 |
 |
 |
| |
Presence of Hepatitis C (HCV) Infection in Baby Boomers with
Medicare Is Independently Associated with Mortality and Resource Utilization
|
| |
| |
RReported by Jules Levin
AASLD 2015 Nov 13-17 San Francisco
Mehmet Sayiner2, Mark Wymer2, Pegah Golabi2, Joel S. Ford3,
Indie Srishord2, Zobair M. Younossi2,1; 1Center For Liver Disease,
Department of Medicine, Inova Fairfax Hospital, Falls Church,
VA; 2Betty and Guy Beatty Center for Integrated Research, Inova
Health System, Falls Church, VA; 3Department of Medicine, Inova
Health System, Falls Church, VA
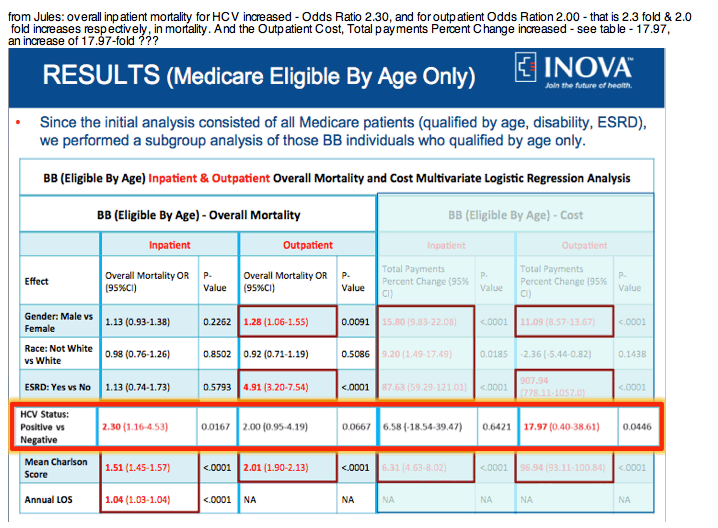
"Baby boomers began aging into Medicare in 2010, 10,000 people/day......In 15 years, 90% of Medicare beneficiaries will be from BB generation....AIM of this study: To evaluate resource utilization and short term mortality of Medicare recipients of BB cohort with HCV......HCV was independently associated with increased overall mortality and resource utilization in both inpatient and outpatient Medicare-BB subjects" [from Jules; my reading of the Tables below mortality in HCV+ baby boomers in Medicare increased by 2 to 2.3 fold and outpatient cost by 17.97 fold and although not statistically significant inpatient costs increased by 6.58-fold].





-----------------------------------------
Program Abstract
Hepatitis C (HCV) Infection in Baby Boomers Are Independently
Associated with Mortality and Resource Utilization
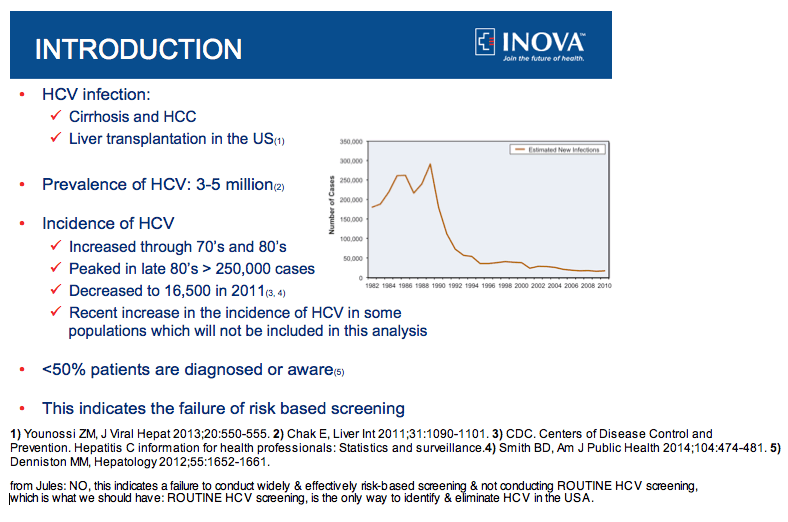
Background and aim: HCV is more common among Baby boomers (BB) (born 1946-1965). As this cohort age, they will increasingly become Medicare eligible. Our aim was to evaluate resource utilization and short term mortality of BB-Medicare recipients with HCV.
Method: We used inpatient and outpatient Medicare databases (2005-2010) with clinical data, admission and discharge information, ICD-9 codes, procedure codes, and billing information. Medicare patients who were considered BB were identified using all HCV-related ICD-9 codes. Charlson Index [comorbidity index/mortality sore.....https://en.wikipedia.org/wiki/Comorbidity] was calculated as a measure of comorbidity. The outcome measures included resource utilizations [payment per case and inpatient length of stay (LOS)] and short term mortality (90 days).
