 |
 |
 |
| |
Summary for AASLD 2016 for Hepatitis C - New HCV two and three drug regimens on their way: what do they promise? And what do clinicians need to look out for under DAA combination therapy and beyond SVR?
|
| |
| |
New HCV three drug regimens on their way: what do they promise? And what do clinicians need to look out for under DAA combination therapy and beyond SVR?
Jürgen K. Rockstroh M.D., Professor of Medicine
University of Bonn, Germany
Correspondence:
Prof. Dr. J.K. Rockstroh
Department of Medicine I
University of Bonn
Sigmund-Freud-Str. 25
53105 Bonn
Germany
Introduction
At present, besides the Abbvie 3-D regimen, mostly dual hepatitis C (HCV) direct acting antiviral (DAA) combinations which are coformulated as single tablet regimens have become the gold standard for first line treatment of all HCV genotypes. Despite SVR rates on average above 95% there are still attempts in the field to develop three drug combinations (so called triplets) or very potent new dual regimens which may allow shortening of treatment duration and may also add to the antiviral pangenotypic activity of all oral DAA combination therapy. Obviously, even with the currently licensed HCV drugs, three drug combinations may play a role in retreatment of the few patients which experience virological failure under dual DAA-based HCV therapy. Various studies at AASLD this year where devoted to effectiveness and safety of these new three DAA regimens in treatment naïve as well as treatment experienced patients including prior DAA-based treatment failure (1-7). In addition, data on the new and very potent Abbvie dual combination (Glecaprevir (ABT-493)/Pibrentasvir (ABT-530)), again in treatment-naïve, experienced- and prior DAA-failures, was presented (8-10). Another important topic was feedback on safety and effectiveness of various all oral DAA combinations from real-world cohorts including a whole variety of special populations including intravenous drug users, patients on opioid substitution therapy, patients in the prison setting, HIV coinfected, patients with renal insufficiency, patients older than 70 years, patients receiving short treatment durations of 8 week and much more (11-19). As more and more data arises from very diverse patient populations it appears as if no special or hard to treat patient group seems to exist any longer. In the end it really is more about getting access to therapy feasible for some of those more marginalized patient groups. A further important topic was around clinically relevant issues which clinicians who treat HCV need to be aware of, including risk for hepatitis B (HBV) reactivation after starting DAA therapy, as well as the risk for development of hepatocellular cancer (HCC) after achieving SVR (20-24). Although HCV remained to be a widely recognized topic throughout AASLD, it is becoming apparent that other topics in hepatology including NASH, alcoholic hepatitis, hepatitis B, HCC and primary biliary cholangitis are gaining importance and presentation space especially in the late-breaker session. A more intensified discussion on national HCV screening programs, HCV treatment uptake and linkage to care at AASLD would be desirable to politically underline the need to continue the fight to ensure global access of HCV therapies throughout the world.
Risk of HBV reactivation after starting DAA therapy
More recently, the FDA has issued a Drug Safety Communication: which warns about the risk of hepatitis B reactivating in some patients treated with direct-acting antivirals for hepatitis C. The detailed data of the HBV reactivation cases collected by the FDA until now were presented as a late breaker poster at AASLD (20). Overall, 29 cases were collected globally. Relevant clinical and laboratory information was unfortunately not available for all patient cases which limit the interpretation. Table 1 summarizes the main available baseline characteristics of the 29 reported patient cases. Of note the median time to occurrence of HBV reactivation was 46 days underlining that HBV reactivation can occur early after starting DAA therapy and that monitoring of liver enzymes during DAA therapy will be of importance in patients at risk Also the clinical outcome with two deaths, one liver transplantation and six hospitalizations suggests that HBV reactivation is associated with significant morbidity and mortality. However, it needs to be stressed that HBV reactivation appears to be a very rare event and indeed has not be found or reported in many real-life cohorts so far.
Table 1: HBV Reactivation Associated with DAA Therapy for HCV: A Review of US FDA Spontaneous Post-Marketing Cases: Baseline characteristics

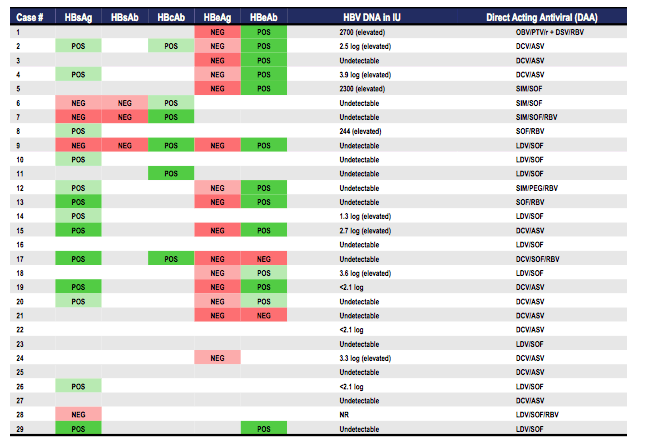
HBV reactivation was seen for different HCV genotypes and various DAA combinations, so clearly no drug specific risk exists but rather a general risk for HBV reactivation under DAA therapy. Figure 1 shows in more detail the baseline HCV/HBV virological characteristics of the HBV reactivation cases as well as the respective DAA drug combinations used. Of note most patients with HBV reactivation were patients with known chronic HBV infection and a positive HBs-Ag (see figure 1). It is important to remember that HBV screening in general has been recommended in HCV patients by most guidelines and that a risk of reactivation already existed in the IFN-era in patients with a positive HBs-Ag. Some of the cases (n=3) however, only had anti-HBc antibodies positive as a sign of past HBV infection but then also developed HBV reactivation. All three subjects were undetectable for HBV-DNA at baseline making occult HBV infection unlikely (see figure 1). This implies that patients with anti-HBc should also be monitored more closely.
Figure 1: A Review of US FDA Spontaneous Post-Marketing Cases:
Baseline HCV/HBV Virological Characteristics and DAA Used
In an additional poster HBV reactivation rates were compared under/after IFN based therapy versus all oral DAA HCV therapy in HCV/HBV coinfected subjects and found no difference in HBV reactivation rates between the two treatment groups (limitation is low number of DAA treated patients: 148 versus 1037) (21). Clinically relevant development of hepatitis however, was more likely in the DAA treated group and also HBV reactivation occurred much earlier in patients treated with DAAs than those treated with interferon. As interferon is also used for HBV therapy and can suppress HBV2 replication this makes perfect sense.
AASLD: Hepatitis B Reactivation Associated with Direct Acting Antiviral Therapy for Hepatitis C: A review of Spontaneous Post-Marketing Cases - (12/06/16)
Surveillance for hepatocellular carcinoma (HCC) and risk for HCC after achieving SVR following DAA therapy.
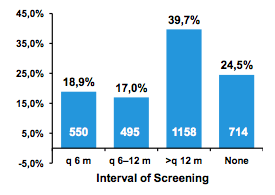
Currently, there is an ongoing controversial discussion about a potentially increased risk for HCC after DAA combination therapy. This hot topic was addressed in several studies presented at AASLD (23,24). Noteworthy, there were also several studies which addressed HCC surveillance in a broader sense (22). In a retrospective cohort study of 2,376 consecutive chronic hepatitis C (CHC) patients with cirrhosis, patients were monitored for > 1 year at a University medical center between 1998 and 2015 (22). The median follow-up was 45.4 months (range: 12-231). The adherence to HCC screening is shown in figure 2 and shows very poor surveillance rates which emphasize the educational need to remind HCV treaters that after SVR particularly in previous cirrhotics there needs to be 6-monthly screening for HCC. Within this study patients with more frequent surveillance were diagnosed with earlier staged HCC than patients with less frequent monitoring. Clearly, further efforts are needed to improve adherence to HCC surveillance in CHC patient with cirrhosis.
Figure 2: Adherence rates to HCC surveillance in HCV infected cirrhotics
AASLD: Poor Adherence to Hepatocellular Carcinoma (HCC) Surveillance in a U.S. Cohort of 2,917 Patients with Chronic Hepatitis C (CHC) and Cirrhosis - (11/28/16)
Probably the largest study on the association of treatment completion with the DAA sofosbuvir (SOF) with risk of incident liver cancer in real-world data was presented from Gilead (23). The study included adult HCV patients who had at least 12 weeks of SOF-containing therapy dispensed and who had no evidence of subsequent other HCV treatment (N=9616) (from US administrative claim data). For comparison, adult patients diagnosed with HCV without evidence of HCV treatment who had active follow-up time after SOF approval (N=95274) were identified. All included patients had a minimum of 6 months of enrollment and no evidence of prior liver cancer at baseline. The baseline characteristics for the two groups are shown below in table 2.
Table 2: Characteristics of SOF-treated HCV and untreated HCV cohorts
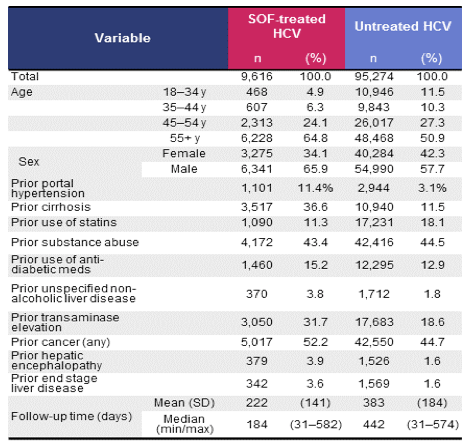
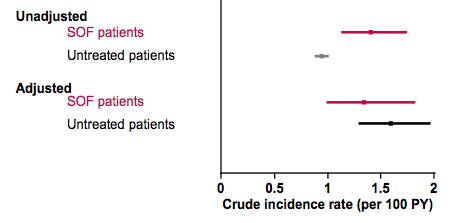
Of note, patients who received sofosbuvir containing HCV therapy were older, more likely to be male, more likely to already have developed cirrhosis and/or portal hypertension. As these baseline characteristics may impact risk for HCC development it is important to adjust for these factors. Figure 3 shows the cumulative incidence rates of HCC in each cohort, before and after adjustment for co-variants. Before adjustment for significant covariates, HCC incidence appears higher in SOF-treated patients vs. untreated patients. After adjustment for significant covariates, rates in SOF-treated patients are not higher; indeed, they are nominally lower than rates among untreated patients.
Figure 3: Cumulative incidence rates of HCC for SOF treated patients as well as for untreated patients, before and after adjustment for co-variants.
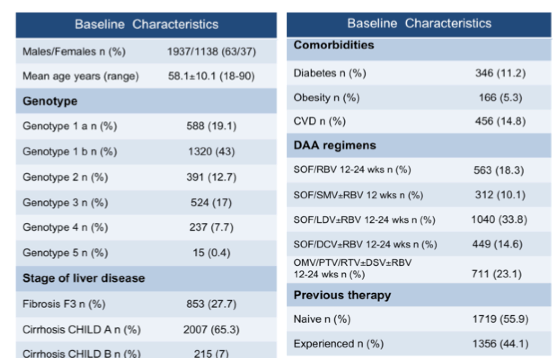
A further interesting oral presentation at AASLD from Italy studied incidence and pattern of "de novo" hepatocellular carcinoma in HCV patients with advanced liver disease treated with oral DAAs (24). Overall 3075 patients were included with a mean follow-up of 300.8 ± 100 days after initiation of DAAs. Patients with a past history of HCC were excluded. The patients were treated with approved DAAs regimens and monitored monthly. The baseline characteristics of the cohort are shown in table 3.
Table 3: Baseline characteristics of an Italian cohort treated with DAAs
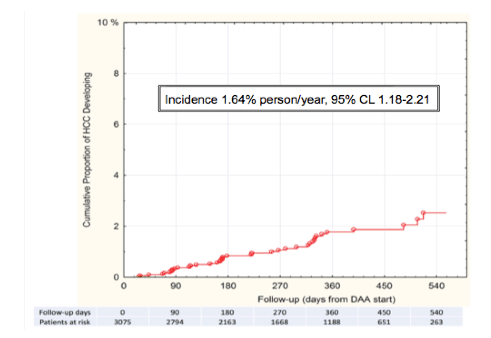
Clearly, this was a predominantly cirrhotic patient population with increased risk for development of HCC. 56% of patients were HCV treatment naïve. During the observation period 41 patients developed HCC, and the overall calculated incidence x100 patient-years was 1.64 (95% CI : 1.18-2.21) (see figure 4). Interestingly, this was even somewhat lower than has been reported from natural history studies in untreated HCV patients with cirrhosis where annual incidence rates were between 2-8 and 3.9% respectively (25,26).
Figure 4: Cumulative proportion of HCC in the studied cohort (Kaplan-Meier)
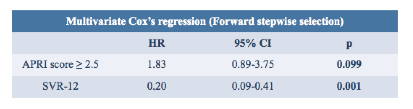
HCC incidence in cirrhotics was then analyzed by subgroups (see table 4). Variables included into the multivariate analysis were gender, HCV genotype, APRI score, Child Pugh stage, DAA regimen and SVR12. The best baseline predictor of the HCC risk was APRI (see table 4).
Table 4: HCC incidence in cirrhotics by subgroups (multivariate analysis
Patterns of HCC development in relation to timing of DAA therapy were also investigated and are shown in detail in figure 5.
Figure 5: Patterns of HCC development in relation to timing of DAA therapy
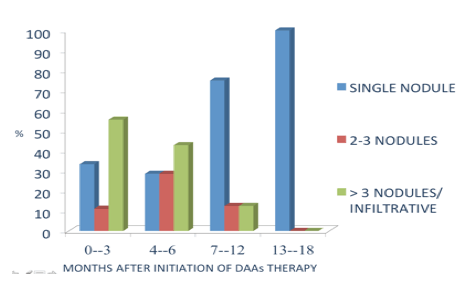
Of note several HCC cases were noted very shortly after initiating DAA therapy suggesting that they already had been present upon start of DAA therapy and may have been missed by prior screening efforts. Also several HCC were described as presenting with multiple nodules and being infiltrative suggestive of more aggressive disease forms. The atypical HCC patterns seen in about half of the cases deserve better understanding.
