 |
 |
 |
| |
Evaluation and Management of Fracture Risk in HIV Patients in the VA system: .....Fractures - HIV+ Vets NO SCREENING/PREVENTION! ..... One Quarter of HIV+ Vets Have Recurrent Fracture--After Minimal Testing or Treatment
|
| |
| |
IAS 2015, July 19-22, 2015, Vancouver
from Jules: hardly anyone was getting DXA or Vit D levels checked
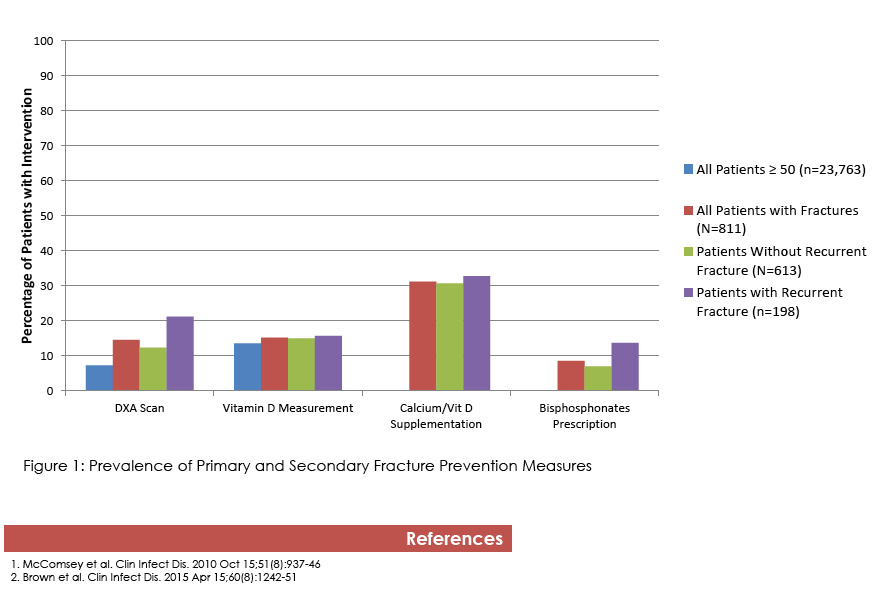
"Prior to incident fracture, 1735 (7.3%) had a DXA scan done, and 3242 (13.6%) had vitamin D levels measured"
"Following the incident OF, a DXA scan was performed only in 139 (17.1%) of patients, and 238 (29.4%) had a Vitamin D measurement. Calcium or Vitamin D supplementation were prescribed in 295 (36.4%), and bisphosphonates in 89 (11%) patients."

Mark Mascolini
One quarter of HIV-positive US veterans 50 or older had a second osteoporotic fracture after an initial fracture, according to a 23,763-veteran analysis [1]. But only 17% had a DXA scan after their first fracture and only 29% had vitamin D measured.
Meta-analysis confirms that HIV-positive people have higher fracture rates than the general population because of an array of traditional and HIV-specific risk factors [2]. Bone guidelines for people with HIV have recommended DXA scans for people older than 50 since 2010 [3], and 2015 guidelines repeat that recommendation [4]. To chart incident (new) and recurrent osteoporotic fractures in HIV-positive veterans--plus screening and treatment rates--before the 2010 guidelines appeared, researchers conducted this retrospective analysis.
The study focused on HIV-positive veterans 50 or older while in care from 1996 to 2010. The investigators used ICD-9 codes to identify incident osteoporotic fractures (wrist, hip, vertebrae) and recurrent fractures, defined as any new osteoporotic fracture diagnosed at least 6 months after the incident fracture. Then they determined proportions of veterans with incident or recurrent fracture who had bone-related testing (DXA scan or vitamin D level) or treatment (calcium, vitamin D, or bisphosphonate).
The analysis included 23,763 HIV-positive veterans 50 or older, 98% of them men, 35% black, and 39% with HCV coinfection. Incident osteoporotic fractures occurred in 811 vets for a rate of 2.92 per 1000 person-years. Before these new fractures, only 1735 veterans (7.3%) had a DXA scan and only 3242 (13.6%) had vitamin D measured.
Among veterans with an incident fracture, 198 (24.4%) had a recurrent osteoporotic fracture for a recurrence rate of 70 per 1000 person-years. After incident fractures, only 139 veterans (17.1%) had a DXA scan and only 238 (29.4%) had vitamin D measured. Among veterans with an incident osteoporotic fracture, 295 (36.4%) got calcium or vitamin D supplementation and 89 (11%) got a bisphosphonate prescription.
Regression analysis determined that every additional 10 years of age boosted recurrent fracture risk 41% (adjusted hazard ratio [aHR] 1.41, 95% confidence interval 1.19 to 1.65, P < 0.01). Race, HCV coinfection, smoking status, and body mass index did not affect recurrent fracture risk in this analysis.
Four fracture preventive measures predicted fracture recurrence at the following adjusted hazard ratios (and 95% confidence intervals):
-- DXA scan: aHR 1.91 (1.22 to 3.00), P < 0.01
-- Vitamin D measurement: aHR 2.52 (1.61 to 3.93), P < 0.01
-- Calcium/vitamin D supplementation: aHR 1.49 (1.05 to 2.13), P = 0.03
-- Bisphosphonate prescription: aHR 2.07 (1.21 to 3.56), P < 0.01
These associations indicate that DXA scanning, vitamin D measurement, and treatment appropriately targeted veterans more likely to break a bone a second time. Still, the researchers stress that, before the 2010 HIV bone guidelines came out, "only a very small proportion of HIV-infected US Veterans ≥ 50 years old received primary or secondary fracture prevention." If those low testing and treatment rates persist after release of the 2010 and 2015 guidelines [3,4], "an effort to educate HIV providers on prevention and management of osteoporotic fracture would be needed."
The 2015 HIV bone guidelines are available at the NATAP link listed in reference 4.
References
1. Cutrell J, Zhang S, Drechsler H, Tebas P, Maalouf NM, Bedimo R. Evaluation and management of fracture risk in HIV patients in the VA system. IAS 2015. 8th Conference on HIV Pathogenesis, Treatment and Prevention. July 19-22, 2015. Vancouver. Abstract WEPEB345.
2. Shiau S, Broun EC, Arpadi SM, Yin MT. Incident fractures in HIV-infected individuals: a systematic review and meta-analysis. AIDS. 2013;27:1949-1957.
3. McComsey GA, Tebas P, Shane E, et al. Bone disease in HIV infection: a practical review and recommendations for HIV care providers. Clin Infect Dis. 2010;51:937-946.
4. Brown TT, Hoy J, Borderi M, et al. Recommendations for evaluation and management of bone disease in HIV. Clin Infect Dis. 2015;60:1242-1251. http://www.natap.org/2014/HIV/012315_01.htm
---------------


|
| |
|
 |
 |
|
|