 |
 |
 |
| |
Differing cART Responses in Naive Women and Those With Short-Term cART in Pregnancy
|
| |
| |
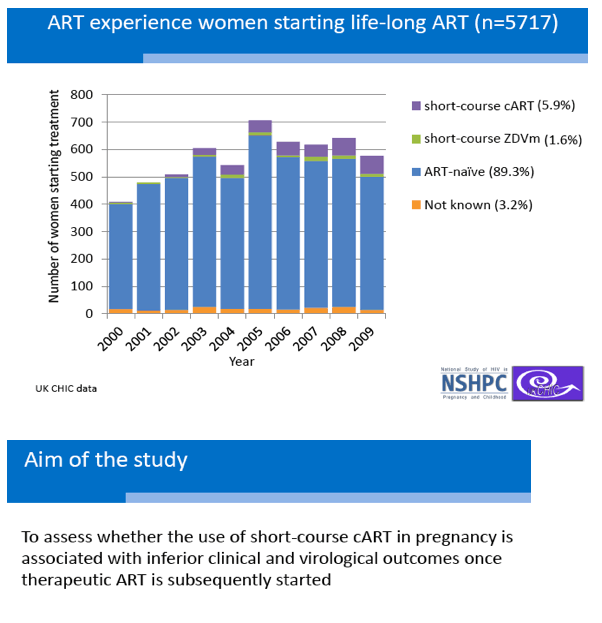
Aim of the study: To assess whether the use of short-course cART in pregnancy is associated with inferior clinical and virological outcomes once therapeutic ART is subsequently started
15th European AIDS Conference, October 21-24, 2015, Barcelona
Mark Mascolini
Women who took short-term combination antiretroviral therapy (cART) during pregnancy reached an undetectable viral load after later starting steady cART as often as women who began steady cART with no previous use during pregnancy, according to results of a large United Kingdom (UK) study [1]. But women with short-term cART experience in pregnancy proved more likely to interrupt cART and to rebound 6 to 24 months after of viral suppression.
With collaborators from other institutions, University College London researchers gathered data on women starting cART in the United Kingdom by linking datasets from the UK and Ireland National Study of HIV in Pregnancy and Childhood (NSHPC) and the UK CHIC cohort. The analysis included women starting lifelong cART in 2006-2010 after being diagnosed with HIV for more than 1 year. All study participants were 16 to 49 years old.
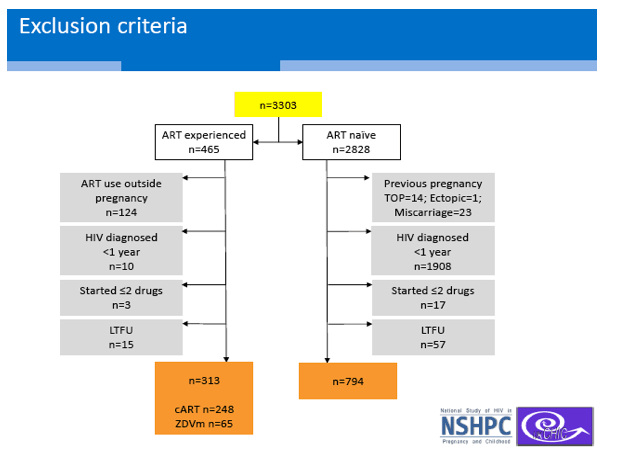
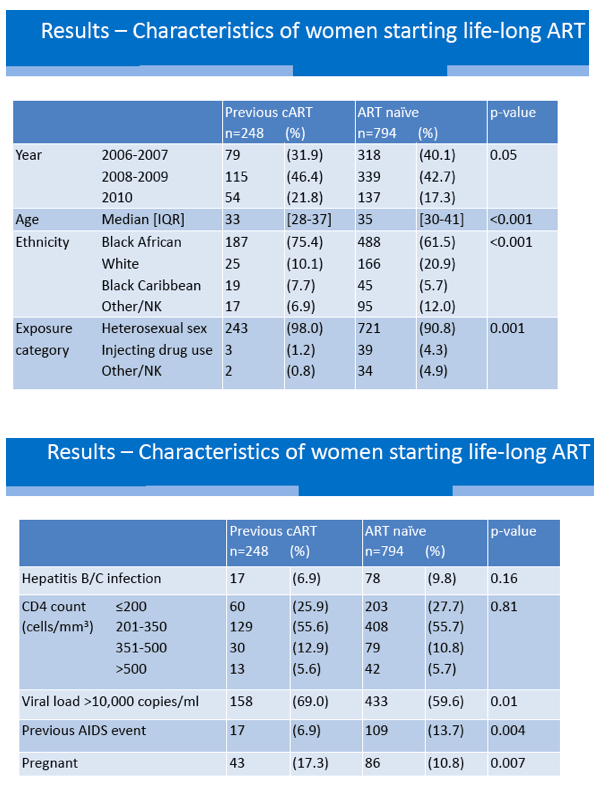
Of the 1042 women studied, 794 (76%) began cART with no antiretroviral experience (the naive group) and 248 started steady cART after taking short-term cART during pregnancy (the experienced group). Median age was lower in the experienced group (33 versus 35, P < 0.001), and the experienced group included a higher proportion of black Africans or Caribbeans (83.1% versus 67.2%) and a lower proportion of whites (10.1% versus 20.9%) (P < 0.001). The experienced group included a higher proportion who acquired HIV heterosexually (98% versus 90.8%) and a lower proportion who became infected by injecting drugs (1.2% versus 4.3%) (P = 0.001).
