 |
 |
 |
| |
Follow-up Screening Rates Low for Breast and Cervical Cancer in HIV+ Women
|
| |
| |
IDSA/IDWeek 2015, October 7-11, San Diego
Mark Mascolini
Only half of HIV-positive women at a large New Jersey HIV clinic had follow-up cervical cancer screening, and fewer than one third had ongoing screening for breast cancer [1]. Women diagnosed with breast cancer averaged 44 years in age.
Rutgers New Jersey Medical School researchers noted that one third of HIV-positive people in the United States are now women. As these women age thanks to better antiretroviral therapy, they run an increasing risk of cancer. A 2011 population study found an overall jump in reproductive cancers in women with HIV [2]. The Rutgers team conducted this study to measure reproductive cancer rates in women with HIV and to assess adherence to cancer screening guidelines.
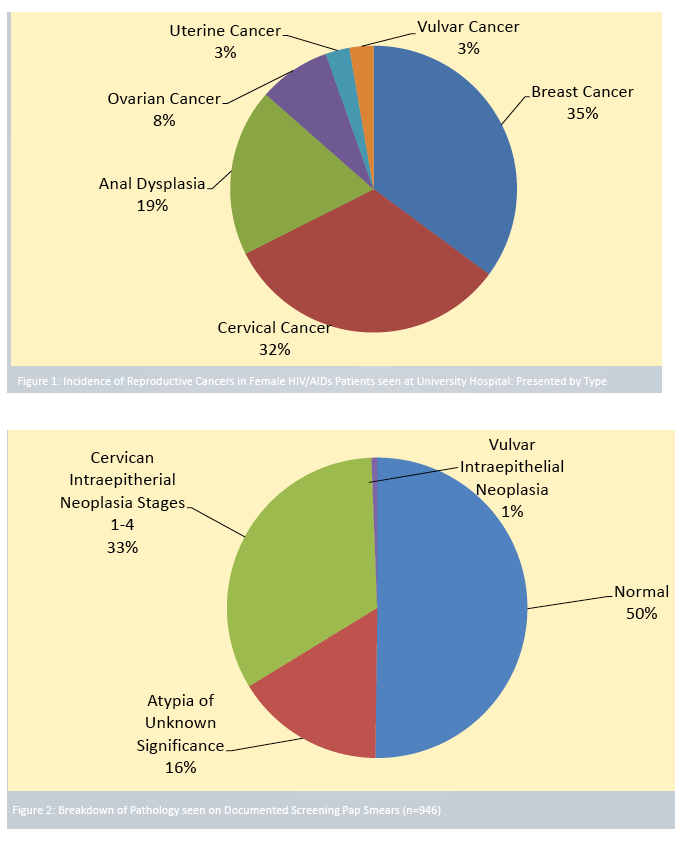
The researchers focused on 1812 HIV-positive women seen at Rutgers at some point from 2002 through 2014. This group included 1089 women who had at least two outpatient visits in the Rutgers HIV clinic after 2002. Among the 1812 women in the chart review, 78 (4.3%) had one or more malignancy, including 37 reproductive cancers (2.0%). The most frequent reproductive cancers were breast cancer in 13 women (35%), cervical cancer in 12 (32%), and anal dysplasia in 7 (19%), followed by ovarian cancer (8%), uterine cancer (3%), and vulvar cancer (3%).
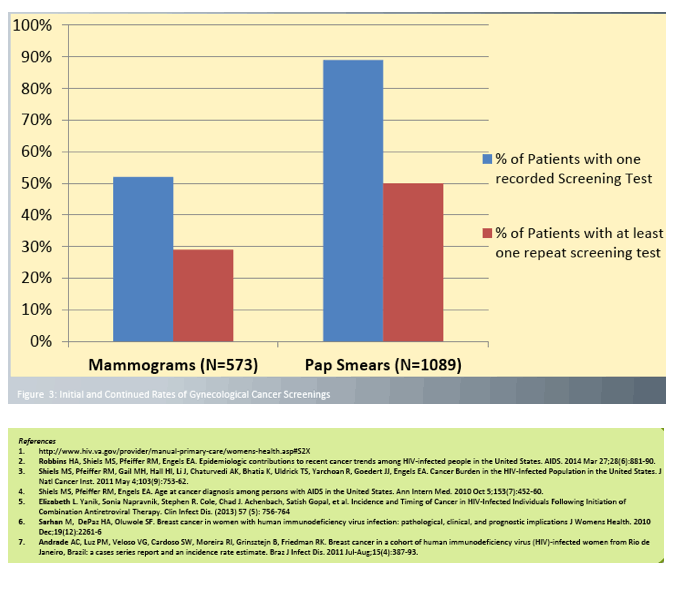
Among 1089 women seen at least twice as outpatients, 89% had at least one recorded Pap smear for cervical cancer and 50% had at least one additional Pap smear screening. Among 573 women over 50 years old, 52% had at least one mammogram, but only 29% had at least one more mammogram during the study period.
Among the 13 women with breast cancer, 4 got diagnosed before age 40, another 4 were diagnosed with screening mammograms, and the remaining 5 did not get screened and got diagnosed with masses. Age at breast cancer diagnosis averaged 44 and ranged from 24 to 60. More than half of breast cancer cases (54%) were stage 2 or later. None of these HIV-positive women diagnosed with breast cancer had a family history of breast cancer or prior chest radiation. Three women with breast cancer had anal dysplasia, and 1 of these also had cervical cancer. Six of 13 women with breast cancer had a recent history of alcohol abuse.
Despite the young age at breast cancer diagnosis in these women, the Rutgers teams observed that younger age at diagnosis did not correlate with more aggressive cancers or worse outcomes. "What is concerning," they added, "is that the average age in our general female HIV/AIDS population is only 50 and the average at diagnosis of breast cancer is 44." They also underlined the concern that the women diagnosed with breast cancer did not have traditional risk factors that would alert clinicians to screen more aggressively.
The researchers observed that their analysis is limited by the inability to determine if women received follow-up screening at other centers. Still, they believe their findings support "a need for measures to improve our patients' adherence to screening practices, re-evaluation of our current timeline for screening mammograms in our female HIV/AIDS population, and larger structural changes to the care provided in Newark related to cancer screenings." They suggested that clinicians could benefit from "a universal database" of cancer screening tests.
Reference
1. Mittal J, Nizami S, Tlamsa A, Kang M, Zucker J, Cennimo D. The incidence of gynecological cancers and evaluation of screening in female HIV/AIDS patients at university hospital. IDWeek 2015, October 7-11, San Diego. Abstract 1703. https://idsa.confex.com/idsa/2015/webprogram/Paper50741.html
2. Shiels MS, Pfeiffer RM, Gail MH, et al. Cancer burden in the HIV-infected population in the United States. J Natl Cancer Inst. 2011;103:753-762.


|
| |
|
 |
 |
|
|