 |
 |
 |
| |
Why Undiagnosed HIV and HIV Incidence Are Falling in SF MSM and Static in London MSM
|
| |
| |
20th International AIDS Conference, July 20-25, 2014, Melbourne
Mark Mascolini
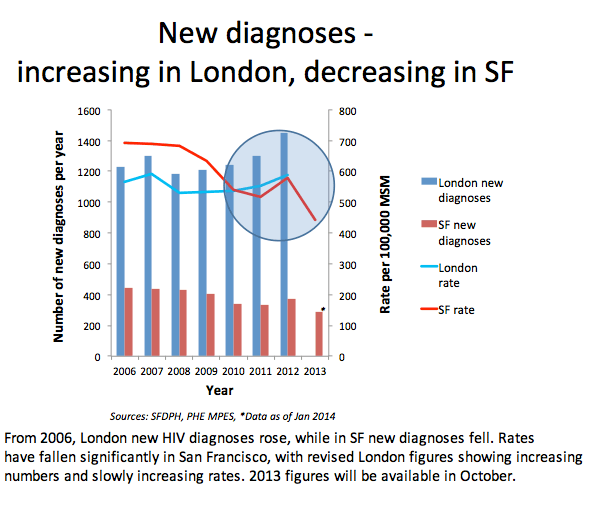
Higher HIV testing rates and safer sex may explain why HIV incidence is falling among San Francisco men who have sex with men (MSM) but rising in London MSM, and why undiagnosed HIV rates are dropping in San Francisco but not in London [1]. Results of this extensive data analysis suggest that HIV testing, awareness, and condom use trump linkage to care and retention in care in HIV prevention.
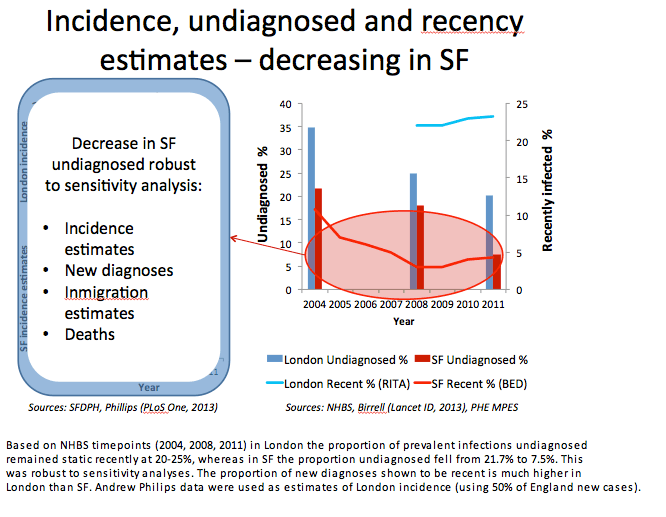
Colin Brown (Public Health England) and colleagues in London in San Francisco observed that HIV infection is endemic in San Francisco (24% of 64,000 MSM) and London (9% of 234,000 MSM) and that similar numbers of MSM have an HIV diagnosis (13,000 and 14,000). But MSM epidemics in the two gay meccas differ in important ways: Estimated undiagnosed HIV infections are down in San Francisco since 2006 (from 21.7% to 7.5%) but static in London (around 20% to 25%). And HIV incidence (the new-infection rate) has dwindled from 694 to 442 per 100,000 men in San Francisco while climbing in London from 563 to 696 per 100,000.
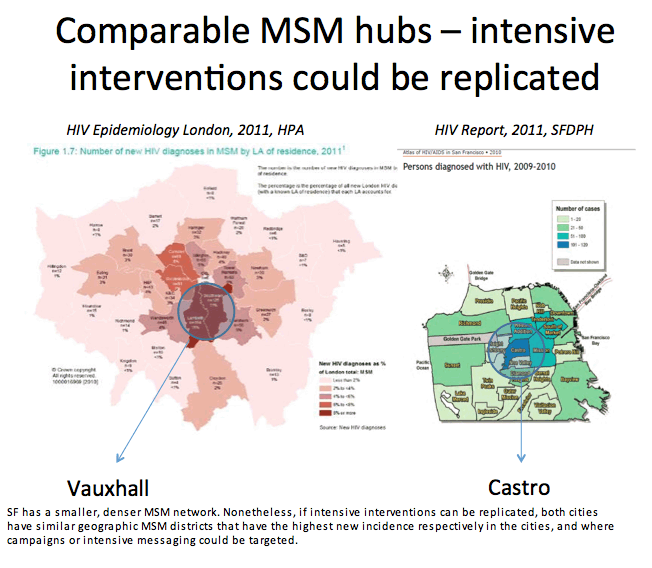
To determine what accounts for these differences, Brown and coworkers conducted an extensive review of surveillance and behavioral data since 2004 in both cities, focusing on risk behavior, HIV testing rates, and treatment coverage and response. San Francisco has a smaller, denser MSM network than London, the researchers noted, but strategies aimed at factors distinguishing the two epidemics could be targeted to well-identified MSM districts in both cities.
