 |
 |
 |
| |
Behavioral and Clinical Factors Among HIV-infected Women in Care ≥ Age 50 Years - United States, 2009-2011 ..... 37.5% >50 years of age....60-62% Black
|
| |
| |
Reported b Jules Levin
IDSA 2015 Oct 7-11 San Diego, CA
Maggie W. Collison1, 2, Emma L. Frazier2, Ann Do2, Madeline Y. Sutton2
1Michigan State University 2Division of HIV/AIDS Prevention, Centers for Disease Control and Prevention
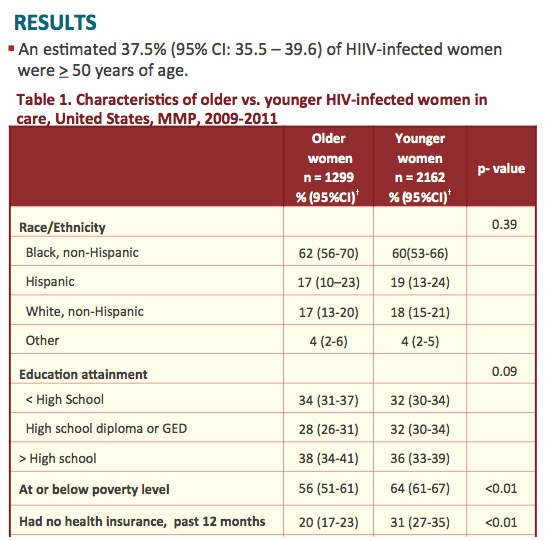
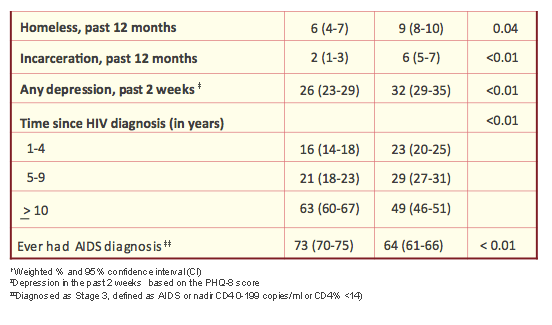
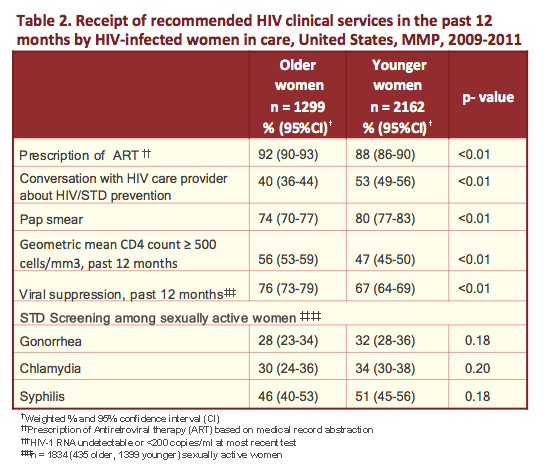
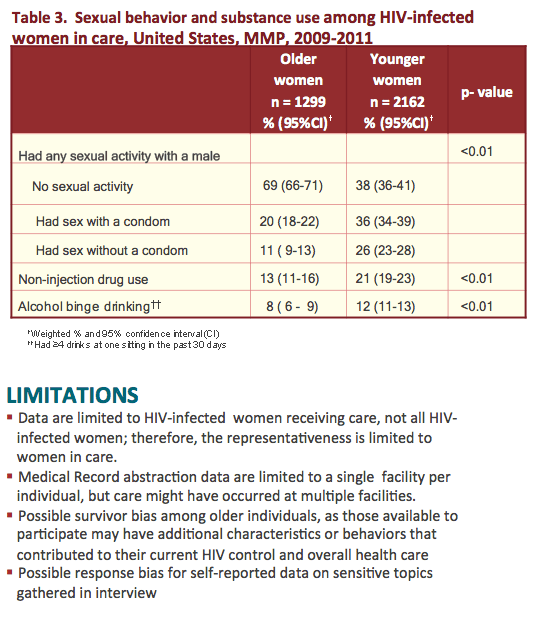
from Jules: some noteworthy study findings - 26% of older women & 32% of younger women reported any depression in the past 2 weeks; 20% of older women (>50) had no health insurance vs 31% who were <50; 6% of older women were homeless vs 9% of younger women; 34% of older & 32% of younger have less than a high school diploma; 56% of older & 61% of younger women are at or below the poverty line; 73% of older & 64% of younger ever had an AIDS diagnosis; 69% of older & 38% of younger report no sexual activity; 11% of older & 26% of younger reported sex without a condom; 8% of older & 12% of younger reported alcohol binge drinking (4 or more drinks at 1 sitting in last 30 days). Take a look at Table 2 as results reported regarding STD & clinical services are remarkable: rates among sexually active women of gonorrhea, chlamydia & syphilis are 28-32%, 30-34%, and 46-51%, respectively.
Program Abstract
Background: CDC estimates that persons aged ≥ 50 years will comprise 50% of persons living with HIV in the United States by 2020. Women comprise 20% of persons living with HIV, yet little is known about how older HIV-infected women compare with younger women. Our goals were to describe characteristics of a sample of HIV-infected women in care aged ≥ 50 years in order to inform and improve HIV prevention and care efforts for older women.
Methods: We used matched interview and medical record abstraction data from the 2009, 2010, and 2011 data collection cycles of the Medical Monitoring Project (MMP), which collected cross-sectional data annually from a representative sample of HIV-positive adults in care. We included women diagnosed at least one year prior to interview and stratified the analysis by age groups (< 50 vs. ≥ 50 years). We examined selected demographic, behavioral and clinical characteristics. Bivariate analyses were completed using chi-square analysis.
Results: The characteristics of the 3,461 women included in this analysis were as follows: 2,084 (61%) non-Hispanic Black, 1,299 (37.5%) aged ≥ 50 years, median years since HIV diagnosis 10.8 (IQR 5.86 - 16.1). Compared with women age < 50 years, women ≥ 50 were less likely to be at or below poverty (55.9% vs 64.0%; p < 0.003), to report sex without a condom with a male partner (11.1% vs 25.6%; p < 0.0001), to report any drug use (13.3% vs 20.9%; p < 0.0001), and to report symptoms consistent with major depression (12.5% vs 16.6%; p < 0.001). However, women age ≥ 50 years were more likely to be prescribed antiretroviral therapy (91.6% vs 87.8%; p < 0.004) and to have had the most recent viral load <200 copies per mL (75.8% vs 66.8%; p < 0.001). Among women reporting sexual activity in the previous 12 months, there were no significant differences in medically documented screening rates for gonorrhea (28.2% vs 32.1%, p > 0.05) or chlamydia (30.3% vs 33.9%, p > 0.05).
Conclusion: Older HIV-infected women comprise more than one-third of HIV-infected women in care. Although our sample of women are engaged in HIV clinical care, there remain some opportunities to strengthen routine gonorrhea and chlamydia screenings among all sexually active HIV-infected women, including older women of whom >10% reported sex without a condom.



|
| |
|
 |
 |
|
|