AASLD: "Incidence and pattern of "de novo" hepatocellular carcinoma in HCV patients treated with oral DAAs" - (11/17/16)
Various special patient populations from real-life cohorts
Intravenous drug users and patients on opioid substitution therapy
People who inject drugs (PWID) are the driving force of chronic hepatitis C (CHC) in the western world, but treatment uptake has been low in this often marginalized patient population. Shortened treatment durations appear particularly attractive in this patient group where adherence always has been a challenge. In this study from Denmark investigators hypothesized that maintaining ribavirin (RBV) in a 4 week DAA regimen and adding pegylated-interferon 2 alpha (PEG 2a) could give high cure rates in drug users (11). The study was conducted at one drug treatment center. Thirty-two patients were randomized 1:1 to either
LDV/SOF+RBV or LDV/SOF/RBV+PEG 2a for 4 weeks. RBV was dosed weight based and PEG 2a at 180 ug weekly. Main inclusion criteria: Treatment naïve patient with CHC (all genotypes), in opium substitution therapy (OST), age< 50 years, weight<100 kg, viral load<2mill IU/ml and liver stiffness measure (LSM)< 8 kPa. Subjects were allowed any kind of concomitant drug or alcohol use but should be compliant to their OST program. Primary endpoint was sustained virological response at week 12 after end of treatment (SVR 12) in the intention to treat (ITT) population. The baseline characteristics of the two study groups are shown in table 5.
Table 5: Baseline characteristics
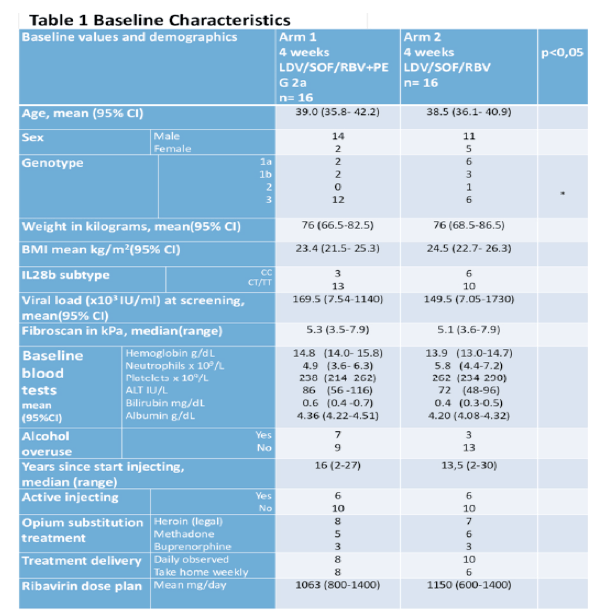
Of note over 50% of the study participants had a HCV genotype 3 where IFN sensitivity can be expected to be high whereas ledipasvir has little GT3 activity. More than half of the study subjects were on heroin substitution therapy. All patients had no advanced fibrosis. The SVR12 results of this pilot study are shown in figure 6.
Figure 6: SVR12 results (Intent-to-treat analysis)
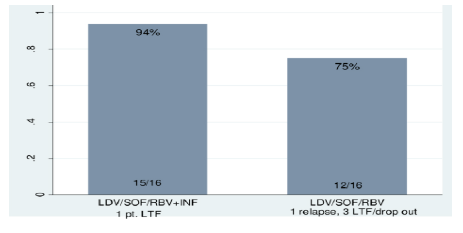
In summary, 4 weeks of sofosbuvir, ledipasvir and ribavirin with or without interferon was highly effective in curing CHC in this hard to reach but easy to treat population of non-cirrhotic drug users on OST with only one virological relapse detected in an adherent patient. Clearly, the numbers are too small to generalize findings but at least it appears that in non-cirrhotic patients this may be an interesting treatment alternative when treatment duration is of concern.
Patients in the prison setting
Chronic HCV is highly prevalent in the Department of Corrections (DOC). HCV treatment in this setting would allow eliminating HCV and preventing continued transmission. In this study SVR12 rates were compared in the Virginia DOC through telemedicine to HCV patients in the privately-insured and indigent clinics treated with Ledipasvir/Sofosbuvir (12). DOC pts were evaluated via telemedicine for disease severity and appropriateness for therapy following AASLD-IDSA Guidelines. Those with decompensated cirrhosis, significant co-morbidities, or those with less than 9 months on their sentence were excluded. The baseline characteristics for the three groups (Department of Correction (DOC), private clinic and indigent clinic) are depicted below in table 6.
Table 6: Baseline characteristics
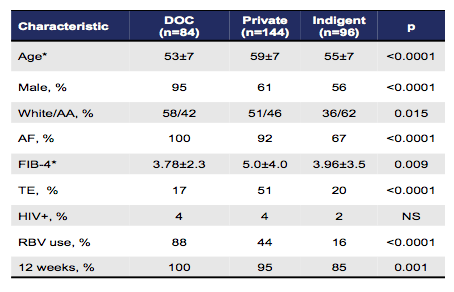
*mean, ±SD
Of note, patients in the DOC were younger, more likely to be white, have advanced fibrosis (AF), receive ribavirin and 12 weeks of DAA therapy. The SVR12 rates obtained for the three groups are shown in figure 7.
Figure 7: Results: SVR12 rates
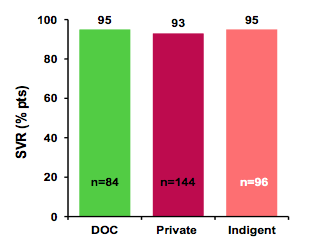
Multivariate analysis identified FIB-4 (p<.0001) and RBV use (p=.028) as predictors of SVR-12 while demographics, treatment duration, prior treatment and HIV status, or patient population were not associated with SVR-12. In conclusion treatment of HCV in the DOC by telemedicine with DAA is not only feasible, but has a very high SVR12. The higher SVR12 in the DOC compared to the cure rates in the private clinic setting may be due to directly observed therapy or differences in patient characteristics.
HIV/HCV coinfected patients
Several HIV coinfection real-life cohorts looked at overall safety and efficacy of DAA-based HCV therapy in this particular patient group. At EASL a researcher group from Seville, Spain had claimed lower HCV cure rates in HIV-coinfected versus HCV monoinfected patients (95 vs 98%, respectively) (27). Therefore, the German Hepatitis C-Registry compared SVR12 rates between HIV/HCV co-infected and HCV mono-infected subjects (16). Overall, 488 HIV/HCV coinfected and 5,657 HCV mono infected subjects were included into this analysis. The baseline characteristics are shown below in table 7.
Table 7: National German HCV Cohort Study: Baseline characteristics
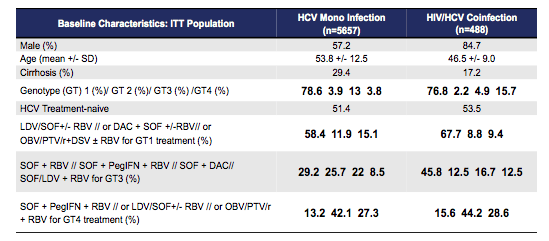
Of note cirrhosis was less frequent in the HIV-coinfected patient group (was just the other way around in the Spanish study from EASL) and much more males were also found in the coinfected group. The SVR12 rates by HCV-genotype and respective treatment group are depicted below in figure 8.
Figure 8: Results: SVR12 rates by HCV-genotype and treatment group (ITT analysis)
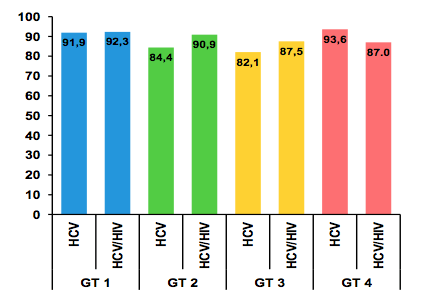
No significant difference in overall SVR rates was observed between the two treatment groups. This was also true for the subgroup of cirrhotics only (see figure 9).
Figure 9: Cirrhotics per treatment group (ITT analysis)
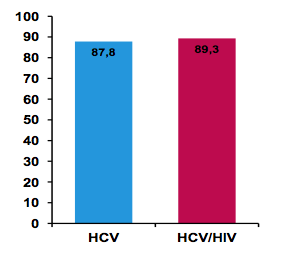
In conclusion, this analysis from a large national real-life patient cohort finds no difference in HCV cure rates between HIV/HCV and HCV mono-infected patients and therefore supports current HCV guidelines which no longer see a need to consider HIV co-infected individuals as a special patient population.
These findings are also supported by a large analysis presented by Dr. Naggie who compared SVR rates form clinical coinfection trials to outcome data reported from real world cohorts (see figure 10) (15).
Figure 10: Clinical Trials Compared to Real-World Cohorts: SVR12 in GT 1 HIV/HCV Co-infected Patients on LDV/SOF for 12-24 Weeks.
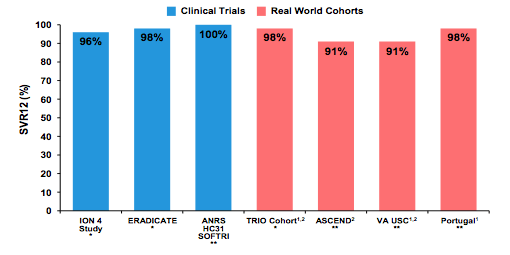
More data presented at AASLD from coinfection cohorts comes from Madrid (16). Therapeutic outcomes were evaluated in a prospective registry of HIV/HCV-coinfected patients receiving direct-acting antiviral agents (DAA)-based HCV therapy (Rx). This so called Madrid-CoRe is a prospective registry of all coinfected adults undergoing DAA Rx in Hospitals from the Madrid Regional Health Service. HCV virologic responses were assessed at 12 and 24 weeks after completion of Rx (SVR). HCV relapse was defined as a rebound of HCV-RNA after the end of Rx. The baseline characteristics are shown below in table 8.
Table 8: Baseline characteristics
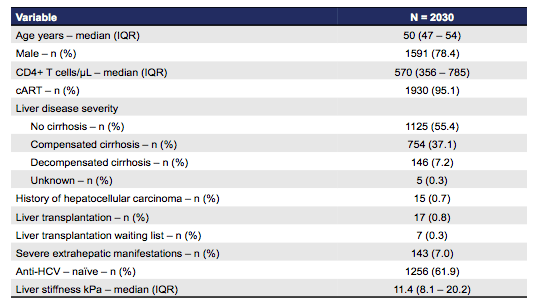
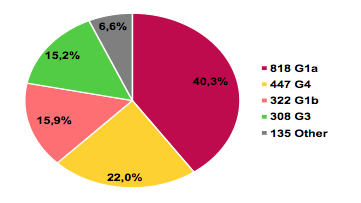
The baseline characteristics clearly show that near to 50% of patients already had cirrhosis which is clearly much higher than what has been studied on average in clinical trials. 627 (30.9%) of patients received ribavirin. The most commonly used DAA therapy was SOF/LDV in n=1279 patients followed by SOS + DAC in 300 subjects. The HCV genotype distribution is shown in figure 11
Figure 11 HCV genotype distribution
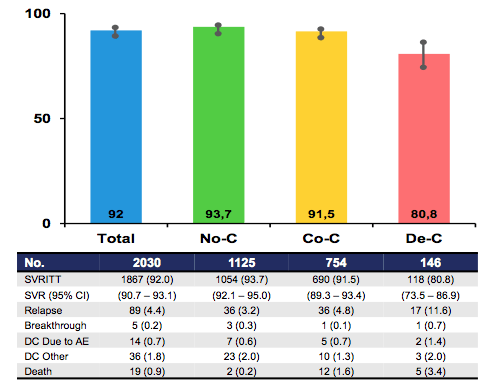
Treatment response by stage of liver disease is depicted in figure 12. The lowest SVR rate of only 80.8% was observed in patients with decompensated cirrhosis highlighting that this remains a difficult to treat patient group. Also recorded deaths, as well as treatment discontinuations due to adverse events were numerically higher in this challenging patient group. In contrast SVR rates were above 93% in non-cirrhotic patients clearly emphasizing the advantages of early treatment.
Figure 12: Madrid-CoRe: Treatment Outcomes by Severity of Liver-Disease: No-C = no cirrhosis, Co-C = compensated cirrhosis, De-C = decompensated cirrhosis
AASLD: Real World Effectiveness of Ledipasvir/Sofosbuvir in Patients Coinfected With HCV and HIV-1:A Comparative Analysis of Clinical Trials with Four Real World Cohorts - (11/14/16)
AASLD: Real-world Outcomes With New HCV Antivirals in HIV/HCV-coinfected Subjects:Madrid Coinfection Registry (Madrid-CoRE) Findings - (11/30/16)
EASL: HIV Coinfection Impairs the Response to DAA-based HCV Therapy - (05/09/16)
Patients with renal insufficiency or on hemodialysis
Exciting new data was presented on the Glecaprevir (GLE, formerly ABT-493; activity against HCV NS3/4A) and pibrentasvir (PIB, formerly ABT-530; activity against NS5A,) combination. Neither compound undergoes significant renal excretion which makes them potentially suitable for patients with renal disease. Phase 1 studies demonstrated no clinically relevant increases in the exposure of GLE/PIB in patients with renal disease compared to those with normal renal function. At AASLD for the first time results from the EXPEDITION-IV study were presented which evaluated the safety and efficacy of GLE/PIB administered for 12 weeks in GT1-GT6 HCV-infected patients with severe renal impairment (17). The study design is shown below in figure 13. As the DAAs recommended to date for treatment of HCV in patients with advanced renal insufficiency are only active predominantly in HCV GT 1 and 4 there remains a need for new active HCV regimens particularly for HCV GT 2 and 3 patients with end-stage renal disease. The pangenotypic activity of G/P may be promising in this regard.
