 |
 |
 |
| |
Age, IDU, Viral Load Testing Rate Predict HIV Control and Rebound in Canadian MSM
|
| |
| |
IAS 2015, July 19-22, 2015, Vancouver
Mark Mascolini
A higher viral load testing rate predicted both viral suppression and rebound with a first antiretroviral regimen in a study of more than 3000 men who have sex with men (MSM) across Canada [1]. Older age predicted suppression and younger age favored rebound. Injection drug use (IDU) cut chances of suppression and boosted rebound risk. Starting a boosted protease inhibitor (PI) trimmed chances of viral suppression 20% compared with starting a nonnucleoside (NNRTI).
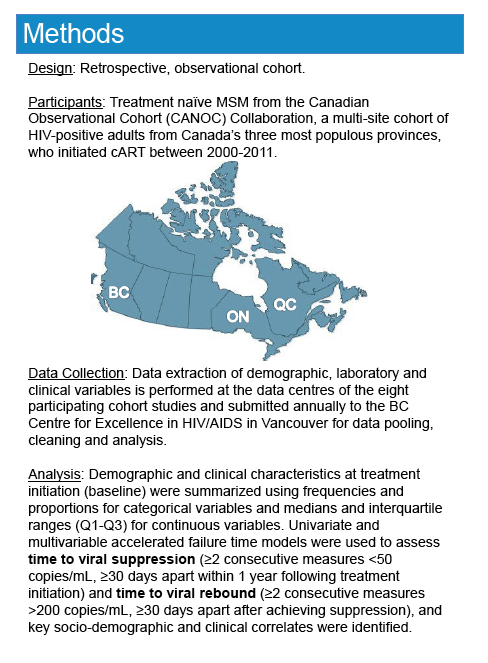
MSM account for the lion's share of HIV infections across Canada, but relatively little is known about antiretroviral treatment outcomes nationally among MSM. To address that question, researchers retrospectively analyzed data on MSM in the Canadian Observational Cohort (CANOC) starting antiretroviral therapy (ART) from 2000 through 2011 in the country's three most populous provinces, British Columbia, Ontario, and Quebec. Eight participating cohort centers submit data annually to a central unit, where data get pooled and analyzed.
The CANOC team defined viral suppression as two or more consecutive viral loads below 50 copies measured at least 30 days apart within 1 year after ART began. They defined rebound as two or more consecutive viral loads at or above 200 copies measured at least 30 days apart after viral suppression.
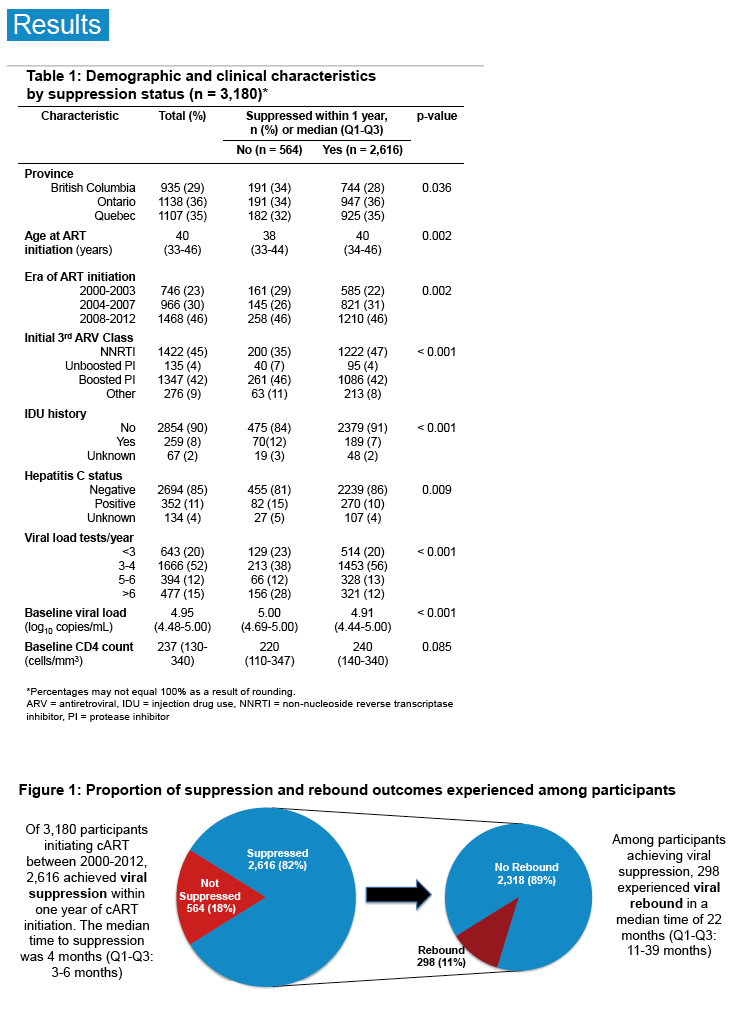
The analysis included 3180 MSM, 259 (8%) of whom reported injection drug use, with similar proportions from British Columbia (29%), Ontario (36%), and Quebec (35%). While 23% of men started ART in 2000-2003, 30% began in 2004-2007 and 46% in 2008-2012. Median age when ART began stood at 40 years, median viral load stood at 4.95 log10 (about 89,000 copies), and median CD4 count at 237.
