 |
 |
 |
| |
Under 3% With HIV Complete HPV Vaccine Series in Large Denver Survey
|
| |
| |
IDSA/IDWeek 2015, October 7-11, San Diego
Mark Mascolini
Fewer than 3% of HIV-positive adults in a large Denver public healthcare system completed the 3-shot human papillomavirus (HPV) vaccine series, compared with 13% of HIV-negative people [1]. Men were less likely than women to get all 3 doses.
HPV infection causes most cervical and anal cancers, noted University of Colorado and Denver Public Health researchers who conducted this study. And HPV-related disease is more prevalent and aggressive in people with HIV. HPV vaccines have proved safe and immunogenic in people with HIV, and US authorities recommend HPV vaccination for youngsters and young adults with HIV infection [2].
This retrospective cohort study involved HIV-positive and negative people eligible for HPV vaccination and in care at Denver Health. The analysis focused on people who made a primary care visit within an 18-month period from 2006 through 2014 for women and from 2011 through 2014 for men. Among adults, women 18 to 26 are eligible for HPV vaccination, as are HIV-positive men 18 to 26 and HIV-negative men 18 to 21. The researchers also conducted a cross-sectional Web-based survey of healthcare providers seeing HIV-positive people at 4 major Denver clinics.
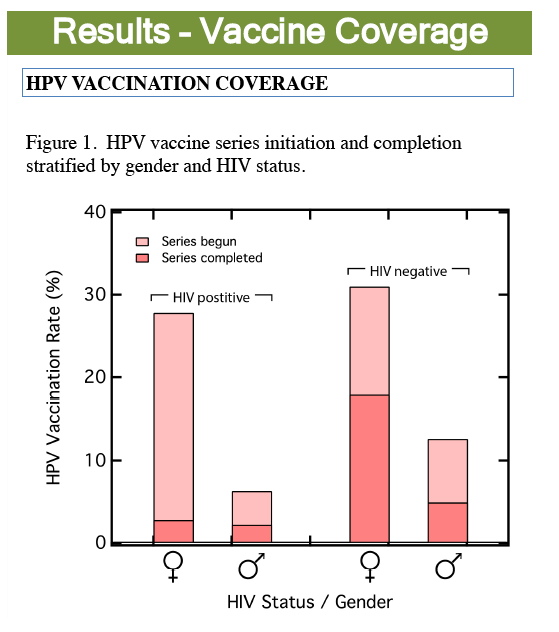
The study included 304 young adults with HIV and 54,298 without HIV. Overall 8.9% of HIV-positive people and 24.3% of HIV negative people began the HPV vaccine series. Only 2.3% with HIV and 13.2% without HIV completed the 3-shot series, a significant difference (P < 0.001). Among people with HIV, a higher proportion of women than men started the vaccine course (27.8% versus 6.3%), but similar proportions of women and men completed the series (2.8% and 2.2%). Among HIV-negative people, 31% of women and 12.5% of men started the HPV vaccine series, while 17.9% and 4.9% completed the course. Overall, men were significantly less likely than women to get the 3 HPV vaccine injections (P = 0.03).
More than 75% of providers responded to the survey, which found that 56% strongly agreed and 19% somewhat agreed that they recommend HPV vaccination to all eligible people with HIV. But half said they do not routinely assess HPV vaccination status in their HIV patients. Almost all clinicians (91%) believed HPV vaccines are effective in HIV-positive people. And most strongly agreed (38%) or somewhat agreed (41%) that most HIV-positive people have already been exposed to HIV.
The most frequently perceived barriers to HPV vaccination in people with HIV were difficulty ensuring that patients will complete the 3-dose series (53%), lack of adequate reimbursement (44%), and inability to verify whether patients have already been vaccinated (44%). A large minority of clinicians (41%) said their clinic does not have enough vaccine-eligible patients to make it worthwhile to offer the vaccine or they "don't have enough time to think about the HPV vaccine due to other clinical issues that take precedent."
The Denver team encouraged greater HPV vaccination coverage through (1) increased vaccine availability in clinics, (2) education of providers about HPV vaccine safety and efficacy in people with HIV, (3) automatic reminder programs that encourage patients to complete the vaccine series, and (4) increased clinic use of available immunization registries "to facilitate information sharing of patient vaccination."
References
1. Marx GE, Daley MF, Burman WJ, Shlay JC. Low human papillomavirus vaccination coverage in HIV-positive patients in Denver, Colorado. IDWeek 2015, October 7-11, San Diego. Abstract 1699. https://idsa.confex.com/idsa/2015/webprogram/Paper53150.html
2. Centers for Disease Control and Prevention. HIV infection and adult vaccination. http://www.cdc.gov/vaccines/adults/rec-vac/health-conditions/hiv.html
--------------------------
Reported by Jules Levin









|
| |
|
 |
 |
|
|