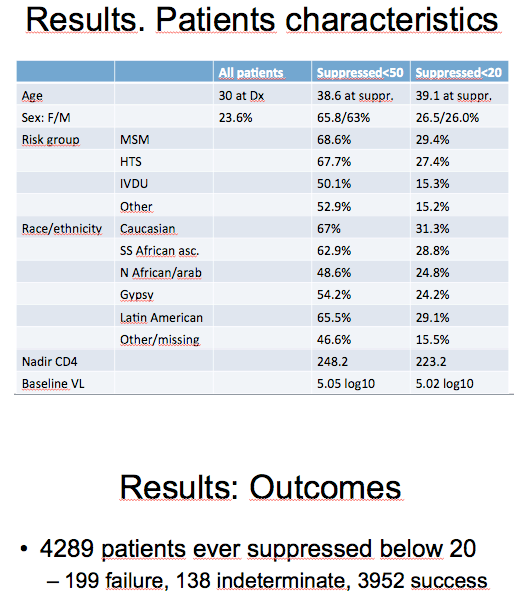
This slide summarizes the main epidemiological characteristics of the different study populations. As you can see, a slightly higher, but statistically significant, proportion of women than of men achieved ES below 50 (3330/5063, 65.8 % vs. 10341/16411, 63.0 %; p<0.000). However, the proportion fully suppressed was similar in both genders (1057, 26.5 % vs. 3232, 26.0 %, p=0.47). Differences were also observed in the age at effective suppression, in the distribution by mechanism of HIV transmission and by racial or ethnic origin, in the nadir CD4 cell count and baseline viral load.
Median age was 39.1 (33.4-45.1) for fully suppressed patients and 38.6 (33.1-44.7) for the remaining group at time of reaching effective suppression. Median age at HIV diagnosis was lower for patients who did not reach such endpoint (30, IQR 20-37 vs 32, IQR 22-38)
A higher proportion of patients who declared a probable acquisition of HIV through sexual contact achieved full suppression (1398/4520, 29.4 % for men who had sex (MSM) with men; 1538/5604, 27.4 % for heterosexual contacts; 1071/6983, 15.3 % for those who had shared needles (IVDU); and 352/2316, 15.2 % for those with unknown or undeclared mechanism of transmission; p<0.000). Similar results were observed regarding the proportions of patients reaching effective suppression as you can see in the slide (3099/4520: 68.6% for MSM; 3792/5604: 67.7% for HTS; 3501/6983: 50.1% for IVDU; and 1225/2316: 52.9% for others)
Differences were also observed in the proportion of patients ever fully suppressed below 20 according to its racial/ethnic classification: 3991/12765 (31.3 % for Caucasians; 232/805, 28.8 % for black; 240/826, 29.1 % for Central and South Americans; 38/153, 24.8 % for North Africans and Arabs; 109/451, 24.2 % for gypsies; and 1004/6480, 15.5 % for others or those with this datum missing (p<0.000). As for effective suppression below 50 the respective percentages were 67.0%, 62.9%, 65.5%, 48.6, 54.2% and 46.6%)
The mean nadir CD4+ cell count was lower for patients achieving full suppression (223.2 vs 248.2 difference: 25.2, 95% CI: 18.9 to 31.4), but the mean count at the time of effective suppression was very slightly higher (443.8 vs 434.5; difference: -9.2; 95% CI: -18.4 to -0.5).
OUTCOMES
After full suppression, those 4289 patients were followed-up for a median of 639 days, to a total of eight thousands and sixty nine (8069) patient-years. In this period, 199 patients were classified as treatment-failure, 138 as indeterminate outcome and three thousands nine hundreds and fifty two (3952) as treatment-success.
Regarding the main objective of the study, two thousands six hundred and twenty three (2623) patients remained fully suppressed during four thousands one hundred and ninety four (4194) patient-years, while 1668 had one or more viremic episodes over 20 copies/mL (excluding VF) during three thousands nine hundred and thirty (3930) patient-years. In 824 of the latter, viremia remained always below 50 copies/mL: in 550 cases just one blip was recorded, in 177 between 2 and 3 blips, in 69 cases there were 4 or 5 blips and in 28 cases 6 or more blips occurred (during one thousand nine hundreds and sixteen (1916.4) patient-years for the whole group and 1174 p-y, 459 p-y, 197 p-y and 87.7 p-y respectively for the subgroups). In 563 at least one episode of viremia between 50 and 200 occurred. And in 278 viremia over 200 was recorded independent of VF.
