 |
 |
 |
| |
Community-Acquired Pneumonia More Frequent With HIV in Veterans Cohort
|
| |
| |
IDWeek 2015, October 7-11, San Diego
Mark Mascolini
A significantly higher proportion of HIV-positive than negative US veterans in the Veterans Aging Cohort Study (VACS) had community-acquired pneumonia (CAP) identified by ICD-9 code in a 6500-person analysis [1]. Among veterans with chart-confirmed CAP, those with HIV were significantly younger than those without HIV.
CAP remains a frequent complication of HIV infection and could become more common as the HIV population ages. VACS researchers who conducted this study noted that research on CAP and other common comorbidities often relies on ICD-9 codes. Thus verifying and enhancing the reliability of ICD-9 codes has gained importance.
To address this issue VACS investigators compared reliability of ICD-9 codes for CAP compared with the gold standard of chart review in the VACS-8 cohort, a group of HIV-positive and negative veterans at 8 VACS sites. HIV-positive and negative veterans are site-matched by age, gender, and race. This analysis focused on 3257 HIV-positive and 3266 HIV-negative veterans enrolled in 2005-2008. The VACS team searched their records for inpatient ICD-9 codes consistent with bacterial or viral CAP. The researchers confirmed CAP on admission when their charts showed (1) symptoms, signs, or lab data, (2) radiologic findings, and (3) treatment with antibacterial drugs. Veterans who developed these indicators of pneumonia more than 48 hours after admission were determined to have health-care associated pneumonia (HCAP). The investigators calculated positive predictive value of ICD-9 codes for verified CAP as the number of chart review-confirmed pneumonias divided by the number of cases identified by specific ICD-9 codes.
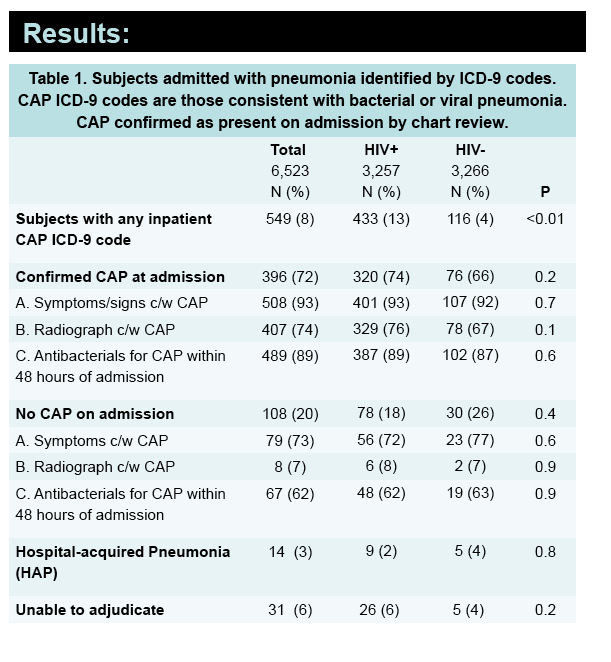
A significantly higher proportion of veterans with than without HIV had any inpatient CAP ICD-9 code (13% versus 4%, P < 0.01). Among the 433 HIV-positive veterans with a CAP ICD-9 code, 320 (74%) had CAP confirmed by chart review, as did 76 of 116 HIV-negative veterans (66%), and this difference was not significant (P = 0.2). The researchers identified HCAP in 2% of HIV-positive veterans and 4% of HIV-negative veterans, a nonsignificant difference (P = 0.8).