Figure 13: EXPEDITION-IV Study Design
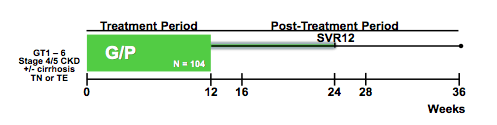
Primary endpoint was SVR12 defined as HCV RNA below the lower limit of quantification (LLOQ; 15 IU/mL). Baseline characteristics are summarized in table 7.
Table 9: EXPEDTION-IV Baseline characteristics
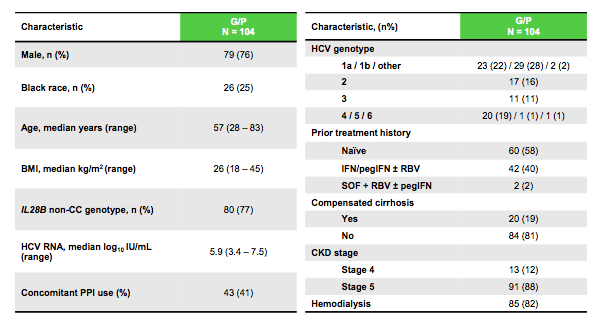
Of note the majority of patients included (82%) was already on hemodialysis. A fifth already had cirrhosis and 42% had previously failed mostly on an IFN-containing HCV regimen. The SVR12 rates are shown below in figure 14.
Figure 14: EXPEDITION-IV: Results - SVR12
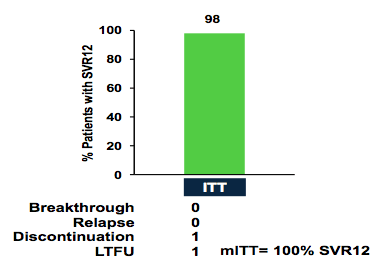
An amazing 100% of patients were cured in the modified ITT analysis underlining the potency of this regimen throughout all genotypes. Clearly the numbers for some of the genotypes were small but the data strongly encourages collecting more data on this regimen in patients with renal insufficiency and HCV GT2 or 3 infection.
AASLD: EXPEDITION-4: EFFICACY AND SAFETY OF GLECAPREVIR/PIBRENTASVIR (ABT-493/ABT-530) IN PATIENTS WITH RENAL IMPAIRMENT AND CHRONIC HEPATITIS C VIRUS GENOTYPE 1 - 6 INFECTION - (11/15/16)
Patients older than 70 years
Few registrational trials reported outcomes of novel direct-acting antiviral (DAA) therapies in elderly patients. Within the German hepatitis- C registry (DHC-R) investigators evaluated the effectiveness and safety of all-oral DAA regimen in patients >70 yrs. of age vs. younger patients (≤70 yrs.) (18). This data analysis is based on 8090 patients who started antiviral HCV treatment on or before 30 Sep 2015. Of 7133 patients who started all-oral DAA combination treatments, 686 (9.6%) were > 70 years of age. Patients from the elderly group were more likely to have a HCV genotype 1b infection (79% vs 37.8%, respectively). 51% of the patients > 70 were treatment experienced and 44% already had liver cirrhosis. The SVR12 rates per protocol were similar in patients >70 years of age compared to younger patients. However, only few elderly patients were infected with HCV GT 3- 6. Figure 15 summarizes the SVR12 rates by genotype and regimen used for the two age groups. Lower response rates were seen for the sofosbuvir and ribavirin combination but high cure rates independent of age group were obtained for all oral DAA combinations in particular for GT 1a and 1b.
Figure 15: SVR12 rates by age group, GT, cirrhosis state and HCV DAA regimen used
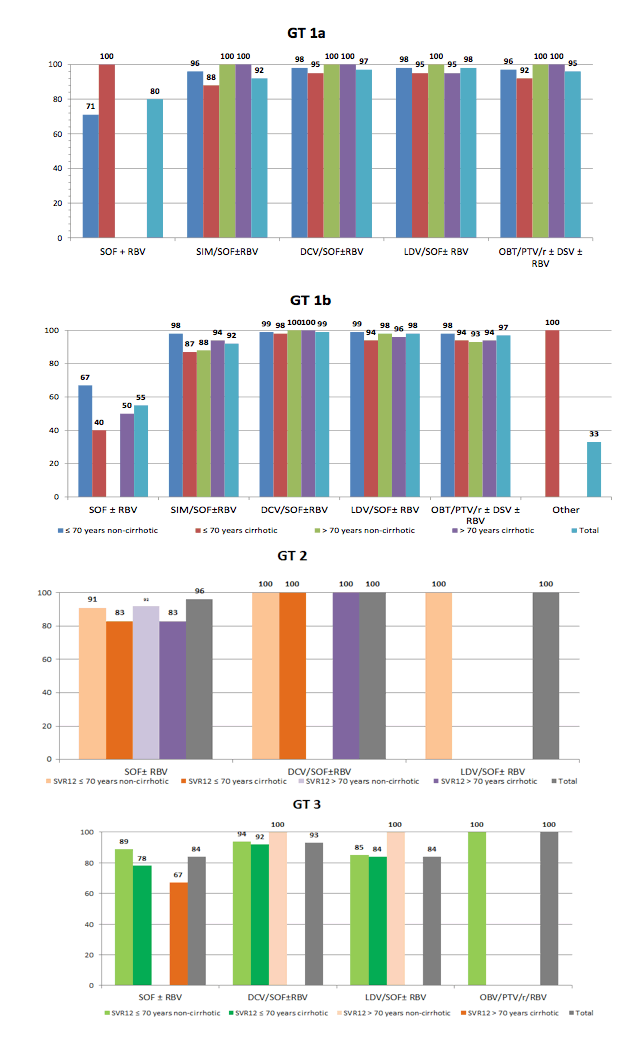
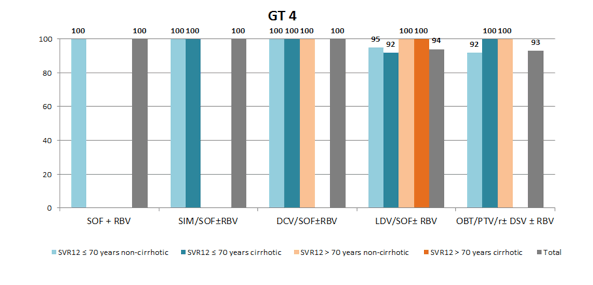
Patients receiving short treatment durations of 8 week
A post-hoc analysis of the ION-3 registrational trial indicated that 8 weeks of treatment with LDV/SOF is effective in selected patients with genotype 1 chronic HCV. Therefore in the German label treatment of 8 weeks can be considered in treatment naïve HCV genotype 1 patient without cirrhosis and an HCV viral load below 6 Mill I.E./ml. Indeed, several real-world cohort studies by now have also suggested that SVR rates with an 8-week regimen are comparable to a 12 week course. A controversy remains though around this issue where the ASSLD guidelines do not recommend shorter treatment durations in patients with HIV coinfection whereas some European guidelines do. Using individual patient data from multiple real world cohorts, an analysis was presented at AASLD which aimed at determining the effectiveness of 8 weeks of treatment, to examine variables associated with relapse and to compare the efficacy of 8 weeks with 12 weeks of therapy (19). The primary analysis used pooled data from non-cirrhotic patients from the HCVTRIO, IFI, Temple University/Burman's pharmacy, and Kaiser Permanente Southern California cohorts. All patients had fibrosis staging through biopsy, transient elastography, or fibrosure test. Exact logistic regression was used to determine predictors of relapse. The secondary analysis was a systematic review and meta-analysis of additional real world cohorts to compare the effectiveness of an 8 and 12 week course. Overall, 5,637 cases were included into the analysis. The per protocol SVR12 rates were: 2196/2293 (95.8%) for 8 weeks and 3251/3344 (97.2%) for 12 weeks. SVR12 rates among all subgroups was greater than 95%, including in black patients, those with HIV co-infection and those with stage 3 fibrosis. Sex, age, race, genotype subtype, and fibrosis stage did not predict relapse among patients receiving 8 weeks of treatment. Systematic review yielded 6 studies meeting inclusion criteria for inclusion into the metaanalyses. Quality of evidence was determined by the Ottawa-Newcastle Scale. The forest plot depicting the relative risk for relapse for 8 versus 12 weeks is shown below in figure 16.
Figure 16: Forest plot Depicting Relative Risk for Relapse
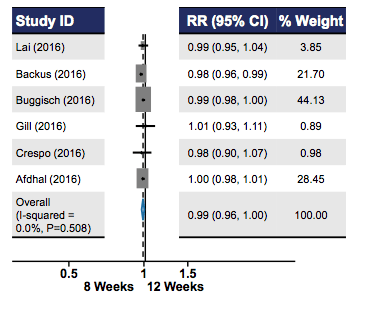
In conclusion, real-world data from a large individual patient data cohort and a meta-analysis of additional cohort studies demonstrates that 8 weeks of LDV/SOF achieves high SVR rates >95% in appropriately selected patients, regardless of fibrosis stage, race or HIV co-infection and has comparable outcomes to 12 weeks duration. Therefore, the 8 week LDV/SOF regimen needs to be incorporated into treatment algorithms, which may help to reduce cost and thereby increase access to therapy for more patients.
In addition to the metaanalyses various other real-life cohorts also reported back from 8 weeks of therapy in selected patient populations again enhancing the good response rates observed in non-cirrhotic patients (28,29). Of note these were in particular HIV/HCV coinfected patients where currently AASLD HCV guidelines do not recommend shortened treatment durations in HIV coinfection. In light of the growing body of good response rates after 8 weeks of sofosbuvir/ledipasvir in easy to treat patients this may need to be re-discussed.
AASLD: EIGHT WEEKS TREATMENT DURATION WITH LEDIPASVIR/SOFOSBUVIR (LDV/SOF) IS EFFECTIVE FOR APPROPRIATELY SELECTED PATIENTS WITH GENOTYPE 1 HEPATITIS C VIRUS (HCV) INFECTION: AN ANALYSIS OF MULTIPLE REAL WORLD COHORTS TOTALING >6,500 PATIENTS - (11/21/16)
AASLD: Ledipasvir/Sofosbuvir for 8 Weeks Results in High SVR Rates in Treatment-Naïve Patients With Chronic HCV Infection and HIV/HCV Coinfection - in Russia - (11/17/16)
HCV three drug rescue combinations with licensed drugs
Although, undoubtfully current SVR rates are high there are few patients who fail all oral DAA combination therapy, often with the emergence of resistance-associated substitutions (RAS) which then can pose quite some challenge when designing a new retreatment option. Combining drugs from all three available HCV DAA classes appears an attractive possibility as it promises high potency even in the presence of mutations against NS5A. At AASLD data from a randomized open-label study was presented which evaluated sofosbuvir (SOF) + grazoprevir (GZR) + elbasvir (EBV) + ribavirin (RBV) 16 vs 24 weeks in patients with NS5A or NS3 RASs at initial treatment failure following therapy with either SOF + LDV or DCV or SMV (30). Antiviral efficacy was evaluated using the secondary endpoint of SVR4 (SVR 4 weeks post-treatment). On-treatment responses and safety were also assessed. Twenty-six patients (20 males; mean age: 60 years) chronically infected with HCV genotype 1 (1a: n=8; 1b: n=11; 1d: n=1) or 4 (n=6) were randomized and treated. NS5A RASs were present in 24 patients (Y93H, n=17; L31M, n=7; Q30R, n=4); NS3 RAS were present in 2 patients. The main baseline characteristics are summarized in table 10.
Table 10: Baseline characteristics
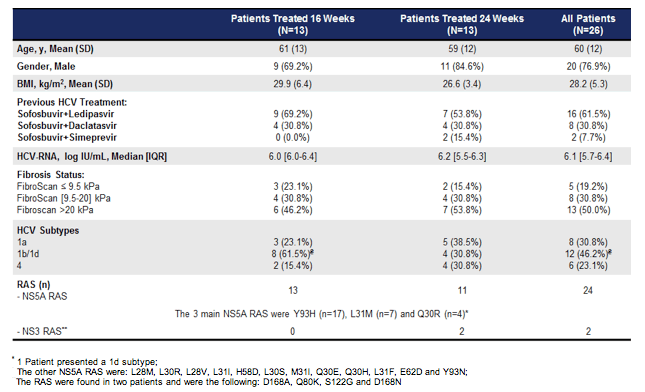
1 Patient presented a 1d subtype;
* The other NS5A RAS were: L28M, L30R, L28V, L31l, H58D, L30S, M31l, Q30E, Q30H, L31F, E62D and Y93N;
**The RAS were found in two patients and were the following: D168A, Q80K, S122G and D168N
Figure 17 shows the on treatment as well as SVR4 treatment responses for the two treatment groups. Of note at week 4 post treatment (SVR4) there were missing values for three patients. Two patients were still on therapy and had not yet reached this time-point; one patient was a patient randomized to 24 weeks treatment who had a liver transplantation, stopped prematurely treatment at W12, had negative HCV RNA 3 weeks later and died. No relapse was observed to date.