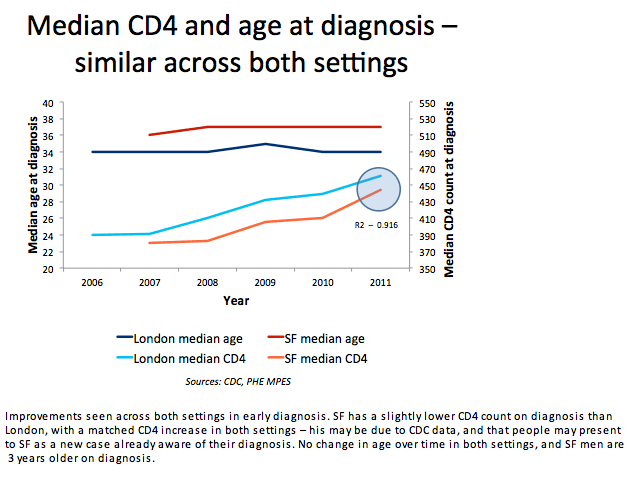
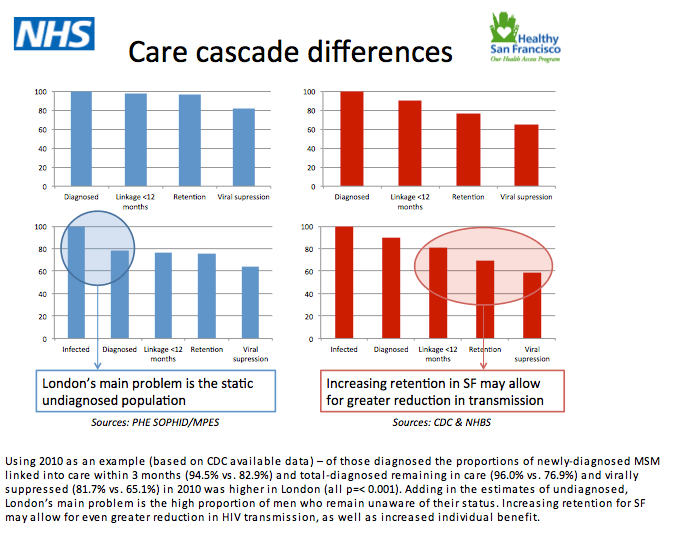
Data from public health authorities in the US and the UK indicate that MSM in San Francisco and London get diagnosed with HIV at a similar median age (later 30s) and with a similar CD4 count (mid-high 400s). Numbers from 2010 indicate London holds the edge over San Francisco in the HIV care cascade, including proportion of newly diagnosed men linked to care in 3 months (94.5% versus 82.9%), proportion remaining in care (96.0% versus 76.9%), and proportion virally suppressed (81.7% vs. 65.1%) (P < 0.001 for all comparisons).
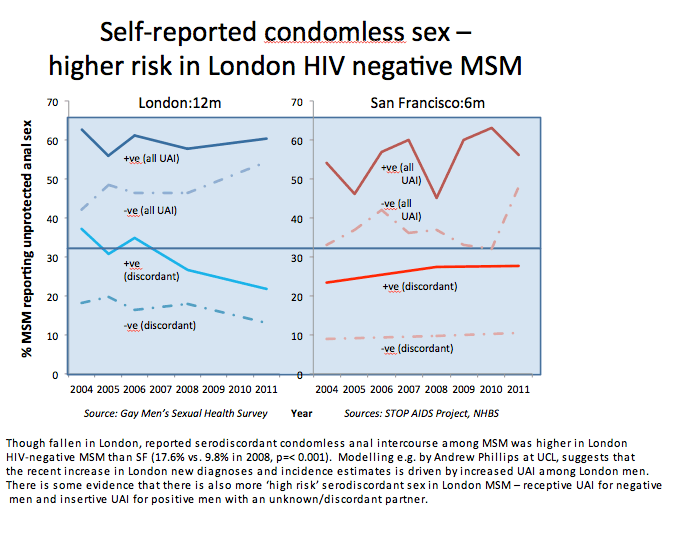
But San Francisco has certain advantages over London on the HIV-prevention front. Data from 2004 through 2011 show that San Francisco MSM get tested for HIV more often than their London counterparts. Higher proportions of San Francisco MSM were ever tested or tested in the past year, and higher proportions of HIV-negative San Franciscans than Londoners got tested in 2009, 2010, and 2011. MSM in San Francisco apparently take fewer sexual risks, with rates of HIV-discordant condom-free anal sex significantly lower in San Francisco than London in 2008 (9.8% versus 17.6%, P < 0.001). Other analyses show higher rates of condomless receptive anal intercourse in HIV-negative London men and condomless insertive anal intercourse with HIV-negative partners by HIV-positive London men.