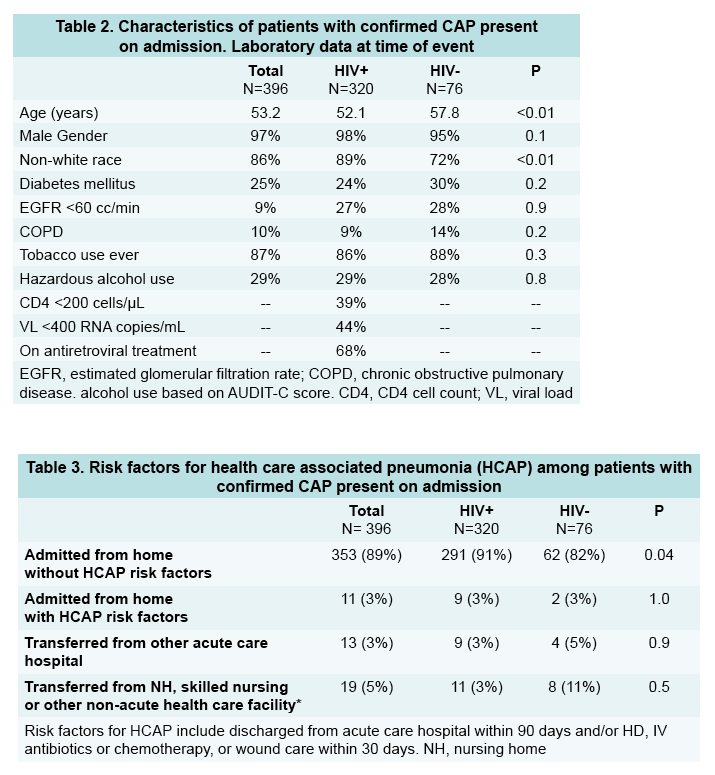
Among veterans with chart-confirmed CAP, those with HIV were significantly younger (52.1 versus 57.8, P < 0.01) and significantly more likely to be nonwhite (89% versus 72%, P < 0.01). Veterans with confirmed CAP and HIV did not differ from the HIV-negative confirmed-CAP group in gender or prevalence of diabetes, estimated glomerular filtration rate below 60, chronic obstructive pulmonary disease, tobacco use, or hazardous alcohol use. A significantly higher proportion of HIV-positive than negative veterans with confirmed CAP were admitted from home without HCAP risk factors (91% versus 82%, P = 0.04).
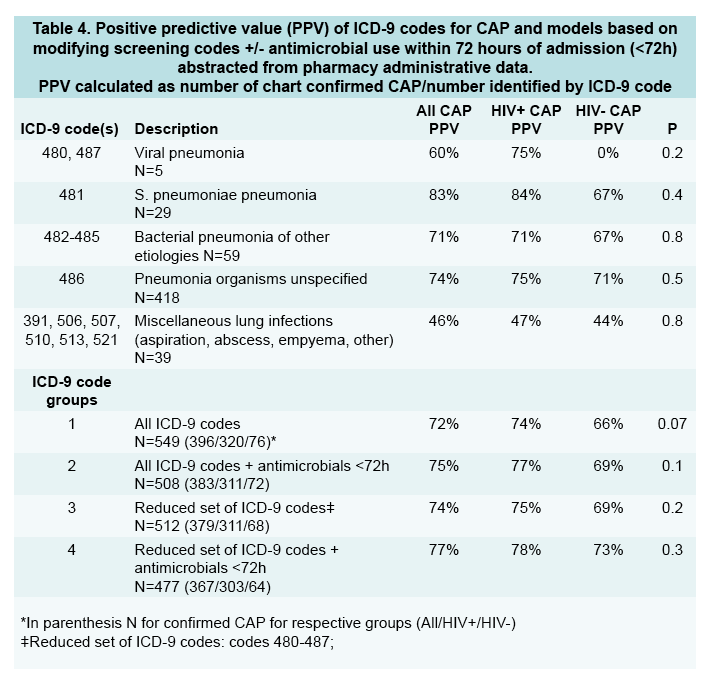
Positive predictive value of all ICD-9 codes for CAP was marginally higher in veterans with than without HIV (74% versus 66%, P = 0.07). For veterans with HIV, positive predictive value improved slightly when the researchers considered (1) all ICD-9 codes plus antimicrobial use within 72 hours of admission (77%), (2) a reduced set of ICD-9 codes (75%), or (3) a reduced set of ICD-9 codes plus antimicrobial use within 72 hours of admission (78%).
