 |
 |
 |
| |
HIV Boosts Risk of Persistently High ALT After HCV Clearance - "Persistent Aminotransferase Elevation
following HCV clearance in Adults
with and without HIV"
|
| |
| |
18th International Workshop on Comorbidities and Adverse Drug Reactions in HIV, September 12-13, 2016, New York
Mark Mascolini
One in 5 HIV-positive people had persistent alanine aminotransferase (ALT) elevations after HCV clearance in a 275-person longitudinal study [1]. HIV independently raised the risk of persistently high ALT.
Direct-acting antivirals (DAAs) clear HCV in most people with or without HIV infection. National Institute of Allergy and Infectious Disease (NIAID) researchers who conducted this study noted that continued monitoring may be prudent after sustained virologic response (SVR) to DAAs in people with advanced fibrosis. But regular post-SVR screening is not recommended for people without cirrhosis. Still, ALT may remain elevated after SVR, with unknown consequences.
The NIAID team performed this prospective longitudinal study to see how often ALT stays high in HIV-positive and negative people successfully treated for HCV. They also aimed to pin down predictors of persistently elevated ALT after HCV clearance.
The study involved 275 people with chronic HCV who achieved and maintained SVR. At annual visits they had liver function tests and assays for hepatitis B surface antigen, HCV RNA, and HIV RNA. People with HIV were taking antiretrovirals, and 261 participants had liver biopsy before anti-HCV therapy. The researchers defined ALT elevation as a value above 30 U/L.
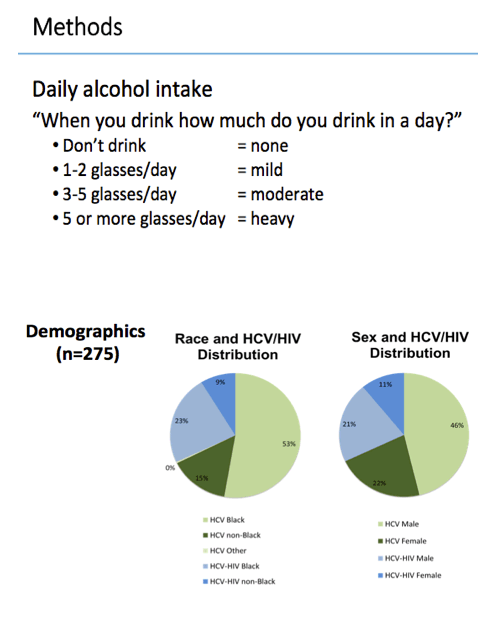
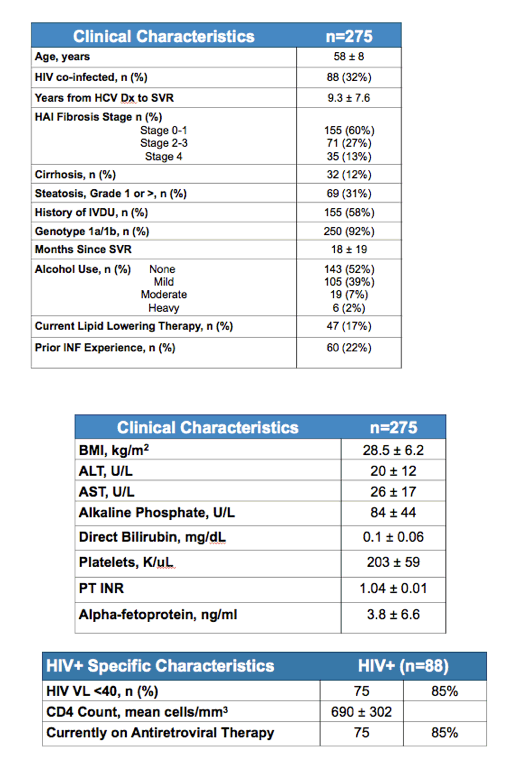
Of the 275 participants, 88 (32%) had HIV infection, 76% were black, and 67% were men. The group averaged 58 years in age, and time from HCV diagnosis to SVR averaged 9.3 years. Time since SVR averaged 18 months. HAI fibrosis stages were 0-1 in 60%, 2-3 in 27%, and 4 in 13%. Thirty-two people (12%) had cirrhosis, and 69 (31%) had grade 1 or worse steatosis. More than half of participants, 58%, had a history of injecting drugs.
While 52% of participants did not drink alcohol, 39% were moderate drinkers (1-2 drinks daily), 7% moderate drinkers (3-4 drinks daily), and 2% heavy drinkers (5 or more drinks daily). ALT averaged 20 U/L, aspartate aminotransferase 26 U/L, and alkaline phosphatase 84 U/L. Among people with HIV, 85% were taking antiretroviral therapy, 85% had a viral load below 40 copies, and CD4 count averaged 690.
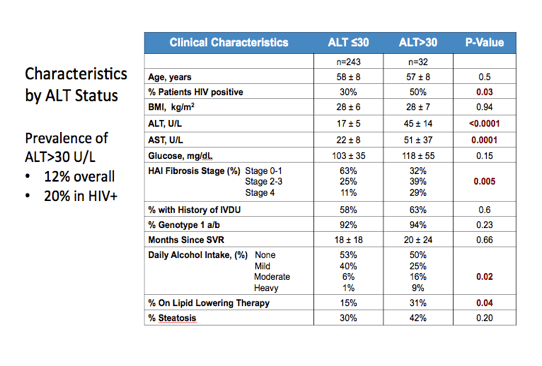
Thirty-two people overall (12%) had an ALT above 30 U/L after SVR, while 18 (20%) with HIV has persistently high ALT. Moderate and heavy drinking were more common in people with high ALT (25%) than in those with lower ALT (7%) (P = 0.02), and a higher proportion of people with high ALT were taking antilipid agents (31% versus 15%, P = 0.04).
Logistic regression analysis identified four independent predictors of ALT above 30 U/L after SVR: HIV positivity (P = 0.01), worse fibrosis stage (P = 0.0005), heavier alcohol drinking (P = 0.0007), and lipid-lowering therapy (P = 0.04). When the researchers analyzed ALT as a continuous variable, HIV, fibrosis stage, and more alcohol use remained independent predictors of higher ALT. Antiretroviral therapy, HIV RNA, and CD4 count did not predict ALT elevation.
The NIAID investigators stressed that HIV infection boosts the risk of post-SVR ALT elevation independently of alcohol use or fibrosis stage. They underlined the continuing importance of alcohol counseling after SVR. And they noted that the potential long-term impact of persistently elevated ALT remains to be determined.
Reference
1. Hadigan C, Howard L, Sheehan J, et al. Persistent aminotransferase elevations following HCV clearance in adults with and without HIV. 18th International Workshop on Comorbidities and Adverse Drug Reactions in HIV, September 12-13, 2016, New York. Abstract O024.


|
| |
|
 |
 |
|
|