 |
 |
 |
| |
Differences by HIV Serostatus in Coronary Artery
Disease Severity following Stress Testing
|
| |
| |
Reported by Jules Levin
CROI 2016 Feb 22-24 Boston
Matthew J. Feinstein MD1, Brian Poole BA2, Tim S. Provias MD1, Frank J. Palella MD3, Chad J. Achenbach MD MPH3, Donald M. Lloyd-Jones MD ScM4
from the Division of Cardiovascular Diseases1and Division of Infectious Diseases2, Department of Medicine3; and Department of Preventive Medicine4; Northwestern University Feinberg School of Medicine
Program Abstract
HIV-infected persons develop coronary artery disease (CAD) more commonly and earlier than uninfected patients. The role of noninvasive cardiovascular testing to stratify CAD risk in this population is not well-defined; no prior studies have evaluated cardiovascular stress testing in this group. We hypothesized that, among persons with abnormal stress tests, HIV-infected patients have a greater burden of CAD on coronary angiography than uninfected matched controls.
Cohort study using a cohort created in the Northwestern Medicine Enterprise Data Warehouse (NMEDW) of HIV-infected patients and age, sex, and race-matched controls who underwent cardiovascular stress testing and subsequent coronary angiography from 2000 to 2015. Persons with incomplete data for either stress tests or coronary angiography were excluded, as were persons whose stress tests did not precede coronary angiography. Relative risks were used to assess differences in CAD burden by HIV serostatus for persons with abnormal stress tests. The cutoffs for moderate and severe CAD on angiography were at least one coronary artery stenosis of ≥50% and ≥70%, respectively.
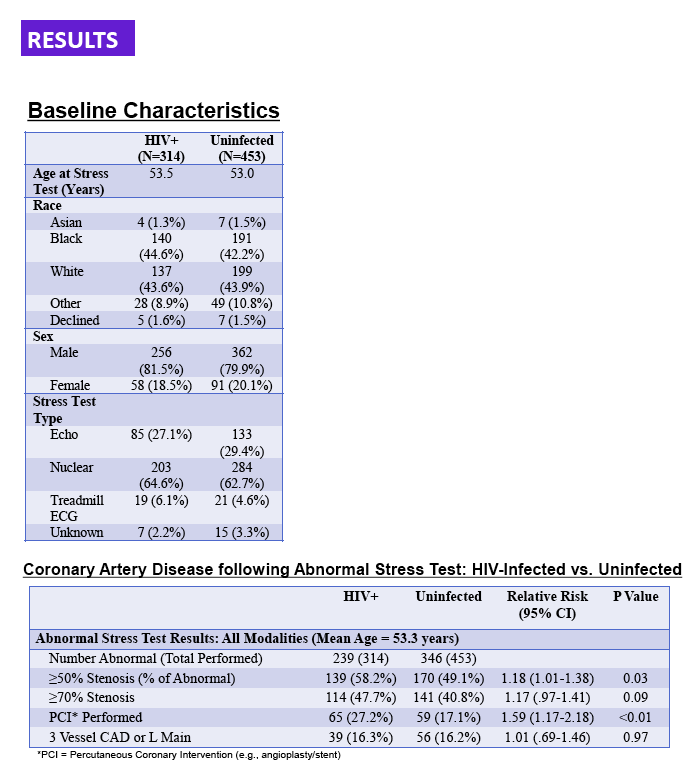
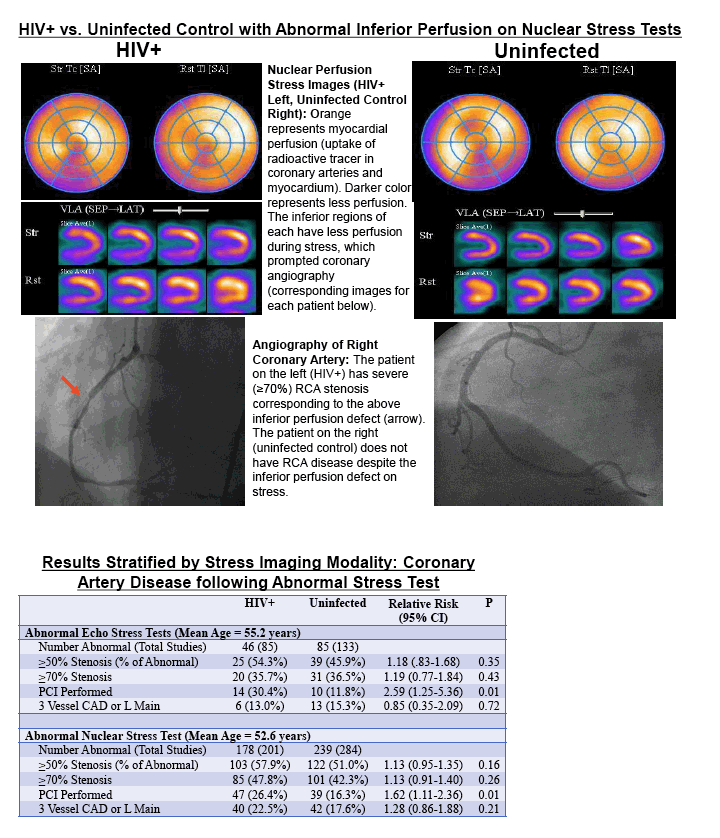
There were 239 HIV-infected patients (mean age at stress test 53.5 years, 44.6% black, 43.6% white, 18.5% women) and 346 uninfected matched patients (mean age at stress test 53.0 years, 42.2% black, 43.9% white, 20.1% women) with abnormal stress tests (73% nuclear, 23% echocardiographic, 4% other) that prompted coronary angiography. HIV infection was associated with significantly greater risk for moderate or severe CAD on angiography (RR 1.18, 95% CI 1.01-1.38, P=0.03) and subsequent percutaneous coronary intervention (RR 1.59, 95% CI 1.17-2.18, P<0.01) following abnormal stress testing (Table). Among HIV-infected patients with abnormal stress tests, those with a nadir HDL cholesterol level under 30 mg/dl were at significantly elevated risk for severe CAD (RR 1.53, 95% CI 1.05-2.23, P=0.02); this remained true when analyses were restricted to men only (RR 1.75, 95% CI 1.12-2.77, P=0.01). Risks for severe CAD among HIV-infected persons with abnormal stress tests did not significantly differ by peak total cholesterol level, CD4 nadir, and plasma HIV RNA nadir.
HIV-infected patients with abnormal cardiovascular stress tests had significantly greater CAD burden and were more likely to undergo PCI compared with uninfected controls. The implications of these findings for CAD screening for HIV-infected persons require further study.


|
| |
|
 |
 |
|
|