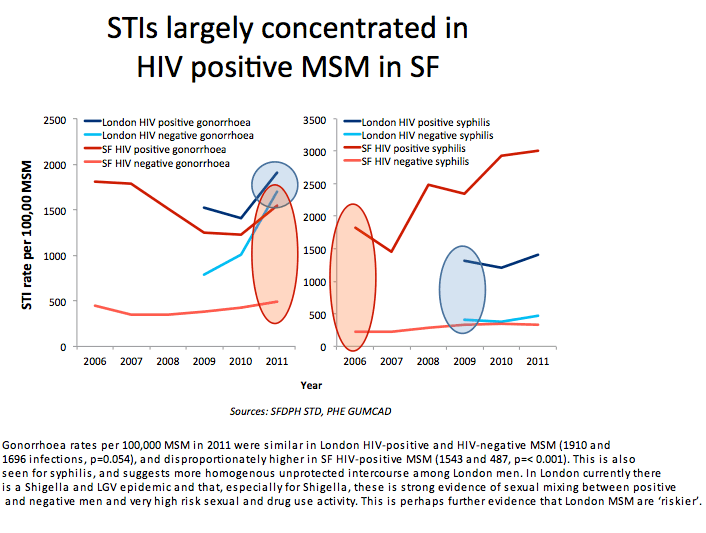
Rates of gonorrhea and syphilis per 100,000 MSM are similar in HIV-positive and negative London MSM (1910 and 1696). But in San Francisco those rates are much higher in HIV-positive than negative men (1543 versus 487). That difference, the researchers surmised, could reflect more sexual mixing between positive and negative men in London than in San Francisco.
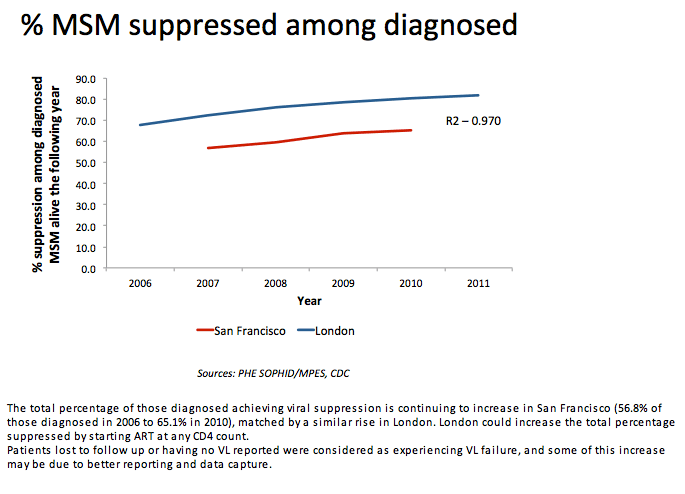
The researchers concluded that the reduced proportion of undiagnosed HIV and lower HIV incidence in San Francisco MSM--compared with static or rising rates in London MSM--may reflect (1) higher HIV testing rates and possibly retesting rates among HIV-negative San Francisco MSM than negative London men, (2) safer sex in San Francisco, including more condom use and greater HIV status disclosure, and (3) a "culture of positive openness" in San Francisco. These findings suggested to Brown and colleagues that HIV testing and safer sex may mean more for prevention than the better referral and retention in care seen in London.
The researchers acknowledged that other factors, like immigration of HIV-positive men from outside the UK to London, may contribute to the static epidemic there. They also stressed that "the safety myth of negative-negative serosorting should be challenged" because negative men may not know their HIV status.
Reference
1. Brown CS, Das M, Hsu L, et al. A divergent tale of two cities: why has HIV control in men who have sex with men (MSM) differed between London and San Francisco (SF) since 2006? AIDS 2014. 20th International AIDS Conference. July 20-25, 2014. Melbourne. Abstract THAC0205LB.
-------------------------






|
| |
|
 |
 |
|
|