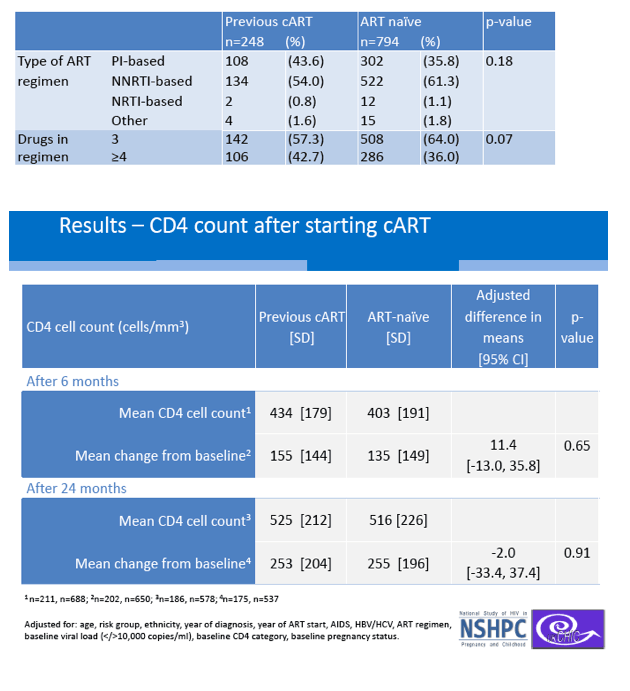
Baseline CD4 counts were similar in experienced and naive women. A higher proportion of experienced women had a pretreatment viral load above 10,000 copies (69% versus 59.6%, P = 0.01), though a lower proportion had an AIDS diagnosis (6.9% versus 13.7%, P = 0.004). A lower proportion of experienced women started a nonnucleoside regimen (54% versus 61.3%) and a higher proportion started a protease inhibitor (43.6% versus 35.8%) but these differences lacked statistical significance (P = 0.18).
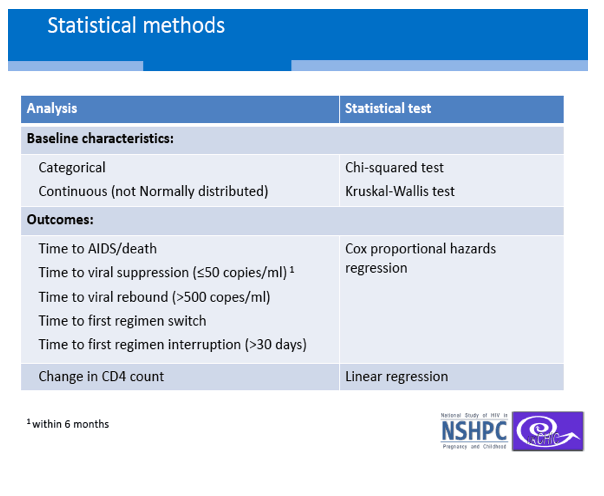
An analysis adjusted for age, ethnicity, baseline CD4 count and viral load, and other variables determined that experienced women gained about 11 more CD4 cells than naive women through 6 months of steady cART, a nonsignificant difference (adjusted mean difference 11.4, 95% confidence interval [CI] -13.0 to 35.8, P = 0.65). After 24 months of therapy even that difference disappeared (adjusted mean difference -2.0, 95% CI -33.4 to 37.4, P = 0.91).