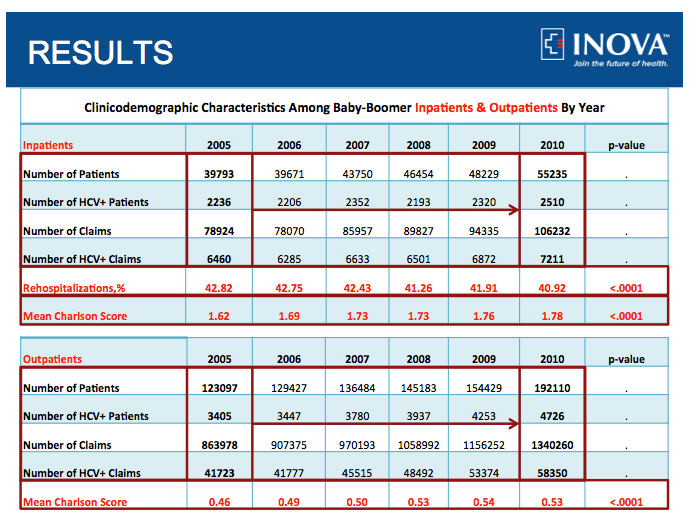
Results: We included 1,153,862 BB who received Medicare services from 2005 to 2010. Of these, 3.2% (N=37,365) were HCV (+). During this period, Medicare-BB in the inpatient setting increased from 39,793 to 55,235, and their claims increased from 78,924 to 106,232.
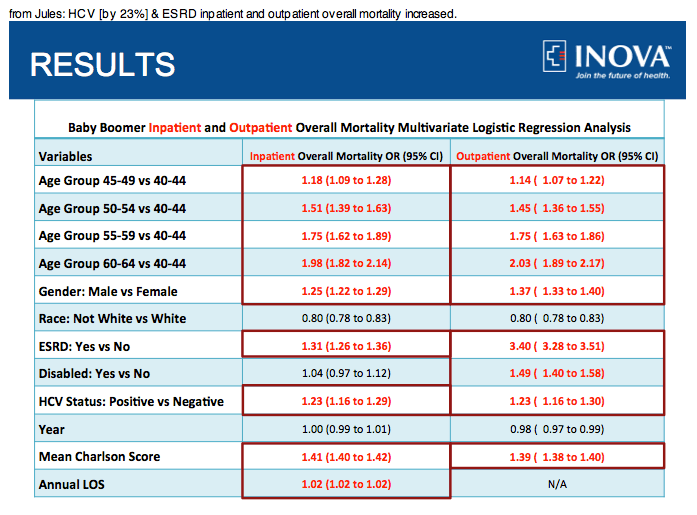
During the study period, both overall mortality [8.94% to 10.25% (p<.0001)] and mean Charlson score increased [1.62 to 1.78 (p<.0001)]. HCV(+) (OR=1.23, [1.16-1.29]), older age (OR=1.98, [1.82-2.14]), male gender (OR=1.25, [1.22-1.29]), ESRD (OR=1.31, [1.26-1.36]), Charlson score (OR=1.41, [1.40-1.42]), and LOS (OR=1.02, [1.02-1.02]) were independently associated with increased short-term mortality.
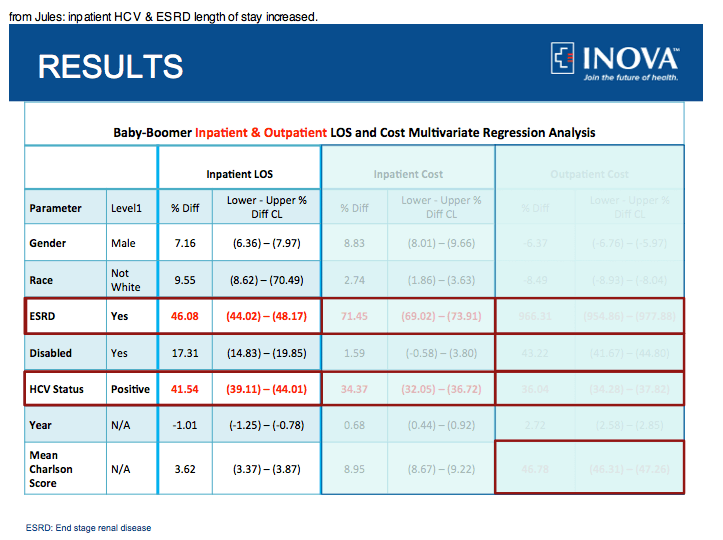
Annual inpatient LOS exhibited a steady decrease from 12.98 to 11.74 days (p<.0001), whereas annual total payments increased from $22,157 to $23,185 (p<.0001). During the study, the number of outpatients Medicare BB patients (123,097 to 192,110) and claims (863,978 to 1,340,260) increased. During the study, overall short-term mortality of Medicare-BB in outpatient increased from 3.15% to 3.31% (p=0.0131), while the mean Charlson score increased from
0.46 to 0.53 (p<.0001). Again, HCV(+) (OR=1.23, [1.16-1.30]), older age (OR=2.03, [1.89-2.17]), ESRD (OR=3.40, [3.28-3.51]), disabled status (OR=1.49, [1.40-1.58]), and Charlson score (OR=1.39, [1.38-1.40]) were independently associated with an increased risk of short-term mortality.
Annual total payments increased from $3,781 to $4,001 (p<.0001). HCV(+) (36.04%, [34.28 to 37.82]), BB age category of 45-49 (4.21%, [3.14-5.28]), ESRD (966.31%, [954.86-977.88]), disabled status (43.22%, [41.67-44.80]), Charlson score (46.78%, [46.31-47.26]), and year study (2.72%, (2.58-2.85]) were all independently associated with an increase in total payments.
Conclusions: Prevalence of HCV is higher in Baby boomers Medicare recipients. For the entire BB cohort, HCV positivity is independently associated with higher mortality and resource utilization.
-----------------------------------
from Jules: you can see in this Table number of inpatient HCV claims increased by 11% from 2005 thru 2010 and outpatient claims increased by 39%.
|
| |
|
 |
 |
|
|