 |
 |
 |
| |
HIV and Cardiovascular Disease: Report back from 2015 Conference on
Retroviruses and Opportunistic Infections by Priscilla Hsue MD
|
| |
| |
Professor of Medicine, UCSF
This year at CROI, cardiovascular themed studies in HIV were strongly represented and were the topic of a plenary session given by Dr. Steven Grinspoon, MGH, as well as three oral presentations, and a special presentation by Dr. Monica Shah, regarding the National Heart, Lung, and Blood Institute High-Impact AIDS Research. There were over 30 abstracts on cardiovascular disease and HIV which is a noticeable increase from prior years.
Dr. Grinspoon's plenary session highlighted the work that his group has done evaluating the role of monocyte/macrophage activation in HIV-related vascular inflammation. He discussed the upcoming clinical trial that he is leading in collaboration with ACTG and NHLBI entitled REPRIEVE which will evaluate the impact of pitavastatin on clinical outcomes among HIV-infected individuals.
http://www.croiwebcasts.org/console/player/25786?mediaType=podiumVideo&
Indeed, a major focus of studies this year were investigating the impact of statin intervention in HIV-infected individuals. In Abstract 136. [webcast] Dr. Janet Lo reported on her group's results in a randomized, double-blind placebo-controlled study of 40 HIV-infected individuals with evidence of increased arterial inflammation using FDG-PET and LDL <130mg/dL. Individuals were treated with atorvastatin ranging from 20-40mg daily or placebo for 1 year. Change in FDG-PET uptake of the most diseased segment of the aorta was not different between the two groups, although adequate images could only be compared in 21 patients. In contrast, atorvastatin therapy reduced non-calcified plaque volume as compared to placebo with a median change of -19.4% vs. 20.4% (p=0.009). Overall plaque volume decreased 4.7% with atorvastatin vs. an 18.2% increase with placebo. Direct LDL and lipoprotein-associated phospholipase A2 decreased significantly in the atorvastatin treated individuals. This study has been published in Lancet (Lo J et al Vol 2, February 2015).
Similar findings were reported in Abstract 137 [webcast,] by Dr. Chris Longenecker along with Dr. Grace McComsey. SATURN-HIV was a 96 week double-blind randomized clinical trial of 10mg rosuvastatin daily vs. placebo among HIV-infected individuals with LDL-C less than or equal to 130mg/dL and evidence of heightened T-cell activation or increased inflammation (aka "JUPITER-HIV"). While CCA (common carotid artery) intima media thickness in the placebo group progressed significantly, it was unchanged in the statin group, with a mean difference between groups of 0.014mm/year, and a between group p value of 0.074 (p<0.05). There was no difference between development of new plaque among those without plaque at baseline between the two groups, while there was a trend toward more detectable CAC in the statin treated group among those without CAC at baseline, (15% statin vs. 6% placebo, p=0.19).
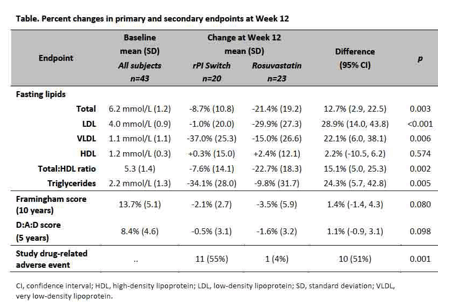
The impact of switching ART compared to statin therapy was evaluated in Abstract 733 [poster] by Dr. Baker and colleagues. This was a 12 week study of n=43 individuals with either a detectable HIV RNA level or total cholesterol less than or equal to 272mg/dl on a ritonavir boosted regimen. Within the switch group, most individuals were changed to raltegravir, rilpivirine or unboosted atazanavir. The rosuvastatin treated individuals had greater declines in total cholesterol, LDL cholesterol, and total/HDL ratio as compared to the ritonavir boosted individuals who switched regimens, and there were non-significant decreases in both the Framingham score and DAD score in the HIV-infected individuals on rosuvastatin. In contrast, the individuals who switched ART had greater decreases in VLDL and triglycerides as compared to the rosuvastatin treated patients. Individuals who switched regimens had more drug-related adverse events.
