 |
 |
 |
| |
Modified FRAX tool underestimates fracture rates in older men with HIV
|
| |
| |
CROI 2015, February 23-26, 2015, Seattle, Washington
Mark Mascolini
A modified version of FRAX, the web-based fracture risk calculator, underestimated fracture rates in HIV-positive men more than HIV-negative men in the Veterans Aging Cohort Study-Virtual Cohort (VACS-VC) [1]. Using a common FRAX threshold for pharmacologic intervention would leave untreated 97% of men who end up with a fracture.
Studies in diverse populations record higher fracture rates in people with HIV than in comparison groups. In the United States the HIV Medicine Association recommends DXA scans for men and women over 50. The European AIDS Clinical Society goes one step further, recommending DXA for HIV-positive men over 50 and postmenopausal women and FRAX without bone mineral density determination for HIV-positive people over 40. In the general population FRAX sees wide use to inform decisions on screening and treatment to prevent fracture.
A web-based algorithm (www.shef.ac.uk/FRAX) developed by the World Health Organization, FRAX calculates 10-year probability of (1) major osteoporotic fractures (of the hip, spine, humerus, and wrist) and (2) hip fracture. Michael Yin (Columbia University) and colleagues at other centers noted that FRAX does not predict osteoporosis by DXA or prevalent fractures in people with HIV. They conducted this VACS-VC analysis to see if FRAX predicts 10-year fracture risk and incidence equally in older men with and without HIV.
FRAX figures fracture risk by assessing data such as age, sex, race, weight, and smoking. HIV is not on the FRAX risk list. But because FRAX may underestimate fracture risk with HIV, some authorities advise checking off "secondary osteoporosis" on the FRAX list as a surrogate for HIV infection.
To see how well FRAX works in older men with and without HIV, Yin and colleagues mined data from the VACS-VC cohort of HIV-positive and negative men 50 to 70 years old. They included men with near-complete data from the year 2000. "Near-complete" means men did not need data on secondary osteoporosis or parental hip fracture. As a result the researchers call their index a modified FRAX. To determine fracture incidence, the investigators used ICD-9 codes to identify new fractures of the hip, spine, upper arm, or wrist from 2001 through 2010.
Yin and colleagues aimed to rate FRAX by two measures: (1) calibration (agreement between observed and predicted fractures), and (2) discrimination (ability to discriminate between men with and without fracture). Calibration is reckoned as an observed/estimated (O/E) ratio, with a ratio of 1.0 indicating perfect accuracy.
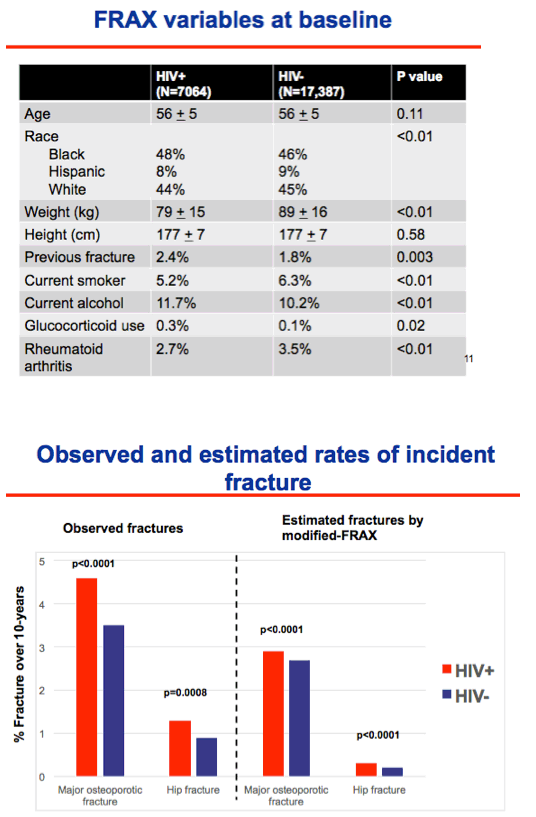
The analysis involved 24,451 men, 7064 (29%) with HIV and 17,387 without HIV. Both groups averaged 56 years in age, and each group included similar proportions of blacks and whites (about 45% each). The HIV group had higher rates of several fracture risk factors: lower average weight (79 versus 89 kg, P < 0.01), higher proportion of previous fractures (2.4% versus 1.8%, P = 0.003), higher proportion of current alcohol drinkers (11.7% versus 10.2%, P < 0.01), and higher proportion of current glucocorticoid use (0.3% versus 0.1%, P = 0.02). The HIV group did better than the HIV-negative group in two risk categories: current smokers (5.2% versus 6.3%, P < 0.01) and rheumatoid arthritis (2.7% versus 3.5%, P < 0.01).
Modified FRAX predicted a significantly higher fracture rate at osteoporotic sites in men with than without HIV over 10 years (2.85% versus 2.71%, P < 0.0001) and a higher hip fracture rate in men with HIV over 10 years (0.29% versus 0.24%, P < 0.0001). These FRAX predictions lay well below 10-year observed fracture incidence, which was significantly higher in men with than without HIV at osteoporotic sites (4.61% versus 3.50%, P < 0.0001) and at the hip (1.32% versus 0.85%, P = 0.0008).
