 |
 |
 |
| |
Allogeneic bone marrow transplantation in two HIV-1 infected patients shows no detectable HIV-1 RNA or DNA, and a profound reduction in HIV-1 antibodies
|
| |
| |
......and absent CD4+ T cell responses to HIV-1 antigen. We also found a profound reduction in HIV-1 Ab detectability in both patients by WB
Reported by Jules Levin
20th International AIDS Conference, 20-25 July, 2014, Melbourne, Australia
Kersten K Koelsch1,2, William Hey-Cunningham1, Sarah C Sasson2, Chester Pearson1, Katherine H Marks2, Yin Xu1, Michelle Bailey1, Bonnie M Hiener3, Sarah Palmer3,4, John Zaunders1, Jeffrey J Post5,6,8, Samuel T Milliken2,7, Anthony D Kelleher1,2, David A Cooper1,2
1The Kirby Institute, UNSW Medicine, UNSW Australia, Sydney, Australia, 2St Vincent's Hospital, Sydney, Darlinghurst, NSW, Australia, 3Westmead Millennium Institute, Westmead, NSW, Australia, 4 University of Sydney, Sydney, NSW, Australia, 5 Prince of Wales Hospital, Randwick, NSW, Australia, 6 The
Albion Centre, Surry Hills, NSW, Australia, 7 The Kinghorn Cancer Centre, Darlinghurst, NSW, Australia, 8 Prince of Wales Clinical School, UNSW Medicine, UNSW Australia, Sydney, Australia
IAC: No Detectable HIV RNA or DNA in 2 Bone Marrow Transplant Patients Still on ART - Mark Mascolini - (07/25/14).......Two HIV-positive Australian men who had allogeneic hematopoietic stem-cell transplantation (HSCT) with reduced-intensity conditioning (RIC) for hematologic malignancies and continue antiretroviral therapy (ART) have no HIV RNA or DNA detectable by highly sensitive assays [1]. Fourth-generation chemiluminescence microparticle immunoassay (CMIA) can detect only low levels of HIV antigen and antibody in the two men.

----------------------
Program Abstract
Background: Allogeneic bone marrow transplantation (BMT) can have significant effects on viral reservoirs in HIV-1 infected individuals, and in one case led to an apparent sterilising cure.
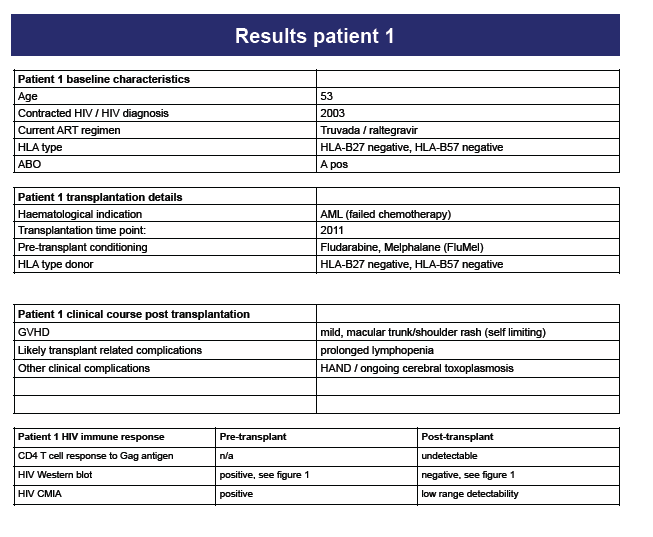
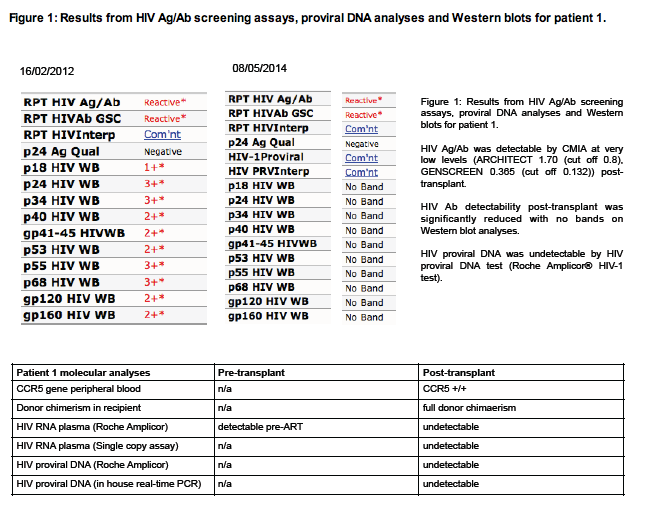
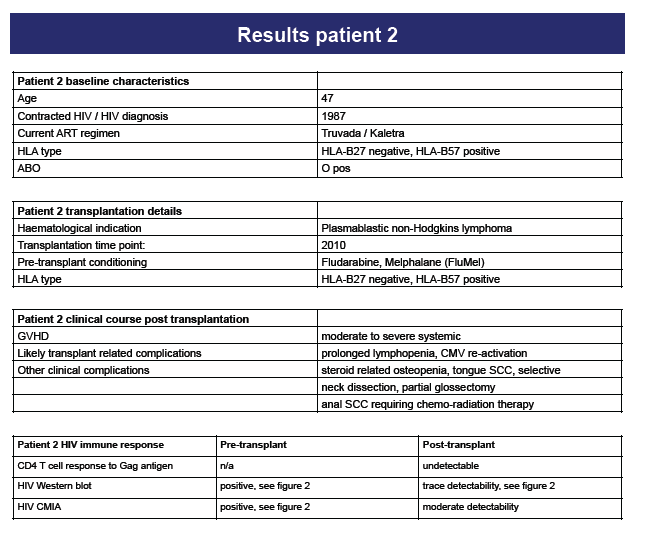