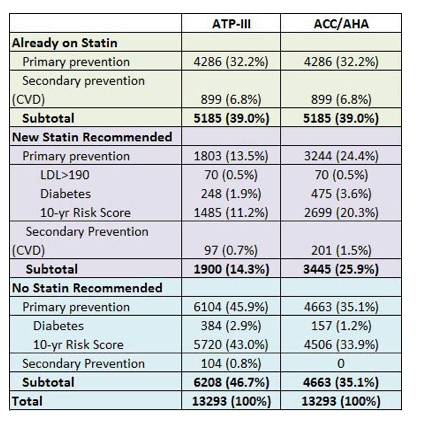
The impact of the new ACC/AHA Cholesterol guidelines which were released in fall 2013 was evaluated in two studies in the setting of HIV. In abstract 750 (poster), Dr. Clement and colleagues used the Veterans Affairs (VA Clinical Case Registry, CCR), to evaluate the impact of the new guidelines among HIV-infected veterans. She found that overall, 11.6% of HIV-infected adults (N=13293 males) not previously eligible for statin therapy using the prior guidelines (ATP-III) would now be recommended for statin treatment using the new ACC/AHA guidelines (representing an increase from 53.3% previously eligible to 64.9% eligible).
Most of the increase was from individuals meeting criteria for primary prevention with 9.1% newly recommended based on the revised ASCVD risk score, 1.7% recommended base on diabetes, and 0.8% recommended due to cvd.
A similar study was performed by Dr. Susan Regan and colleagues (Abstract 734, poster) in the Partners HealthCare System HIV longitudinal cohort of N=2239 HIV infected adults. In this Boston cohort, 41.8% were recommended for statin therapy using the new ACC/AHA guidelines as compared to 25.7% using the 2008 ATPIII guidelines and similar to the prior abstract, the most common indication for statin use was CVD risk of 7.5% using the new risk prediction algorithm.
Among individuals with a CVD event, statin therapy was recommended for 44% of individuals using ATPIII and 62% using ACC/AHA. Interestingly, despite more individuals being recommended for statin therapy, around 40% of patients with CVD events would not qualify for statin treatment using the ACC/AHA guidelines. This study underlies the issue that even among individuals with HIV, traditional risk factors only account for approximately 20% of cad and unknown factors which may be more prominent in HIV infection are likely not captured using traditional risk calculators.
So, should we as clinicians prescribe statins for all HIV patients? Will statin target the inflammatory pathways of interest in HIV? The data on clinical outcomes and statin intervention are largely mixed and will be the focus of the REPRIEVE study. Data from the SATURN study (Abstract 137, webcast) along with Janet Lo's atorvastatin study suggest that inflammatory markers and immune activation are largely not reduced by statin therapy. New drugs for lipid lowering and inflammatory interventions are being evaluated by other ongoing clinical trials.
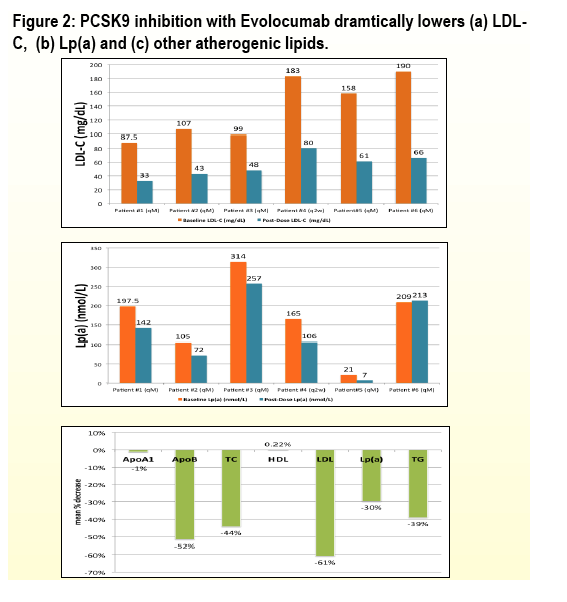
The focus of Abstract 731 (poster) was on PCSK9 which is a promising new target of pharmacologic inhibition that has had impressive results for lowering low-density lipoprotein-cholesterol (LDL-C) in the general population and may prove to be a valuable therapy in HIV-infected patients. Patients with HIV are at high risk for CVD and tend to be difficult to treat due to drug-drug interactions with anti-retroviral therapies and limited efficacy of stains. We aimed to collect preliminary data on PCSK9 levels and its homeostasis in this small cohort study. We found that PCSK9 is elevated in HIV infection, with high levels of PCSK9 that were never before observed in prior studies with >20,000 patients. PCSK9 elevation was not related to HIV-specific parameters, such as viral load or CD4 count. We have also shown, in a pilot study of 6 patients inadvertently enrolled into clinical trials of PCSK9 inhibitors, that PCSK9 inhibition with a monoclonal antibody was highly effective and appeared to be safe in 6 patients with reductions in LDL-C of around 60%.
