 |
 |
 |
| |
Inflammatory Cytokine/IL-10 Ratios Tied to Regional Brain Atrophy With HIV
|
| |
| |
20th International AIDS Conference, July 20-25, 2014, Melbourne
Mark Mascolini
High ratios of several inflammatory cytokines to IL-10 (an antiinflammatory) correlated with regional brain atrophy in a study of 52 antiretroviral-treated adults with well-controlled HIV replication [1]. High ratios indicate high levels of inflammatory cytokines and low levels of inflammation-quelling IL-10.
HIV-associated neurocognitive disorder (HAND) remains prevalent even in populations with HIV replication well controlled by antiretroviral therapy [2,3]. University of Hawaii researchers who conducted the cytokine study noted that inflammatory cytokines can disrupt the blood-brain barrier, let HIV enter the brain, and contribute to development of HAND. They observed that certain inflammatory cytokines (such as IL-6, IL-8, and TNF-alpha) remain elevated despite suppression of HIV in the peripheral circulation.
IL-10, the Hawaii team added, inhibits monocyte synthesis of proinflammatory cytokines and helps regulate immunologic and inflammatory responses. Thus they hypothesized that "the balance between proinflammatory mediators and antiinflammatory IL-10 may be important in neurological disease." They cited previous research linking (1) a high IL-1beta/IL-10 ratio and dementia in probable Alzheimer's disease, (2) a high IL-6/IL-10 ratio and major depression, and (3) a high TNF-alpha/IL-10 ratio and HIV disease progression.
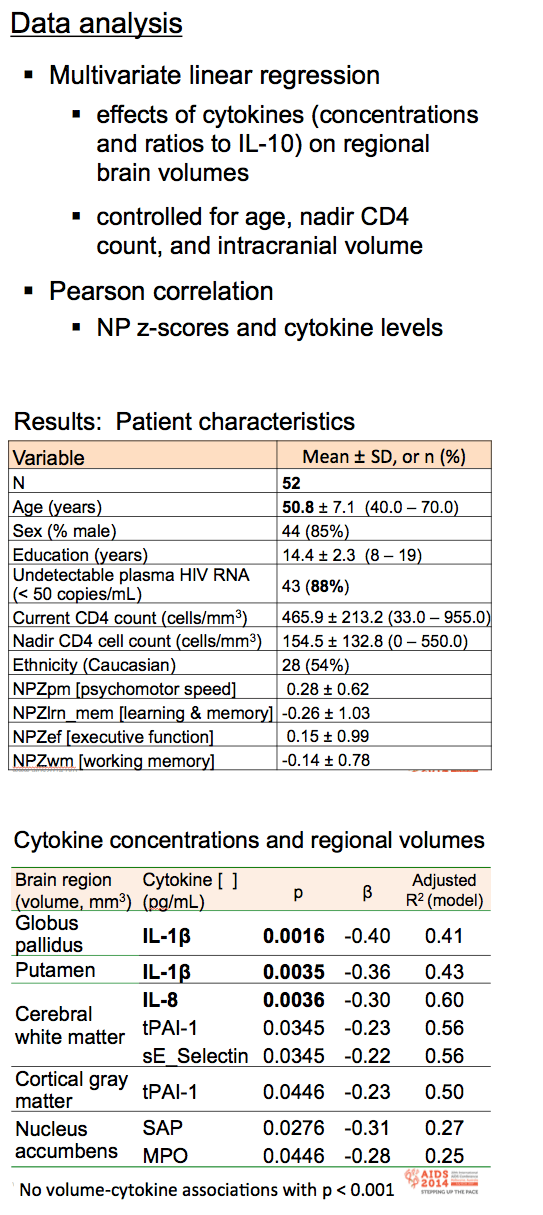
To analyze cytokine levels, cytokine/IL-10 ratios, and their relationships to brain region volumes and neuropsychological test performance in people with chronic, suppressed HIV infection, these researchers focused on a subset of adults enrolled in the HIV Aging With HIV-Cardiovascular Disease study who had magnetic resonance brain imaging, cytokine levels measured by multiplex Luminex assay, and neuropsychological testing. The investigators converted individual neuropsychological test scores to z-scores using normative data adjusted for age, gender, and education then computed composite scores: a global score (NPZ14), psychomotor speed (NPZpm), learning and memory (NVZlrn_mem), executive functioning (NPZef), and working memory (NPZwm).
All participants were at least 40 years old and taking a stable antiretroviral regimen for more than 6 months. Age averaged 50.8 years, 44 participants (85%) were men, 28 (54%) were white, and 43 had an undetectable viral load. Current CD4 count averaged 466.
Most absolute cytokine concentrations did not relate to regional brain volumes, though correlations were significant at P < 0.01 for IL-1beta and the globus pallidus (beta -0.40, P = 0.0016) and the putamen (beta -0.36, P = 0.0035) and for IL-8 and cerebral white matter (beta -0.30, P = 0.0036).