Methods: We studied two HIV-1 infected patients who had undergone allogeneic BMT with reduced intensity conditioning (RIC) for haematologic malignancies. HIV-1 antigens and antibodies (Ag/Ab) were measured by 4th generation chemiluminescence microparticle immunoassay (CMIA) and by Western blot (WB). HIV-1 specific CD4+ T cell responses were measured by CD25/CD134 upregulation. HIV-1 RNA levels in plasma were measured by two separate real-time PCR assays with 20 as well as single copy/ml sensitivity; HIV-1 DNA levels were assessed in peripheral blood mononuclear cells (PBMCs) as well as in isolated CD4+ T cells by PCR using three different primer sets. Both patients were tested for the presence of the CCR5∼32 mutation by PCR.
Results: Two subjects (A and B) received HLA matched, allogeneic stem cell transplants in 2010 (A) and 2011 (B) for non-Hodgkin''s lymphoma and acute myeloid leukaemia respectively. Both patients remained on antiretroviral therapy during and following the procedure. Post-transplant, subject A experienced systemic grade 2 graft versus host disease (GVHD), whereas subject B developed only mild, skin related GVHD. Patient A was heterozygous for the CCR5∼32 mutation post- transplant, patient B was CCR5 wildtype. Following BMT, both patients had no detectable HIV-1 RNA in plasma by either real-time PCR assay, and no detectable HIV-1 DNA by PCR in PBMCs or CD4+ T cells. CD4+ T cell responses to HIV-1 antigen were absent in both patients. Ag/Abs to HIV-1 were detectable by CMIA and WB in both patients prior to BMT. Post-transplant, both patients had low level detectable Ag/Abs on CMIA, but by WB there was only trace antibody detectability in patient A and absent antibodies in patient B.
Conclusions: Assessment of the HIV-1 reservoir size in these two patients after allogeneic BMT with RIC shows undetectable HIV-1 RNA and DNA in peripheral blood and absent CD4+ T cell responses to HIV-1 antigen. We also found a profound reduction in HIV-1 Ab detectability in both patients by WB.
---------------------------


|
| |
|
 |
 |
|
|