 |
 |
 |
| |
IL-6 is a stronger predictor of clinical events than hsCRP or D-dimer in HIV disease - SMART/ESPIRIT
|
| |
| |
Reported by Jules Levin
CROI 2015 Feb 23-26, Seattle, WA
AH Borges1, JL O'Connor2, AN Phillips2, JD Neaton3, B Grund4, J Neuhaus3, MJ Vjecha5, A Calmy6, KK Koelsch7,8and JD Lundgren1 for the INSIGHT, SMART and ESPRIT Study Groups 1CHIP, Department of Infectious Diseases, Section 2100, Rigshospitalet - University of Copenhagen Denmark; 2Research Department of Infection and Population Health, University College London, London, UK; 3Department of Biostatistics, University of Minnesota,
Minneapolis, Minnesota, USA; 4School of Statistics, University of Minnesota, Minneapolis, Minnesota, USA; 5Institute for Clinical Research, Inc., and Veterans Affairs Medical Center, Washington, D. C., USA; 6Division of Infectious Diseases, Geneva University Hospitals,
Geneva, Switzerland; 7The Kirby Institute for Infection and Immunity in Society, University of New South Wales, Sydney, Australia; 8St. Vincent's Centre for Applied Medical Research, St. Vincent's Hospital, Sydney, Australia

program abstract
Background: High-sensitivity C-reactive protein (hsCRP), interleukin-6 (IL-6) and D-dimer have been linked to risk of death and of many clinical outcomes during HIV infection. However, the strength of associations these biomarkers have with different types of clinical events is not well understood.
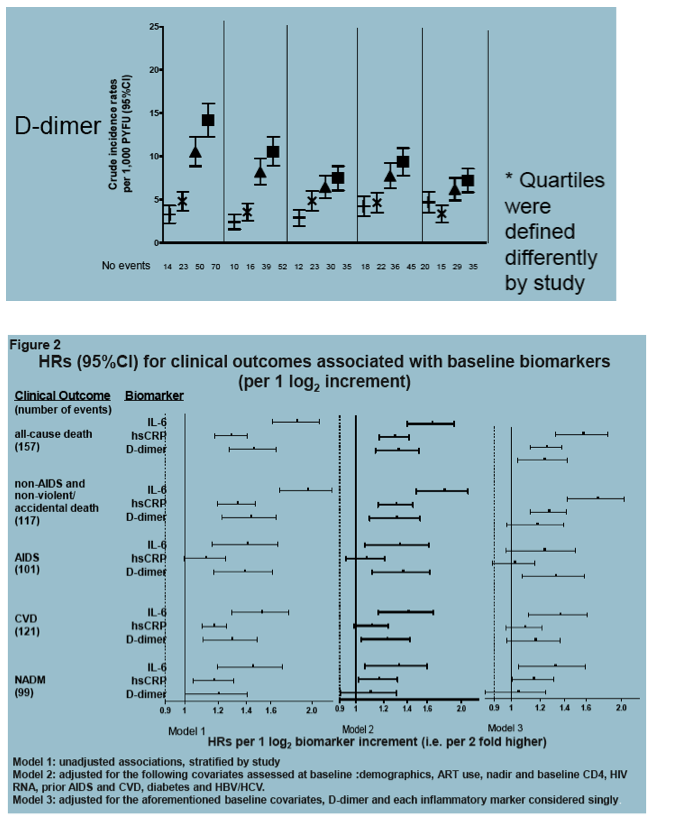
Methods: Participants receiving standard of care in the control arms of 2 HIV trials (SMART and ESPRIT) with biomarkers measured at baseline were followed from study entry to ascertain all-cause death, non-AIDS death, progression to AIDS, cardiovascular disease (CVD) and non-AIDS-defining malignancies (NADM). Marginal Cox models were used to model multiple unordered events and to test for equal effects of biomarkers on different clinical endpoints. HRs (95% CIs) stratified by study of each endpoint for log2-transformed hsCRP, IL-6 and D-dimer levels (i.e., per 2 fold higher) were calculated using the following Cox models: (1) unadjusted; (2) adjusted for demographics, ART use, nadir and baseline CD4, HIV RNA, prior AIDS and CVD, diabetes and HBV/HCV. We then recalculated HRs for IL-6 and D-dimer using models (3) that included both biomarkers simultaneously and HRs for hsCRP using a model also adjusted for D-dimer.