Figure 17: On treatment and SVR4 results
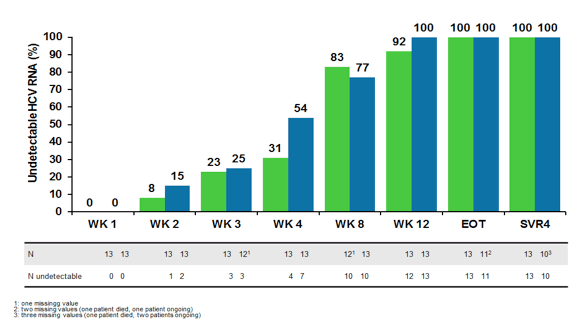
These findings suggest that retreating patients who failed a DAA-based regimen with NS5A/NS3 RASs with the combination of SOF + GZR + EBV + RBV for 16 weeks is efficacious and represent an interesting option particulalrly since this combination is already available in most countries. As drugs are from two companies and not part of a registered label reimbursement of this combination , however can represent a challenge.
New DAA combinations
New dual DAA combinations
One of this year AASLD highlights was clearly the wealth of data on the new and very potent Abbvie dual combination (Glecaprevir (ABT-493)/Pibrentasvir (ABT-530)), which was presented for treatment-naïve, experienced- and prior DAA-failure patients (8-10). The ENDURANCE-1 (NCT02604017) is a phase 3, randomized, open label, multicenter study enrolling patients without cirrhosis and with chronic HCV GT1 infection or HCV GT1/HIV-1 co-infection who are treatment-naïve or treatment-experienced (prior interferon [IFN] or pegIFN ± ribavirin [RBV], or sofosbuvir + RBV ± pegIFN therapy). Patients were randomized 1:1 to receive Glecaprevir/Pibrentasvir 300mg/120mg once daily for either 8 (Arm B) or 12 (Arm A) weeks (see figure 18). The primary endpoint is an evaluation of the non-inferiority of SVR at post-treatment week 12 (SVR12) among mono-infected HCV GT1 DAA-naïve patients with 12 weeks of treatment to a pre-specified historical SVR12 rate of 97%. This is followed in sequential fashion by an evaluation of the non-inferiority in SVR12 rates among mono-infected HCV GT1 DAA-naïve patients for 8 versus 12 weeks of treatment.
Figure 18: Study design of ENDURANCE-1
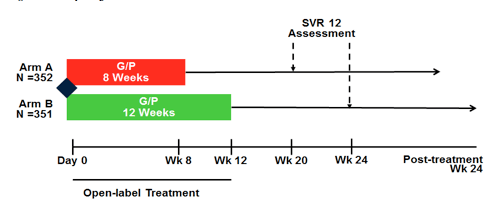
Overall, ENDURANCE-1 enrolled 703 patients (352 in Arm A and 351 in Arm B), including 33 (5%) patients with HCV GT1/HIV-1 co-infection, across 125 sites worldwide. At baseline, mean HCV RNA was 6.08 log10 IU/ml, 73% of patients had non-CC IL28B genotype, 43% had GT1a subtype, and 15% were fibrosis stage F2-F3. At baseline 1 and 0.3% of patients from the 8 versus 12 week arm displayed baseline polymorphisms in the NS3 region and 27% of both arms showed NS5A polymorphisms. The results for the ITT population excluding HIV coinfected patients and SOF-experienced patients are shown below in figure 19.
Figure 19: ENDURANCE-1: GLE/PIB x 8 Weeks or 12 Weeks in GT1 Non-cirrhotics
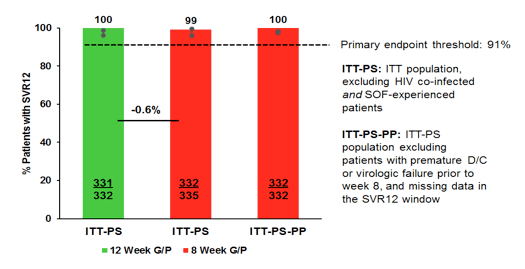
In summary, 99-100% of GT1 infected patients without cirrhosis achieved SVR12 with 8 or 12 weeks of Glecaprevir/Pibrentasvir (G/P). Indeed, 8-week treatment was non-inferior to 12-week treatment. SVR12 rates were high regardless of HIV-1 coinfection, prior treatment experience, baseline viral load or presence of baseline polymorphisms. G/P was well tolerated with no significant laboratory abnormalities. Only 0.1% of AEs led to discontinuation. The advent of another DAA combination which promises shorter treatment durations of 8 weeks will be particularly important for hard-to-reach populations with adherence challenges where shortening of treatment duration may be very instrumental. Also this may help to further lower cost burden of DAA therapy.
The next trial called SURVEYOR-II, part 4 evaluated the safety and efficacy of the shorter 8-week GLE/PIB treatment in patients with GT4-6 infection, and a larger cohort of GT2-infected patients (9). SURVEYOR-II part 4 is a phase 2, open-label, randomized, multicenter study where treatment-naïve or interferon- or sofosbuvir-experienced patients with GT2, 4, 5 or 6 infection without cirrhosis were enrolled into a single arm to receive 8-weeks of once-daily GLE/PIB (300 mg/120 mg). The corresponding study design is shown below in figure 20.
Figure 20: SURVEYOR-II part 4: study design
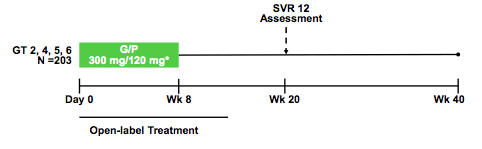
The primary endpoint was the number of patients with SVR12. For DAA-naïve GT2-infected patients, non-inferiority of SVR12 rates was evaluated by comparison to a historical standard-of care (12 weeks SOF + ribavirin) SVR12 rate of 95%. Safety was also assessed. Of the 203 patients enrolled, 145 (71%) had GT2 infection, and 46 (22%), 2 (1%), and 10 (5%) had GT 4, 5, and 6 infection, respectively. 48% of the patients included were male, 76% White, 10% Black, 11% Asian. 87% of patients were treatment-naïve, 10% IFN-experienced, 3% SOF-experienced and 84% had no significant fibrosis (F0-F1), 6% were F2, and 10% F3. 9% were on regular PPI use. The main SVR12 rates by genotype are shown below in figure 21.
Figure 21: SURVEYOR-II Part 4: GLE/PIB x 8 Weeks SVR12 results
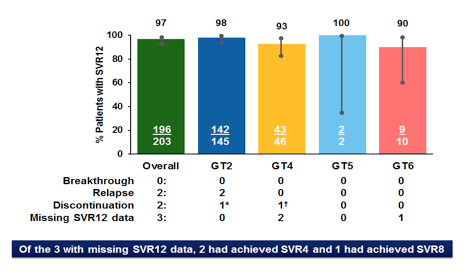
In DAA-naïve patients with GT2 infection, 8 week treatment was non-inferior to the historical 95% SVR12 rate achieved with 12 weeks of SOF/RBV. G/P for 8 weeks was well tolerated, with no discontinuations due to adverse events, no DAA-related serious adverse events and rare (single patient) grade 3 (AST or Bilirubin) lab abnormalities. Both GT2 patients who experienced a virological relapse were treatment experienced and showed at baseline the L31M NS5A polymorphism; no treatment-emergent new polymorphisms after relapse were found.
In summary, eight-week treatment with GLE/PIB yielded an overall SVR4 rate of 97% in non-cirrhotic patients with GT 2, 4, 5 or 6 infection, regardless of baseline polymorphisms or prior treatment experience.
The next study with GLE/PIB was a large, phase 3 trial (ENDURANCE-4) investigating the safety and efficacy of a 12-week treatment of once-daily, co-formulated ABT-493/ABT-530 in patients with HCV GT 4, 5, or 6 infection without cirrhosis (10). ENDURANCE-4 (NCT02636595) is a phase 3, multicenter, open label, single arm study that enrolled patients without cirrhosis who were either HCV treatment-naïve or treatment-experienced (interferon [IFN] or pegylated IFN ± ribavirin [RBV], or sofosbuvir + RBV with or without pegIFN). Patients were over 18 years of age with chronic HCV GT 4, 5, or 6 infection. Key exclusion criteria included presence of cirrhosis, as determined by either a liver biopsy (METAVIR score ≤3), a FibroScan score <12.5 kPa, or a FibroTest score of ≤0.48 and an APRI <1. Additional exclusion criteria were co-infection with HIV or HBV, or infection with more than one HCV GT. Enrolled patients received ABT-493/ABT-530 300mg/120mg once daily for
12 weeks. The study design is shown below in figure 22. Efficacy was calculated using a two-sided 95% confidence interval as the percent of patients achieving SVR at post-treatment week 12 (SVR12).
Figure 22: ENDURANCE-4: Study design
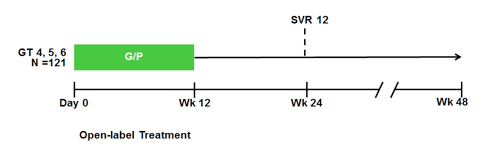
The study enrolled 121 patients at 32 sites across 8 countries in Europe, North America, and Africa; 76 patients were infected with GT4, 26 with GT5, and 19 with GT6. 64% were male, 71% were of white race. At baseline, the mean HCV RNA was 6.13 log10 IU/mL, 31% of patients were treatment-experienced, 14% had fibrosis stage of F2-F3, and most (75%) had non-CC IL28B genotype. The SVR12 rates overall as well as for the different genotypes included are shown below in figure 23.
Figure 23: ENDURANCE-4: SVR12 results
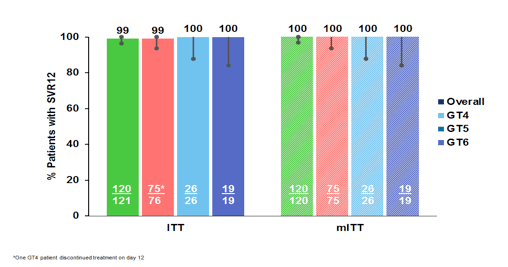
In summary, 99% of GT4-6 patients (120/121) without cirrhosis achieved SVR12 in ITT population following treatment with G/P with no virological failures. G/P was well tolerated: serious adverse events occurred in <1% of patients, there were no grade 3 or 4 lab abnormalities and discontinuation because of adverse events was rare. Overall, three patients discontinued because of anxiety, heartburn and one patient because of an ischemic transient attack.
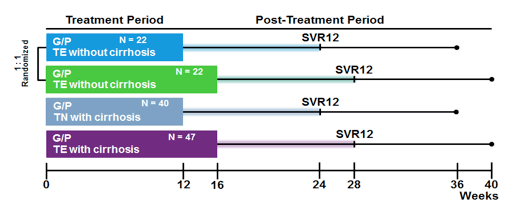
The final Glecaprevir/Pibrentasvir study to report back on was the SURVEYOR-II, Part 3, which is evaluating the efficacy and safety of co-formulated G/P in patients with chronic HCV GT3 infection, including those with prior treatment-experience and/or cirrhosis, for 12 or 16 weeks (31). SURVEYOR-II (NCT02243293) is a partially-randomized, open-label, multicenter, operationally adaptive phase 2/3 study. In part 3, treatment-experienced (prior IFN ± ribavirin or SOF plus ribavirin ± peg-IFN therapy) patients without cirrhosis were randomized 1:1 to receive either 12 or 16 weeks of G/P (300 mg/120 mg) once daily. Treatment-naïve or treatment-experienced patients with compensated cirrhosis were also treated with G/P (300mg/120 mg) once daily for 12 or 16 weeks, respectively. The primary endpoints were safety and the percentage of patients achieving SVR (HCV RNA <25 IU/mL)
at post-treatment week 12 (SVR12). The study design is shown below in figure 24.
Figure 24: SURVEYOR-2, part 3: study design
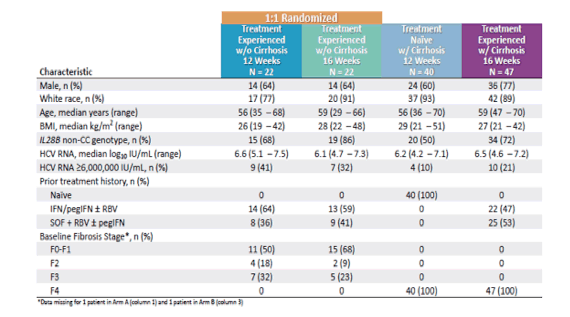
A total of 131 patients were enrolled in the study: 40 treatment-naïve with cirrhosis, and 46 and 45 treatment-experienced with and without cirrhosis, respectively. The mean baseline HCV RNA was 6.20 log10 IU/ml, and 66% of patients had non-CC IL28B genotype. The baseline characteristics for all treatment groups are summarized in figure 25.
Figure 25: SURVEYOR-II, part 3 baseline characteristics
The overall SVR12 rate for the four treatment arms is depicted below in figure 26.
Figure 26: SURVEYOR-II, part 3 SVR12 results
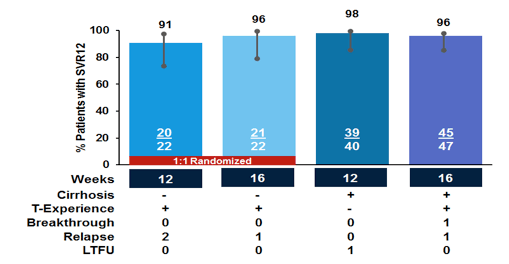
Of note overall virological response was very good with 91-98% SVR12 rates throughout the 4 groups. Three relapses were however, noted in the non-cirrhotic group (2 in the 12 week arm and 1 in the 16 week arm) and 1 relapse in the cirrhotic patients receiving 16 weeks of therapy. In that arm also one breakthrough occurred. This is somewhat in contrast to first results from small pilot trials with no failures. So although still a rare event, particularly in the difficult group of cirrhotic GT 3 patients there seem to be some challenges to treat patients remaining. It is also important to highlight that the breakthrough may be attributable to non-adherence reminding us all, especially when more hard-to reach patient populations will receive access to HCV therapy that despite short treatment durations there still remains a need for adherence training and awareness. More details on the respective five virological failures is summarized in table 11.
