 |
 |
 |
| |
Predicting Fractures by DEXA- new technique
|
| |
| |
"We conducted a pilot case-control study to determine whether HSA parameters correlate with fracture in HIV-infected adults [from Jules: can fracture risk be predicted by HSA from DEXA]..... A history of fracture was associated with decreased composite measures of estimated bone strength on hip structural analysis [HSA] among HIV-infected adults, particularly at the intertrochanteric area. Further work is needed to characterize the role of HSA in assessing fracture risk in HIV patients.Ó
Decreased bone strength on hip structural analysis in HIV+ adults with versus without fractures
Reported by Jules Levin
IAS 2015 Vancouver July 19-23
Presented by Darrell Tan
D. Tan1, J. Raboud2, L. Szadkowski3, E. Szabo4, H. Hu4, Q. Wong4, A. Cheung3, S. Walmsley5
1St. Michael's Hospital, Toronto, Canada, 2Dalla Lana School of Public Health, University of Toronto, Toronto, Canada, 3Toronto General Research Institute, Toronto, Canada, 4Centre for Excellence in Skeletal Health Assessment, University of Toronto, Toronto, Canada, 5University Health Network, Toronto, Canada
program abstract
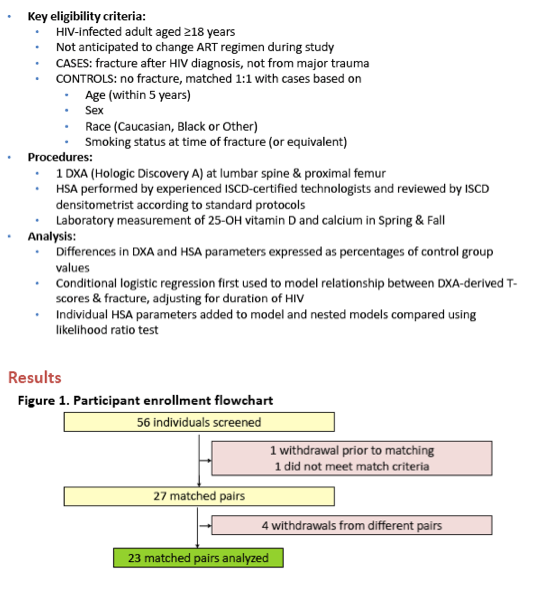
Background: Bone mineral density (BMD) as assessed by dual-energy x-ray absorptiometry (DXA) is often used to assess fracture risk, but is limited by the lack of a clear fracture threshold and of validation in younger people or patients with HIV. We conducted a pilot case-control study to determine whether bone geometric parameters and estimated strength as assessed by hip structural analysis (HSA) correlate with fractures in this population.
Methods: Adults with a history of low-trauma fracture after HIV diagnosis (cases) were matched 1:1 with HIV-infected adults without prior fractures (controls) based on age, sex, race and smoking history. Participants underwent DXA at the hip and lumbar spine, and image files underwent HSA by trained study personnel. The buckling ratio (a measure of cortical stability under compressive loads, i.e. axial strength), section modulus (a measure of bending strength), cross-sectional area and average cortical thickness were compared between cases and controls using Wilcoxon signed rank sum tests, with differences expressed as percentages of control group values.
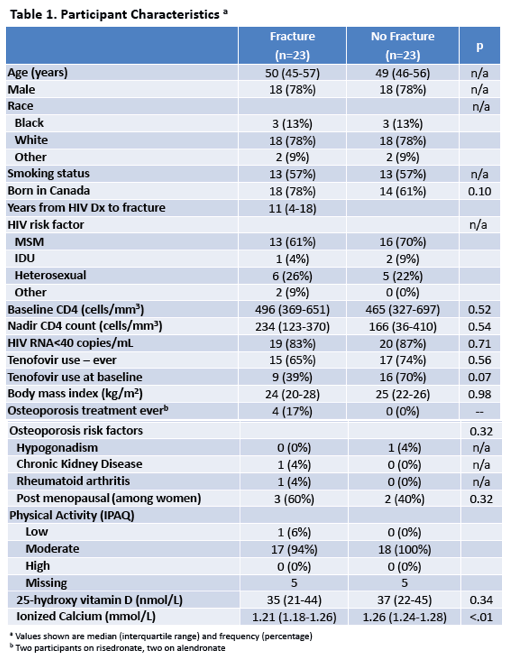
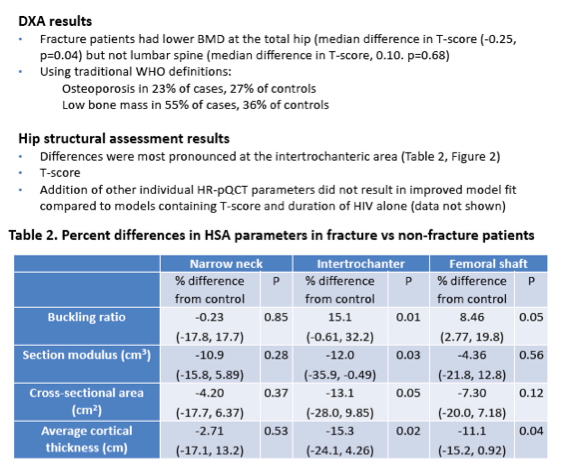
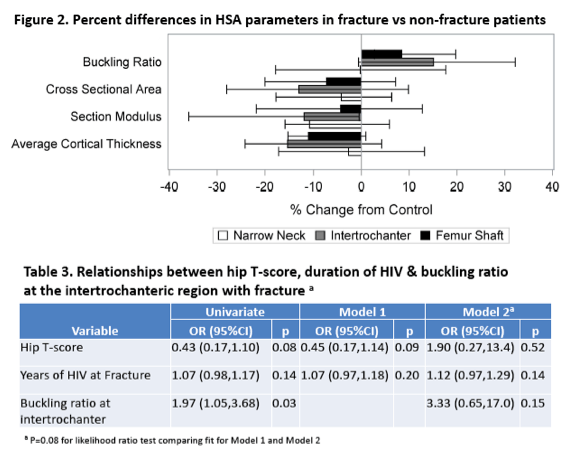
Results: 23 matched pairs were included, with median (IQR) age 50 (46,56) years, 78% male, 78% white and 57% smokers. Median (IQR) duration of HIV was 19 (11,23) years for cases and 10 (7,18) years for controls. On DXA, cases had significantly lower BMD at the total hip (median difference =-4.3%, p=0.04), but not the lumbar spine (-3.47%, p=0.33). Statistically significant differences on HSA were observed at the intertrochanteric area, where the buckling ratio was 15.1% greater (p=0.01), section modulus was 12.0% lower (p=0.03), cross-sectional area was 13.1% lower (p=0.05) and average cortical thickness was 15.3% lower (p=0.02) among cases than controls (see Table). At the femoral shaft, buckling ratio was significantly greater by 8.46% (p=0.05) and average cortical thickness was significantly lower by 11.1% (p=0.04). Differences at the narrow neck did not reach statistical significance.
Conclusions: A history of fracture was associated with decreased composite measures of estimated bone strength on hip structural analysis among HIV-infected adults, particularly at the intertrochanteric area. Further work is needed to characterize the role of HSA in assessing fracture risk in HIV patients.

|
| |
|
 |
 |
|
|