During the first year of treatment, 2616 men (82%) achieved viral suppression. Median time to suppression measured 4 months. Of the 2616 suppressors, 298 (11%) rebounded in a median of 22 months. Multivariate analysis identified several independent predictors of suppression and rebound at the following adjusted hazard ratios (aHR) and 95% confidence intervals:
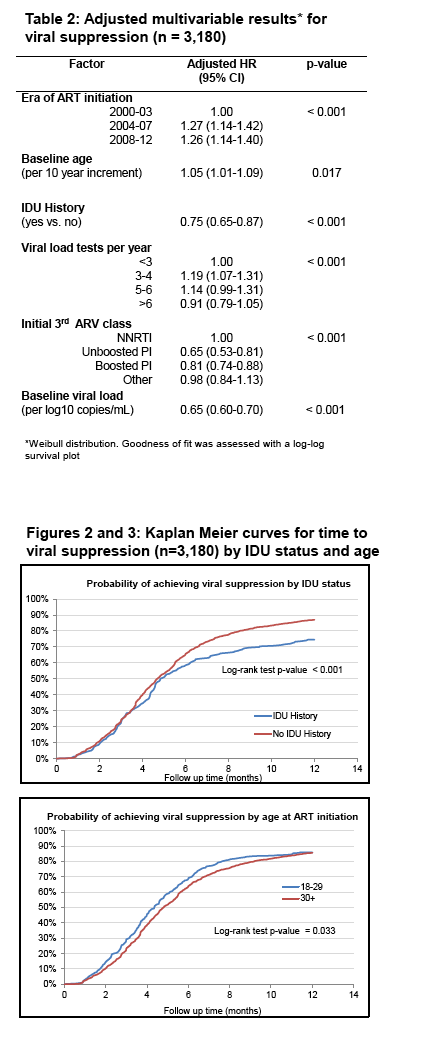
Suppression predictors
Starting ART in 2004-07 vs 2000-03: aHR 1.27 (1.14 to 1.42)
Starting ART in 2008-12 vs 2000-03: aHR 1.26 (1.14 to 1.40)
Every 10 more years of age at baseline: aHR 1.05 (1.01 to 1.09)
IDU history: aHR 0.75 (0.65 to 0.87)
3-4 viral load tests per year vs <3: aHR 1.19 (1.07 to 1.31)
5-6 viral load tests per year vs <3: aHR 1.14 (0.99 to 1.31)
Started unboosted PI vs NNRTI: aHR 0.65 (0.53 to 0.81)
Started boosted PI vs NNRTI: aHR 0.81 (0.74 to 0.88)
Every 10-fold higher baseline viral load: aHR 0.65 (0.60 to 0.70)
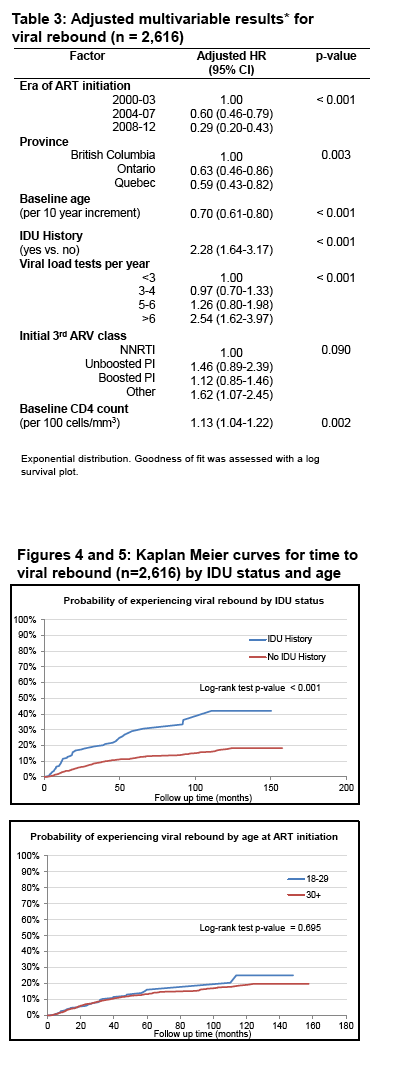
Rebound predictors
Starting ART in 2004-07 vs 2000-03: aHR 0.60 (0.46 to 0.79)
Starting ART in 2008-12 vs 2000-03: aHR 0.29 (0.20 to 0.43)
Ontario vs British Columbia: aHR 0.63 (0.46 to 0.86)
Quebec vs British Columbia: aHR 0.59 (0.43 to 0.82)
Every 10 more years of age at baseline: aHR 0.70 (0.61 to 0.80)
IDU history: aHR 2.28 (1.64 to 3.17)
>6 viral load tests per year vs <3: aHR 2.54 (1.62 to 3.97)
Every 100-cell higher baseline CD4 count: aHR 1.13 (1.04 to 1.22)
The CANOC researchers noted that Canadian MSM nearly meet the UNAIDS target that 90% of people starting ART reach an undetectable viral load. Notably, both younger age and injection drug use history heightened the risk of failure to reach an undetectable viral load and the risk of rebound in suppressors. The authors suggested that dual finding "reinforces the importance of prioritizing appropriately tailored case management interventions to avoid future treatment failure among Canadian MSM."
Reference
1. Tanner Z, Lachowsky N, Patterson S, et al. Predictors of viral suppression and rebound among HIV-positive gay, bisexual, and other men who have sex with men in a large multi-site Canadian cohort. IAS 2015. 8th Conference on HIV Pathogenesis, Treatment and Prevention. July 19-22, 2015. Vancouver. Abstract MOPED743.
---------------------


|
| |
|
 |
 |
|
|