 |
 |
 |
| |
Portal Pressure Changes After HCV Eradication in HIV/HCV+ Patients With Cirrhosis
|
| |
| |
Reported by Jules Levin
CROI 2015 Feb 23-26, Seattle, WA
Sanchez-Conde M1, Perez-Latorre L1,2, Rincon D1,2, Miralles P1,2, Catalina MV1,2, Lopez JC1,2, Banares R1,2,3, Berenguer J1,2
1Hospital General Universitario Gregorio Maranon, 2Instituto de Investigacion Sanitaria Gregorio Maranon (IiSGM), 3Universidad Complutense, Madrid, SPAIN



program abstract
Background: In patients with compensated cirrhosis (CR), hepatic venous pressure gradient (HVPG) is the most accurate predictor of liver-related events (LRE). In cirrhotic patients receiving pharmacologic treatment for prevention of variceal rebleeding, a decrease in HVPG ≥ 20% or to ≤ 12 mm Hg is associated with a marked reduction in the long-term risk of developing LRE and with improved survival (Hepatology 2003;37:902-908). We assessed the effect of sustained viral response (SVR) after pegylated interferon plus ribavirin (PR) on HVPG in HIV/HCV+ patients with CR.
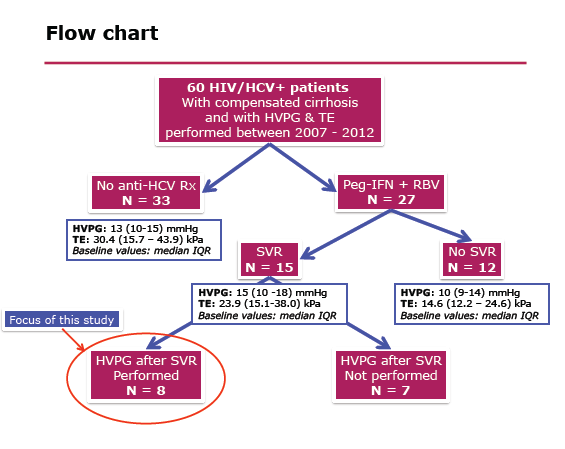
Methods: We reviewed the records of the portal hemodynamic laboratory of our institution to identify all HIV/HCV+ patients with CR who had a determination of HVPG before and after PR therapy between 2007 and 2012.
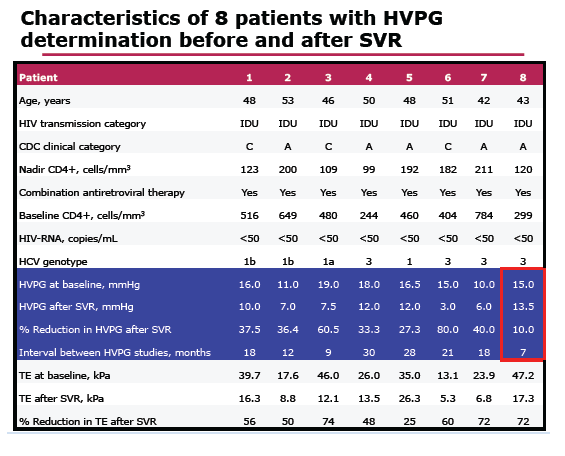
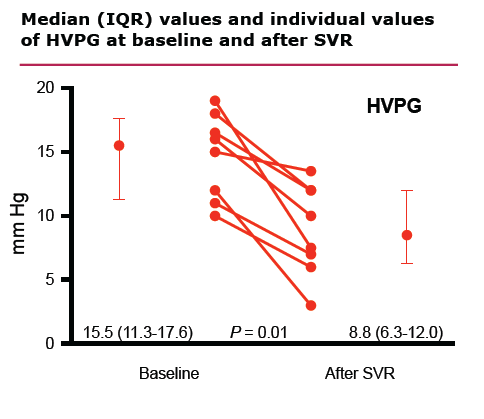
Results: HVPG was determined in 60 HIV/HCV+ patients with CR. A total of 27/60 patients were treated with PR, and 15/27 treated patients achieved SVR. Consent to perform a 2nd HVPG determination was given by 8/15 patients with SVR. In these 8 patients, the 2nd HVPG determination was performed a median time of 18 (10 - 26) months after the discontinuation of PR. The median (IQR) HVPG was 15.5 (11.3-17.6) mmHg at baseline, and 8.8 (6.3-12.00) mmHg following SVR; P=0.01.
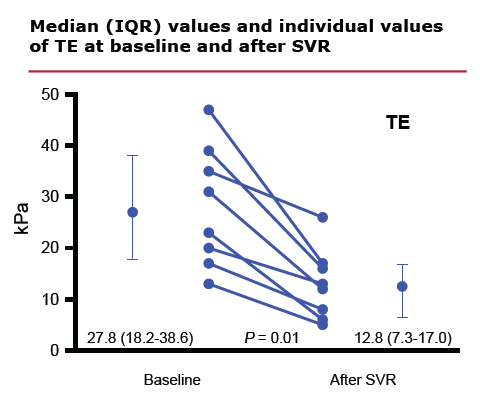
After SVR, 7/8 patients experienced a decrease in HVPG ≥ 20% and all 7 had HVPG ≤ 12 mm Hg. In one patient with SVR, HVPG decreased 10% with a last value of 13.3 mmHg. After a median follow-up time of 60 months, all 8 patients were alive and free from LRE. Figure 1 shows median and IQR values and individual values of HVPG at baseline and after SVR.
Conclusions: Our results suggest that eradication of HCV is associated with a marked and clinically significant reduction of HVPG in most HIV/HCV+ patients with CR and PH. However, some patients with CR and portal hypertension may remain at risk for LRE despite eradication of HCV.

|
| |
|
 |
 |
|
|