Table 11: Details of the virological failures
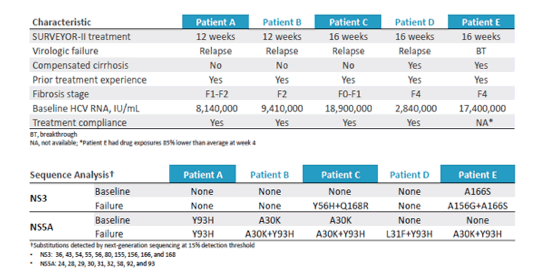
Interestingly, some patients who developed virological failure had no resistance-associated polymorphisms at baseline but some did; so under consideration of the few failures it is not answerable at this time whether the RAS at baseline contributed to virological failure or not. Clearly, in case of failure patients are very likely to develop more RAS in particular several NS5A polymorphisms.
G/P was well tolerated, with mostly mild adverse events, no DAA-related serious DAAs, few occurrences of grade 3 lab abnormalities (ALT or AST) and no study drug discontinuation.
In summary, treatment with G/P for 12 or 16 weeks was highly efficacious in treatment-experienced patients with HCV GT3 infection without cirrhosis as well as in treatment-naïve or experienced patients with cirrhosis. Rare cases of virological failure need to be collected in order to better understand which factors may predict relapse.
AASLD: ENDURANCE-1: A Phase 3 Evaluation of the Efficacy and Safety of 8- versus 12-week Treatment with Glecaprevir/Pibrentasvir (formerly ABT-493/ABT-530) in HCV Genotype 1 Infected Patients with or without HIV-1 Co-infection and without Cirrhosis - (11/15/16)
AASLD: ENDURANCE-2: Safety and Efficacy of Glecaprevir/Pibrentasvir in Hepatitis C Virus Genotype 2-infected Patients without Cirrhosis: a Randomized, Double-Blind, Placebo-Controlled Study - (11/14/16)
AASLD: EXPEDITION-4: EFFICACY AND SAFETY OF GLECAPREVIR/PIBRENTASVIR (ABT-493/ABT-530) IN PATIENTS WITH RENAL IMPAIRMENT AND CHRONIC HEPATITIS C VIRUS GENOTYPE 1 - 6 INFECTION - (11/15/16)
AASLD: SURVEYOR-II, PART 3: EFFICACY AND SAFETY OF GLECAPREVIR/PIBRENTASVIR (ABT-493/ABT-530) IN PATIENTS WITH HEPATITIS C VIRUS GENOTYPE 3 INFECTION WITH PRIOR TREATMENT EXPERIENCE AND/OR CIRRHOSIS - (11/14/16)
AASLD: SURVEYOR-II, Part 4: Glecaprevir/Pibrentasvir Demonstrates High SVR Rates in Patients With HCV Genotype 2, 4, 5, or 6 Infection Without Cirrhosis Following an 8-Week Treatment Duration - (11/16/16)
AASLD: ENDURANCE-4: Efficacy and Safety of Glecaprevir/Pibrentasvir (Formerly ABT-493/ABT-530) Treatment in Patients with Chronic HCV Genotype 4, 5, or 6 Infection - (11/14/16)
EASL: HIGH SVR RATES WITH ABT-493 + ABT-530 CO-ADMINISTERED FOR 8 WEEKS IN NON-CIRRHOTIC PATIENTS WITH HCV GENOTYPE 3 INFECTION - (04/18/16)
SURVEYOR-II: High SVR4 Rates Achieved With the Next Generation NS3/4A Protease Inhibitor ABT-493 and NS5A Inhibitor ABT-530 in Non-Cirrhotic Treatment-Naïve and Treatment-Experienced Patients With HCV Genotype 3 Infection - (12/01/15)
New three drug combinations
At AASLD various new three drug combinations were presented which may offer new potent pangenotypic regimens which may also be used for treatment of prior all oral DAA failures but also could allow shorter treatment durations because of increased potency. One of the prominently featured new 3-drug regimens was the combination of the already licensed and broadly available sofosbuvir/velpatasvir regimen combined together with the new pangenotypic HCV protease inhibitor Voxilaprevir (VOX, GS-9857) into a new fix-dose formulation. The so called POLARIS-2 study is a phase 3 study (NCT02607800) which compared treatment with SOF/VEL/VOX fixed dose combination (FDC) for 8 weeks to SOF/VEL FDC for 12 weeks in patients with genotype 1-6 HCV infection with and without compensated cirrhosis who have not previously received treatment with an HCV direct-acting antiviral agent (DAA) (1). Genotype 1-4 HCV-infected patients were randomized equally to receive open-label SOF/VEL/VOX (400 mg /100mg /100 mg daily) FDC for 8 weeks or SOF/VEL (400 mg /100 mg daily) FDC for 12 weeks and stratified according to HCV genotype, prior treatment with an interferon-based regimen, and cirrhosis status. Patients with other genotypes assessed at screening were enrolled in the SOF/VEL/VOX treatment arm. Patients with genotype 3 HCV infection and cirrhosis were excluded from this study but eligible for another Phase 3 trial (POLARIS-3). The primary endpoint was SVR12 with a pre-specified non-inferiority margin of 5%. The study design of POLARIS-2 is shown below in figure 27.
Figure 27: POLARIS-2 study design
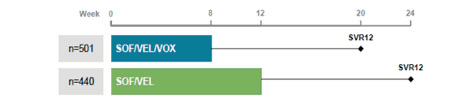
Of 941 HCV-infected patients enrolled and treated, 52% were male, 80% were white, 18% had cirrhosis, 23% had failed prior interferon-based therapy, 32% had the IL28B CC genotype; the median HCV RNA was 6.3 log10 IU/mL. The main baseline characteristics for the two study groups are shown below in table 12.
Table 12: POLARIS-2: Baseline characteristics
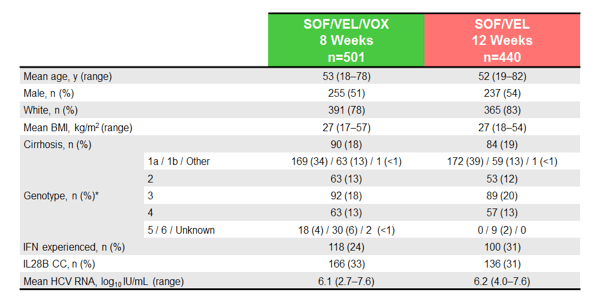
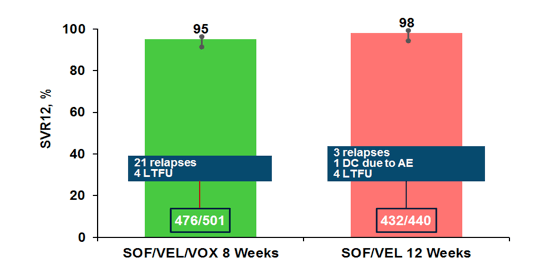
Of note, 18 and 19% of patients had cirrhosis at baseline in the two study arms, respectively. The SVR12 rates for the two study arms are shown in figure 28. Clearly the 8 week arm despite a high cure rate of 95% underperformed with 21 relapses suggesting that shortening of treatment duration may not be the way forward with this regimen for all genotypes or at least offered no advantage over the 12 week treatment arm with the dual regimen only.
Figure 28: POLARIS-2 study: SVR12 Results
The SVR12 rates by HCV genotype are shown below in figure 29.
Figure 29: POLARIS-2: SVR12 rates by HCV genotype for the two study arms
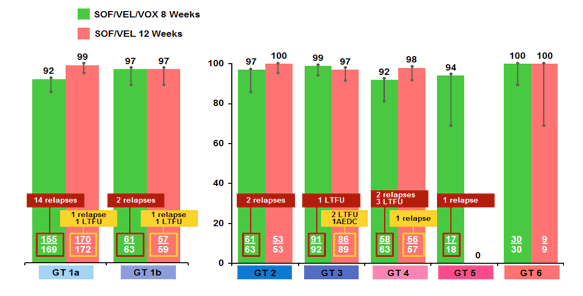
Interestingly, most relapses occurred in the GT1a 8 week triple drug arm suggesting that at least for this HCV genotype shorter treatment duration with this 3-drug regimen may be challenging whereas this may be different for HCV GT1b or even GT3.
Two patients (<1%), both in the SOF/VEL group, discontinued treatment prematurely due to
adverse events (AEs) assessed by the investigator as unrelated to study drug. The most common AEs (>10% in either group) were headache, fatigue, diarrhea and nausea; diarrhea and nausea were more common in the SOF/VEL/VOX group.
Treatment with the single tablet regimens of either SOF/VEL/VOX for 8 weeks or SOF/VEL for 12 weeks resulted in high SVR12 rates and was safe and well tolerated in genotype 1-6 DAA-naive patients with and without compensated cirrhosis. Higher relapse rates were noted in the 8 weeks of 3-drug treatment arm particularly in GT1a patients.
The POLARIS-3 study evaluated treatment with SOF/VEL/VOX FDC for 8 weeks and SOF/VEL FDC for 12 weeks in patients with genotype 3 HCV infection and cirrhosis (2). The hypothesis raised was that potentially addition of the HCV PI to SOF/VEL would allow shortening of treatment duration to 8 weeks. Overall, patients at 84 sites in North America, Europe, Australia, and New Zealand were randomized 1:1 to receive open-label SOF/VEL (400 mg /100 mg daily) FDC for 12 weeks or SOF/VEL/VOX (400 mg /100 mg /100 mg daily) FDC for 8 weeks. Patients were stratified according to their prior treatment with an interferon-based regimen. Patients had cirrhosis defined by liver biopsy, Fibroscan >12.5 kPa, or combined Fibrotest >0.74 and APRI >2.0. HCV RNA was measured with the CAP/CTM HCV 2.0 assay with LLOQ =15 IU/mL. The primary endpoint compares the sustained virologic response 12 weeks after treatment (SVR12) of each treatment, to a pre-specified historic control rate of 83%. Secondary endpoints included safety and tolerability, viral resistance, and additional efficacy outcomes. The study design is shown in figure 30.
Figure 30: POLARIS-3: Study design
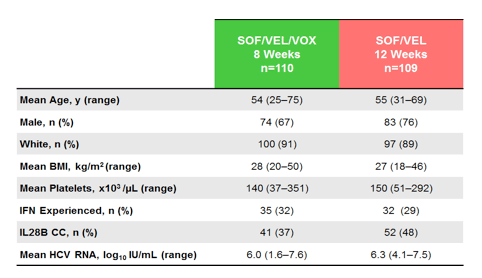
Of 219 patients randomized and treated, 72% were male, 89% were white, 42% had the IL28B CC genotype, and 30% had previously failed treatment with an interferon-based regimen. Patients from the US (44%) and other regions (56%) were well represented. Most (90%) patients with treatment experience had received a Peg-IFN+RBV regimen. Importantly, by inclusion criteria all patients had cirrhosis so clearly resembling a more challenging to treat patient population; the median platelet count was 139x103 cells/mL with 24% of patients having a platelet count of <100 x103 cells/mL. Baseline characteristics are shown below in figure 31.
Figure 31: POLARIS-3: Baseline characteristics
Overall, both treatment groups reached a high SVR12 rate of 96% with 2 relapses observed in the 3-drug arm and 1 relapse and 1 breakthrough in the dual treatment arm. Interestingly, there were 6 patients with Y93H at baseline in the SOF/VEL/VOX group and 4 in the SOF/VEL group which all achieved SVR12. No treatment emergent RASs were found in the SOF/VEL/VOX group whereas in the SOF/VEL group, both virologic failures developed an Y93H. The SVR12 rates for both treatment groups are shown below in figure 32.
Figure 32: POLARIS-3 SVR12 results
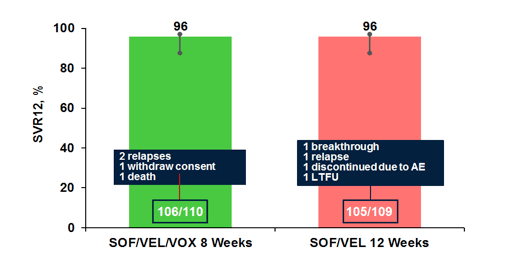
In summary, the single tablet regimen of SOF/VEL/VOX for 8 weeks has the potential to be a safe, well tolerated and effective treatment option for genotype 3 patients with cirrhosis.
The next important studies on the new SOF/VEL/VOX fixed dose combination were performed in patients with prior failure to DAA based HCV therapies. The POLARIS-1 study aimed at evaluating treatment with the SOF/VEL/VOX fixed dose combination (FDC) for 12
Weeks in patients who previously received an NS5A inhibitor (3). Overall, patients from 108 sites in North America, Europe, Australia and New Zealand were enrolled. Eligible patients received at least 4 weeks of a prior NS5A inhibitor-containing regimen which was not discontinued due to an adverse event or unsuccessful due to non-compliance. Those with HCV genotype (GT) 1 were randomized 1:1 to receive SOF/VEL/VOX (400mg/100mg/100mg) or matching placebo daily for 12 weeks, stratified by the presence or absence of cirrhosis. Patients of all other GTs were assigned to receive SOF/VEL/VOX for 12 weeks. Those patients assigned to receive placebo will be offered deferred treatment with SOF/VEL/VOX for 12 weeks. The primary endpoint evaluates the superiority of the sustained virologic response 12 weeks after treatment (SVR12) to a pre-specified performance goal of 85%. The study design of POLARIS-1 is shown below in figure 33.