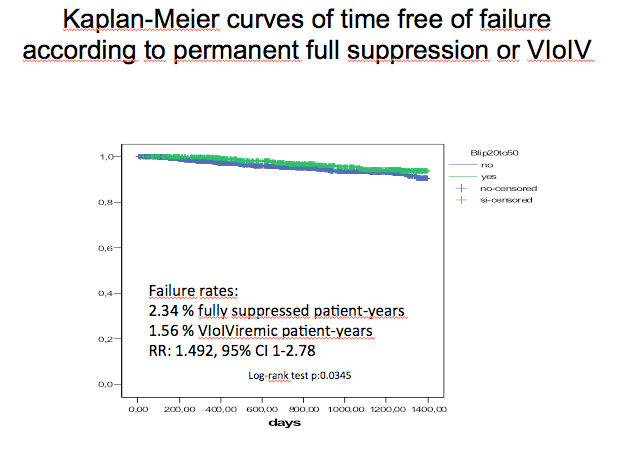
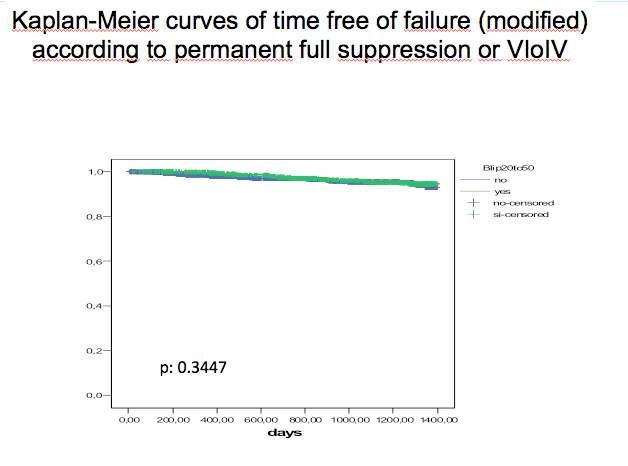
VF, as defined in our protocol, occurred in 98 cases of persistently fully suppressed patients for an incidence rate of 2.34 cases per 100 patient-years of follow-up (95%CI: 1.91-2.83) ; and in 30 case of patients who suffered any blip between 20 and 50 for an incidence rate of 1.56 cases per 100 patient-years (95%CI: 1.08-2.21) (incidence rate ratio: 1.492, 95% CI: 1-2.78): 18 events in patients with just one blip, 10 events in patients with 2-3 blips, 2 events in patients with 4-5 blips and zero events in 28 patients with more than 5 blips (incidence rates for subgroup of semi-categorical number of blips: 1.54, 2.17, 1.01 and 0) . (You can see) the Kaplan-Meier curves of time to VF this small but significant difference favouring the group of patients who had a VLoL blip after becoming fully suppressed. Other variables that were associated with VF in bivariate analyses were nadir CD4 count, baseline VL, transmission risk group, race/ethnicity and time on effective suppression below 50 before full suppression below 20 (age and sex were not). We performed Cox models to adjust for differences in these variables. The difference favouring VLoLV as compared with persistent full suppression persisted in these models (in the final model, nadir CD4 cell count, and time on effective suppression remained associated with VF, but not risk).
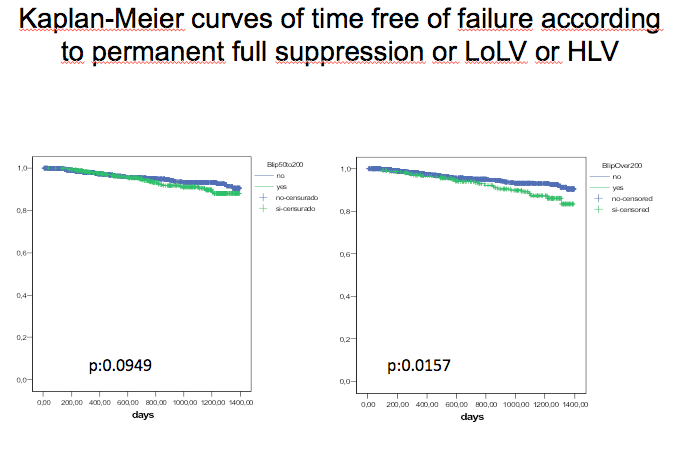
In the opposite direction, we found a trend towards an increased risk of VF in patients experiencing low level viremic episodes (50 to 200) as compared with persistently fully suppressed, as you can see in this Kaplan-Meier curves, where the upper line corresponds to these patients and the lower one, to ever lower viremic. As for patients with transient higher than 200 viremic episodes, the incidence of VF was significantly higher than that of the remaining patients, as can be seen in the graph on the right hand side of the slide.
We reviewed one-by one every episode of VF and of indeterminate result to confirm that they were correctly classified and check if there was any particular pattern to explain our finding discordant with those of other studies on the subject. Indeed we found a unbalanced incidence of cases of double high-level viremia (therefore defining VF) followed by return to full suppression, higher in the group of patients previously fully suppressed; and a higher number of patients who suffered VF after switching to PI monotherapy, who regained full suppression after returning to their previous combination regimen. When these cases are classified as treatment success, the risk of VF of the group of persistently fully suppressed below 20 patients is not different from that of the group with VLoLV.
CONCLUSIONS
In the population of HIV-infected patients on ART who achieve full viral suppression below 20 cop/mL, those who experience subsequent episodes of VLoLV (between 20 and 50 cop/mL), the risk of VF (as defined in our protocol) is not higher than that of patients who remain fully suppressed.
In this conditions, nadir CD4 cell count (inversely), some categories of HIV-transmision risk-groups and time effectively suppressed (below 50) prior to full suppression (inversely) were associated with VF.
The selection criteria, and variable definitions used in this study, and probably in most if not all epidemiological and even experimental, probably have as deep an impact in the results as the biological factors themselves.
Thank you for your attention
------------------------------------








|
| |
|
 |
 |
|
|