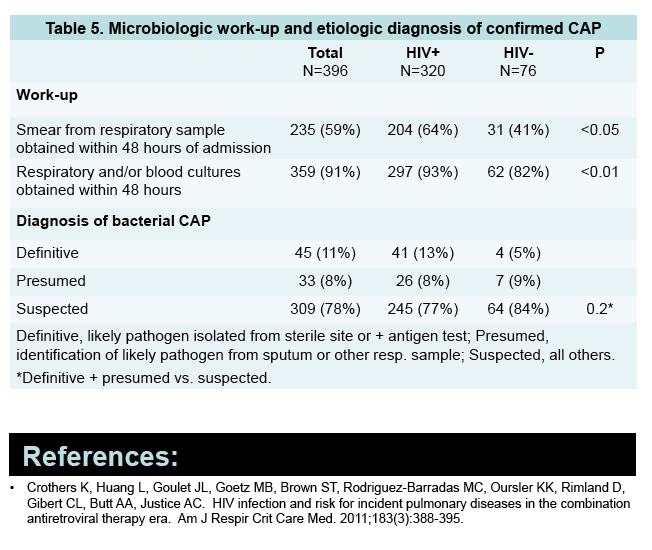
Among veterans with confirmed CAP, two microbiologic confirmatory findings were more frequent in veterans with than without HIV: smear from respiratory sample within 48 hours of admission (64% versus 41%, P < 0.05), and respiratory and/or blood cultures within 48 hours of admission (93% versus 82%, P < 0.01).
The researchers concluded that within the VA system, research results would not be significantly biased by HIV status. They proposed that an algorithm including radiologic findings could improve positive predictive value of ICD-9 codes for CAP. They stressed that, although significantly more veterans with HIV had samples sent for microbiologic evaluation, overall diagnostic yield proved low and did not differ significantly between veterans with and without HIV.
Reference
1. Rodriguez-Barradas MC, Akgun K, Brown S, et al. Community acquired pneumonia (CAP) requiring hospitalization in HIV infected and un-infected patients: evaluation of patients identified by ICD-9 codes. IDWeek 2015, October 7-11, San Diego. Abstract 1583.
----------------------
Reported by Jules Levin
Community Acquired Pneumonia (CAP) Requiring Hospitalization in HIV Infected (HIV+) and Un-infected (HIV-) Patients: Evaluation of Patients Identified by ICD-9 Codes
Maria C. Rodriguez-Barradas, MD1,, Kathleen Akgün, MD2,3, Sheldon T. Brown, MD4, Adeel A. Butt, MD5,6; Michael Fine, MD5; Matthew B. Goetz, M7; Christopher J. Graber, MD7; Laurence Huang, MD8, Kathleen A. McGinnis, DrPH, MS2; David Rimland, MD9; Amy Justice, MD2,3; and Kristina Crothers, MD10 1Michael E. DeBakey VAMC and Baylor College of Medicine, Houston, TX; 2VA Connecticut Healthcare System, West Haven, CT and 3Yale University, New Haven CT; 4James J Peters VAMC, Bronx, NY and Icahn School of Medicine at Mt. Sinai, NY, NY; 5VA Pittsburgh Healthcare System, Pittsburgh, PA and 6Hamad Healthcare Quality Institute, Doha, Qatar ; 7VA Greater Los Angeles Healthcare System, Los Angeles, CA; 8San Francisco General Hospital and University of California San Francisco, San Francisco, CA, 9VAMC and Emory University School of Medicine, Atlanta, GA; 10University of Washington, Seattle, WA.



|
| |
|
 |
 |
|
|