Figure 33: POLARIS-1 study design
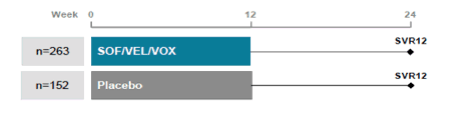
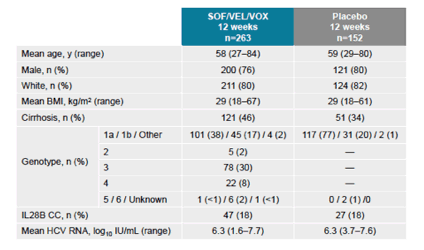
Of 415 patients included, 77% were male, 78% were white, 18% had the IL28B CC genotype, 41% had compensated cirrhosis, 57% were from the US and 73% had GT 1 HCV infection. The majority of patients had DAA experience with an NS5A inhibitor given in combination with an NS5B inhibitor, and the most common prior treatment regimen was ledipasvir/SOF n=133 (51, DCV n= 70 (27%), and Ombitasvir (PrOD), n = 30 (11%). The baseline characteristics of POLARIS-1for both arms are summarized in table 13.
Table 13: POLARIS-1 baseline demographics
Overall, 96% of patients in the 12 week SOF/VEL/VOX arm achieved SVR12, whereas no one in the placebo arm achieved SVR12. Superiority was achieved (p<0.001) compared with the prespecified 85% performance goal for SOF/VEL/VOX. The SVR12 rates by cirrhosis status at baseline are shown below in figure 34.
Figure 34: POLARIS-1:SVR12 rate results by cirrhosis state
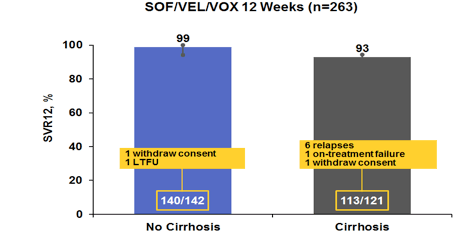
Overall, high SVR rates were noted in this difficult to treat group of prior DAA failures. Of note, 6 relapses and 1 on-treatment failure were observed in the patients with cirrhosis at baseline versus no relapses in patients without any cirrhosis. SVR12 rates by genotype are summarized in figure 35.
Figure 35: POLARIS-1: SOF/VEL/VOX 12 Weeks (n=263) SVR12 rates by genotype
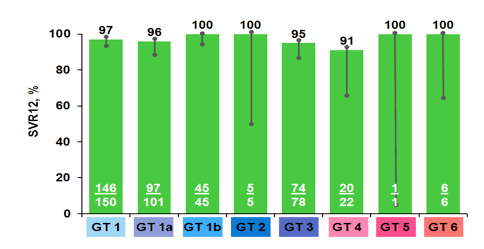
Obviously, some genotypes are underrepresented limiting possible conclusions. But on average cure rates were high independent of prevailing genotype. A subanalysis by baseline RASs is depicted below in figure 36.
Figure 36: POLARIS-1: Results by baseline RASs
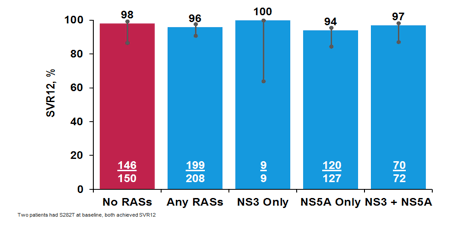
No new resistance associated substitutions (RASs) were observed in patients with HCV relapse (n=6). Safety analysis revealed overall good tolerability. Numerically headache and diarrhea were slightly higher in the 3 drug arm versus placebo treated patients. There was only one discontinuation due to adverse events in the 3-drug arm versus three discontinuations due to AEs in the placebo arm. The main adverse events for the two arms are shown in figure 37.
Figure 37: POLARIS-1: Adverse events
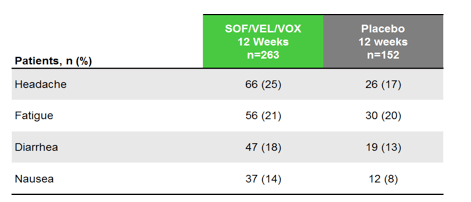
In conclusion, in NS5A-inhibitor experienced patients treatment with SOF/VEL/VOX for 12 weeks resulted in a 96% SVR rate in difficult-to-cure patients. No treatment emergent RASs were observed among patients who developed a relapse. SOF/VEL/VOX was well tolerated with a safety profile similar to that observed in placebo recipients.
The final POLARIS study to report back from is POLARIS-4 which evaluated treatment with a SOF/VEL/VOX fixed dose combination (FDC) for 12 weeks and a SOF/VEL FDC for 12 weeks as salvage regimens in DAA-experienced patients who had not previously received an NS5A inhibitor (4). In this controlled trial of persons who failed non-NS5A containing DAA regimens (SOF 73% or SOF+RBV/IFN) patients were randomized to SOF/VEL/VOX for 12 weeks (n=182) versus SOF/VEL for 12 weeks (n=151). The study design is shown below in figure 38.
Figure 38: POLARIS-4: Study design
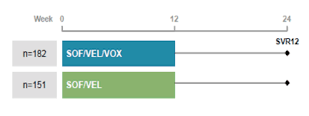
Patients at 101 sites in North America, Europe, Australia and New Zealand were enrolled and those with genotypes 1, 2 or 3 were randomized 1:1 to receive open-label SOF/VEL/VOX or SOF/VEL for 12 weeks, stratified according to genotype and cirrhosis status. Patients of all other genotypes were assigned to receive SOF/VEL/VOX for 12 weeks. DAA-experienced patients who previously were treated with an NS5A inhibitor or with an NS3/4A protease inhibitor in combination with ribavirin and Peg-IFN were excluded. The primary endpoint evaluates the superiority of the sustained virologic response 12 weeks after treatment (SVR12) of each treatment to a pre-specified performance goal of 85%. The main baseline characteristics are shown below in table 14.
Table 14: POLARIS-4: Baseline characteristics
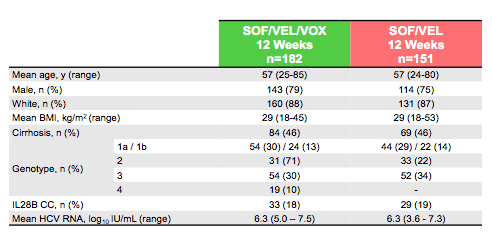
Of the 333 patients who were randomized and treated, 77% were male, 86% were white, 18% had the IL28B CC genotype, 46% had compensated cirrhosis, 57% were from the United
States and 40% had genotype 1 HCV infection. The overall SVR rate as well as the SVR rate by cirrhosis status is shown below in figure 39.
Figure 39: POLARIS-4 results
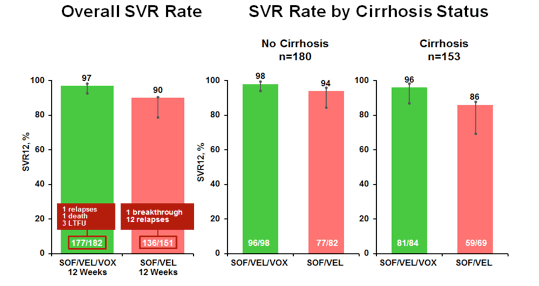
Treatment with SOF/VEL/VOX for 12 weeks resulted in an impressive high SVR12 rate of 97% which was higher than the 90% SVR12 with SOF/VEL for 12 weeks. Overall, only one relapse was noted in the 3 drug arm vs 12 relapses and one breakthrough in the dual treatment arm. Superiority was achieved for SOF/VEL/VOX compared with the prespecified 85% performance goal (p<0.001) but not for SOF/VEL (p=0.092). Baseline RASs did not impact treatment outcome for either SOF/VEL/VOX or SOF/VEL. Of note no treatment emergent RASs were found in SOF/VEL/VOX treated patients whereas 11/15 patients receiving SOF/VEL developed an Y93H. The SVR12 rate by genotype is shown below in figure 40.
Figure 40: POLARIS-4: results by genotype
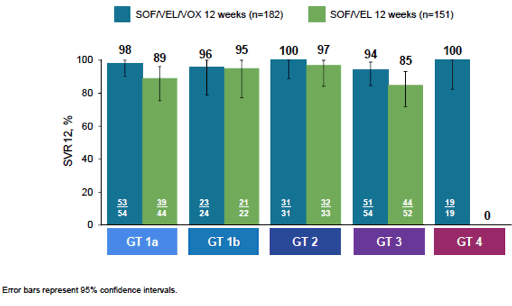
Treatment was well tolerated, only one patient has discontinued therapy with SOF/VEL after 8 weeks of treatment (due to headache). No serious adverse events attributed to either study medication had been reported.
The single tablet regimens of SOF/VEL/VOX and SOF/VEL for 12 weeks have the potential to provide safe, well tolerated and effective retreatment options for patients who did not previously achieve SVR following treatment with non-NS5A inhibitor-containing DAA regimens. Lower relapse rates can be expected for the 3 drug regimen over the dual regimen.
AASLD: A Randomized, Phase 3 Trial of Sofosbuvir/Velpatasvir/Voxilaprevir for 8 Weeks and Sofosbuvir/Velpatasvir for 12 Weeks for Patients with Genotype 3 HCV Infection and Cirrhosis: The POLARIS-3 Study - (11/15/16)
AASLD: A Randomized Phase 3 Trial of Sofosbuvir/Velpatasvir/Voxilaprevir for 8 Weeks Compared to Sofosbuvir/Velpatasvir for 12 Weeks in DAA-Naïve Genotype 1-6 HCV Infected Patients: The POLARIS-2 Study - (11/15/16)
AASLD: Sofosbuvir/Velpatasvir/Voxilaprevir for 12 Weeks as a Salvage Regimen in NS5A Inhibitor-Experienced Patients With Genotype 1-6 Infection: The Phase 3 POLARIS-1 Study - (11/15/16)
AASLD: A Randomized, Controlled, Phase 3 Trial of Sofosbuvir/Velpatasvir/Voxilaprevir or Sofosbuvir/Velpatasvir for 12 Weeks in Direct-Acting Antiviral-Experienced Patients With Genotype 1-6 HCV Infection: The POLARIS-4 Study - (11/14/16)
AASLD: Integrated Analysis of Sofosbuvir +Ribavirin, Ledipasvir/Sofosbuvir or Sofosbuvir/Velpatasvir for the Treatment of Genotype 4 Chronic HCV Infection - (11/15/16)
Another interesting new 3 drug combination presented at AASLD was MK3. MK3 is a three-drug regimen formulated into a fixed-dose combination tablet. The regimen is given as two tablets, once-daily, without regard to food. This triplet is also called MK-3682B and consists of the HCV NS5B polymerase nucleotide inhibitor MK-3682, the already registered HCV NS3/4A protease inhibitor grazoprevir and the HCV NS5A next-generation inhibitor Ruzasvir (MK-8408).
The C-CREST part B trial evaluated the safety and efficacy of the FDC regimen, with or without ribavirin (RBV), in non-cirrhotic and cirrhotic GT1-, 2-, and 3-infected patients (5). Overall 664 patients with chronic HCV infection were treated in Part B. The study design is shown below in figure 41.
Figure 41: Study design
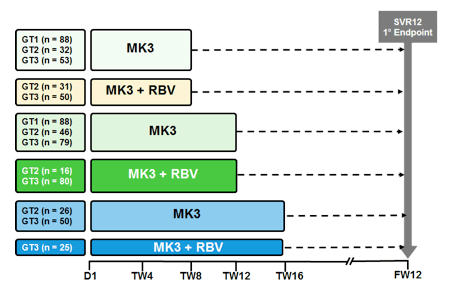
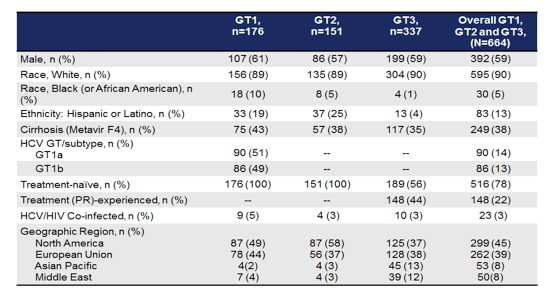
So for the GT1 patients it was a randomized comparison between 8 and 12 weeks of the triplet in treatment-naïve patients with or without cirrhosis. For GT 2 (treatment-naïve only) or 3 it was 8 versus 12 weeks of the triplet with or without ribavirin versus 16 weeks of the triplet. And then there was an additional arm of the triplet for 16 weeks plus ribavirin for GT 3 patients only. The main baseline characteristics for the different genotype populations are shown below in table 15. Of note only for GT3 patients, treatment experienced patients were also included. Patients could be HCV mono or HIV-coinfected.
Table 15: baseline characteristics
The overall SVR response rates by genotype are depicted below in figure 42.
Figure 42: SVR12 results of the C-CREST part B study by genotype
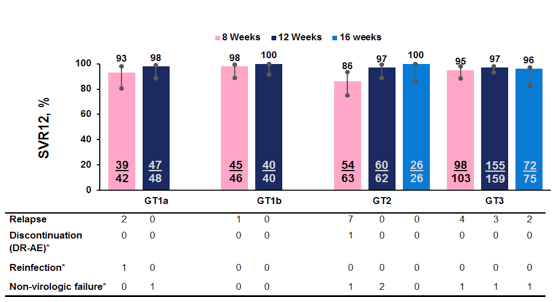
Of note high SVR12 rates were obtained for all genotypes throughout all study arms. Numerically, however relapse rates appeared to be higher in the shorter treatment arm of 8 weeks for GT1, even more clear for GT2 and slightly also for GT3. No relapse at all was observed under 12 weeks of treatment in GT1 and GT2 patients, whereas there were few failures for GT3 in the 12 or 16 week arm, respectively. Furthermore, the addition of ribavirin for the GT 2 or 3 patients did not increase SVR12. Efficacy was maintained in GT3 treatment-experienced patients with cirrhosis (SVR12 = 99%). Figure 43 shows a subanalysis by cirrhosis status for the HCV GT1 patients only.