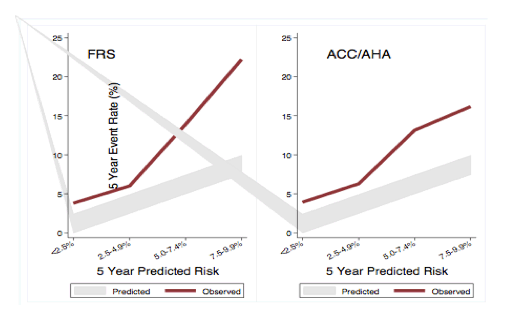
To further investigate the issue of CVD risk prediction in HIV, in Abstract 751, investigators in Boston calculated the Framingham risk scores and ACC/AHA risk scores in the Partner's Cohort (N=2270 patients) in a 3 year interval ending in 2009. Risk scores were discordant in 17% of individuals with the ACC/AHA risk calculator predicting risk in 10% of patients and FRS predicting high risk in 7% of individuals. Both the ACC/AHA risk score and the FRS underestimated CVD risk in HIV patients, comparing 5-year observed to predicted event rates.
Four different risk calculator were compared in the HIV Outpatient Study (Abstract 747, poster) which represent 2392 individuals receiving care at 10 US clinic sites as of 9/2013 and had a year of followup, 1 assessment of cholesterol and two measurements of blood pressure. The Framingham point score, pooled cohort equation, systematic coronary risk evaluation and DAD equations were compared as shown in the Table below:
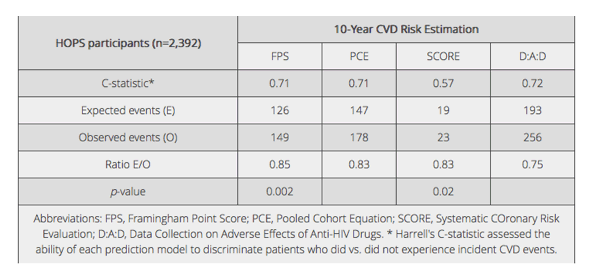
Overall all four risk prediction equations underestimated the 10 year risk of CVD in this HOPS cohort of HIV-infected adults in the U.S. The FPS, PCE, and DAD had moderate discrimination with a c-statistic ranging from 0.68 to 0.72 and the SCORE had poor discrimination (c-statistic =0.59).
The Veterans Aging Cohort Study Virtual Cohort (VACS VC) was used to evaluate the role of copy years of viremia, CD4 years, and VACS index years (age, HIV-1 RNA, CD4, LFTs, Hg, platelet, creatinine, and known HCV infection) in abstract 746 (poster). Among 12,131 individuals included in the analysis, cumulative measures of HIV viral load, CD4 count, and the VACS index provided added information about AMI (acute myocardial infarction) risk. The VAC index was the most comprehensive as shown in the table below
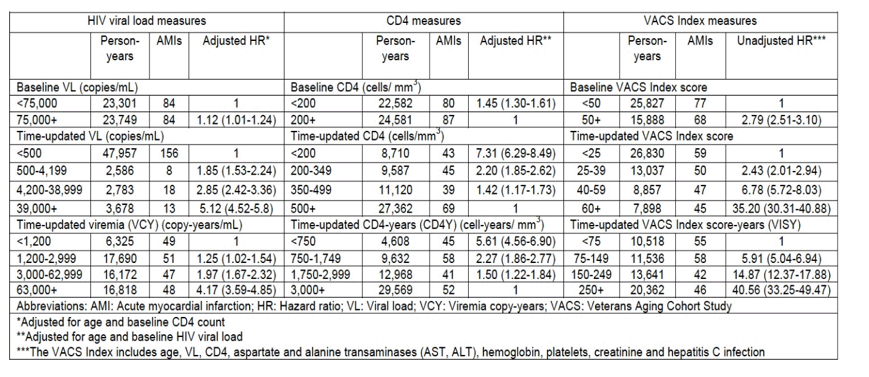
Table 1. Multivariable Cox Proportional Hazards analyses of factors associated with time to Acute Myocardial Infarction among patients starting Initial ART regimens in the VACS Virtual Cohort; 2000-2009.
The authors concluded that Participants with the highest cumulative viremia (in the upper quartile of viremia
copy-years) ran a 2.6-fold increased risk of MIs.Cumulative CD4 counts were not statistically significantly associated with an
increase of MI incidence.
Participants in the highest quartile of VACS index score--years ran a 4 times
higher risk of MI incidence during the study.
These results showing that risk predictor algorithms developed in non-HIV populations do not apply to HIV infected individuals is not surprising. They do not take into account HIV-related features that likely contribute including ART, chronic inflammation, and immune activation. Interestingly, even the DAD calculator which was developed in HIV performed similarly to the other calculators demonstrating that even in HIV, one size does not fit all - suggesting perhaps differences in the HOPS patient populations as compared to the DAD individuals. Validation of HIV-specific risk calculators in different HIV cohorts will be needed in the future.
