 |
 |
 |
| |
Smoking and heavy drinking tied to atherosclerosis in MACS men with HIV
|
| |
| |
CROI 2015, February 23-26, 2015, Seattle, Washington
Mark Mascolini
Smoking proved more strongly associated with coronary artery plaque in HIV-positive than negative men in the US Multicenter AIDS Cohort Study (MACS) [1]. Alcohol use protected against atherosclerosis in HIV-negative MACS men but not in men with HIV. Indeed, heavy drinking by HIV-positive men was linked to almost 5 times higher odds of coronary artery stenosis greater than 50%.
Asymptomatic atherosclerosis is common in HIV-positive people, MACS researchers who conducted this study noted. Smoking certainly raises the risk of cardiovascular disease, but potential links between smoking and other substance use and atherosclerosis remain poorly characterized in people with HIV. Yet smoking and substance use are highly prevalent in many HIV populations. To get a better understanding of how smoking and other substance habits affect atherosclerosis, MACS investigators conducted this study.
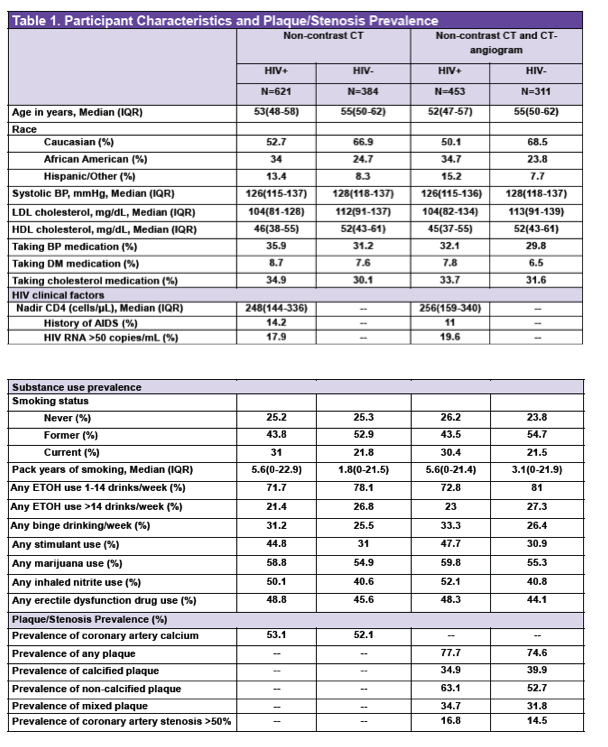
MACS is a prospective cohort of HIV-positive and at-risk men who have sex with men in the United States. Cohort members make twice-yearly visits for checkups and lifestyle survey updates. Men in this cardiovascular substudy had to be 40 to 70 years old, had to weigh under 300 pounds, and could not have a history of cardiac surgery, angioplasty, or stent. For coronary artery calcium measurement, 621 men with HIV and 384 without HIV underwent noncontrast CT scans. A subset of these men--453 with HIV and 311 without HIV--had coronary CT angiography to assess plaque presence, type, and extent.
On their twice-yearly surveys, men reported smoking and use of alcohol and recreational drugs, including stimulants and erectile dysfunction drugs. The MACS team characterized smoking as current or former at the time of CT scanning and measured cumulative pack-years. They rated alcohol use as low/moderate, heavy, and binge drinking, and they weighted use of other substances by frequency of use. Low/moderate drinking meant 1 to 14 drinks a week, while heavy drinking meant more than 14 drinks a week and binge drinking meant 5 or more drinks in succession at least once in the past 30 days. The investigators used logistic regression to identify associations between plaque presence and substance use; they used linear regression to spot associations between plaque extent and substance use.
Median age was somewhat lower in men with HIV (53 versus 55). About one third of HIV-positive men were black, compared with one quarter of HIV-negative men. Current smoking prevalence was higher in men with than without HIV (31% versus 22%), while the HIV group included a lower proportion of former smokers (44% versus 53%). Heavy alcohol use was less prevalent in men with HIV (21% versus 27%), while binge drinking was more common in men with HIV (32% versus 26%). A higher proportion of HIV-positive men used any stimulant (45% versus 31%), and similar proportions used erectile function enhancers (49% versus 47%).
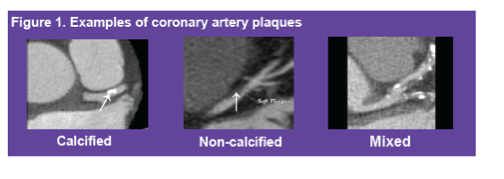
Prevalence of any coronary artery calcium was similar in men with and without HIV (53% and 52%). Men with HIV had a marginally higher prevalence of any plaque (78% versus 75%), a higher prevalence of dangerous noncalcified plaque (63% versus 53%), and a slightly higher prevalence of coronary artery stenosis greater than 50% (17% versus 15%).