Figure 43: SVR12 rates by cirrhosis status for all GT1 patients
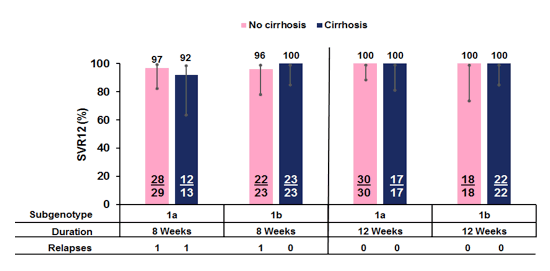
No impact of cirrhosis status at baseline on SVR12 rate was observed within the GT1 patients.
In summary, MK3 (MK-3682/grazoprevir/ruzasvir) for 8 or 12 weeks was highly effective in treatment-naïve GT1 patients (SVR12 97%). MK3 for 12 or 16 weeks was also highly effective in treatment-naïve GT2 patients (SVR12 98%). And finally MK3 was highly effective for 8,12, or 16 weeks in GT3 treatment-naïve or experienced patients. Ribavirin did not add to SVR12. MK3 was generally safe and well tolerated.
C-CREST-1 and 2 part C was a further study which evaluated MK3 as a retreatment regimen for patients who had previously failed therapy with a 3-drug direct-acting antiviral (DAA) combination (6). GT1-, 2-, and 3-infected treatment-naïve, non-cirrhotic patients with chronic HCV infection who relapsed after 8 weeks of therapy with one of 4 regimens including grazoprevir (100 mg), MK-3682 (300 mg or 450 mg), and either elbasvir (50 mg) or MK-8408 (60 mg) were offered retreatment with 16 weeks of a fixed-dose combination of MK-3682 (450 mg)/grazoprevir/ruzasvir (MK-8408) plus ribavirin (RBV). The corresponding study design is shown in the figure 44.
Figure 44: Study design of the C-CREST-1 and 2 part C
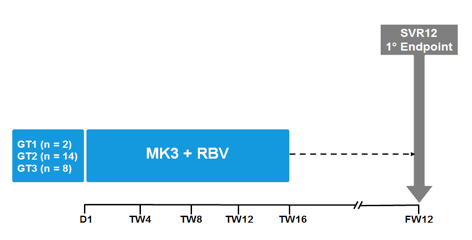
Twenty-four of 26 eligible patients were enrolled, 2 with GT1, 14 with GT2, and 8 with GT3 infection. At the time of relapse following initial therapy, NS5A RAVs were detected in 0% (0/2) GT1, 93% (13/14) GT2 and 88% (7/8) GT3 patients. NS3 RAVs were detected in 50% (1/2) GT1, 100% (14/14) GT2, and 100% (8/8) GT3 patients. NS5B RAVs were detected in 50% (1/2) GT1, 0% (0/14) GT2, and 0% (0/8) GT3 patients. 88% (21/24) patients had RAVs in >1 class. Table 16 summarizes the frequency of RAVS at retreatment.
Table 16: Frequency of RAVS at retreatment
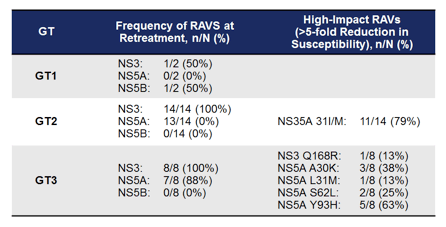
One GT2-infected patient withdrew after a single dose with adverse events (AEs) of vomiting and tachycardia. The remaining 23 patients completed the full 16 weeks of dosing. All patients had undetectable HCV RNA at the end of treatment and 12 weeks after stopping therapy (SVR12). Figure 45 summarizes the SVR12 rate by genotype.
Figure 45: C-CREST Part C: MK3 + RBV x 16 Weeks: SVR12 by Genotype
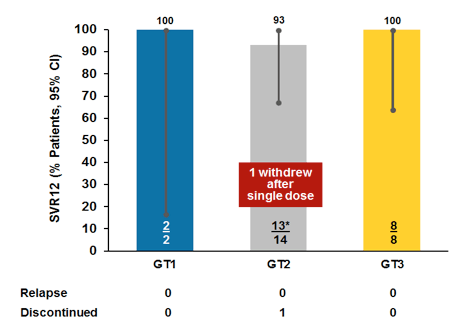
Treatment was generally well tolerated, and no cardiac or renal safety signals were identified. The most frequent study drug-related AEs in >10% of all patients were headache, fatigue, nausea, rash, pruritus, insomnia, decreased hemoglobin and cough.
In summary, a 16-week regimen of the fixed-dose combination of MK-3682 (450 mg)/grazoprevir/ruzasvir plus RBV was highly effective and well-tolerated in GT1-, 2-, and 3-infected treatment-naïve, non-cirrhotic patients who had previously failed 8 weeks of treatment with a 3-drug regimen, despite a high prevalence of baseline NS3 and NS5A RAVs. This offers a new treatment option with high probability of success even in the very challenging to treat group of prior all oral DAA combination treatment failure.
The final MK3 study to report back on was the C-SURGE study which determined the safety and efficacy of the regimen of MK-3682 (NS5B polymerase inhibitor) / grazoprevir (NS3/4A protease inhibitor) / ruzasvir (MK-8408) (NS5A inhibitor) in patients who failed a previous DAA regimen (7). This multicenter, open-label trial randomized compensated cirrhotic (platelet cutoff=75,000μL;excluded Child-Pugh B & C) or non-cirrhotic HCV GT1-infected patients who relapsed after a recommended regimen of LDV/SOF or EBR/GZR to receive a once-daily regimen of MK-3682 (450 mg)/grazoprevir (100 mg)/ruzasvir (60 mg) either 16 weeks + ribavirin (RBV) or 24 weeks without RBV. Patients who failed LDV/SOF were stratified by previous 8 or ≥12 week regimen. Next-generation sequencing (15% sensitivity) was used to test for baseline RAVs. The primary objectives of the trial are to determine the efficacy (the proportion of patients with HCV to determine the efficacy (the proportion of patients with HCV RNA <15 IU/mL at 12 weeks after the end of study therapy; SVR12), and the safety & tolerability of the regimen. The study design is shown below in 46.
Figure 46: C-SURGE: Study design
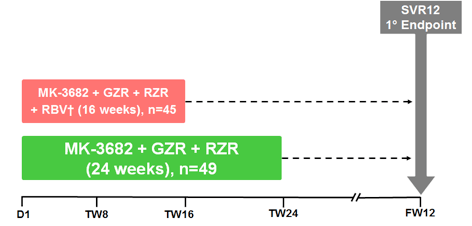
94 GT1 patients were randomized in this trial (78 [83%] GT1a; 16 [17% GT1b]; 64 [68%] HCV RNA >1 million IU/mL at screening). Patients had failed 12 or 24 weeks of LDV/SOF
(59 [63%]), 8 weeks of LDV/SOF (13 [14%]), or 12 weeks of EBR/GZR (22 [23%]). Forty-two patients (45%) had cirrhosis. More than 75% of patients had at least 1 NS5A RAV at baseline. The treatment outcome is shown in figure 47.
Figure 47: Treatment outcome of the C-SURGE trial
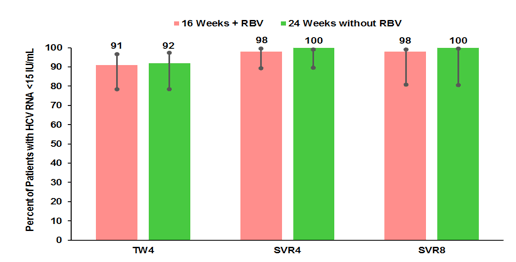
One patient withdrew from the study after receiving three doses. All other patients were undetectable at 8 weeks after stopping therapy (SVR8) indicating a very high cure success rate in a very difficult to treat patient group. Figure 47 summarizes the impact of baseline RAVS on treatment outcome.
Figure 47: Impact of Baseline NS5A or NS3 RAVs on SVR4
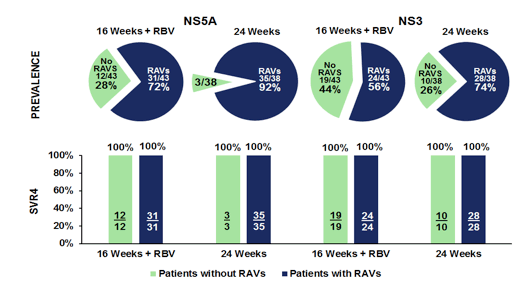
Further subanalysis revealed that there was also no impact of baseline Y93 RAVs in NS5A on SVR4. Treatment was generally well tolerated in both arms. Most adverse events were mild or moderate and no patient discontinued due to an adverse event.
Overall, the retreatment regimen of MK-3682/grazoprevir/ruzasvir in previous all oral DAA combination treatment failure patient led to a very high SVR8 rate with no virological failure observed so far. No difference was found between 16 weeks of MK3 and ribavirin or 24 weeks of MK2 without ribavirin.
In summary, all the new three drug regimens promise great retreatment options for previous all oral DAA failures irrespective of resistance associated substitutions accumulated during virological failure. Treatment duration shortening may work in some selected patient groups and genotypes but not universally.
AASLD: Safety and Efficacy of the Fixed-Dose Combination Regimen of MK-3682 / Grazoprevir / MK-8408 (Ruzasvir) in Cirrhotic or Non-cirrhotic Patients with Chronic HCV GT1 Infection who Previously Failed a Direct-acting Antiviral Regimen (C-SURGE) - (11/15/16)
AASLD: High Sustained Virologic Response Rates in Patients with Chronic HCV GT1, 2 or 3 Infection Following 16 Weeks of MK-3682/Grazoprevir/MK-8408 (Ruzasvir) Plus Ribavirin After Failure of 8 Weeks of Therapy (Part C of C-CREST-1 & 2) - (11/14/16)
AASLD: Safety and Efficacy of the Fixed-Dose Combination Regimen of MK-3682/Grazoprevir/MK-8408 (Ruzasvir) With or Without Ribavirin in Non-cirrhotic or Cirrhotic Patients with Chronic HCV GT1, 2 or 3 Infection (Part B of C-CREST-1 & -2) - (11/14/16)
AASLD: ELBASVIR/GRAZOPREVIR PLUS SOFOSBUVIR ± RIBAVIRIN IN TREATMENT-NAIVE AND TREATMENT-EXPERIENCED PATIENTS WITH HEPATITIS C VIRUS GENOTYPE 3 INFECTION AND COMPENSATED CIRRHOSIS: THE C-ISLE STUDY - (11/14/16)
Summary
⋅HBV reactivation occurs earlier and is clinically more significant in HCV patients coinfected with chronic HBV treated with all oral combination DAA therapy. Overall, HBV reactivation however, is a rare event. Nevertheless HBV serology and HBs-Ag screening is recommended prior therapy.
⋅Further efforts are needed to improve adherence to HCC surveillance in chronic hepatitis C patients with cirrhosis.
⋅Completion of SOF-containing treatment in real-life cohorts was not independently associated with risk of incident liver cancer, regardless of IFN co-medication. The strongest risk factors for liver cancer remain the traditional risk factors such as baseline cirrhosis, older age, and male gender.
⋅Results from a large Italian DAA treated cohort with advanced liver disease indicates that in cirrhotic patients the incidence of HCC during the first 6-9 months following initiation of DAAs therapy is not different from that expected in untreated patients according to historical controls. However, the atypical HCC pattern seen in about half of the cases with more aggressive courses deserves better understanding.
⋅4 weeks of sofosbuvir, ledipasvir and ribavirin with or without interferon was highly effective in curing chronic hepatitis C in a hard to reach but easy to treat population of non-cirrhotic drug users on opioid substitution therapy with only one virological relapse detected in an adherent patient. Clearly, the numbers are too small to generalize findings but at least it appears that in non-cirrhotic patients this may be an interesting treatment alternative when treatment duration is of concern.
⋅Treatment of HCV in the Department of Correction (DOC) by telemedicine with DAA is not only feasible, but has a very high SVR12. The higher SVR12 in the DOC compared to the private clinic setting may be due to directly observed therapy or differences in patient characteristics.
⋅Analysis from the German Hepatitis C-Registry, a large national real-life patient cohort, finds no difference in HCV cure rates between HIV/HCV and HCV mono-infected patients and therefore supports current HCV guidelines which no longer see a need to consider HIV co-infected individuals as a special patient population.
⋅An amazing 100% of HCV patients with all genotypes and advanced renal disease were cured after receiving Glecaprevir and pibrentasvir. Clearly the numbers for some of the genotypes were small but the data strongly encourages collecting more data on this regimen in patients with renal insufficiency and HCV GT2 or 3 infection where so far only limited options exist.
⋅In large real-world cohorts, all-oral DAA treatments are effective and well tolerated in patients >70 years of age and can therefore be safely used in this particular patient group..
⋅Real-world data from a large individual patient data cohort and a meta-analysis of additional cohort studies demonstrated that 8 weeks of LDV/SOF achieve high SVR rates >95% in appropriately selected patients, regardless of fibrosis stage, race or HIV co-infection and has comparable outcomes to 12 weeks duration. Therefore, the 8 week LDV/SOF regimen needs to be incorporated into treatment algorithms, which may help to reduce cost and thereby increase access to therapy for more patients.
⋅In the ENDURANCE-1 trail, 99-100% of GT1 infected patients without cirrhosis achieved SVR12 with 8 or 12 weeks of Glecaprevir/Pibrentasvir (G/P). Indeed, 8-week treatment was non-inferior to 12-week treatment. SVR12 rates were high regardless of HIV-1 coinfection, prior treatment experience, baseline viral load or presence of baseline polymorphisms. G/P was well tolerated with no significant laboratory abnormalities.