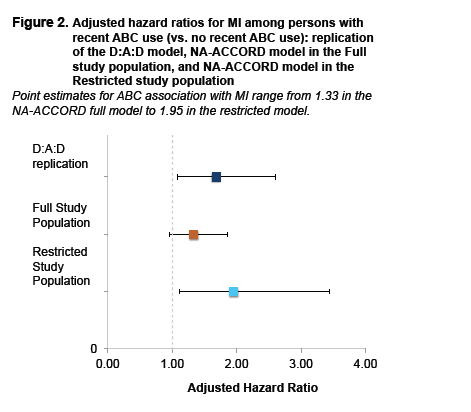

Two studies from NA-ACCORD were also featured. In Abstract 749LB (poster), Frank Palella and colleagues looked at recent ABC use and incident MIs using MESA criteria in the North American Cohort (NA-ACCORD). There were a total of 301 incident MIs in 16,733 adults and 64,607 person-years of followup Recent abacavir use (defined as prescription within 6 months) was associated with 1.71 (1.11, 2.64) increased risk of MI in an adjusted models that were analogous to ones used in DAD, and the results linking current abacavir use to MI risk is similar to the original DAD result reported in 2009. In the full study population in the adjusted analysis, the significance was lost. However, in the restricted population, the finding remained significant even after adjustment. Of note, this is the first study to show risk of ABC present among ART naïve individuals initiating ART which is a new contribution to the field. The controversy over abacavir seems to ebb and tide but has not gone away completely.
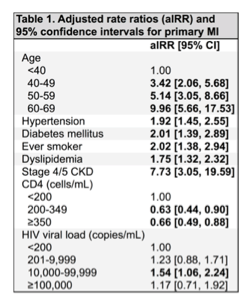
In Abstract 748 (poster) investigators from NA-ACCORD determined the incidence of adjudicated primary MIs distinct from secondary MIs and examined baseline risk factors for primary MIs - the Universal Definition of MI, which includes class primary Type I Mis which are due to atherothrombotic plaque and secondary (type 2) MIs which are due to a mismatch in supply/demand - for example, troponin leak in the setting of sepsis. Seven NA-ACCORD cohorts were included in the study between 1996-2010 time period resulting in 24,919 individuals with 262 Type I MIs and 205 Type II MIs. Traditional risk factors along with lower CD4 count were associated with Type 1 MIs as shown in Table. In contrast, sepsis, cocaine, respiratory failure, and hypertensive emergency were responsible for 50% of Type 2 MIs. This abstract is an important contribution as it is the first to acknowledge the differences in MI definitions which impact treatment and conclusions drawn from studies. For example, type II MIs are not usually treated with aspirin, beta blockers, statins etc but typically by addressing the primary issue - ie drug use, sepsis which is in contrast to Type 1 MIs. The distinction between Type 1 and Type 2 MIs in HIV cohorts thus is a critical one and may underlie some of the contrasting data that has been previously reported in different cohort studies.
The association between a microbiota-derived precursor of TMAO, namely TMA, and coronary plaque was described in Abstract 138 (webcast) by Dr. Suman Srinivasa. One hundred fifty five HIV-infected individuals along with 67 uninfected controls were studied. Serum choline trimethylamine (TMA) and trimethylamine-N-oxide (TMAO) were assessed using mass-spectometry and cardiac CT angiography was used to assess coronary plaque. Among HIV-infected patients, TMA was associated with number of plaques, calcified plaques, calcium score, plaque volume and mass and LPS. After adjustment for Framingham risk score, TMA remained significantly associated with total, calcified, calcium score, plaque volume and mass. After additional adjustment for LPS, TMA remained associated with total plaque segments, calcium score, and plaque mass. There was no association of TMAO to plaque in contrast.
Trimethylamine-N-oxide (TMAO) is metabolized by intestinal microbiota from dietary lipids. In uninfected persons, TMAO levels are associated with cardiovascular events.
TMAO levels and carotid IMT were evaluated in a small study done at UCSF (abstract 755). The median TMAO levels were similar among HIV patients and controls; however TMAO levels between HIV patients were similar to uninfected patients with CAD. Traditional risk factors along with current ARV were associated with higher TMAO levels and TMAO was weakly associated with carotid IMT.
In summary, HIV and cardiovascular diseases were an expanding arena of investigation at CROI 2015. The emphasis this year was on statin interventions, evaluation of the new ACC/AHA cholesterol guidelines in HIV, abacavir and risk of MI, comparison of risk calculators in HIV, and new markers of CV risk such as TMAO. New event driven trials such as REPRIEVE and other smaller proof of concept studies designed to target inflammation in HIV are ongoing, and NHLBI along with NIAID is committed to supporting studies in HIV with dedicated funding for HIV-related investigations.
|
| |
|
 |
 |
|
|