 |
 |
 |
| |
Improvement of kidney function after anti
HCV therapy in hepatitis C/HIV coinfection
|
| |
| |
Reported by Jules Levin
20th International AIDS Conference, July 20-25, 2014, Melbourne
S. Banon, J.L. Casado, I. Rios, V. Diaz, C. Quereda, A. Moreno
Ramon y Cajal Hospital, Dept of Infectious Diseases, Madrid, Spain

-------------------------
Program abstract
Background: Chronic hepatitis C virus infection (CHC) is associated with kidney function decline. Virological response to anti-HCV therapy improves kidney function in patients with CHC, but there are no data in HCV/HIV coinfected patients, considering the use of other nephrotoxic drugs and the degree of liver fibrosis.
Methods: Prospective study of 125 patients with HCV/HIV coinfection who received therapy against HCV with pegylated interferon plus ribavirin. Serum creatinine, glomerular filtration rate (GFR, CKD-epi equation), CD4+ count, and HIV RNA level, before and after HCV therapy, were compared.
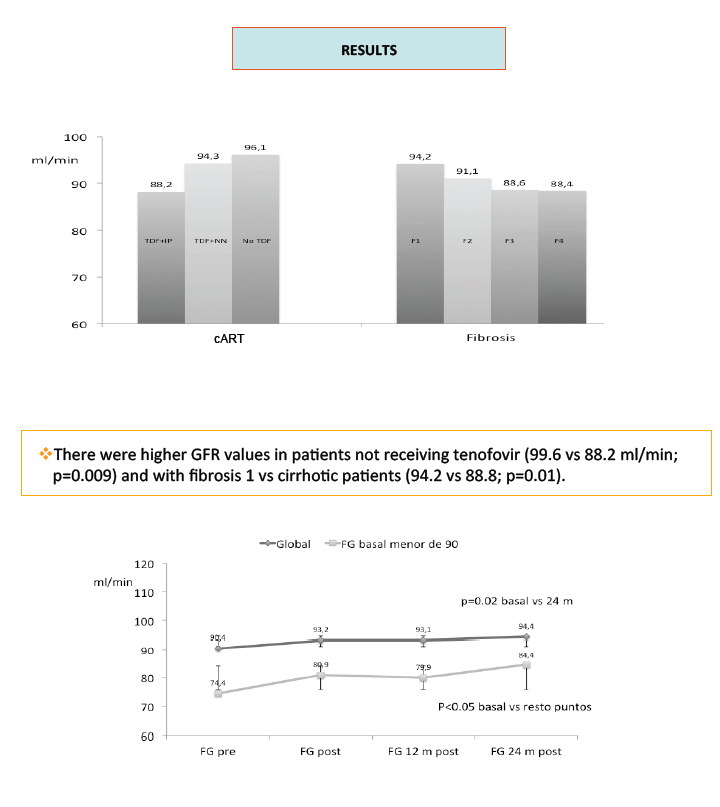
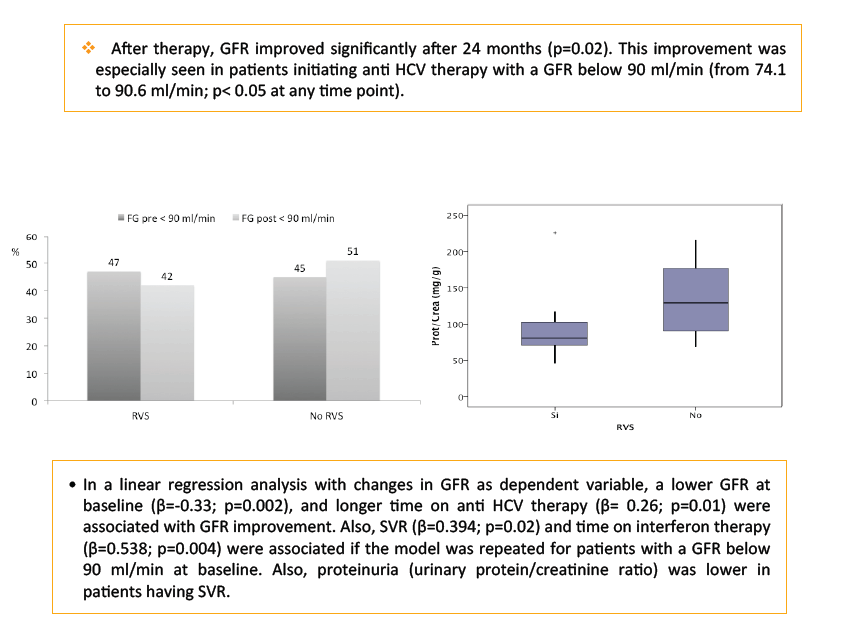
Results: Mean age was 44.3 years (IQR, 25-75), 80% male, and 108 (86%) former IDUs. Prior to HCV therapy, 113 received cART, 54 (48%) including tenofovir plus protease inhibitor (PI). Median CD4+ count was 432 cells/mm3 and 107 out of 113 had undetectable HIV RNA level (< 50 cop/ml). Median time of HCV was 24 years (21-28), 70% were genotype 1 or 4, RNA-HCV was 6.4 log, and 31% had a fibrosis degree 4. After a median of 325 days on therapy, 60 patients (48%) had sustained virological response (SVR). At baseline, mean serum creatinine was 0.91 mg/dl (0.6-1.45), and GFR was 90.3 ml/min/1.73m2 (45.4-150.4), with 46% of patients below 90 ml/min. There were higher GFR values in patients without tenofovir (99.6 vs 88.2 ml/min; p=0.009) and with fibrosis 1 vs cirrhotic patients (94.2 vs 88.8; p=0.01). After therapy, GFR improved significantly after 24 months (p=0.02). This improvement was especially seen in patients initiating anti HCV therapy with a GFR below 90 ml/min (from 74.1 to 90.6 ml/min; p< 0.05 at any time point). In a linear regression analysis with changes in GFR as dependent variable, a lower GFR at baseline (ß=-0.33; p=0.002), and longer time on anti HCV therapy (ß= 0.26; p=0.01) were associated with GFR improvement. Also, SVR (ß=0.394; p=0.02) and time on interferon therapy (ß=0.538; p=0.004) were associated when the model was repeated for patients with a GFR below 90 ml/min at baseline.
Conclusions: A significant improvement of kidney function parameters could be observed after anti HCV therapy in HCV/HIV coinfected patients, especially in case of lower GFR at baseline and sustained virological response.
-----------------------


|
| |
|
 |
 |
|
|