⋅In SURVEYOR-II part 4 eight-week treatment with GLE/PIB yielded an overall SVR4 rate of 97% in non-cirrhotic patients with GT 2, 4, 5 or 6 infection, regardless of baseline polymorphisms or prior treatment experience.
⋅In ENDURANCE-4 99% of GT4-6 patients (120/121) without cirrhosis achieved SVR12 in ITT population following treatment with G/P with no virological failures.
⋅In SURVEYOR-II part 3, treatment with G/P for 12 or 16 weeks was highly efficacious in treatment-experienced patients with HCV GT3 infection without cirrhosis as well as in treatment-naïve or experienced patients with cirrhosis. Rare cases of virological failure need to be collected in order to better understand which factors may predict relapse.
⋅Treatment with the single tablet regimens of either SOF/VEL/VOX for 8 weeks or SOF/VEL for 12 weeks resulted in high SVR12 rates and was safe and well tolerated in genotype 1-6 DAA-naive patients with and without compensated cirrhosis. Higher relapse rates were noted in the 8 weeks of the 3-drug treatment arm particularly in GT1a patients, whereas comparable relapse rates were found for GT 1b and 3.
⋅The single tablet regimen of SOF/VEL/VOX for 8 weeks has the potential to be a safe, well tolerated and effective treatment option for genotype 3 patients with cirrhosis.
⋅In NS5A-inhibitor experienced patients treatment with SOF/VEL/VOX for 12 weeks resulted in a 96% SVR rate in difficult-to-cure patients. No treatment emergent RASs were observed among patients who developed a relapse. SOF/VEL/VOX was well tolerated with a safety profile similar to that observed in placebo recipients.
⋅The single tablet regimens of SOF/VEL/VOX and SOF/VEL for 12 weeks have the potential to provide safe, well tolerated and effective retreatment options for patients who did not previously achieve SVR following treatment with non-NS5A inhibitor-containing DAA regimens. Lower relapse rates can be expected for the 3 drug regimen over the dual regimen.
⋅MK3 (MK-3682/grazoprevir/ruzasvir) for 8 or 12 weeks was highly effective in treatment-naïve GT1 patients (SVR12 97%). MK3 for 12 or 16 weeks was also highly effective in treatment-naïve GT2 patients (SVR12 98%). And finally MK3 was highly effective for 8,12, or 16 weeks in GT3 treatment-naïve or experienced patients. Ribavirin did not add to SVR12. MK3 was generally safe and well tolerated.
⋅In summary, a 16-week regimen of the fixed-dose combination of MK-3682 (450 mg)/grazoprevir/ruzasvir plus RBV was highly effective and well-tolerated in GT1-, 2-, and 3-infected treatment-naïve, non-cirrhotic patients who had previously failed 8 weeks of treatment with a 3-drug regimen, despite a high prevalence of baseline NS3 and NS5A RAVs. This offers a new treatment option with high probability of success even in the very challenging to treat group of prior all oral DAA combination treatment failure.
⋅Overall, the retreatment regimen of MK-3682/grazoprevir/ruzasvir in previous all oral DAA combination treatment failures (LDV/SOF or EBR/GZR) led to a very high SVR8 rate with no virological failure observed so far. No difference was found between 16 weeks of MK3 and ribavirin or 24 weeks of MK2 without ribavirin.
⋅In summary, all the new three drug regimens promise great retreatment options for previous all oral DAA failures irrespective of resistance associated substitutions accumulated during virological failure. Treatment duration shortening may work in some selected patient groups and genotypes but not universally.
References
1. Jacobson IM et al.: A Randomized Phase 3 Trial of Sofosbuvir/Velpatasvir/Voxilaprevir for 8 Weeks Compared to Sofosbuvir/Velpatasvir for 12 Weeks in DAA-Naïve Genotype 1-6 HCV-Infected Patients: The POLARIS-2 Study. 67th Annual Meeting of the American Association for the Study of Liver diseases, November 11-15, 2016, Boston, USA; abstract LB-12
2. Foster G et al.: A Randomized Phase 3 Trial of Sofosbuvir/Velpatasvir/Voxilaprevir for 8 Weeks and Sofosbuvir/Velpatasvir for 12 Weeks for Patients with Genotype 3 HCV Infection and Cirrhosis: The POLARIS-3 Study. 67th Annual Meeting of the American Association for the Study of Liver diseases, November 11-15, 2016, Boston, USA; abstract 258
3. Bourliere M et al.: Sofosbuvir/Velpatasvir/Voxilaprevir for 12 Weeks as a Salvage Regimen in NS5A Inhibitor-Experienced Patients with Genotype 1-6 Infection: The Phase 3 POLARIS-1 Study. 67th Annual Meeting of the American Association for the Study of Liver diseases, November 11-15, 2016, Boston, USA; abstract 194
4. Zeuzem S et al.: A Randomized, Controlled, Phase 3 Trial of Sofosbuvir/Velpatasvir/Voxilaprevir or Sofosbuvir/Velpatasvir for 12 Weeks in Direct Acting Antiviral-Experienced Patients with Genotype 1-6 HCV Infection: The POLARIS-4 Study. 67th Annual Meeting of the American Association for the Study of Liver diseases, November 11-15, 2016, Boston, USA; abstract 109
5. Lawitz E et al.: Safety and Efficacy of the Fixed-Dose Combination Regimen of MK-3682/Grazoprevir/MK-8408 With or Without Ribavirin in Non-cirrhotic or Cirrhotic Patients with Chronic HCV GT1, 2 or 3 Infection (Part B of C-CREST-1 & 2). 67th Annual Meeting of the American Association for the Study of Liver diseases, November 11-15, 2016, Boston, USA; abstract 110
6. Serfaty L et al.. High Sustained Virologic Response (SVR) Rates in Patients with Chronic HCV GT1, 2 or 3 Infection Following 16 Weeks of MK-3682/Grazoprevir/MK-8408 Plus Ribavirin After Failure of 8 Weeks of Therapy (Part C of C-CREST-1 & 2). 67th Annual Meeting of the American Association for the Study of Liver diseases, November 11-15, 2016, Boston, USA; abstract 112
7. Wyles D et al.: Safety and Efficacy of the Fixed-Dose Combination Regimen of MK-3682/Grazoprevir/MK-8408 in Cirrhotic or Non-cirrhotic Patients with Chronic HCV GT1 Infection who Previously Failed a Direct-acting Antiviral Regimen (C-SURGE). 67th Annual Meeting of the American Association for the Study of Liver diseases, November 11-15, 2016, Boston, USA; abstract 193
8. Zeuzem S et al. ENDURANCE-1: Efficacy and Safety of 8- versus 12-week Treatment with ABT-493/ABT-530 in patients with Chronic HCV Genotype 1 Infection. 67th Annual Meeting of the American Association for the Study of Liver diseases, November 11-15, 2016, Boston, USA; abstract 253
9. Hassanein T et al.: Glecaprevir/Pibrentasvir Demonstrates High SVR Rates in Patients with HCV Genotype 2, 4, 5, or 6 Infection without Cirrhosis Following an 8-Week Treatment Duration (SURVEYOR-II, Part 4). 67th Annual Meeting of the American Association for the Study of Liver diseases, November 11-15, 2016, Boston, USA; abstract LB-15
10. Asselah T et al.: ENDURANCE-4: Efficacy and Safety of ABT-493/ABT-530 Treatment in Patients with Chronic HCV Genotype 4, 5, or 6 Infection. 67th Annual Meeting of the American Association for the Study of Liver diseases, November 11-15, 2016, Boston, USA; abstract 114
11. Øvrehus AL et al.: Four weeks of sofosbuvir, ledipasvir and ribavirin with or without interferon give high cure rates in drug users with hepatitis C - a randomized controlled trial (4WIDUC). 67th Annual Meeting of the American Association for the Study of Liver diseases, November 11-15, 2016, Boston, USA; abstract 921
12. Sterling R et al.: Treatment of HCV in the Department of Corrections (DOC) in the era of Oral Direct Acting Antivirals (DAA). 67th Annual Meeting of the American Association for the Study of Liver diseases, November 11-15, 2016, Boston, USA; abstract 882
13. Llerana S et al.: A program of Testing and Treat Intended to Eliminate Hepatitis C in a Prison: The JAILFREE-C study. 67th Annual Meeting of the American Association for the Study of Liver diseases, November 11-15, 2016, Boston, USA; abstract 916
14. Gil-Martin A et al.: Real-world Outcomes With New HCV Antivirals in HIV/HCV-coinfected Subjects: Madrid Coinfection Registry(Madrid-CoRE) Findings. 67th Annual Meeting of the American Association for the Study of Liver diseases, November 11-15, 2016, Boston, USA; abstract 78
15. Naggie S et al.: Real World Effectiveness of Ledipasvir/Sofosbuvir (LDV/SOF) in Patients Coinfected With HCV and HIV-1: A Comparative Analysis of Clinical Trials with Four Real World Cohorts. 67th Annual Meeting of the American Association for the Study of Liver diseases, November 11-15, 2016, Boston, USA; abstract 898
16. Rockstroh J et al.: SVR12 rates under DAA-based HCV therapy from the National German Cohort Study: Does HIV co-infection impair the response to DAA combination therapy? 67th Annual Meeting of the American Association for the Study of Liver diseases, November 11-15, 2016, Boston, USA; abstract 907
17. Gane E, et al.: EXPEDITION-IV: Safety and Efficacy of GLE/PIB in Adults with renal impairment and Chronic Hepatitis C Virus Genotype 1 - 6 Infection. 67th Annual Meeting of the American Association for the Study of Liver diseases, November 11-15, 2016, Boston, USA; abstract LB-11
18. Welzel T et al.: Real-World Effectiveness and Safety of DAA Combination Therapies in Elderly Patients > 70 Years of Age in the German Hepatitis C-Registry (DHC-R). 67th Annual Meeting of the American Association for the Study of Liver diseases, November 11-15, 2016, Boston, USA; abstract 951
19. Sundaram V et al.: Eight weeks treatment duration with Ledipasvir/Sofosbuvir (LDV/SOF) is effective for appropriately selected patients with genotype 1 Hepatitis C virus (HCV) infection: an analysis of multiple real world cohorts totaling >6,500 patients. 67th Annual Meeting of the American Association for the Study of Liver diseases, November 11-15, 2016, Boston, USA; abstract LB-16
20. Bersoff-Matcha S, et al.: Hepatitis B Reactivation Associated with Direct Acting Antiviral Therapy for Hepatitis C: A Review of Spontaneous Post-Marketing Cases. 67th Annual Meeting of the American Association for the Study of Liver diseases, November 11-15, 2016, Boston, USA; abstract LB-17
21. Wang C et al.: Hepatitis B reactivation after interferon-based therapy versus pan-oral direct acting antiviral agents in chronic hepatitis C patients co-infected with hepatitis B virus: a systematic review and meta-analysis. 67th Annual Meeting of the American Association for the Study of Liver diseases, November 11-15, 2016, Boston, USA; abstract 918
22. Tran SA et al.: Poor Adherence to Hepatocellular Carcinoma (HCC) Surveillance in a U.S. Cohort of 2376 Patients with Chronic Hepatitis C (CHC) and Cirrhosis. 67th Annual Meeting of the American Association for the Study of Liver diseases, November 11-15, 2016, Boston, USA; abstract 918
23. Chokkalingam AP et al.: Risk of incident liver cancer following HCV treatment with sofosbuvir-containing regimens. 67th Annual Meeting of the American Association for the Study of Liver diseases, November 11-15, 2016, Boston, USA; abstract 739
24. Romano A et al.: Incidence and pattern of "de novo" hepatocellular carcinoma in HCV patients treated with oral DAAs. 67th Annual Meeting of the American Association for the Study of Liver diseases, November 11-15, 2016, Boston, USA; abstract 19
25. Benvegnù L, et al.: Natural history of compensated viral cirrhosis: a prospective study on the incidence and hierarchy of major complications. Gut. 2004 May;53(5):744-9.
26. Sangiovanni A, et al.: The natural history of compensated cirrhosis due to hepatitis C virus: A 17-year cohort study of 214 patients. Hepatology. 2006 Jun;43(6):1303-10.
27. Neukam K et al.: HIV coinfection impairs the response to DAA-based HCV therapy. 51st EASL; Barcelona, Spain; April 13-17, 2016. Abstract LBP513
28. Isakov V et al.: Ledipasvir/Sofosbuvir for 8 Weeks Results in High SVR Rates in Treatment-Naïve Patients with Chronic HCV Infection and HIV/HCV Co-Infection. 67th Annual Meeting of the American Association for the Study of Liver diseases, November 11-15, 2016, Boston, USA; abstract 2030
29. Buggisch P et al.: 8 weeks treatment under real life conditions with Ledipasvir/Sofosbuvir in HIV co-infected treatment-naïve HCV genotype 1 patients demonstrates similar results to mono-infected HCV patients: data from the German Hepatitis C-Registry (DHC-R). 67th Annual Meeting of the American Association for the Study of Liver diseases, November 11-15, 2016, Boston, USA; abstract 883
30. De Ledinghen V et al.: Retreatment with sofosbuvir + grazoprevir + elbasvir + ribavirin of patients with Hepatitis C virus Genotype 1 or 4 with RASs at failure of a sofosbuvir + ledipasvir or + daclatasvir or + simeprevir regimen (ANRS HC34 REVENGE study). 67th Annual Meeting of the American Association for the Study of Liver diseases, November 11-15, 2016, Boston, USA; abstract LB-18
31. Wyles DL et al.: SURVEYOR-II, Part 3: Efficacy and Safety of ABT-493/ABT-530 in Patients with Hepatitis C Virus Genotype 3 Infection with Prior Treatment Experience and/or Cirrhosis. 67th Annual Meeting of the American Association for the Study of Liver diseases, November 11-15, 2016, Boston, USA; abstract 113
|
| |
|
 |
 |
|
|