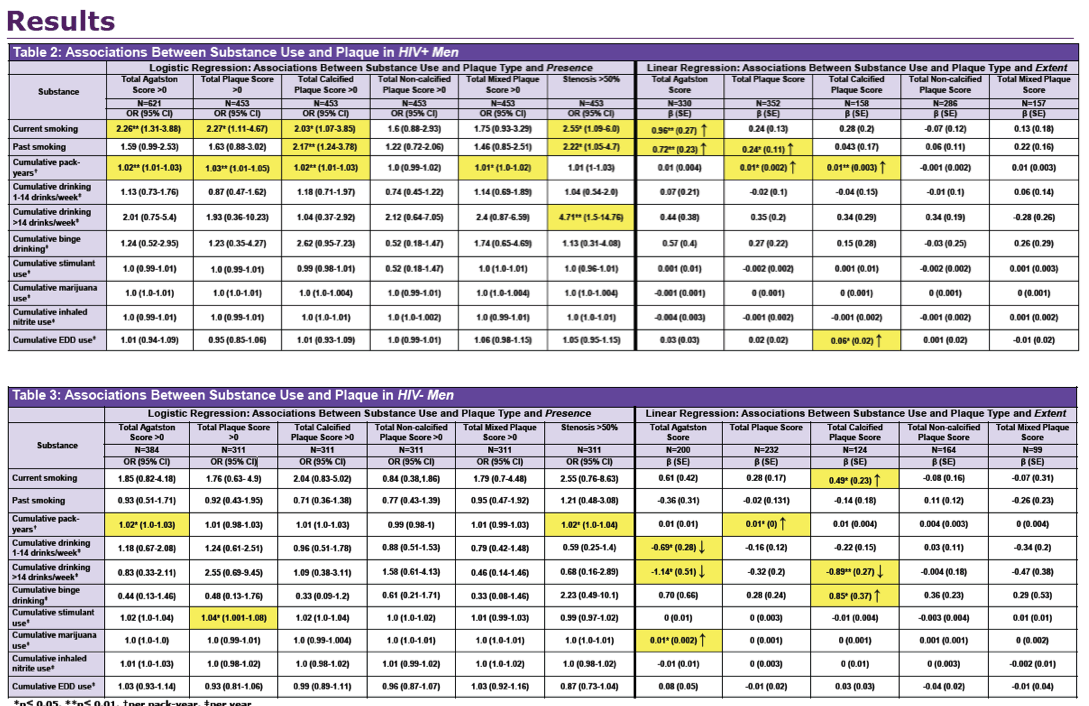
In men with HIV current smoking was associated with total Agatston score [2] (odds ratio [OR] 2.28), total plaque score (OR 2.27), total calcified plaque score (OR 2.03), and stenosis greater than 50% (OR 2.55), but not total noncalcified plaque score. Current smoking was also associated with greater plaque extent by total Agatston score. Past smoking was associated with stenosis greater than 50% (OR 2.22).
The analysis linked cumulative pack-years to total Agatston score (OR 1.02 per year), total plaque score (1.03 per year), total calcified plaque score (OR 1.02 per year), and total mixed plaque score (OR 2.22 per year), as well as to greater plaque extent by total plaque score and total calcified plaque score. In contrast, in men without HIV the only smoking measure linked to plaque presence was cumulative pack-years, which was tied to total Agatston score and to stenosis greater than 50%.
In men with HIV heavy drinking was associated with almost 5 times higher odds of stenosis greater than 50% (OR 4.71, 95% confidence interval 1.5 to 14.76). In contrast to men with HIV, in men without HIV low/moderate drinking was associated with lower plaque extent by Agatston score and heavy drinking was associated with lower plaque extent by Agatston score and calcified plaque score, findings suggesting alcohol offers some protection against atherosclerosis in men without HIV but not men with HIV.
The only other substance association in men with HIV was between cumulative erectile dysfunction drug use and extent of plaque by total calcified plaque score.
The MACS investigators suggested their findings "underscore the importance of effective smoking cessation strategies targeting HIV-positive men to decrease cardiovascular risk burden." They did not speculate on reasons for the lack of alcohol's protective effect in men with HIV, saying that question needs more study.
References
1. Kelly S, Palella F, Post W, et al. Smoking, other substance use and coronary atherosclerosis among HIV-infected and uninfected men. CROI 2015. February 23-26, 2015. Seattle, Washington. Abstract 743.
2. Agatston score reflects the extent of coronary artery calcification detected on CT. Goel A, et al. Agatston score. http://radiopaedia.org/articles/agatston-score
----------------------------------
Reported by Jules Levin
Smoking, Other Substance Use and Coronary Atherosclerosis Among HIV-Infected and Uninfected Men
Sean G. Kelly1, Michael Plankey2, Wendy S. Post3, 4, Xiuhong Li4, Ronald Stall5, Lisa P. Jacobson4, Mallory Witt6, Lawrence Kingsley5, Christopher Cox4, Frank J. Palella Jr.1
1Northwestern University Feinberg School of Medicine, Chicago, IL; 2Georgetown University, Washington DC; 3Johns Hopkins University School of Medicine, Baltimore, MD; 4Johns Hopkins Bloomberg School of Public Health, Baltimore, MD; 5University of Pittsburgh, Pittsburgh, PA; 6Harbor-UCLA Medical Center, Torrance, CA



|
| |
|
 |
 |
|
|