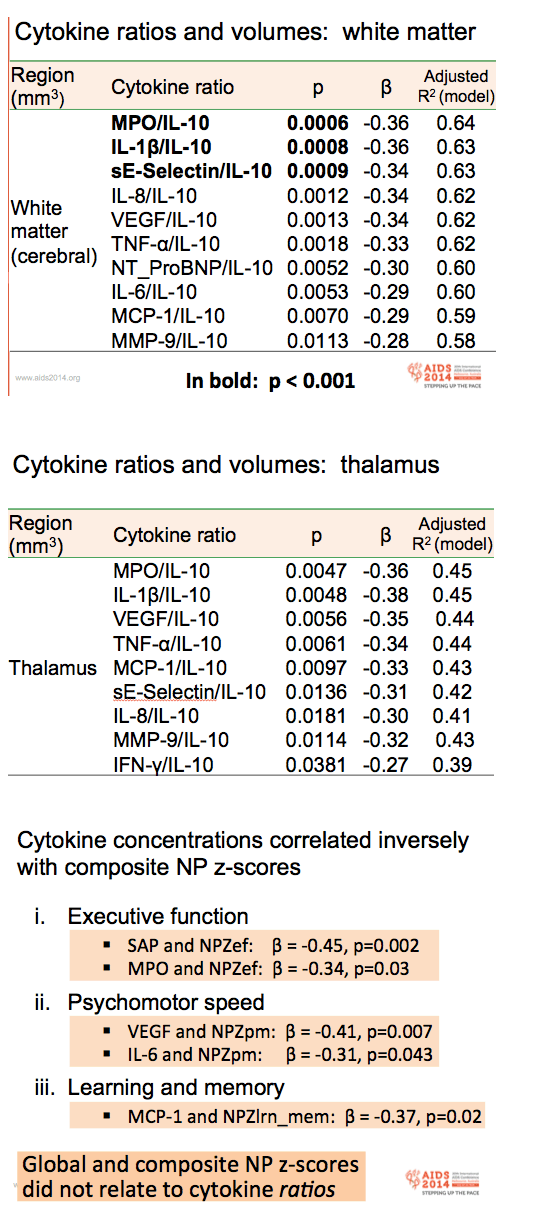
Three cytokine/IL-10 ratios correlated with decreased white matter at P < 0.001: myeloperoxidase/IL-10 (beta -0.36, P = 0.0006), IL-1beta/IL10 (beta -0.36, P = 0.0008), and sE-selectin/IL-10 (beta -0.34, P = 0.0009). Several cytokine/IL-10 ratios correlated with lower thalamus volume: myeloperoxidase/IL-10, IL-1beta/IL-10, VEGF/IL-10, TNF-alpha/IL-10, MCP-1/IL-10, sE-selectin/IL-10, IL-8/IL-10, MMP-9/IL-10, and IFN-gamma/IL-10 The first five associations were significant at P < 0.01.
Certain cytokine concentrations (not ratios) correlated inversely with composite NPz scores for (1) executive function (serum amyloid P: beta -0.45, P = 0.002; and myeloperoxidase: beta -0.34, P = 0.03), (2) psychomotor speed (VEGF: beta -0.41, P = 0.007; and IL-6: beta -0.31, P = 0.043), and (3) learning and memory (MCP-1: beta -0.37, P = 0.02).
The University of Hawaii team concluded that proinflammatory cytokine levels relative to IL-10 are independently associated with decreased white matter and thalamus volume and that these associations were more significant than for absolute cytokine concentrations. They cautioned that their analysis is limited by its cross-sectional nature, lack of HIV-negative controls, and relatively small number of participants.
The researchers proposed that "an inflammatory environment characterized by inadequate IL-10 response to elevated proinflammatory cytokines may be a key factor in HIV neuropathogenesis and persistence of HAND."
References
1. Kallianpur K, Sakoda M, Umaki T, et al. High ratios of circulating pro-inflammatory cytokines to anti-inflammatory IL-10 correlate with regional brain atrophy in chronic suppressed HIV infection. AIDS 2014. 20th International AIDS Conference. July 20-25, 2014. Melbourne. Abstract THAB0104.
2. Chan P, Brew BJ. HIV associated neurocognitive disorders in the modern antiviral treatment era: prevalence, characteristics, biomarkers, and effects of treatment. Curr HIV/AIDS Rep. 2014 Jun 27. Epub ahead of print.
3. Heaton RK, Clifford DB, Franklin DR Jr, et al. HIV-associated neurocognitive disorders persist in the era of potent antiretroviral therapy: CHARTER Study. Neurology. 2010;75:2087-2096.
----------------------------






|
| |
|
 |
 |
|
|