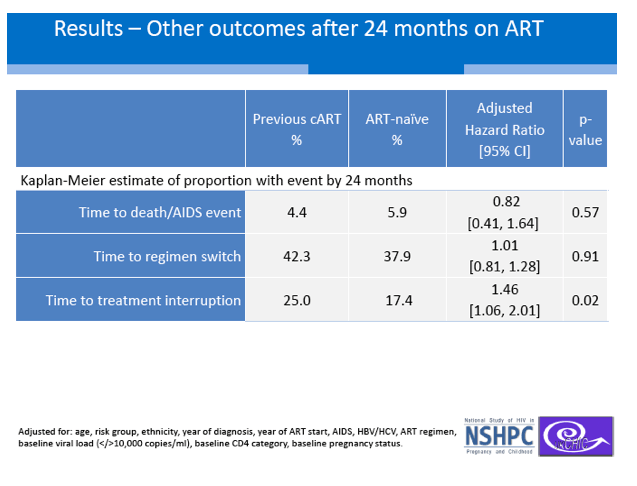
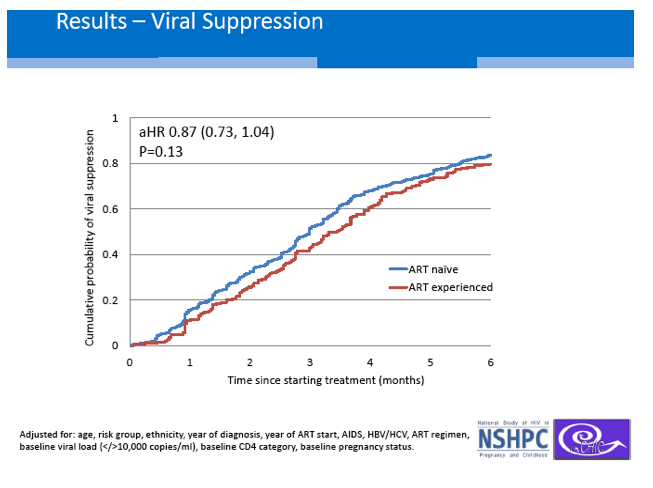
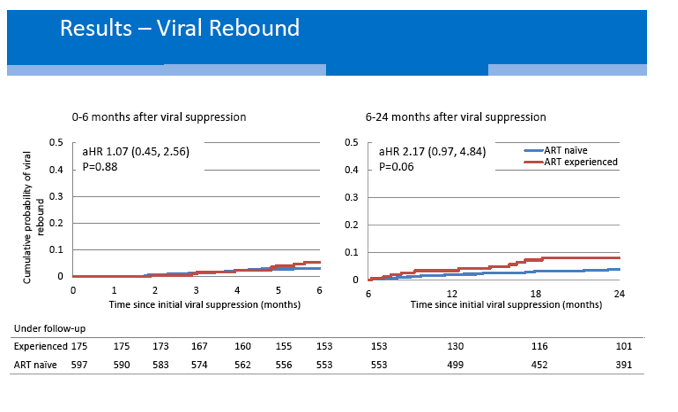
After 6 months of steady cART, experienced women had a nonsignificantly lower chance of reaching an undetectable viral load (adjusted hazard ratio [aHR] 0.87, 95% CI 0.73 to 1.04, P = 0.13). Six to 24 months after viral suppression, the experienced group had a doubled risk of viral rebound at a hazard ratio within a whisker of statistical significance (aHR 2.17, 95% CI 0.97 to 4.84, P = 0.06). After 24 months on cART, the experienced and naive groups did not differ by time to death or an AIDS diagnosis or by time to a regimen switch. But the experienced group had nearly a 50% higher risk of interrupting treatment (aHR 1.46, 95% CI 1.06 to 2.01, P = 0.02).
The researchers noted that their analysis is limited by lack of data on women recently diagnosed with HIV and by insufficient resistance data for meaningful analysis. With those limitations in mind, they concluded that women who took short-term cART during pregnancy were as likely to achieve viral suppression within 6 months as women who did not take short-term cART during pregnancy. CD4 gains were similar in the two groups, but women who took cART during pregnancy were more likely to interrupt steady cART once it began and more likely to have a viral rebound 6 to 24 months after viral suppression.
With more women starting long-term cART at diagnosis regardless of CD4 count, the researchers noted, the proportion of women with short-term experience during pregnancy is dwindling in the UK--and elsewhere. For women who do have short-term cART experience for any reason before starting long-term therapy, the researchers say they "may expect slightly poorer outcomes," but the differences from women with no short-term experience will be small.
Reference
1. Huntington S, Thorne C, Newell ML, et al. Outcomes after 2 years on antiretroviral therapy (ART): comparison of women who were ART-naive and women who previously used short-course ART in pregnancy. 15th European AIDS Conference, October 21-24, 2015, Barcelona. Abstract PS6/4.
------------------------
Reported by Jules Levin
Outcomes after 2 years on ART in women who previously used short-course ART in pregnancy and women who were ART-naïve
S Huntingtona,b, C Thornea, ML Newellc, J Andersond, G Taylore, D Pillayb,f, T Hillb, P Tookeya, C Sabinb on behalf of UK CHIC and the NSHPC
aUCL Institute of Child Health, UK;
bUCL Research Dept of Infection & Population Health, UK;
cUniversity of Southampton, UK;
dHomerton University Hospital NHS Foundation Trust, UK;
eImperial College, UK;
fAfrica Centre for Health and Population Studies, S. Africa



|
| |
|
 |
 |
|
|