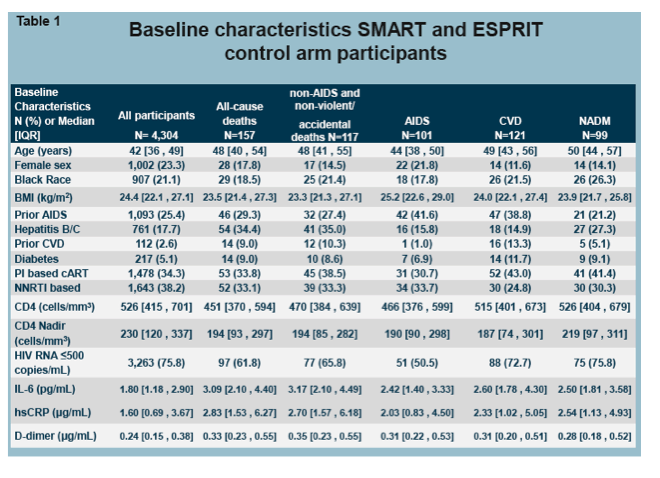
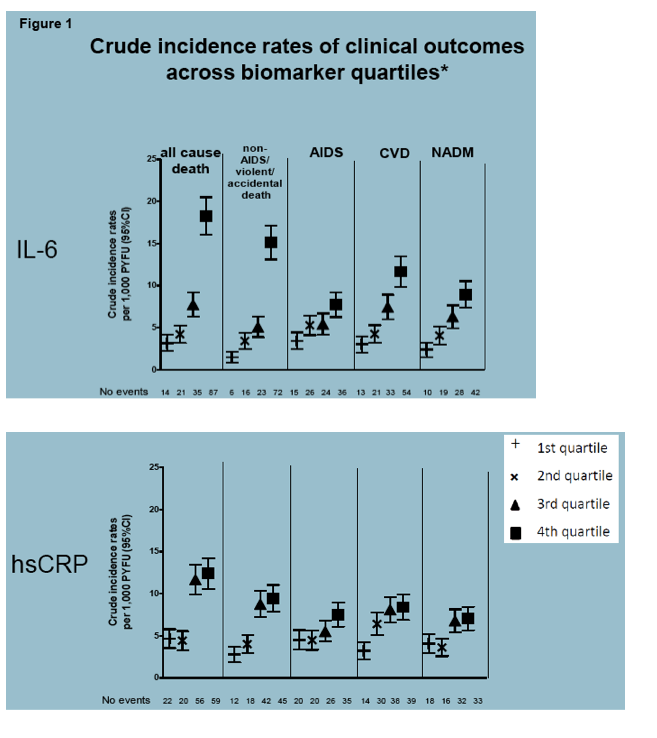
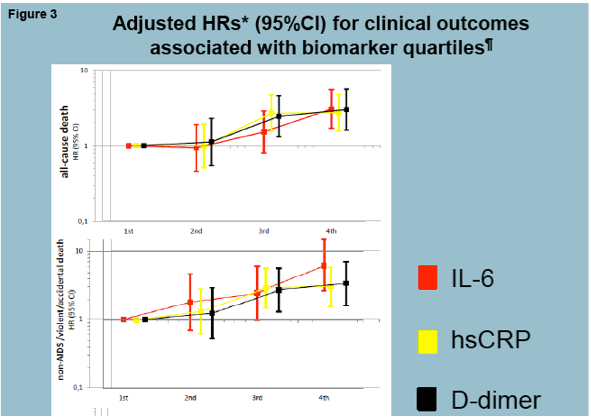
Results: There were 19000 person-years of follow-up among 4304 participants (median age 42y, median CD4 526, 77% men), including 157 all-cause deaths, 117 non-AIDS deaths, 101 progressions to AIDS, 121 CVD and 99 NADM (Table). In multivariable analyses, independent associations between IL-6 and clinical endpoints were strongest for non-AIDS death (1.71; 1.43-2.04) and similar for all-cause death (1.56; 1.33-1.84), CVD (1.35; 1.12-1.62) and NADM (1.30; 1.06-1.61). When compared to hsCRP, IL-6 was found to be more strongly associated with all outcomes investigated both in univariable and multivariable models. Likewise, IL-6 was a stronger predictor for most outcomes than D-dimer, except for progression to AIDS. We found evidence of heterogeneity in the predictive ability of IL-6 for different endpoints (p
Conclusions: The upstream inflammatory marker IL-6 is a stronger predictor of a variety of non-AIDS clinical events than the downstream inflammatory marker hsCRP or the hypercoagulation marker D-Dimer. IL-6 predicts fatal non-AIDS events more strongly than CVD or NADM. Evaluation of the clinical benefits from interventions able to reduce IL-6 levels in HIV is warranted.


|
| |
|
 |
 |
|
|