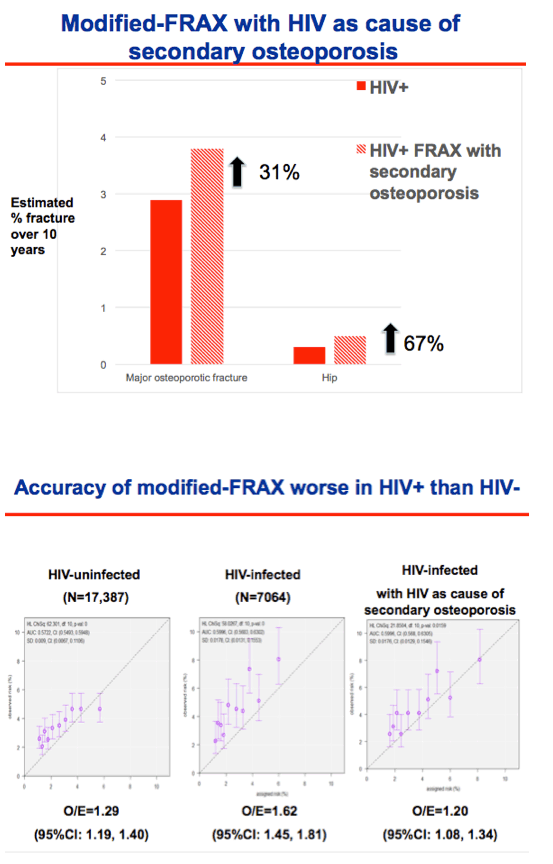
When the investigators further modified the FRAX algorithm to include HIV as a cause of secondary osteoporosis, 10-year predicted major osteoporotic fractures rose 31% and 10-year predicted hip fractures rose 67%. But the resulting predictions still lay well below observed fracture incidence.
Accuracy of modified FRAX determined by the observed/estimated ratio was worse in men with HIV (O/E ratio 1.62, 95% confidence interval [CI] 1.45 to 1.81) than in men without HIV (O/E ratio 1.29, 95% CI 1.19 to 1.40). Accuracy improved in HIV-positive men to a level similar to HIV-negative men when FRAX included HIV as a cause of secondary osteoporosis (O/E ratio 1.20, 95% CI 1.08 to 1.34).
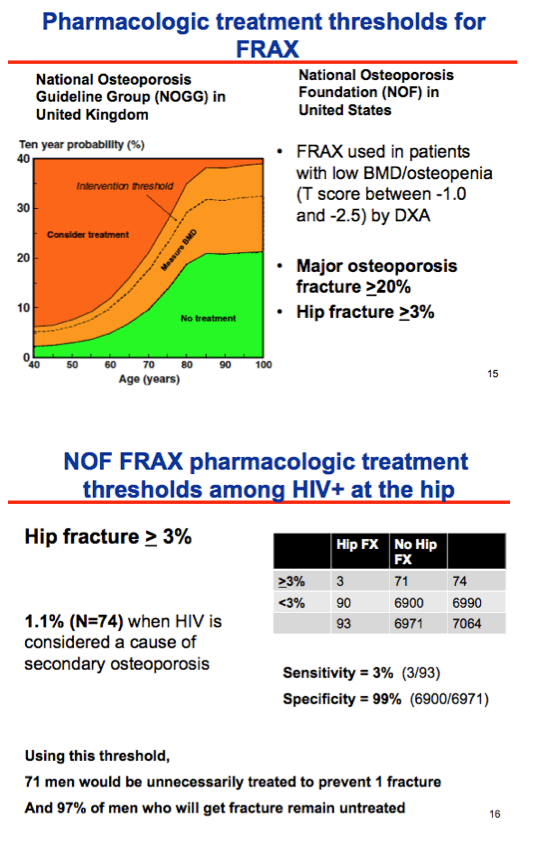
Discrimination was poor with the modified FRAX and did not differ between men with and without HIV. Adding secondary osteoporosis to the equation did not improve discrimination. Using National Osteoporosis Foundation FRAX-based pharmacologic treatment thresholds in this population of men with HIV would result in unnecessarily treating 71 men to prevent one fracture, yet 97% of men who endure a fracture would remain untreated.
Yin and colleagues concluded that modified FRAX accuracy is limited in older men with HIV and that its role in risk stratification of men with HIV or triggering pharmacotherapy "requires additional study."
webcast:
http://www.croiwebcasts.org/console/player/25795?mediaType=slideVideo&
Reference
1. Yin MT, Skanderson M, Shiau S, et al. Fracture prediction with modified FRAX in older HIV+ and HIV- men. CROI 2015. February 23-26, 2015. Seattle, Washington. Abstract 141.







|
| |
|
 |
 |
|
|